

|
Points on the Lung MeridianChapter 3:
Commonly Used Meridian Points
From R. C. Schafer, DC, PhD, FICC's best-selling book:
“Applied Physiotherapy in Chiropractic”
The following materials are provided as a service to our profession. There is no charge for individuals to copy and file these materials. However, they cannot be sold or used in any group or commercial venture without written permission from ACAPress.
All of Dr. Schafer's books are now available on CDs, with all proceeds being donated
to chiropractic research. Please review the complete list of available books.The Theoretical Basis of Meridian Therapy Theoretical Concepts The Nonneural Theories The Neural Theories The Cutaneovisceral Reflex The Viscerocutaneous Reflex Segmental and Intersegmental Effects Near and Distant Effects The Gate Control Theory and Its Clinical Significance Scientific Evidence Empirical Evidence Meridian Trigger points and Their Palpation Standard Methods of Stimulation Site Location Locating Points Background Preparation Types and Characteristics of Acupuncture Points Electrical Analysis The Human Inch Major Points: Locations, Primary Indications, and Precautions The Lung Meridian The Large Intestine Meridian The Stomach Meridian The Spleen Meridian The Heart Meridian The Small Intestine Meridian The Urinary Bladder Meridian The Kidney Meridian The Heart Constrictor Meridian The Triple Heater Meridian The Gallbladder Meridian The Liver Meridian The Conception Vessel Meridian The Governing Vessel Meridian Alarm Points Master Points Association Points Closing Remarks ReferencesChapter 3: Commonly Used Meridian Points
This chapter delineates a few of the many theories attempting to explain the mechanisms of acupuncture point (acupoint) stimulation and meridian therapy. Stimulation of specific points on the body as a mechanism for pain control has achieved great interest in this country in recent years. The majority of studies center on stimulating endorphin production in the body. (See Table 3.1). Antidotal and clinical evidence as well as patient records from Oriental cultures point to numerous cases where specific point stimulation has affected visceral and functional disease processes. In the context of physiologic therapeutics, the location, primary indications, and precautions associated with the major points (ie, those most commonly used) are reviewed.
Table 3.1. Isolated Peptides of the Endorphin Superfamily
After Fields [47]
I. Peptides of the pro-opiamelanocortin series A. Opioid peptides II. Enkephalinsb–endorphin
a–endorphin
n–endorphin
B. Nonopioidsn MSH
b MSH
n MSH3Met5–enkephalin
Leu5–enkephalin
Met5-Arg6-Phe7–enkephalinIII. C–terminally extended enkephalins Dynorphin IV. Others
a–neoendorphin
b–neoendorphinKyotorphin
Dermophin
Casei-morphin
-------------------------------, as described by Judovich and Bates, shows how visceral pain can radiate to certain parts of the skin. A familiar example is cardiac ischemia with radiating pain to the left arm. [25, 26] In this context, Wernoe stimulated the rectum of a decapitated plaice electrically and found that the skin became pale. He also stimulated areas of the gastrointestinal tract of the eel and cod and noted that in each case the skin became lighter over an area of several dermatomal segments. [27] It can therefore be readily appreciated that a visceral problem can exhibit in a specific dermatomal segment via a viscerocutaneous reflex and that the stimulation of the skin can have a distinct effect on a related visceral area via a cutaneovisceral reflex.
SEGMENTAL AND INTERSEGMENTAL EFFECTS
Most of the reflexes used to explain the effects of acupuncture are segmental and follow specified dermatomal patterns. [28–30] Others, however, are intersegmental. For instance, stimulation of acupuncture points of the foot has been shown to affect organs over 10 dermatomes away. [31, 32] A possible explanation of this phenomenon is via the long reflex of Sherrington. [33, 34] In contrast, those reflexes that fit into the dermatomes are segmental reflexes, often referred to as Sherrington’s short reflexes. The scratch reflex of a dog is a good example of an intersegmental cutaneomotor reflex.
NEAR AND DISTANT EFFECTS
One of the most perplexing problems is that some of the effects of acupuncture cannot be explained neurologically by either segmental or intersegmental mechanisms. For example, the effects of stimulating the acupuncture points of the head cannot be readily explained. However, some research has shown that a distinct reflex may probably exist between the nose and the heart or between the turbinates and the sexual organs. [35, 36] Some scientific explanation for this is therefore likely.
The scientific proof for these reflexes is important, but it does not fully or even adequately explain exactly what happens according to the empiric results obtained. The Chinese for many years have attempted an explanation in the philosophical terms of Taoism with reference to Yin/Yang (law of opposites) and to the circulation of biologic energy (life force, Qi [pronounced chi]).
THE GATE CONTROL THEORY AND ITS CLINICAL SIGNIFICANCE
The next consideration is the more recent Gate Theory, as described in Chapter 2. Although this theory, originally set forth by Melzack and Wall, has been amended to some extent, it is basically the same as originally proposed, and it would be well to summarize it here. [37–39]
The gate theory holds that the large myelinated nerve fibers of the skin have an inhibitory effect, when stimulated, on the small pain-evoking fibers that enter the same segment of the cord. [40] The large, rapid-conducting, alpha and beta fibers of the skin conduct impulses via the dorsal columns to the brainstem and from there to the cerebral cortex. Small diameter, slow-conducting C fibers convey protopathic or pathologic and traumatic pain signals of the small fibers that arise from the deeper tissues of the body. If this were not so, the body would be in a constant state of pain. The stimuli from the dermis specifically produce inhibition in the cells of the substantia gelatinosa of Rolando, which is found in the dorsal horn of the spinal cord. It is believed that the dermal stimulus depolarizes the cells here, which renders them incapable of receiving and transmitting pain signals. Thus, painful stimuli are blocked (ie, the "gate" is closed), according to Melzack and Wall. If, however, the small fiber system is excessively stimulated by some disease process, the small fiber system then gains dominance and the patient perceives pain. It is then said that the pain gate has been opened by the increased stimulation from the small fibers of the deep somatic and visceral tissues.
This theory has many practical applications in clinical practice. For example, let us suppose that the "gates" are open and the patient is in severe pain. What can be done to relieve this suffering? Studies have shown that the inhibitory effects are enhanced when the large diameter fibers of the skin are sufficiently stimulated and the pain gate in the dorsal horn may be closed. In addition, these fast-conducting fibers may also arouse inhibitory responses in the brainstem that produce a downward projection of impulses to various levels of the spinal cord that further inhibit the transmission of pain signals that would normally progress to the brain. [41] It is by way of this system of inhibitory projections that the full value (ie, relief from pain) can be realized.
Surgical research on patients with intractable pain has shown that the implantation of a dorsal column stimulator (ie, TENS) can often completely block the transmission of painful or protopathic impulses. [42, 43]
SCIENTIFIC EVIDENCE
Meridian therapy with needles, moxa, electrical stimulation, or by means of other modalities most likely work by such a mechanism; viz, by blocking pain signals in or to the brain by projecting inhibitory impulses to the thalamus and/or cerebral cortex and ultimately to the cord, and finally, by blocking noxious stimuli through the pathophysiologic reflex and thus producing muscular relaxation. Therefore, it should be noted that acupuncture is veiled in empiric evidence. Obviously, then, current scientific proof for acupuncture explains in part much of what happens when acupoints are stimulated.
Although the Melzack-Wall theory explains how pain pathways can be blocked, it does not adequately explain any possible localized tissue changes that are known to occur. By extension of this theory, however, local tissue changes may be postulated on the basis of localized vascular changes; ie, improvement in the local microcirculation. [44]
Recent studies, several without a credible basis, have been advocated. In France, ECG readings on heart patients showed improvement after acupuncture treatments. [45] In Russia, a sensitive stethoscope supposedly noted different sounds over acupoints. The Russians also noted a difference in the skin temperature over acupuncture points.
Much research still needs to be performed. It appears to be that there are demonstrable entities called acupuncture points, but scientific verification for chartable meridians connecting these points is still wanting at this writing. However, according to a 1985 paper from Russia referring to research being conducted at the Department of Neurology of the Kiev Institute for Physicians, Macheret and his associates have shown the existence of complex functional relationships between various parts of the human body and the internal organs. Their findings appear to support the existence of "channels" that are identical to those that the Orientals call meridians. "The ‘body channels’ in their peripheral link are connected with somatic and vegetative conductors running both independently in the form of nerve trunks, and like plexuses that get around the vessels and the muscles and reach the ‘root’ spinal cells and truncus sympathicus nodes from which the corresponding segmental associations pass to the internal organs." According to these researchers, the channels in their central link constitute the conductive pathways of the spinal cord and the brain. [46]
EMPIRIC EVIDENCE
The volume of recently acquired empiric evidence cannot be denied. To mention just a few for example, Fields has shown that acupuncture, through the stimulation of endorphins, is an effective modality in the treatment of pain, behavior modification, relief of the symptoms of drug withdrawal, and stimulating the autoimmune system. [47] After treating just one point for acute dysmenorrhea in 10 patients, Slagoski found complete effectiveness in the resolution of the pain syndrome. [48] Tseung and Vazharov describe case after case of musculoskeletal disorders, anxiety and depression, growth problems, primary infertility, impotence, induction of labor, episcleritis, chronic asthmatic bronchitis, and canker sores (aphthous stomatitis) that responded to acupuncture after failing to respond under Western medical treatment. [49, 50]
Kitzinger, a medical doctor, believes that even if acupuncture may achieve good, even spectacular, results by itself, he recommends combining it with neural therapy (electrical), manipulative therapy (chiropractic), and other standard physiotherapeutic modalities when vertebrogenic disorders are treated. He states that "Combining acupuncture with manipulative therapy for a blockage is not only feasible, but also in some cases, the only correct procedure to achieve a therapeutic breakthrough." [51] Shafshak compared the effectiveness of electroacupuncture to that of standard physiotherapy in the treatment of tension myositis: 93.3% responded completely to electroacupuncture and 90.9% recovered completely in response to physiotherapy. [52]
While acupuncture per se has not been as effective in treating disorders of a purely psychic nature, it has been in relieving physiologic disturbances. Odell reports that when it is used in conjunction with hypnosis and visualization techniques, it has shown to be a consistent and invaluable tool in a behavioral reprogramming technique. [53]
Meridian Trigger points and Their PalpationStandard Methods of Stimulation
Acupuncture points are commonly stimulated by several methods:
Using 30-, 32-, or 34-gauge, 1/2 to 1-1/2-inch stainless steel needles that are carefully inserted at specific preselected sites for durations ranging from a few seconds to 20 minutes or more.
Using electrical stimulation with any modality designed for this purpose.
Using a specially designed blunt instrument (teishin).
Using finger or thumb pressure.
Using a helium neon or infrared laser (controversial).
Using tiny beads sometimes called acupatches or acu-aids.
Other methods of stimulation include use of moxa (a herb that is burned near or on the skin), sparks from a hand-held device, and microcurrent stimulators, to name a few.
When low-volt electric modalities are used in stimulating acupoints, it is generally believed that a frequency of approximately 5 pulses per second (pps) is ideal for maximal endorphin release. The intensity of current, using a small diameter electrode, should be as high as the patient can comfortably tolerate. Stimulating the most painful trigger point contralateral to the patient's pain (eg, elbow) while the patient moves the involved part has been found effective in rapidly alleviating musculoskeletal pain.
In summary, when acupuncture sites are stimulated by means of low-volt electric current, several factors should be kept in mind:
The exact site of the point or of its contralateral partner must be stimulated.
A small diameter electrode must be used.
The correct frequency must be selected.
The correct duration must be determined.
It should be noted that many of these factors are also important when other methods are used.
Site Location
Acupuncture points are usually tender to the touch and located in palpable depressions under the skin. Although most pertinent sites are usually tender, there are many situations where a lack of normal tenderness at a site may also be diagnostic.
As previously described, recent evidence suggests that acupuncture works by means of an extravascular transport mechanism. This means that the points will be located at a certain depth below the skin surface. Some research studies indicate that stimulation primarily affects the nervi vasorum (autonomic fibers congruent with the blood vessels), and this further lends credence to inserting the needle to a specific depth.
Locating Points
Of prime importance in meridian/trigger point therapy are the proper palpation and localization of the acupoint. But first, a specific definition of a meridian point should be attempted.
Felix Mann states that in all diseases, physical or mental, tender areas are present at certain points on the surface of the body — points that disappear when the illness is cured. He calls these sites acupuncture points. In Chinese literature, we find descriptions of over a thousand of these points. The more common 365 points are located on certain fixed lines or pathways called meridians. It is our opinion that an acupuncture point is, in many instances, identical to the trigger point described by Travell or the concepts described by Matsumoto and Hiyodo in their writings.
In locating important acupoints for treatment and meridian dysfunction, one technique involves systemic palpation (ie, of alarm points) of the body at predetermined sites. These points will be described later in this chapter.
BACKGROUND
The palpating hands of the examiner contain sensitive nerve endings that are quite perceptive to changes in tissue tone, temperature, texture, surface humidity, etc. The fingertips are particularly well supplied with touch and pressure receptors, while the dorsal surface of the hand is especially endowed with heat receptors. For these reasons, both the fingertips and the back of the hand should be used during the evaluation procedure. As examiners gain experience in point location, they will find it increasingly easier to locate critical sites.
Acupoints will often be found that are spontaneously tender. For instance, a patient with appendicitis will point to McBurney’s point as being exquisitely painful. Individuals with headaches often relate a spontaneously tender area on the nuchal line of the occiput. In other cases, areas will be painful only when pressure is applied. Many of the points above the ankles and in the hand and wrist belong to this category. A third type of acupoint is not tender even when moderate pressure is applied. Many acupuncture points are of this type.
PREPARATION
In searching for the acupuncture point, the patient must first be positioned in a comfortable position. The patient should be disrobed in such a fashion that the points are readily accessible to palpation. Care must be taken in all cases to preserve the modesty of the patient. As during the routine physical examination, it is generally best to have the patient undress and then robed in a gown that ties in the back. The waist band of the patient should be loosened for comfort and to afford free access to points of the lumbar, sacral, and lower abdominal areas.
Most examiners find it convenient to begin the examination with the patient seated on a low stool, and then transfer the patient to a comfortable cushioned table for examination in the prone and supine positions. Prior to searching for acupuncture points, the doctor should remove any jewelry that might scratch or irritate a patient. Personal hygiene, as always, is of utmost importance. The examiner’s hands should be thoroughly washed before and after each examination.
TYPES AND CHARACTERISTICS OF ACUPUNCTURE POINTS
Several types of acupuncture points or lesions might be discovered:
Fibrositic nodules. Most commonly, the fibrositic nodule will be the point located. This area feels like a small node or mass of tissue several millimeters in diameter. It will be tender to pressure and often spontaneously painful. It is similar to the fibrositic rheumatoid nodules often located at the back of the neck, in the shoulders, or in the lumbar area.
Indurated areas. In many instances, a hard (indurated) area will be found. Instead of a nodule, the palpator might feel a localized area of tense muscle fibers in a muscle.
Atrophic areas. In other cases, the acupuncture point might be characterized as a localized swollen and discolored area or an atrophied area of tissue.
ELECTRIC ANALYSIS
The examiner might be unable to locate acupuncture points by palpation. In these cases, it may be of value to make use of one of the many electric devices available for their detection. These instruments measure skin resistance to an electric current, showing areas where the resistance is altered. Once a point is localized, whether manually or with an electric device, it should be carefully marked with a skin pencil or felt-tipped pen and then charted in the patient’s records so that a comparison can be made from one visit to another.In Japan, Nakatani mapped out areas of altered skin resistance into pathways that correlate with meridians. He treats the most altered points. This system is called Ryodoraku, [54] which, when translated, means good electroconduction system.
The fact that an acupuncture point exhibits altered electrical resistance allows an examiner to determine specific sites by using any instrument that measures (objectively with an ohmmeter or subjectively by the intensity of the sound made by an instrument) skin resistance at an isolated point. It is presently thought that sites that are reactive (ie, involved in a complaint), especially when we are dealing with a musculoskeletal complaint, are more conductive than surrounding tissue. These points are usually more tender and conduct current more readily (less resistance to an electric current). These points give a higher reading on an ohmmeter and produce a louder sound. Chinese physicians refer to these sites as ah shi (ouch) points; American physicians usually call them as trigger points.
If the correct site is chosen for stimulation, the most common reaction will be hyperemia (histamine reaction) around the point stimulated. Also noted, especially when needles are used, will be a sensation of tingling or numbness radiating or referred distally from the site stimulated. This sensation is called the deqi (also spelled tae chi). [55] A lack of hyperemia or deqi appears to correlate with poor results, thus indicating that the proper site was not treated.
In 1984, studies conducted by Y. M. Sin showed that acupuncture stimulation not only gave good symptomatic relief in inflammatory disease but also suppressed the underlying progress of the disease. [56]
The Human Inch
Besides palpation and measuring electrical resistance, charted acupuncture points can be located by using a topographic system of anatomical measurement. The unit of measure is called the human inch, tsun, or cun, and the system of measurement uses the patient’s own anatomical proportions to establish the parameters to be used in (1) locating points and (2) determining the depth of needle insertion.
The human inch for a particular patient can be determined by measuring the distance between the patient’s two joint creases of the volar surface of the middle phalanx of the middle finger when it is flexed. It can also be determined by measuring the width of the patient’s thumb. Either hand can be used unless one thumb has been deformed by trauma or disease.
Once the human inch is known, various portions of the patient’s body may be measured lengthwise or transversely and that measurement may be divided into a certain number of human inches. Because a human inch is a proportional measurement for a specific individual, the number of cuns on a body part (eg, a forearm or leg) is approximately the same whether the patient is young or old, tall or short, or lean or obese. [55] The only exception to this is where obvious growth, surgical, or pathologic asymmetries are present (eg, disproportionate limb-trunk dwarfism).
Major Points: Locations, Primary Indications, and PrecautionsAs the result of millions of observations of patient responses over several centuries, Oriental physicians have charted over 300 major points on the body and have attributed certain related functions to these locations. As a general rule, however, it is thought that any localized point in an area of musculoskeletal pain can be stimulated to inhibit pain in that location.
In 1984, Peter Eckman, MD, PhD, developed a schematic model of the general effects of acupuncture. [57]
In the following sections, we will attempt to describe the most common sites of stimulation and the indications for treatment as cited by various authorities. We must state unequivocally, however, that little or no scientific verification has been done in the West to substantiate these projected effects. Thus, the reader is cautioned to use every possible diagnostic tool available necessary to evaluate the patient’s complaints and to use this chapter as a reference to those sites used by Oriental physicians. The complete validity of the effects described must await further research substantiation.
The major points on the lung (LU) meridian are LU-1 and LU-7.
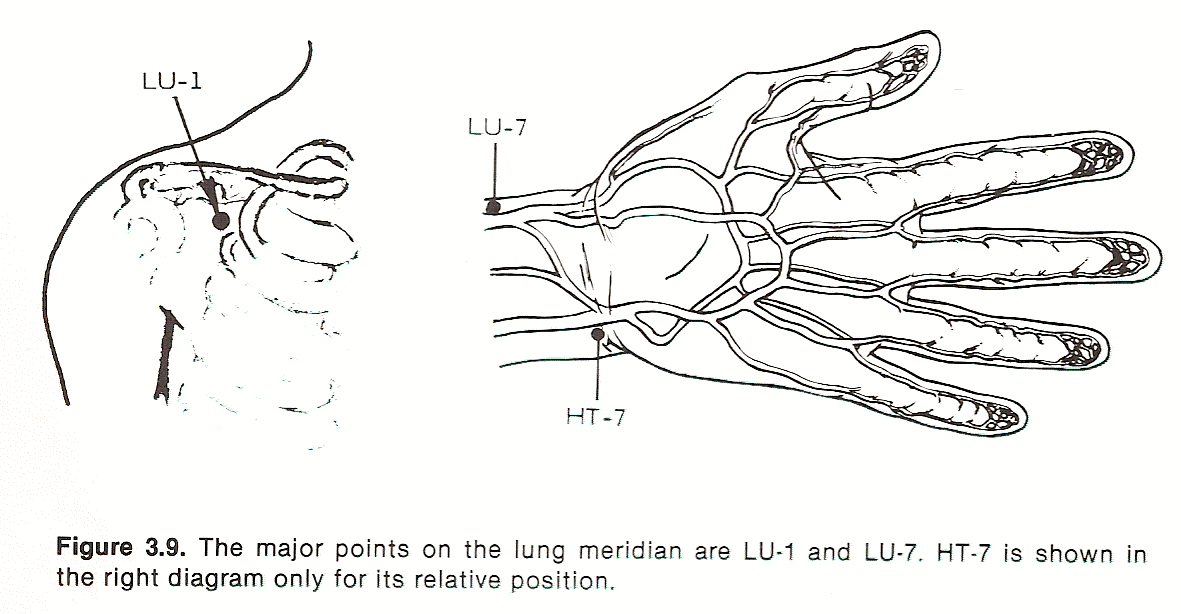
Location. The site of this point (Zhongfu) is found on the anterior lateral aspect of the chest. Using your finger, palpate below the clavicle and seek a tender spot in the space between the first and second rib, approximately 6 cun lateral to the anterior midline of the chest.
Indications. This point is the alarm point for the lung meridian, thus it may be tender in any condition related to the lung meridian. This site is primarily used for chronic respiratory complaints because it is the major point influencing the lungs. Stimulation may also be made at this site for shoulder disorders, especially those exhibiting painful adduction.
Location. This point (Lieque) may be found just lateral to the radial artery at a spot 1.5 cun from the transverse crease on the volar aspect of the wrist, proximal to the styloid process of the radius. A slight depression marks the site of LU-7.
The remainder of this page is only available to
doctors of chiropractic,
and licensed acupuncturists
by purchasing Schafer's text:
Applied Physiotherapy in Chiropractic