

|
General Symptomatology Structural Considerations Selected Clinical Implications Cervical Curve Alterations Cervical Subluxation/Fixation Syndromes Neurologic Effects of Whiplash and Similar Syndromes Neck and Arm Pain of Cervical Origin Selected Thoracic Considerations Structural Considerations Thoracic Subluxation/Fixation Syndromes Thoracic Disc Lesions Spinal Tumors Thoracic Scoliosis Selected Lumbar Considerations The Lumbar Nociceptive Receptor System Mechanical and Chemical Factors of Low Back Pain Neurogenic Low-Back Pain Syndromes Selected Pelvic Considerations Sacroiliac Subluxation/Fixation Syndromes Coccyx Syndromes Pubic Syndromes Neurologic Aspects of Scoliosis BibliographyChapter 7
Specific Potentialities of the Subluxation Complex
From R. C. Schafer, DC, PhD, FICC's best-selling book:
“Basic Principles of Chiropractic Neuroscience”
The following materials are provided as a service to our profession. There is no charge for individuals to copy and file these materials. However, they cannot be sold or used in any group or commercial venture without written permission from ACAPress.
All of Dr. Schafer's books are now available on CDs, with all proceeds being donated
to chiropractic research. Please review the complete list of available books.
General Considerations Innervation of the Spinal Dura Nerve Root Compression/Irritation Axoplasmic Flow Disturbances Cerebrospinal Fluid Flow Alterations Cord Compression Selected Cervical Considerations
Chapter 7: Specific Potentialities of the Subluxation Complex
Studies reported by Drum, Hargrave-Wilson, Kunert, Burke, Gayral/Neuwirth, and others have shown that a subluxation complex, often leading to spondylosis, can effect a wide variety of disturbances that may appear to be disrelated on the surface. Most of the remote effects can be grouped under the general classifications of nerve root neuropathy, basilar venous congestion, cervical autonomic disturbances, CSF pressure and flow disturbances, axoplasmic flow blocks, irritation of the recurrent meningeal nerve, the Barre-Lieou syndrome, and/or the vertebral artery syndrome.
Cervical Dura Attachments
In describing the relationship of structural pathology to the nerve root, Kirkaldy-Willis takes a broader view. He states that the nerves of the lumbar spine may be entrapped:
(1) at the back of the IVD,
Changes at these sites can produce dysfunction, disc herniation, instability, lateral entrapment, central stenosis. However, he does state that the pain from a disc lesion or stenosis may come from irritation and inflammation of the dura. The motor loss in these lesions may be attributable a reflex inhibition and vascular insufficiency rather than from nerve compression.
Foraminal Encroachment
Subarticular Entrapment
It has been known for several years that much of the protein synthesized within a nerve cell body moves, along with other materials such as neurotransmitters, from the cell body and along the nerve fiber (anterograde material transport system). Two mechanisms have been isolated, and they are characterized by their fast (410–50 mm/day) and slow (1–3 mm/day) rates, regardless of their fiber size. Guth initially recognized this total system for transporting the "trophic" substances normally carried by efferent nerves. It is also recognized that there is a retrograde flow of materials; ie, from terminals toward the nerve cell body.
(1) nerve roots are highly susceptible to compression, spinal nerves are not;
Indirect injury to the cord may be caused by the rupture of tissues of the spine by violent forces such as falls, crushes, or blows. This type of injury, which is normally closed with respect to the spinal column and cord, is of a lesser degree than direct injury. It takes the form of concussion, hemorrhage, or edema of the cord. The cord may cease to function below the site at which the force was applied even if the cord itself received no direct injury. Such dysfunction may be temporary or long standing, thus the prognosis must be guarded. Injuries to the spinal column in which the cerebrospinal fluid is rapidly depleted may be fatal. Direct injury to the cord, the nerve roots, or both may be caused by impact forces or shattered bone fragments. The cord may be bruised, compressed, crushed, pierced, or cut. An open wound is often involved.
The tissues of the posterior neck normally provide stability and support for the cranium, a flexible and protective spine for movement, balance adaptation, and housing for the spinal cord and vertebral artery. From a broad viewpoint, primary cervical subluxation syndromes may reflect themselves in the total habitus; from a neurologic viewpoint, insults may manifest throughout the motor, sensory, and autonomic nervous systems. Unlike the lumbar region, cervical disc herniations are not frequently associated with severe trauma; however, traumatic nerve root or cord compression has a high incidence in this area.
This chapter describes the primary neurologic implications of subluxation syndromes, either as a primary factor or secondary to trauma or pathology, within the cervical spine, thoracic spine, lumbar spine, and pelvic articulations.
GENERAL CONSIDERATIONS
This chapter describes many causes for and effects of a spinal subluxation complex. In clinical practice, however, causes and effects are rarely found as isolated entities. Several factors will usually be involved and superimposed on each other.
Innervation of the Spinal Dura
It has long been known that the spinal dura mater has an intrinsic nerve supply. Spinal meningeal rami are derived from gray communicating rami and spinal nerves. The spinal nerves contribute sensory fibers to the meningeal rami. Several meningeal rami enter each IVF, and most are located anteriorly to the sensory ganglia within the IVF.
Bridge found that these intrinsic nerve fibers reach the anterior surface of the dura by three main courses. Here the nerves divide into ascending and usually longer descending filaments that run longitudinally and parallel on the dural surface, and a considerable amount of nerve overlaps from adjacent segments. Finer filaments penetrate the dural substance where they subdivide.
Kimmel reported that most of these fibers penetrate the dura near the midline, while others enter laterally near the exiting spinal nerve roots. At each segment level, two or three nerves enter the spinal dura mater and contain only small nerve fibers. In contrast, Edgar/Nundy could determine no definitive nerve endings, but the nerves could be traced to the posterior aspect of the spinal dura. These observations help to clarify the wide distribution of back pain that is often found following protrusion of a single IVD.
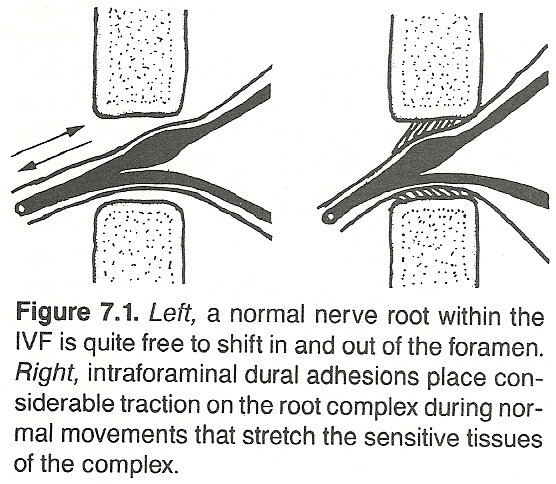
Sunderland states that the nerve sheaths in the cervical region are not firmly attached to their respective foramina. Only the C4 C6 cervical nerves have a strong attachment to the vertebral column, and this is to the gutter of the vertebral transverse process. He believes that these observations have relevance to any local lesion that may fix, deform, or otherwise affect the nerve and its roots to the point of interfering with their function, and they also may be important to traction injuries of nerve roots.
Painful Irritations
The sympathetic nervous system, in conjunction with a sensory root compression or independently, plays a role in the interpretation of pain. Compression of the recurrent meningeal branch of the spinal nerves, for example, results in a wider distribution of pain and muscle spasm than the local pathology may indicate.
Many authorities attribute most lumbosciatic pains to IVD faults. The typical disc lesion is thought to produce restrictions in the dura mater during straight-leg-raising or neck flexion tests.
Cyriax believes that lumbago does not arise from tissue that has undergone degeneration (eg, myofibrosis) because the incidence of backache falls by two-thirds between the ages of 60 and 70 and has almost ceased by the age of 80. He attributes the pain to the impingement of discoid material on the dura mater or its root sleeve. He feels that the syndrome is initiated by an attack of internal derangement at a low lumbar IVD as the result of a momentary posterior displacement of a movable piece of intra-articular fibrocartilage. The prolonged subsequent pain is believed to be caused entirely by bruising of the dura mater.
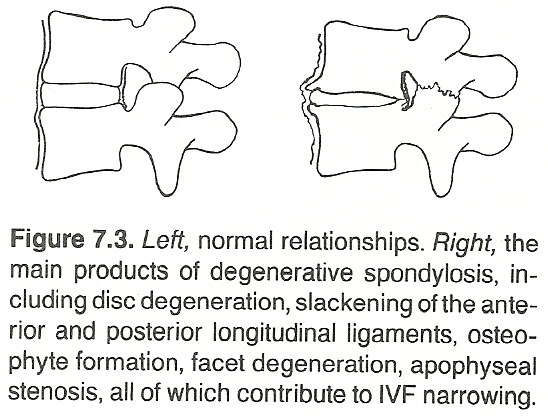
(2) laterally in the central canal,
(3) in the cauda equina,
(4) more laterally in the nerve canal, and
(5) posteriorly in the zygapophyseal joints.
Nerve Root Compression/Irritation
It has long been held within chiropractic that many effects of a subluxation syndrome can be attributed to nerve root compression. Sharpless, Luttges, Sunderland, Pleasure, Schaumber/Spencer, and several others in recent years have contributed greatly to our understanding of the phenomena involved.
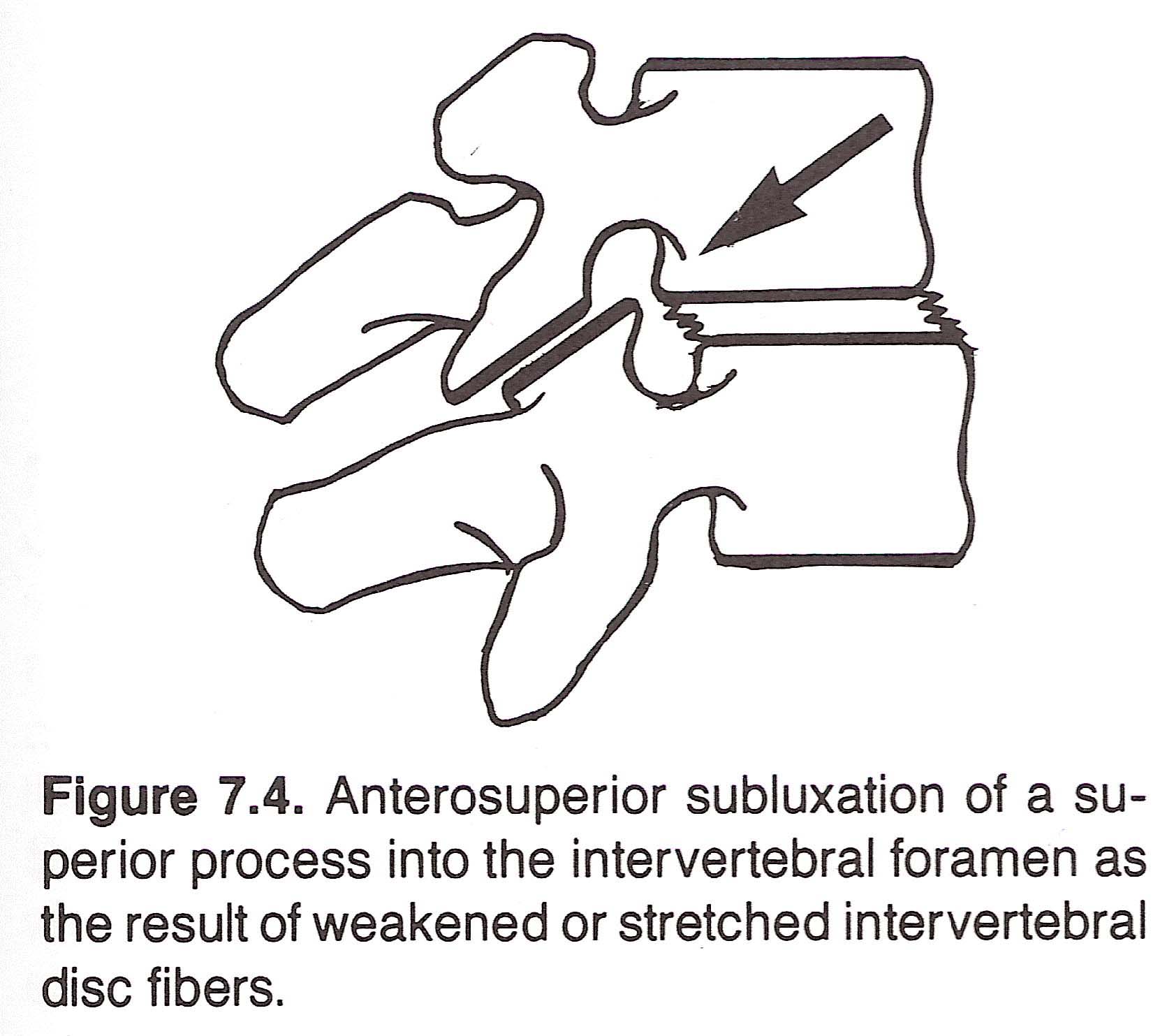
During their exit from the IVFs, the nerve roots course close to the inner edge of the superior facet. In subluxation, the superior process can override the surface of the inferior process and produce direct irritation of the root by the inferior process, with or without compression. (See Figure 7.4) Direct compression also can result by the root being caught between the inferior process and the body of the superior vertebra or caught between a hypertrophied inferior process and the superior body. Olsson and coworkers, however, reported that mechanical pressure on a root is more often from the formation of edema within the nerve sheaths and epineurium, regardless of cause.
Many years ago, Oppenheimer, Hadley, and others noted that many patients suffering from pain and discomfort suggestive of rheumatism or arthritis were the result of nerve root compression arising from narrowing of the IVF. They explained that the primary causes were discogenic disease, inflammatory swelling, and penetration by an articular process.
Sunderland points out that IVF narrowing results from normal extension or any number of pathologic changes in and about the foramen that would reduce its dimensions or lead to nerve compression. Thus, the same effect would be achieved in a subluxation fixed in extension or in some other manner causing IVF narrowing.
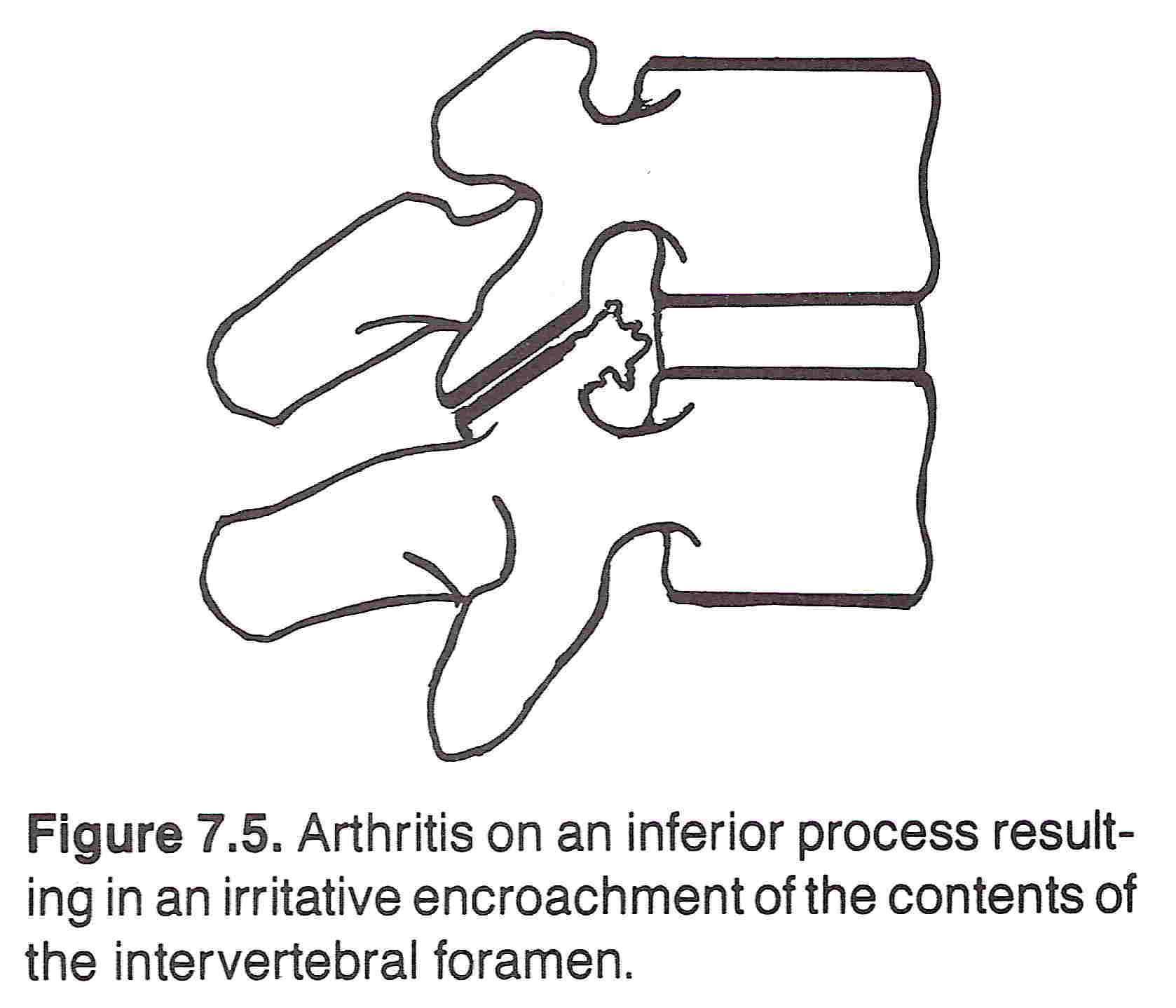
This type of compression usually occurs from arthritic hypertrophy of an articular facet. (See Figure 7.5) It is an occurrence often associated with advanced spondylosis. The bony mass often compresses the nerve root lying beneath the medial border of the superior articular facet. The root is caught between the posterior aspect of the vertebral body and the facet. Besides somatic sensory and motor manifestations, hearing, visual, and equilibrium disturbances may be associated, according to Pang, Chrisman/Gervais, Davis, and others.
Pedicular Kinking
This condition is associated with chronic IVD degeneration where the disc space is quite thin and the vertebral bodies approximate each other asymmetrically because of lateral disc collapse or a laterally tilted vertebral body (eg, scoliosis). As the superior vertebral body descends, it may impose its pedicle on the exiting nerve root. Macnab feels that the most common mechanism is that the nerve root becomes entrapped in the gutter formed by a wide lateral protrusion of the disc and the superior pedicle.
Axial Compression
Axial compression from the upright position is never a problem with a healthy, well-hydrated disc. If the disc space narrows considerably, the spinal canal can be narrowed in the midline by several mechanisms. Typically, these include posterior subluxation of the superior vertebra, anterior subluxation of the inferior vertebra, a diffuse posterior anular protrusion or rupture, kinking of the ligamentum flavum, thickened capsules from laminae shingling, arthritic hypertrophy of the superior processes, or a combination of these factors.
It should be kept in mind, however, that the IVF is usually quite roomy. There can be complete disc collapse without any degree of compression. Also, there can be considerable compression on a root without any overt signs of malfunction if the pressure develops slowly and adaptation is sufficient. Entrapment, from whatever cause, can be encouraged by a transforaminal ligament, an adhesion, or an overgrowth restricting the normal mobility of the root in the IVF.
Spinal Canal Stenosis
Spinal stenosis often produces a bony root entrapment syndrome. Narrowing of the spinal canal can occur either laterally or in the midline of the canal. If it occurs laterally, compression of the nerve roots can result from foraminal impingement (ie, subluxation), pedicular kinking, or subarticular entrapment. If it occurs in the midline, compression of the cord or cauda equina may result.
Major Effects of Spinal-Level Nerve Compression
Spinal nerve pressure or irritation may manifest as sensory, motor, autonomic, or combined signs and symptoms. Initial results are often interacting. In studying the effects at injured and compressed nerves, Granit and associates found that nerve impulses set up in a motor root are transmitted to the sensory fibers in a cut or compressed region of the nerve and can be picked up in the sensory root of the same segment.
Causey/Palmer concluded that, in acute experiments, the failure to conduct an impulse after local pressure is applied to a nerve was caused by local anoxia. Rydevik found that this was true but also found that biomechanical nerve root deformation was also a factor in inducing motor weakness and altered sensibilities.
Axoplasmic Flow Disturbances
Most pathologists agree that it takes much more than an invasion of a pathogenic organism to cause an infectious disease: an inadequate tissue resistance is also necessary for the invading organism to survive and multiply. The idea of "improving natural resistance to disease" was at the foundation of many pioneer chiropractic concepts.
Whereas allopathy has traditionally emphasized the virulence of the invader, chiropractic has emphasized the resistance of the host. During pioneer chiropractic, this hypothesis was based primarily on empiric findings, which were later substantiated considerably by the studies of Zhigalina, Gondienko, Selye, and Speransky that were described in Chapter 2. Studies on the effects of axoplasmic flow interruption have added even greater validity to the chiropractic approach.
The Neuronal Transport System
In recent years, Ochs, Korr, Fernandez, Rainer, Sjostrand, and several other researchers have found that any type of neuronal constriction, compression, or ischemia will cause a local transport block and an accumulation (damming) of the fluid proximal to the restriction. Weiss had earlier described this as a form of persistent endoneurial edema found just proximal to a compressed area.
Pressures successful in blocking axoplasmic flow are far below those necessary to block nerve conduction. It has been hypothesized that some effects previously attributed to nerve root compression (eg, from vertebral subluxation) may be effects from interference with normal axoplasmic flow.
Current Research Findings
Current research supports three important facts:
(2) nerve roots become highly vulnerable to IVF compression when the roots are subjected to traction and the IVF is narrowed;
(3) spinal nerves, while not highly susceptible to compression, are highly susceptible to axoplasmic transport block.
Cerebrospinal Fluid Flow Alterations
Stagnant or altered CSF flow has an adverse influence on the CNS. Freedman states that biomechanical aberrations of the spinal column may adversely affect CSF flow and CNS function. It is thought that this factor may be a common physiologic denominator within various (although seemingly different but often equally effective) chiropractic adjustment techniques.
Spinal Nerve Flow
In 1968, Steer/Horney answered the question whether CSF passes peripherally from the spinal cord to spinal nerves. To test the possibility, blue powder suspended in CSF was introduced into the lumbar subarachnoid space of pigs and sheep. Nerves and other tissues were examined 4–21 days later. Particles were found widely distributed; eg, in the brachial and lumbosacral plexuses, thoracic nerves and muscles, skin, and the jugular vein.
Occipital Subluxation Effects
Almost any situation that would cause constriction in the connecting area between the cerebral subarachnoid space and the vertebral canal can limit the escape of CSF into the inferior vertebral canal. This results in a degree of increased intracranial pressure. An atlanto-occipital subluxation may cause the dura mater of the cisterna cerebellaris to be pressed against the posterior medullary velum and partially occlude the foramina of Luschka and Magendie and interfere with the flow from the 4th ventricle. The resulting increase of intraventricular fluid accumulation may create a large variety of symptoms such as deep-seated, stubborn, "internal pressure" headaches; nausea; a tendency toward projectile vomiting; bizarre and unusual visual disturbances; and protopathic ataxias.
Lower Spinal Subluxation Effects
Disorders classified under the category of CSF flow alterations refer to the mechanical effect upon the flow of CSF within the CNS and perhaps within the peripheral nerves themselves. Stagnation possibly occurs in association because of the intimate relationship between spinal fluid and venoid blood, contributing to toxicity in the nerve root area. According to some researchers, minute pressure on meninges can alter the flow of CSF and interfere with the system's ability to remove wastes and provide nutritional substances to the cord and related nerves. This may be either the result of direct mechanical pressure or impairment of motion necessary for proper inflow and outflow of this nutrient material.
Cord Compression
Most spinal cord injuries are caused by extreme flexion in which subluxation, fracture, and/or dislocation are co-associated. It is not unusual for what appears initially to be a severe posttraumatic subluxation syndrome to be complicated by a spinal fracture/dislocation. Initial signs are often misleading. Hemorrhage may occur at the site with the same reaction as brain injury (liquefaction, softening, disintegration). Congenital fusions and stenosis may predispose to spinal cord trauma during strenuous activity.
Primary Types
There are direct and indirect classes of spinal cord injuries:
If the cervical cord is injured, there is loss of sensation and flaccid paralysis. The lower limbs exhibit a spastic paralysis. If the space in which the spinal fluid flows between the spinal cord and the surrounding vertebral column is either compressed or enlarged, severe headache occurs. Posttraumatic penile erection strongly suggests either cervical or thoracic cord injury.
Nontraumatic Types
Cord compression may also be the result of chronic subluxation, spondylosis, osteophytes, longitudinal ligament thickening or buckling, or tumor development.
SELECTED CERVICAL CONSIDERATIONS
Valentini, Fitz-Ritson, Cole, Seeman, Mears, and others have shown that nowhere in the spine is the relationship between the osseous structures and the surrounding neurologic and vascular beds as intimate or subject to disturbance as it is in the cervical region. The effects of local subluxation may express themselves upward within the brain stem and downward to the lumbar spine and pelvis. Many peripheral nerve symptoms in the shoulder, arm, and hand will find their origin in the brachial plexus.
General Symptomatology
Local and remote effects of cervical subluxation are shown in Table 7.1.
Table 7.1. Local and Remote Features of Cervical Subluxation
Articular grating Ataxia Atypical facial pains Blurred vision Cold sweats Deafness Diplopia Drop attacks Dysarthria Dysequilibrium Nausea Dysphagia Dysphonia Epileptiform attacks Fatigue Giddiness | Headaches Horner's syndrome Indigestion Irritability Lermoyez's syndrome Memory faults Meniere's syndrome Mental confusion Neuralgia Neck pain Numbness Nystagmus Pallor Paresis | Poor concentration Precordial discomfort Pseudoangina Psychiatric disturbances Retro-orbital pain Stiffness (neck) Tenderness Tension Tinnitus Tonsillitis Upper extremity coolness, pain, and/or altered reflexes Vertigo Vomiting |
Structural Considerations
 |
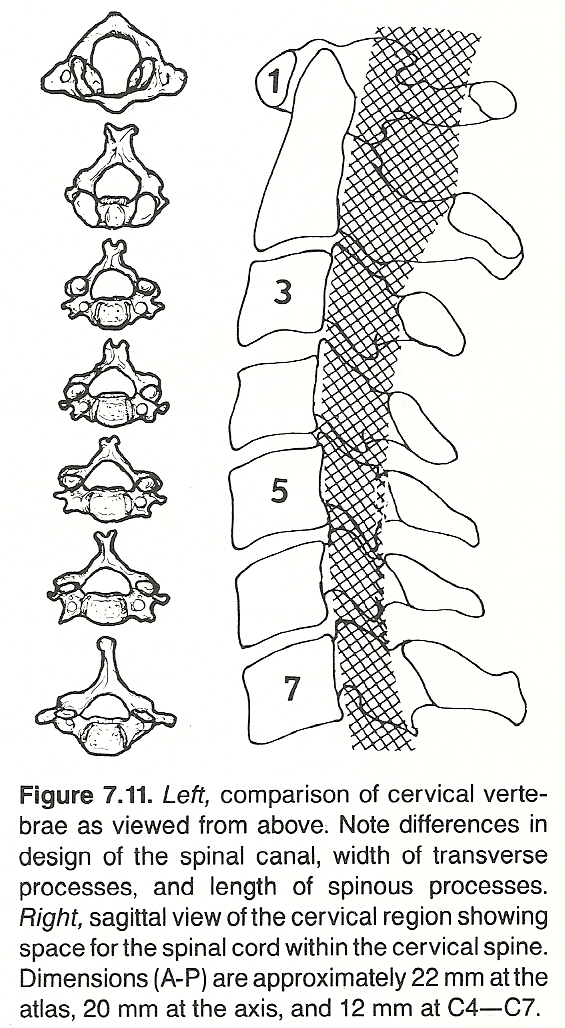
The highly mobile cervical spine is unique in that it must provide flexibility and yet protect highly complex neurologic centers within; ie, the lower portion of the medulla oblongata and that portion of the spinal cord which emits the cervical and brachial plexus. The tips of the cervical spinous processes normally correspond to the level of the succeeding cord segment; eg, the C5 spinous process is on a level with the C6 segment of the cord.
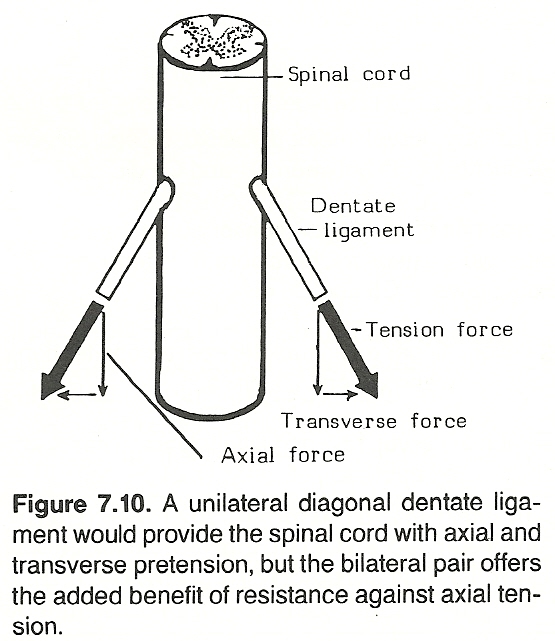
The Cervical Cord Suspension System
The spinal cord is tethered within the dura by the dentate ligaments. Grieve points out that the upper dentates are the strongest and are attached to the dura inside the posterior cranial fossa, behind the canal for the 12th cranial nerve. Because these intraspinal ligaments, which are under tension, project inferiorly and the nerve roots are angled superiorly, the tensile forces on the cord are balanced during spinal motion. This allows the cord to maintain its central position within the vertebral canal — a position which provides maximum protection. Further protection is provided by cerebrospinal fluid, epidural and extradural fat, and the longitudinal ligaments of the canal.
Nerve Root Attachments
It was described earlier that the nerve roots' sleeves of dura and related arachnoid tissue within the cervical canal are loosely attached to the cervical IVFs. These attachments increase in strength during degenerative processes and with advancing age. The lower roots (C4 C7) are firmly attached in the gutter of the transverse process by the epineurial sheath, extensions from the prevertebral fascia, and other connective-tissue fibers of the area.
The segmental functions of the cervical nerves are shown in Table 7.3. Subluxation syndromes and traumatic traction involving the cervical and brachial plexuses will be described later in this chapter.
Cervical Spinal Receptors
 |
The abundant proprioceptors of the vertebral column enable the brain to know where each segment is and what it is doing at any given time without visual confirmation. The apophyseal joints of the cervical spine, especially their capsules, are richly innervated with mechanoreceptors and afferent fibers endowed more than any other spinal region. Activity from the cervical articular receptors exerts significant facilitatory and inhibitory reflex effects on the muscles of the neck and both the upper and lower extremities.
Wyke believes that the patterns of "normal cervical articular mechanoreceptor reflexes are profoundly distorted when cervical articular nociceptive afferent activity is added to that derived from the normally functioning cervical mechanoreceptors." To underscore this point, he states that:
(1) manipulation of the head on the neck can produce coordinated flexion and extension movements on the paralyzed arm and leg of a hemiplegic patient,
(2) arm movement control without visual aid is considerably affected by rotation of the head, and
(3) induced unilateral local anesthesia of the cervical joints in healthy subjects produces severe postural instability, dizziness, nystagmus, and muscular incoordination. These signs and symptoms are similar to those experienced by some patients who suffer from cervical spondylosis, ankylosing spondylitis, and gross fixations, and some while wearing an orthopedic cervical collar.
Lieb shows several full-spine radiographs of severe spinal distortions that have been greatly improved through correction of dental occlusion. If the temporomandibular joint has such a proprioceptive influence upon spinal posture, it is no wonder that chiropractors who specialize in upper-cervical or sacral correction can exhibit an abundance of before-and-after films because each spinal segment is richly endowed with an equal or greater number of receptors than those of the joint of the jaw.
Cervical Righting Mechanisms
Several extensors of the neck arise from the lower cervical and upper thoracic vertebrae and exert an oblique posteroinferior pull on the occiput. If this line of pull falls behind the atlanto-occipital joint, a rotary movement results that tilts the occiput posteriorly and lifts the face so that the neck is hyperextended. However, if this posterior rotation of the head is inhibited by the cervical flexors (which is normal), the oblique pull tends to have a posterior translatory component when the head is anterior to the midline. This serves to bring the head back toward the vertical gravity line and into better alignment.
The longus group, in addition, exerts a bowstring action on the anterior cervical segments, which assists in axial extension of the neck. Thus, the extensors serve to return the head to the midline following flexion, but axial extension is completed by a straightening of the cervical lordosis produced by segmental flexion. If this segmental flexion did not occur during extension, the head would rest in the neutral position facing superiorly. Simultaneously, the thoracic extensors tend to straighten the dorsal curve so that the alignment of the entire cervicothoracic region is improved.
Chronic flexion of the lower cervicals tends to produce elongation of the upper posterior thoracic soft tissues and adaptive shortening of the anterior elements (eg, anterior longitudinal ligament, anterior disc anulus, pectorals, intercostals). This is often seen in aging where it is contributed to by degeneration of the normally elastic ligamentum nuchae, which helps to resist anterior deviation of the head. If this chronic flexion state occurs, cervical extension to the midline following flexion is fairly limited to increasing the cervical lordosis with little axial extension of the neck by segmental flexion. The neck angles forward, and the jaw juts out as the occiput rolls backward.
The Cervical Challenge. Goodheart reports that "challenging" vertebral position during spinal analysis provides a precise method of localizing a subluxation complex so that a specific adjustment may be made. He has found that light pressure (5 8 lbs) directed into a cervical lesion will cause an increase in strength of a previously weakened muscle and pressure in the opposite direction will produce weakness in the same muscle. It is theorized that when a subluxated facet is pushed farther out of alignment, the righting reflex of the body will temporarily pull this lesion back into position, and vice versa, in an attempt to maintain structural homeostasis. The direction of correction is then said to be toward the side that produces weakness during evaluation.
The function and innervation of the major muscles of the neck are shown in Table 7.2.
| Muscle | Major Function | |
| Erector spinae, upper | Extension, rotation | |
| Longus capitis | Flexion | |
| Longus colli | Flexion | |
| Rectus capitis anterior | Flexion | |
| Rectus capitis lateral | Flexion | |
| Scalenes | Flexion, rotation | |
| Semispinalis capitis | Extension, rotation | |
| Semispinalis cervicis | Extension, rotation | |
| Splenius capitis | Extension, rotation | |
| Splenius cervicis | Extension, rotation | |
| Sternocleidomastoid | Flexion, rotation | |
| Trapezius, upper | Extension, rotatiomn |
| Segment | Function |
| CERVICAL PLEXUS (C1–C4) | |
| Motor to head and neck extensors, infrahyoid, rectus capitis anterior and lateral, and longus capitis. | |
| Sensory to lateral occiput and submandibular area; motor, same as C1 plus longus colli. | |
| Sensory to lateral occiput and lateral neck, overlapping C2 area; motor to head and neck extensors, infrahyoid, longus capitis, longus colli, levator scapulae, scaleni, and trapezius. | |
| Sensory to lower lateral neck and medial shoulder area; motor to head and neck extensors, longus coli, levator scapulae, scaleni, trapezius, and diaphragm. | |
| BRACHIAL PLEXUS (C5–T1) | |
| Sensory to clavicle level and lateral arm (axillary nerve); motor to Deltoid, biceps; biceps tendon reflex. Primary root in shoulder abduction, exits between C4 and C5 discs. | |
| Sensory to lateral forearm, thumb, index and half of 2nd finger (sensory branches of musculocutaneous nerve); motor to biceps, wrist extensors; brachioradialis tendon reflex. Primary root in wrist extension, exits between C5 and C6 discs. | |
| Sensory to second finger; motor to wrist flexors, finger extensors, triceps; triceps tendon reflex. Primary root in finger extension, exits between C6 and C7 discs. | |
| Sensory to medial forearm (medial antebrachial nerve), ring and little fingers (ulnar nerve); motor to finger flexors, interossei; no reflex applicable. Primary root in finger flexion, exits between C7 and T1 discs. | |
| Sensory to medial arm (medial brachial cutaneous nerve); motor to interossei; no reflex applicable. Primary root in finger abduction, exits between T1 and T2 discs. | |
Dynamics of the Cervical Cord
 |
Breig has shown that the length of the spinal canal shortens during extension and lengthens during flexion (forward and lateral). Thus, the spinal cord must do likewise to avoid injury during flexion. This is accomplished because the cord is pleated in an accordion-like fashion during rest and unfolds during any lengthening process.
Changes During Rotation and Lateral Flexion. The ipsilateral anterior roots relax and the dorsal roots become taut during rotation. During lateral flexion, the IVFs narrow in height ipsilaterally and elongate contralaterally. Undue tension can be placed on the contralateral dentate bands and IVF contents, and compressive forces can be applied to the contents of the ipsilateral IVF. This is especially true if degenerative changes have occurred.
Changes During Flexion. During flexion, the slack in the cord and its neurons, the dura, and the roots progresses to tension. Because the cord is attached to the coccyx, any tension arising in the cervical area will be transmitted as far caudally as the lower sacral roots. Breig/Turnbull/Hassler report that the cross-section of the cord increases or decreases, as an elastic bar, whenever the cord respectively shortens or lengthens.
Although the spinal cord has a high stretch coefficient when tension is applied slowly, Goddard/Reid found that elastic deformation is only necessary at the extremes of spinal motion. Only about 2 or 3 mm of segment-level movement occurs in the cervical spine. The meninges, which have more white fibers than elastic fibers, are not as elastic. They become taut when their length approaches a 5% increase.
While the cord and dura are both under tension during spinal motion, according to Penning, that of the dura is from its structural properties and extradural attachments plus root tension, and that of the cord is from the rubber-like dentate bands. This process also mandates that any tension applied to the cord will be rapidly transmitted to the dura and roots, and vice versa.
Changes During Extension. The spinal cord and the roots slacken during extension and slightly gravitate because of gravitational pull, according to Reid. The "free space" of the canal is decreased by three factors during extension:(1) posterior bulging of the IVD,
(2) buckling of the relaxed dura, and
(3) anterior bulging of the ligamentum flavum.
Selected Clinical Implications
The same tension mechanisms occurring in the cord, dura, and roots during normal physiologic flexion are thought to occur chronically in the relaxed state when the cervical curve or a single motion unit is hypolordotic. In addition, it has been Brodal's experience that normal consequences will be compounded whenever a stretched (bow-string) cord is applied against any space-occupying lesion (spondylotic ridge, IVD protrusion, tumor). In time, this will result in actual flattening of the cord at this point and ischemic degeneration from pressure on the anterior spinal artery, the radicular arteries, and/or their capillary beds. Such findings have been reported by Fried and associates, Hoff, and Brieg. Likewise, it can be projected that the same factors which narrow the canal during normal extension will occur chronically in the relaxed state when the cervical curve or a single motion unit is hyperlordotic.
Nerve function of the cervical and brachial plexuses is shown in Table 7.4.
| Nerve | Function |
| Nerve Function of the Cervical Plexus (C1–C4) | |
| Lesser occipital | Sensory to skin behind ear and mastoid process. |
| Greater auricular | Sensory to skin over parotid, jaw angle, ear lobe, and front of mastoid process. |
| Cervical cutaneous | Sensory to skin over anterolateral portion of neck. |
| Supraclaviculars | Sensory to skin over medial infraclavicular area, pectoralis major and deltoid. |
| Muscular branches | Motor to capitis anterior and lateralis, longus capitis, longus colli, hyoid muscles, sternocleidomastoideus, trapezius, levator scapulae, scalenus medius. |
| Phrenic | Sensory to costal and mediastinal pleura and pericardium. Motor to diaphragm. |
| Nerve Function of the Brachial Plexus (C5–T1) | |
| Nerve | Function |
| Radial | Motor for wrist and thumb extension; sensory to dorsal web space between thumb and index finger. |
| Ulnar | Motor for little finger abduction; sensory to distal ulnar aspect of little finger. |
| Median | Motor for thumb opposition and abduction; sensory to distal radial aspect of index finger. |
| Axillary | Motor to deltoid muscle; sensory to lateral arm and deltoid patch on upper arm. |
| Musculocutaneous | Motor to biceps muscle; sensory to lateral forearm. |
Cervical Nerve Root Insults
Disturbances of nerve function associated with subluxation syndromes basically manifest as abnormalities in sensory interpretations and/or motor activities. These disturbances may be through one of two primary mechanisms: direct nerve or nerve root disorders, or of a reflex nature.
Sensory Changes. When direct nerve root involvement occurs on the posterior root of a specific neuromere, it manifests as an increase or decrease in sensitivity over the dermatome. A typical example includes foraminal occlusion or irritating factors exhibited clinically as hyperesthesia, particularly on the dorsal and lateral aspects of the thumb and radial side of the hand, when involvement occurs between C5 and C6.
Another example is on the dorsum of the hand, the index and middle fingers, and the anteroradial side of the forearm, thumb, index and middle fingers, when involvement occurs between C6 and C7. In other instances, this nerve root involvement may cause hypertonicity and the sensation of deep pain in the musculature supplied by the neuromere. For example, in C6 involvement, there is deep pain in the biceps; or in C7 involvement, there is deep pain in the triceps and supinators of the forearm. Direct pressure near the nerve root or along its distribution may be particularly painful.
Motor Changes. Nerve root insults from subluxations or trauma also may be evident as disturbances in motor reflexes and/or muscular strength. Examples of these reflexes include the tendon reflexes such as seen in the reduced biceps reflex when involvement occurs between C5 and C6; or the reduced triceps reflex when involvement occurs between C6 and C7. These reflexes must also be compared bilaterally to judge whether hyporeflexia is unilateral. Unilateral hyperreflexia is pathognomonic of an upper motor neuron lesion. Prolonged and/or severe nerve root irritation also may produce evidence of trophic changes in the tissues supplied.
Underlying Factors. The common subluxation picture is rarely pure. It is often superimposed upon other manifest and subclinical processes in the mature patient such as vertebral instability, osteochondrophytic ridges at the uncovertebral joints, apophyseal thickening and exostosis, or canal encroachment by a buckling ligamentum flavum, spinal stenosis, posterior vertebral body spurs, disc protrusions, dura and dentate thickening, arachnoid cysts, dura and arachnoid adhesions, and ossification of the posterior longitudinal ligament.
Loss of disc space, especially in the lower cervical area, may contribute as a source of chronic irritation to an already inflamed root by altering the angulation of the IVF tunnel. The sequence of inflammation, granulation, fibrosis, adhesion formation, and nerve root stricture may follow, along with a loss in root mobility and elasticity. These degenerative changes are not as pronounced during youth.
Upper Cervical Trauma
A severely stressful movement of the cervical spine may result in unconsciousness and possible death if the spinal cord is damaged. The cause may be fracture or dislocation that injures the spinal cord, often fatally if it occurs within the upper cervical area. Even mild spinal cord trauma may result in sensory and motor paralysis.
Neck hyperextension injuries may cause compression injury to the vertebral arteries causing a temporary oxygen loss to the brain that may result in unconsciousness, if not greater damage through rupture. Less severe disturbances in this area often arise from muscular spasm of one or more of the six muscle bundles that have attachments on the occiput, atlas, or axis. Unequal tension and ultimate fibrotic changes within the paravertebral structures can readily involve the delicate nerve fibers and vascular flow.
A study of most clinical subluxations will reveal that they are infrequently "unusual" positions. They are often normal positions in a state of fixation. In the neutral position, for example, an inferior atlas subluxation-fixation exhibits the posterior arch of the atlas approximating the spinous process of the axis the normal position of the atlas during extension. The same is true of superior, posterior, and lateral listings: all are normal positions if found in flexion, rotation, or lateral bending, but abnormal if found in other positions.
In a discussion of spinal motion of any region or segment complex, it should be kept in mind that minor pathologic changes and individual variances from the "norm" considerably alter the biodynamics that lead to the neurologic insults involved. Neither static position on roentgenography nor dynamic palpation alone or combined can be used as the basis to determine the need or the results of adjustive therapy. Static palpation is often grossly in error because of the many anomalies in asymmetry found in the typical spine. The whole clinical picture must be utilized.
Lower Cervical Trauma
The nerve root is anterior and inferior to the facets in the cervical spine. If subluxation of a vertebra occurs in a superior direction, the contents of the IVF become stretched because elongating and narrowing the vertical diameter of the IVF will cause traction upon the nerve trunk plus compression against the anterior portion of the foramen. If there is subluxation in an inferior direction, shortening and widening of the foramen occurs.
Because the nerve sheath is often firmly anchored by tissues connecting it to the borders of the foramen in the adult, an overstretch is exerted on the nerve sheath whenever its shape is altered. It thus can be recognized that enlarging the IVF can cause as much trouble as a reduction in the size of the IVF. Also, it is impossible to subluxate a vertebra between C2 and L5 without changing the shape of its IVD in compensation.
Cervical fractures and dislocations concomitant with a subluxation syndrome are not common except in the elderly where a degree of osteoporosis is evident. In the young, they are usually the result of severe trauma. Signs of paravertebral tenderness, limitation in movement, muscle spasm, and neurologic deficit should be sought.
As in upper-cervical damage, emergency management is necessary to avoid paralysis and death. Fracture and/or dislocation of any cervical vertebra require hospitalization for reduction, bone traction, and casting. Keep in mind that overdiagnosing instability of the C2–C3 interface is a common pitfall.
Effects of Pathologic Changes on the Cord
Several factors may produce cord compression (static or dynamic) or reduce cord flexibility (increasing cord tension) besides fracture and dislocation. Some common examples are space-occupying lesions (eg, tumor, hemorrhage, edema), central stenosis, IVD protrusion, end-plate fracture, ligamentous hypertrophy, soft-tissue sclerosis, CSF disorders, root-sleeve fibrosis or swelling, ischemia consequences, glial scars from demyelinating disease, and postinflammatory adhesions. But, according to Kapandji, the most common cause is osteophytes extending from the uncovertebral joints.
Breig feels that it is increased cord tension (regardless of cause) and its histologic and microcirculatory effects that produce conductivity and circulatory impairment. He states that these disorders account for most motor, sensory, and autonomic dysfunctions associated with cervical cord syndromes.
Cervical Curve Alterations
Cervical Scoliosis
Cervical scoliosis is often mechanically predisposed by flattening rather than exaggeration of the cervical lordosis. This is especially common during youth. The posterior joints become lax during flattening of the cervical spine, and this encourages retropositioning and posterior subluxations that are frequently the first step toward cervical scoliosis.
In typical rotary cervical scoliosis, the spinous processes tend to rotate toward the convex side of the lateral curve, the vertebral bodies rotate toward the concave side, and the discs and articular facets become subjected to abnormal stretching forces as they open on the side of convexity and to compressive forces on the side of concavity. This type of cervical scoliosis is usually compensatory to a lower scoliosis to the other side and a common cause of recurring episodes of nontraumatic torticollis.
When a cervical disc is loaded unilaterally, the disc initially becomes wedge-shaped. This vertically stretches the anular fibers that are opposite the weight-bearing side, but this action is quickly counteracted by forces transmitted laterally from the resilient nucleus to help the disc return to its normal shape. This self-stabilization factor is the product of a healthy nucleus and anulus working as a mechanical couple.
Cervical scoliotic rotation is also associated with a lateral tilt that increases the distance between the lateral margins of the vertebral bodies on the convex side of the curve. This stretches the lateral anulus, which produces a contraction of that part of the disc and a compensatory bulging of its contralateral (thinned) aspect. If the anular filaments become stretched and weakened, losing some of their stiffness property, the nucleus may shift from its central position so that the vertebral segment is unable to return to its normal position. A firmly locked rotational subluxation can result.
When uninterrupted compression is applied to any active and mobile joint, cartilaginous erosion followed by arthritis can be expected. When continuous stretching is applied to any active and mobile synovial joint, capsulitis and a barrage of nociceptive CNS input can be anticipated. This can produce systemic effects.
Cervical Curve Reversal
Compared with the primary thoracic kyphosis, which is a structural curve, the cervical and lumbar anterior curves are functional arcs produced by their slightly wedge-shaped IVDs. They normally flatten in the nonweight-bearing supine position and quickly adapt to changes involving the direction of force. Although the cervical curve is the first secondary curve to develop in the infant, its maintenance in the erect posture is determined by the integrity of the lumbar curve.
A flattened cervical spine that is not compensatory to a flattened lumbar spine may be the result of a local disorder such as a subluxation syndrome caused by posterior shifting of one or more disc nuclei, hypertonicity of anterior musculature, or anterior ligamentous shortening as the result of local overstress, inflammation, occupational posture, or congenital anomaly. The clinical picture is often the result of trauma-producing whiplash injury, herniated disc, subluxation, dislocation, fracture, or ligamentous injury. Torticollis, arthritis, malignancy, tuberculosis, osteomyelitis, or other pathologies also may be involved. The condition occurs more frequently after the age of 40, and the sexes appear equally affected.
Cervical flattening is often the result of paraspinal spasm secondary to an underlying injury, irritation, or inflammatory process. The acute clinical picture is one of torticollis. Other manifestations include headaches (occipital, occipital-frontal, supraorbital), vertigo, tenderness elicited on lateral C4–C6 nerve roots, neuritis involving branches of the brachial plexus due to nerve root pressure, hyperesthesia of one or more fingers, and loss or lessening of the biceps reflex on the same or contralateral side. Infrequently, the triceps reflex may be involved. One or more symptoms are often aggravated by an abnormal position of the head such as during reading in bed, an awkward sleeping position, or long-distance driving.
Cervical Subluxation/Fixation Syndromes
Occipitoatlantal Subluxation/Fixation Syndromes
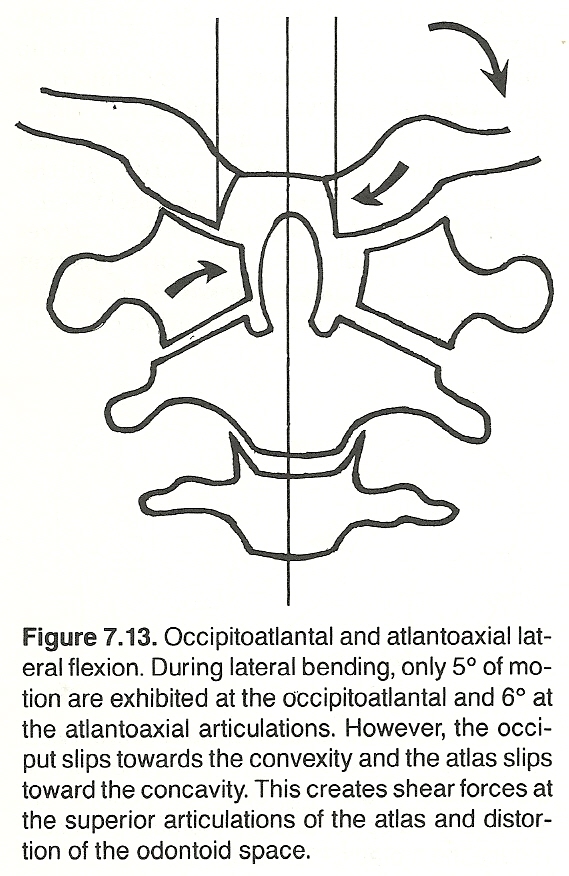
Because all freely movable articulations are subject to subluxation, the atlanto-occipital diarthrosis is no exception. The stress at this point is unusual when one considers that the total weight of the cranium is supported by the ring of the atlas, about 1/20th the circumference of the skull, and several spinal muscles, subject to spasm and hypertonicity, have their attachments on the occiput.
Relative to the atlas, the condyles may slip right or left with attended inferiority or superiority and may or may not present with a degree of rotation. In some instances, pure suboccipital jamming may be found as the result of muscle contraction or a blow to the vertex of the skull.
Neurologic disturbances may result from muscular and fibrotic changes along the cranial nerve pathways that emit from the skull and pass intimately between and under suboccipital fasciculi. Five of the cranial nerves are thus vulnerable: the facial, glossopharyngeal, vagus, spinal accessory, and hypoglossal. In addition, circulatory impairment of major and minor nerves of the neck may alter the function of those cranial nerves that do not exit from the skull proper such as the olfactory, optic, oculomotor, trochlear, trigeminal, abducens, and auditory, but which are contained within the cranium and remote from direct vertebral subluxation encroachment effects.
In studying tonic reflexes of the neck during cervical rotation, Deering and associates determined that the reflex is ipsilateral and that the receiver field lies in the region of the upper joints of the neck, especially the atlanto-occipital, C1, and C2 joints.
 |
Atlas Subluxations
Being near the end of a kinematic chain, the atlanto-occipital joints are subject to numerable degrees of subluxation in flexion, extension, rotation, and laterality. Rotary subluxation is not uncommon, especially if the atlantal cups are shallow. Excessive rotation is allowed by the lax check ligaments and capsules. Head weight, the angle of force, the planes of articulation, and the integrity of the para-articular tissues determine the stability present.
The atlas may be found to have sideslipped to the right or left, tipped bilaterally superior or inferior, or rotated, relative to the axis. There are no true bony IVFs for passage of the C1 and C2 spinal nerves, thus avoidance of the type of IVF encroachments produced in the lower spine.
The dura mater of the spinal cord is firmly fixed to the margin of the foramen magnum and to the C2 and C3 vertebrae. In other spinal areas, it is separated from the vertebral canal by the epidural space. Since both the C1 nerve and the vertebral artery pass through this membrane close to the superior pillar of the atlas and beneath the overhanging occiput, atlanto-occipital distortion may cause traction of the dura to produce irritation of the artery and nerve unilaterally and compressional occlusion contralaterally.
There is also a synapse between the upper cervical nerves and the trigeminal that also supplies the dura mater, which helps to explain why irritation of C1 results in a neuralgia not only confined to a small area at the base of the skull but is also referred to the forehead or eye via the supraorbital branch of the trigeminal. The greater occipital nerve does not tend to do this. It exits between the posterior arch of the atlas and above the lamina of the axis, referring pain to the vertex of the head.
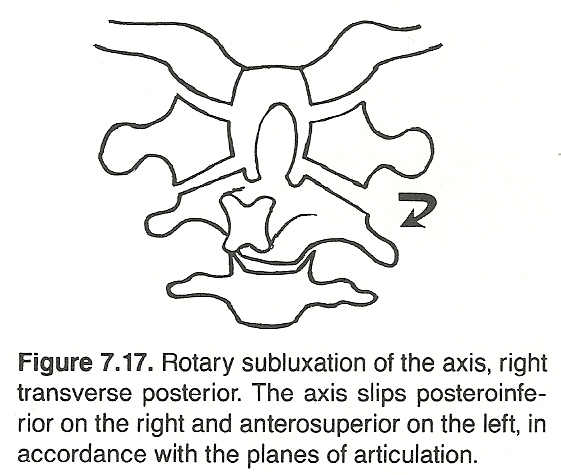
Axis Subluxations
With the possible exception of L5, no other vertebra is probably subluxated more frequently than C2. The most common symptom is a unilateral suboccipital neuralgia on the side of posteriority. Sometimes called cervical migraine, the neuralgia typically begins in the upper neck and extends over the skull into the temporal and possibly the orbital areas. On the side of posteriority, palpation discloses a tender prominence over the articulating process and a contralateral deviation of the spinous process away from the midline. Posterior axis (or occipital) subluxations are sometimes misdiagnosed as anterior atlantal subluxations.
Rotary subluxations of one or more of the upper three vertebrae (particularly the axis) may cause pressure upon the superior cervical ganglion. The syndrome produced may incorporate excessive facial and forehead perspiration, dry mouth and nasal mucous membranes, dryness and tightness of the throat, dilated pupils, tendency toward exophthalmos, migraine attacks due to unilateral angioneurotic edema, facial vasomotor disturbances with possible angioneurotic swelling, and moderate tachycardia with functional arrhythmia.
De Rusha points out that dysphagia and dysarthria may sometimes be attributed to upper-cervical involvement rather than a CNS situation. The C1 joins the hypoglossal nerve, which supplies the intrinsic muscles of the tongue. It then joins the descending cervical which is derived from C2 and C3. A loop of nerves, the ansi hypoglossi, which supplies muscles necessary for deglutition and speaking, is derived from C1–C3.
The superficial sensory cutaneous set of the cervical plexus (C1–C4) is frequently involved in subluxations of the upper four segments, particularly when there are predisposing spondylotic degenerative changes. The greater occipital (C2) nerve does not tend to do this. It exits between the posterior arch of the atlas and above the lamina of the axis.
Neurovascular Effects of Upper Cervical Subluxations
Medulla Oblongata. The medulla oblongata extends well into the lower reaches of the foramen magnum and the ligamentous ring that connects it with the atlas, thus any type of occipital or atlantal subluxation may produce abnormal pressure on this portion of the brain stem. Bilateral posterior shifting of the occiput or atlas may cause pressure upon the pyramids or adjacent olivary bodies, producing a syndrome of upper motor neuron involvement characterized by a degree of spastic paralysis or ataxia. A lateral shifting of the occiput may cause pressure upon the tubercle of Rolando producing pain in the area of trigeminal nerve distribution, headache, sinus discomforts, ocular neuralgias, and aches in the jaw.
Vagus Nerve. As the vagus lies almost in immediate contact with the transverse process of the atlas, rotary subluxation of the atlas may cause pressure which can produce a wide range of symptoms. The syndrome produced may exhibit as nasal and sinus congestion, swallowing and speech difficulties, cardiac arrhythmia, coronary artery spasm, gastric and intestinal colic, and other symptoms of vagal disturbance.
Vertebral Arteries. Janse states that any cervical subluxation (particularly atlantal, axial, or occipital) provoking muscle spasm may produce unilateral or bilateral constriction of the vertebral arteries, resulting in circulatory impairment. A large number of equilibrium, cardiac, respiratory, cranial nerve, extrapyramidal, visual, epileptic, and auditory symptoms may follow.
West points out that the vertebral artery can be completely occluded by just turning the head backward and to the opposite side during postmortem studies. Even without a degree of arteriosclerosis, the vertebral artery can be considered a fairly firm tube in the adult that responds poorly to twisting and pressure.
Vertebral Veins and Deep Cervical Veins. Spasm of the suboccipital muscles may cause a decided impediment of venous drainage from the suboccipital area via the vertebral and deep cervical veins, resulting in a passive congestion with consequent pressure upon the sensory nerve endings in the area. This is sensed by the patient as unilateral or bilateral pain and a throbbing discomfort, and may be palpated as knotty lumps within suboccipital muscles.
Sympathetic Disturbances
The vertebral nerve (sympathetic) runs along the vertebral artery within the arterial foramen of the cervical transverse processes. Neuritis is considered to occur from mechanical irritation to the vertebral artery anywhere along its course, producing symptoms of a vasomotor nature; eg, headache, vertigo, tinnitus, nasal disturbances, facial pain, facial flushing, and pharyngeal paresthesias.
Neuwirth and Kobayshi and associates report that stimulation of the cervical sympathetic trunk can cause alterations of the cerebral circulation and its regulatory mechanism. Thus, irritative lesions involving the cervical region and its articulations may in turn irritate the sympathetic nerve plexuses ascending into the head via the vertebral and carotid arteries. Baklavadzhyan's group found that the cervical sympathetic nerves had a strong influence on the vagus nerve and hypothalamus, as well as on cortical recruiting responses.
Many cases of visual and aural symptoms occur with upper-cervical distortion where the arch of the atlas snugly hugs the occiput, thus possibly irritating the sympathetic plexus of nerves on the vertebral arteries as well as partial compression of the vessels. To appreciate this, we must remember that the visual cortical area of the occipital lobe (cuneate lobe and calcarine fissure area) requires an ideal blood supply dependent on the sympathetics ascending the great vessels of the neck, and this holds true for the inner ear as well.
DeRusha's Maneuver. To test this syndrome, De Rusha suggests having the supine patient read some printed matter while the examiner places gentle traction on the skull cephalad, separating the occipital and atlantal articulations. A positive sign occurs when the patient, often to his or her surprise, experiences momentarily enhanced visual acuity or a reduction in tinnitus.
Cailliet points out that although sympathetic fibers have not been found along the cervical roots, surgical decompression of an entrapped nerve root relieves symptoms attributed to the sympathetics. The mechanism for this effect is not clear.
Lower Cervical Subluxations
A subluxation of one or more of the lower cervical vertebrae often involves the brachial plexus (refer to Table 7.4). Because the distribution of the brachial plexus is so extensive, a multitude of abnormal reflections may be seen in its areas of distribution that must be discerned by knowledge of the pathophysiology involved.
A few of the more common disturbances caused by lower cervical subluxations and trauma would include shoulder neuralgias, neuralgias along the medial arm and forearm or elbow, unclassified wrist drop and hand dystrophies, acroparesthesia, weak grip strength, and vague "rheumatic" wrist or hand complaints. A subluxation of one or more of the C3, C4, or C5 segments may involve the phrenic nerve and produce symptoms of severe chronic hiccup and other diaphragmatic disorders.
Subluxation-Induced Reflex Syndromes
Various spinosomatic and spinovisceral syndromes may result from cervical subluxations. For example, the involvement may be in the area of C–C4. This area includes the cervical portion of the sympathetic gangliated chain and the IX XII cranial nerves as they exit from the base of the skull and pass into their compartments within the deep cervical fascia. The syndrome may include:
(1) suboccipital or postocular migraine,
(2) greater occipital nerve extension neuralgia,
(3) mandibular, cervical, auricular, pectoral, or precordial neuralgia,
(4) paroxysmal torticollis,
(5) congestion of the upper respiratory mucosa, paranasal sinuses, or eustachian tube with hearing loss,
(6) cardiorespiratory attacks,
(7) ocular muscle malfunction,
(8) pathologic hiccups,
(9) scalenus anticus syndrome, and
(10) painful spasms in the suboccipital area.
Phillips states that if a subluxation produces a stretching of the paravertebral musculature, there will be a continuous barrage of afferent impulses in the Ia fibers. "These afferent impulses monosynaptically bombard the alpha motor neurons causing the paravertebral musculature to go into tetany (spasm). There is a cessation of this afferent barrage when the stretch is released. The muscle stretching also initiates afferent impulses in the Group II afferents from flower spray endings that may reinforce the spastic muscle condition." He goes on to say that trauma to facet joints, disturbed articular relationships, spasms of closely related muscles, and overlying trigger points, all the results of a subluxation, set up a barrage of flexor-reflex afferent impulses via Group II--IV fibers that converge upon the internuncial pool in lamina seven of the spinal cord. "This abundant supply of flexor-reflex afferent impulses excites the alpha motor neurons through multisynaptic connections causing an excess of excitation of paravertebral muscles resulting in spasm."
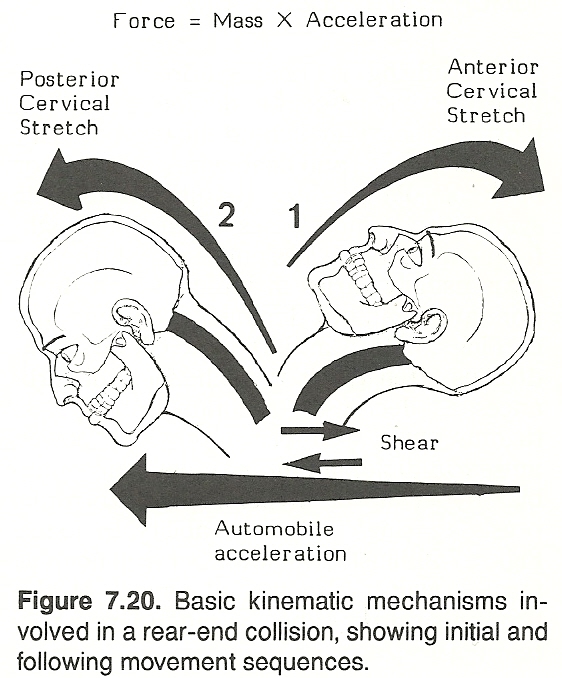 |
Neurologic Effects of Whiplash and Similar Cervical Syndromes
Severe sprain (eg, whiplash) can be assumed if cervical pain arises immediately after the accident or shortly thereafter. Difficulty in opening the mouth (when the TMJ is intact) points to severely strained suprahyoid muscles, according to Macnab. If severe muscle splinting of the neck is accompanied by pain in the mastoid-mandible area, the possibility of fracture (probably odontoid or midcervical) must be eliminated immediately. Severe pain and spasm not arising until the following day suggest severe strain of one or more posterior cervical muscle groups. Specific involvement depends on the position of the head and neck during impact.
Pain, spasm, and related neurologic focal signs generally suggest either cord damage or root injury from associated lateral hyperflexion or dislocation that may have been spontaneously reduced. Besides neck pain, a wide variety of usually overlapping features may be exhibited after an extension injury. For example, expressions may be seen in:
1. Neuropathy (radiculitis, cerebral concussion, IVF fault, hoarseness, dysphagia, headache, visual disturbances, nystagmus).
2. Vasomotor disturbances (vertebral artery injury, tinnitus).
3. Musculoskeletal impairment (overt hypermobility and hypomobility at different segments, and extensive trigger point development).
4. Audiovestibular faults (deafness, vertigo)
5. Deficits of memory (cerebral concussion amnesia).
In discussing the greater occipital-trigeminal syndrome, Palmateer states that whiplash injury can cause trauma of both cervical and upper thoracic areas of the spine. The signs and symptoms may be from altered function of the cervical autonomic spinal accessory nerve, various cervical and upper thoracic nerve roots, and compression of the vertebral artery. Traction on the C2 root may cause pain to radiate through the greater occipital nerve supply to the occipital scalp and into the eye via connections with the ophthalmic division of the trigeminal nerve.
Disturbances of Hearing and Vision of Cervical Origin
In studying cervical syndromes, Chrisman/Gervais associate deafness, tinnitus, blurred vision, pain behind the eye, pupillary dilation, vertigo, and headache (unilateral or bilateral). Pang states that the audiologic symptoms, in most cases, consist of a high-frequency hearing loss and tinnitus. The tinnitus usually varies in intensity and duration, and tends to diminish with time.
According to Roca and Dionne, cervical syndromes often result in such visual disturbances as decreased accommodation, nystagmus, decreased prism vergence power, aniscoria, diplopia, blurred vision, photophobia, hyperphoria, hypertropia, exotropia, ptosis, tearing, and the inability to focus.
Disturbances of Equilibrium of Cervical Origin
It has long been recognized that dizziness and/or vertigo can be caused by injury to or a disturbance in the neck muscles. The theories of the mechanism are reported by Pang, Hilse, Baloh, and Jepson to be:
(1) neuromuscular, by which an alteration in the proprioceptive impulses from deep muscles and tissues causes the dysequilibrium;
(2) neurovascular, in which the injury produces a disorder of the sympathetic vertebral plexus leading to changes in the blood circulation in the inner ear; and
(3) obstructive-vascular, by which injury or degenerative processes cause physical obstruction in the vertebral artery.
Headaches of Cervical Origin
Kraus, Markovich, Bogduk, Keith, Gitelman/Fitz-Ritson, and others have noted the significance of upper-cervical disturbances in relation to headaches, occipital neuralgia, and neck pain. Boake, an allopath, reports that at least 70% of the headache cases he sees in family practice arise from the cervical spine and associated structures, and Mayer and associates relate cervicogenic headaches with upper-cervical hypomobility.
In offering a neurologic appraisal of pain in the head, Kraus states: "It has been my experience that the most common cause of headaches originates in the 'vicious circle' generated by the abnormal and painful contraction of the cervical-nuchal muscles, mainly the trapezius muscle. These contractions generate a type of 'ischemic irritation' that includes the entrapment of the second cervical nerves (greater occipital and lesser occipital) as they travel through the bulk of the muscle, ascending into the back of the head to innervate the posterior scalp region, the temporal areas, and the lobes of the ears, sending terminal branches into the angle of the jaw, the back of the eye, and the vertex of the head." This process can create a distinct clinical syndrome that is easily confused with atypical "vascular migraine" because of the unilaterality of the symptoms and frequent complaints of pain in the back of the eye with or without visual disturbance.
Kraus also states that the second most common entity is the TMJ pain dysfunction syndrome, which has been proven to be more common than many expect and has many protean manifestations to the extent it has become known as The Great Impostor. "The fact that a cervical nerve irritation can create a painful condition in the angle of the jaw or in the temple explains the possible common 'irritative' source of both syndromes."
Markovich reports that the most common headache is the type caused by neuromuscular skeletal imbalance. Frykholm and Khurana/Nirankari more specifically emphasize irritation of the posterior cervical sympathetic plexus. Markovich points out that "the head in the human species has changed its position from the quadruped to the erect, thereby changing the basic relationship between the cervical spine and the head, with its important functional structures, and the rest of the body." For reference, he calls attention to the quite delicate interaction and highly sensitive biofeedback or servo-mechanisms that continually make adjustments in body balance, vision, pressure, and hearing with head and neck posture. "These regulatory, homeostatic mechanisms can be disturbed by a variety of conditions, originating at any level, including the inflammation and/or irritation of the cephalic projection of the upper cervical nerves (cervico-occipital neuralgias)."
Abnormal contraction of the muscles at the occipitocervical area appears to generate a type of "ischemic irritation" that includes the entrapment of the C2 nerves (greater and lesser occipital) as they pierce the thick muscle and ascend to the back of the head to supply the back of the scalp, the temples, and the ear lobes, sending branches to the top of the head, the back of the eye, and the angle of the jaw.
Differentiation of various types of headaches is shown in Table 7.5, adapted from Markovich's data.
However, keep in mind that a patient may not exhibit such a clear-cut picture. For example, vascular migraine may be superimposed on occipitocervical neuralgia or episodes may be interposed, depending upon the causes involved.
| Symptom/Sign | Occipito- cervical Neuralgia | Trigeminal Neuralgia | Vascular Migraine | Temporo- mandibular Traction |
| Pain | Throbbing, paroxysmal | Excruciating, paroxysmal | Severe, paroxysmal | Severe, dull |
| Quality | Spasm | Stabbing | Throbbing | Dull ache |
| Location | Occipital | Facial | Unilateral | Facial |
| Aura | None | None | Visual | None |
| Duration | Days | Brief | Hours | Chronic |
| Associated symptoms and signs | Earache Eye pain Neck pain Paresthesias Anxiety Tinnitus Nausea | Trigger zones | Vomiting Photophobia Irritability | Bruxism Malocclusion Earache Joint clicks |
Neck and Arm Pain of Cervical Origin
Intervertebral Disc Syndromes
The two most common disorders of cervical IVDs are degenerative disease processes and disc protrusion. These disorders may manifest singularly or be combined.
The neurologic signs in the cervical radiculopathies are shown in Table 7.6.
These features vary depending upon the direction of the disc bulge; eg, upon the nerve root, IVF vessels, spinal cord, or combinations of involvement. In some acute and many chronic cases, numbness may manifest without pain. In acute disorders, the cervical signs may be confused with those of shoulder or elbow bursitis, epicondylitis, or facet subluxation, especially when no local cervical symptoms exist.
| Posterior neck numbness and pain radiating to the mastoid and ear. The reflexes test normal. | ||
| Posterior neck numbness and pain radiating along the levator scapulae muscle and sometimes to the pectorals. The reflexes are normal. | ||
| Lateral neck, shoulder, and arm pain and paresthesia, deltoid weakness and possible atrophy, hypesthesia of C5 root distribution over middle deltoid area (axillary nerve distribution). The reflexes test normal. | ||
| Pain radiating down the lateral arm and forearm into the thumb and index finger; hypesthesia of the lateral forearm and thumb; decreased brachioradialis reflex; brachioradialis, biceps, and supinator weakness. | ||
| Pain radiating down the middle forearm to the middle and index fingers, hypesthesia of the middle fingers, decreased triceps and radial reflexes, triceps and grip weakness. | ||
| Possible pain radiating down the medial forearm and hand to the little finger, ulnar hypesthesia, intrinsic muscle weakness of the triceps and grip. However, these symptoms are uncommon. Reflexes are normal. |
Degenerative Disc Disease. Cervical stiffness, muscle spasm, spinous process tenderness, and restricted motion are common features. When pain is present, it is usually poorly localized and often referred to the occiput, shoulder, between the scapulae, arm or forearm (lower cervical lesion), and may be accompanied by paresthesias. Radicular symptoms rarely manifest unless a herniation is present.
Disc Protrusion or Herniation. Generally, central herniation produces local neck pain while lateral herniation produces upper extremity pain. If the protrusion is central, cord signs and symptoms exhibit as lower extremity spasticity and hyperactive reflexes. Sensory changes are rarely evident, but the gait may be ataxic. If the protrusion is posterolateral, the nerve root will be involved rather than the cord. Posterior osteophytes form at the disc attachment peripherally, often compromising the IVFs and vertebral canal. This may be noted by narrowing of the A–P dimension of the spinal canal in lateral films and foraminal encroachment on oblique films. These signs most frequently occur at the C6–C7 level. Anterior osteophytes are considered the result of abnormal ligamentous stress rather than part of the disc degeneration process. They occur most frequently below the C4 level, as do alterations of the covertebral joints.
Spondylosis
Spondylosis is a chronic condition (that may become rapidly symptomatic) in which there is progressive degeneration of the IVDs leading to secondary changes in the surrounding vertebral structures, including the posterior apophyseal joints. It can be the result of direct trauma (eg, disc injury), occupational stress, aging degeneration, or found in association with and adjacent to congenitally defective vertebrae.
The classic picture is one of a middle-aged person with greatly restricted cervical motion, marked muscle spasm, positive cervical compression signs, insidious neck and arm pain aggravated by sneezing or coughing, acute radiculopathy from disc herniation, and some muscle weakness and fasciculations. Whiting also includes neck crepitus; local neck tenderness; headaches; neck pain radiating to the scapulae, trapezius, upper extremities, occiput, or anterior thorax; paresthesia of the upper and/or lower extremities; dizziness and fainting; impaired vibration sense at the ankle; hyperactive patellar and Achilles reflexes; and positive Babinski responses.
Spondylosis may produce compression of either the nerve root or spinal cord. During the degenerative process, intradisc pressure decreases, the anulus protrudes, and the end plates approximate through reduction of disc thickness. As the disc protrudes, it loosens the attachment of the posterior longitudinal ligament. This allows the anulus to extrude into the cavity formed between the posterior vertebral body and the ligament, and this portion of the anulus, in time, becomes fibrous and then calcifies. Because of this process, posterior osteophytes prevail in the cervical and lumbar regions, while anterior spurs are more common to the dorsal spine.
Torticollis
Acquired torticollis (wry neck) is a severe stiff-neck syndrome produced by contraction of the neck muscles, causing the head to be drawn to one side with the chin pointing contralaterally. It may have a traumatic, an inflammatory, or a neuropathic origin, or be of various superimposed factors. The condition may be either continuous (tonic) or spasmodic (clonic). The tonic type is frequently seen in cervical Pott's disease of bone and psychoneurotic states. Considerable care must be taken to determine the etiology and differentiate its many possible causes.
The pain associated with acute torticollis is often thought to be attributed to zygapophyseal capsulitis and covertebral joint inflammation. This can generally be confirmed by palpation and should not be confused with the pain aroused from stretching the rigid muscles on the side of the concavity.
Cervical Subluxation. The most common direct cause of torticollis is that from irritating cervical subluxation (eg, trauma, rotational overstress, unilateral chilling, unilateral lifting, instability). Subluxation also may be an asymptomatic complicating factor to various etiologic factors. Barge believes that the structural cause of torticollis is often a rotatory vertebral malposition and abnormal disc wedging, where the nucleus of an involved disc has been forced to shift away from compressive forces. The patient's symptoms are often self-limiting with time and rest that allows the disc to expand in its nonweightbearing (decompressed) state and the vertebral facets to be relieved of their jammed position. It can be theorized that, if the neck does not achieve this subluxation correction through disc imbibition, a rotatory scoliosis will be produced in adaptation so that the patient may at least have a straight eye level. But, as the now chronic subluxation has not been fully corrected, it can serve as a focus for morbid neurologic and degenerative processes, especially at the zygapophyses, covertebral joints, and IVFs.
Inflammation. "Wry neck" spasm (tonic, rarely clonic) of the sternocleidomastoideus and trapezius may be the result of irritation of the spinal accessory nerve or other cervical nerves by swollen glands, abscess, acute upper respiratory infections, scar, or tumor. A spontaneous subluxation of the atlas may follow severe throat infection (eg, bacterial pharyngitis). Neck rigidity may also be the result of a sterile meningitis from blood in the cerebrospinal fluid. Thus, if a patient has slight fever, rapid pulse, and rigid neck muscles, subarachnoid hemorrhage should be suspected. Lateralizing signs are often inconclusive.
Neuropathic and Idiopathic Forms. Focal neuropathic causes include ocular dysfunctions, syringomyelia, and tumors of the spinal cord or brain. Idiopathic forms are seen in acute calcification of a cervical disc, rheumatic arthritis, tuberculosis, or "nervous" individuals. Nelson feels that wry neck may also be the result of a subphrenic or subclinical visceral irritation being mediated reflexly into the trapezius and cervical muscles.
Severe Trauma. Traumatic dislocations of upper cervical vertebrae cause a distortion of the neck much like that of torticollis. A rotary fracture-dislocation of a cervical vertebra, especially of the atlas on the axis or the axis on C3, will produce neck rigidity and a fast pulse, but fever is absent. Local and remote trigger points are frequently involved. Even in mildly suspicious cases, the posttraumatic neck should always be x-rayed in two or more planes before it is physically examined.
Nuchal Rigidity
The term nuchal rigidity refers to a spasmotic contraction of the posterior muscles of the cervical spine, but it is not identical to a stiff-neck syndrome or the various types of true torticollis. The most common cause of nuchal rigidity, by far, is meningitis. However, the sign is not pathognomonic.
A number of inflammatory conditions may be involved. See Table 7.7.
| Syndrome: Nuchal Rigidity + | Primary Suspect Disorder(s) | |
| Focal neurologic signs | Cerebral hemorrhage Cerebral abscess Encephalitis Meningitis | Osteomyelitis Spondylosis Subluxation (acute) |
| Pyrexia | Cervical pyogenic infection Meningitis | Osteomyelitis Retropharyngeal abscess Subarachnoid hemorrhage |
| Retinal hemorrhage and pyrexia | Collagen disease Stroke | Subarachnoid hemorrhage |
| Tremor and diffuse spasm | Parkinsonism | |
(1) flaccid, atrophic paralysis of the muscles supplied by the involved nerve and
(2) loss of all sensation, including proprioception, in the skin areas distal to the lesion.
Refer to Table 7.3. When partial destruction to various peripheral nerves occurs, the effects are usually more prominent in the distal extremities. The condition is characterized by weakness, atrophy, and poorly demarcated areas of sensory changes. Trophic lesions of the joints, muscles (atrophy), skin, and nails are common in the late stage 4.
Ipsilateral vs Contralateral Symptoms. If symptoms appear on the opposite side of forceful bending of the cervical spine, undoubtedly a nerve has been "pinched" within the powerful muscles dorsal to the sternocleidomastoid. If this is the case, the symptoms usually subside in a few minutes with only slight residual tenderness and paresthesia that disappears within a few hours. On the other hand, if symptoms appear on the same side as the direction of the forceful bending, deep skeletal injury such as severe rotary subluxation, fracture, dislocation, or nerve compression can usually be anticipated.
Mild or Moderate Brachial Traction. After lateroflexion injuries of the neck, a sharp burning pain may radiate along the course of one or more cervical nerves the result of nerve hypertraction from overstretch. Scalenus anticus syndrome may exhibit. This nerve stretch is often called a "hot shot" by athletes, and recurring injury is common, especially in contact sports. It is not limited to sports, however, for any severe cervical lateral flexion can produce the syndrome. Immediate pain may radiate to the back of the head, behind the ear, around the neck, or down toward the clavicle, shoulder, arm or hand. Frequently, there are arm paresthesias, severe arm weakness, diminished active motion, decreased biceps and triceps reflexes, forearm numbness, and cervical movement restriction. These signs and symptoms may disappear and reappear with greater severity.
Root Avulsion. A similar but more severe nerve injury is that to the proximal brachial plexus or its roots that is usually caused by a fall on the shoulder, a blow to the side of the neck, forceful arm traction, or a combination of these mechanisms. The injury is produced by forceful shoulder depression that stretches the brachial plexus especially in the supraclavicular area. The result may be root tear near the vertebral foramen, spinal cord damage, dural cuff leaks of cerebrospinal fluid, and/or vertebral subluxation, fracture, or dislocation. During avulsion, the spinal cord proper is sometimes damaged, and contralateral cord symptoms are found. Such severe manifestations are rarely seen in the well-conditioned patient where the picture is usually limited to pain radiating into the arm and/or hand.
Cervical Rib and Related Syndromes
A cervical rib rising from C7 and ending free or attached to the T1 rib appears in the neck as an angular fullness that may pulsate because of the presence of the subclavian artery above it. It rarely produces symptoms, and it is usually first noticed when percussing the apex of the lung. The bone can be felt behind the artery in the supraclavicular fossa and readily demonstrated in a radiograph. Pain or wasting in the arm and occasionally thrombosis may occur from the impaired circulation.
Grieve points out that some clinicians are far too eager to blame upper limb paresthesias on the presence of a cervical rib just because it is there. Many patients with a cervical rib have no complaints, many without a cervical rib have similar complaints, and many with complaints have symptoms on the contralateral side of a unilateral cervical rib. However, when any anomaly such as a cervical rib is seen radiographically, the examiner should be suspicious that other anomalies not as evident may be associated.
Symptoms usually occur after the age of 11: after the ribs have ossified. Two groups of symptoms are seen, those from scalenus anticus syndrome and those from cervical-rib pressure. When symptoms are exhibited, they are usually from compression of the lower cord of the brachial plexus and subclavian vessels; eg, numbness and pain of varying intensity in the ulnar nerve distribution. The pain is worse at night because of pressure from the recumbent position. Tiredness and weakness of the extremity, finger cramps, numbness, tingling, coldness of the hand, areas of hyperesthesia, muscle degeneration in the hand, a lump at the base of the neck, tremor, and discoloration of the fingers are also characteristic. Work and exercise generally accentuate these symptoms, while rest and elevation of the extremity relieve them.
Thoracic Outlet Syndromes
The cervicothoracic junction area is a unique spinal area that receives far less attention than it deserves in both medicine and chiropractic. It is a common site of developmental anomalies; it is a major site of arterial, lymphatic, and neurologic traffic; and it presents the juncture of the highly mobile cervical spine with the very limited thoracic spine. This latter point is biomechanically significant.
Etiology. The generally accepted causes of cervicobrachial syndromes are compression of the nerve trunks, trauma to nerve trunks, injuries to the sympathetic and vasomotor nerves, trauma to the scalenus anterior muscle, embryologic defects, postural or functional defects, narrowing of the upper thoracic cap as a result of adjacent infections or anatomical defects, acute infection producing myositis, intermittent trauma to the subclavian artery, or a cervical rib.
There are several defined syndromes to consider under the classification of neurovascular compression syndromes (also termed thoracic outlet or inlet syndromes), each of which may produce the symptom complex of radiating pain in the shoulders and down the arms, atrophic disturbance, paresthesias, and vasomotor disturbances. These syndromes, however, do not necessarily indicate the specific cause of the problem; they only define the clinical picture.
Differentiation. Two groups of symptoms are seen, those from scalenus anticus syndrome and those from cervical rib pressure. The symptoms of cervical rib and scalenus syndrome are similar, but the scalenus anticus muscle is the primary factor in the production of neurocirculatory compression whether a cervical rib is present or not. Adson's and similar compression tests will usually be positive.
Compression of nerve tissue results in numbness, pain, paralysis, and loss of function. Compression of vascular structures results in moderate pain and swelling. The obstruction of circulation can result in clotting within the vessels with possible consequent infarction in the tissues supplied. These unilateral phenomena are usually limited to the cervicobrachial distribution.
Craniovertebral Malformations
Varied anomalies arise from upper-cervical malformations. They are usually characterized by an abnormal shift upward of the atlas and axis with the odontoid protruding above Chamberlain's line. Such anomalies are frequently associated with congenital neural malformations and with other osseous deformities (eg, Klippel-Feil syndrome).
Aplasia of the arch of the atlas, basilar impression, platybasia, congenital atlantoaxial instability, occipitalization, and odontoid anomalies are important considerations. As they may remain asymptomatic unless precipitated by the forces of trauma or of degeneration, a concern is that these anomalies may easily be confused with the root/cord signs and symptoms of lower cervical spondylosis. Headache, sensory loss, limb pain, and/or ataxia are often the presenting complaints.
Cervical Ankylosing Spondylitis
Ankylosing spondylitis is characterized by spinal pain, rigidity, spasm, joint deformity, ankylosis, and loss of chest expansion. There may be loose ligaments above a rigid axis leading to atlantoaxial dislocation. Disc spaces are rarely narrowed as the ligaments and discs ossify. The patient moves as if the spine was a metal rod, with head and shoulders moving as a unit.
A related fracture (usually lower cervical) through an ossified disc produces a characteristic chin-on-chest deformity, with or without paralysis from an associated epidural hemorrhage. The first signs are not often cervical but found in the dorsal spine (reduced chest expansion), lumbar spine (vertebral body "squaring"), and sacroiliac joints (erosion). The first cervical sign is usually that of reduced lateral flexion, followed by increasing gross neck flexion at rest and upper cervical subluxation. Deformity is usually greatest at the lumbar spine and hips, but spinal motion is first lost in the lower cervical area.
Cervical Pott's Disease
Cervical tuberculosis has the characteristics of joint tuberculosis elsewhere; viz, joint pain and tenderness, malposition of the bones and of the head, abscess formation, and wry neck with stiffness of the muscles of the back and neck and pain in the occiput. The patient is very protective of neck motion, and the chin is often supported by the hand if an abscess is present. Tenderness is present posteriorly on percussion and anteriorly on palpation where an abscess may be felt. Neck pain exists both day and night; it is often relieved somewhat when recumbent and frequently radiates to the occiput and shoulders.
Rheumatic or traumatic torticollis, however, may present these symptoms, and diagnosis may be impossible without the aid of other tests and diagnostic imaging. If in Pott's disease of bone the abscess causes pressure on the anterior spinal cord, a usually spastic paralysis occurs that is characterized by hyperactive reflexes, a positive Babinski, sustained clonus, and difficulty or inability to void.
Pyogenic Infection
Nontubercular pyogenic infection, most common in middle age, produces an exudative inflammation with hyperemia leading to osteoporosis and osteomyelitis. It may predispose a subluxation syndrome or be the effect of or concomitant with a subluxation syndrome. Early diagnosis is vital. The first clues are neck pain (possibly referred to the scapula or shoulder), fever, muscle spasm, and sometimes dysphagia due to a prevertebral abscess that may be palpable. In time, the end plate becomes involved and the infection enters the disc space. Bone destruction leads to collapse. The abscess may enter the cord or a paravertebral abscess may extend into the thorax, or vice versa.
Cervical Rheumatic Disease
The length of the cervical cord and cervical discs is greatest during flexion and least during extension in the normal spine. The opposite is true in the rheumatic spine because of the loss of vertebral disc and centrum height from destruction and absorption.
Neurologic Injury. Nerve roots may become entrapped within one or more IVFs from a combination of subluxation, perivascular adhesions, dural adhesions, rheumatoid nodules, granulation tissue, and sequestrated disc tissue. Neck pain, with or without radiation to the arms, weakness, feelings of instability, ataxia, and paresthesias are common symptoms. However, these cervical symptoms are difficult to differentiate if the disease initiates in the peripheral joints where signs of peripheral entrapment, myositis, tenosynovitis, and subluxated joints from tendon rupture exist. Related giddiness and fainting spells suggest an associated vertebral artery ischemia that is usually linked with an upward migration of the dens which produces a kinking of the vertebral artery at the atlantal level.
Rheumatic Atlantoaxial Subluxation. Orthopedic subluxation is always a danger, proceeding from the synovitis, apophyseal erosion, and erosion of the vertebral bodies involved that lead to instability from joint destruction and ligamentous laxity. As apophyseal erosion progresses, the dens migrates into the foramen magnum and the atlas becomes fixed to the axis to reduce the possibility of dislocation. These signs determine the severity and prognosis of the general disease. The characteristic anterior subluxation of the atlas on the axis is generally considered an adaptation change to help increase the capacity of the spinal canal as rheumatoid tissue accumulates.
Neoplasms
Malignant tumors are more common in adulthood than youth. In metastatic lesions, pain is constant, day and night, and not relieved with rest. The pain is increased by palpation, percussion, and movement. Cord tumors usually present pain with an insidious onset, but other early neurologic symptoms and signs are not always present during the early stages. Most cancerous tumors are associated with some degree of bone destruction, and a mass may or may not be palpable.
Osseous tumors, benign or malignant, intramedullary or extramedullary, infrequently occur in youth. Neck pain is typical, and paralysis may or may not be present. Diagnostic imaging (x-ray, ultrasound, magnetic) is necessary to rule out such suspicions.
Vertebral Artery Syndromes
The vertebral arteries are the major source of blood supply to the cervical spinal cord and brain stem, including the medulla oblongata, pons, and midbrain. They also supply the visual cortex of the cerebrum and cerebellum via the basilar artery. For an unexplained reason, one artery is usually smaller than its mate, reports Sweat/Sievert.
Vertebral Artery Deflection
The vertebral artery is a captive vessel from C6 upward. Extremes of rotation and flexion occur at the upper cervical region, but the four normal curves in the vertebral artery help to compensate during neck motion. Deflection may be caused by any stretching or elongation of the artery during neck injury. In later years, it is commonly associated with bony spurs from the covertebral joints or grossly hyperplastic posterior vertebral articulations from arthrosis.
Extension of the cervical spine allows the tip of the superior articular process of the posterior joint to glide forward and upward. If sufficiently mobile, the motion may cause encroachment on the vertebral artery and/or the IVF. Thus, deflection of the artery and any resulting symptoms are exaggerated by rotation and/or extension of the neck. As a result of pressure against the artery, there may be temporary lessening in the volume of blood flow. Atheromatous changes may occur later within the vascular wall. Symptoms include headache, giddiness, vertigo, nausea, vomiting, nystagmus, and suboccipital tenderness all which may be aggravated by neck motion.
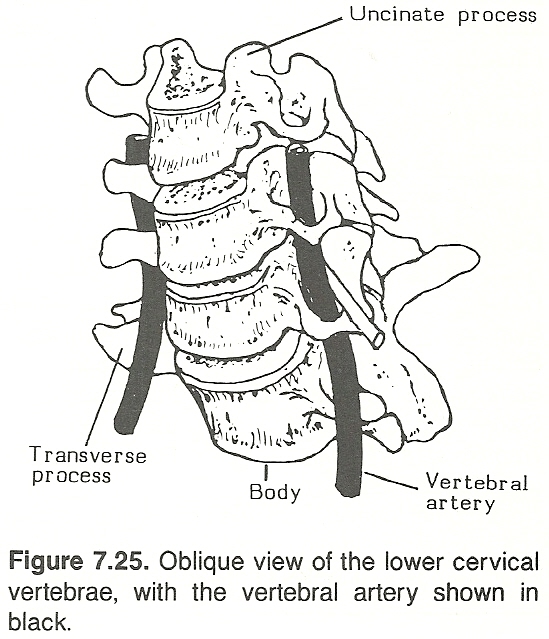 |
Vertebrobasilar System Patency
The major muscles of the trunk and their source of innervation
The vertebral arteries are unique in their course through several bony foramina, and in this intermittently channeled course from C6 upward they must make four nearly right-angle turns (forming a half square) in just 20--30 mm between entering the C2 transverse and entering the foramen magnum. Adding to this tortuous course is that anomalous loops occur in about one in every five people and the C2 area is a common site for aneurysm allowing additional vulnerability to compressive forces.
The vertebral arteries also exhibit special features for particular sites of predilection for degeneration by the change of fixed and unfixed vessel parts, increased vulnerability to bone and muscle movements, and the occlusion of peripheral arteries in their circulation area by difficult to diagnose pathologic changes of the vascular walls. These factors mandate that the probability of advanced degenerative or inflammatory process involving these arteries be eliminated before cervical manipulation or adjustments. Trauma to the vertebral artery has even been reported after emergency resuscitation procedures where passive extension of the neck is usually necessary to insert an air tube.
According to Jepson, Milne, and others, any minor compromise (eg, compression, atherosclerosis, thrombosis, vasospasm, kinking, longus colli and scalenus anticus spasm) producing an insufficiency of blood flow can lead to a singular symptom or a large number of seemingly unrelated cranial manifestations such as occipital headaches, memory lapses, dizziness, tinnitus, nausea and vomiting, lightheadedness or syncope, intermittent blurred vision, suboccipital tenderness, and, sometimes, retro-occular pain (episodic), speech impairment, extremity paresthesia and weakness, drop attacks, and gait defects all which can be generally grouped under the title of Barre-Lieou syndrome, especially when cervical trauma and an underlying spondylosis are involved. These signs and symptoms, which sometimes fluctuate from side to side, can mimic a posttraumatic cervical syndrome, multiple sclerosis, amyotrophic lateral sclerosis, or a tumor within the posterior fossa.
Severe interference (eg, thrombosis, osteophytic kinking, spondylotic foraminal impingement, extension effects of IVD degeneration) leads to involvement of the nucleus ambiguous of the vagus (eg, dysphagia, ipsilateral palatal weakness), descending root and nucleus of cranial V (ipsilateral facial hypesthesia, especially around the lips), descending sympathetic fibers (Horner's syndrome), vestibular nuclei (rotary nystagmus), midbrain and cerebellum (ipsilateral arm/leg malcoordination, intention tremor, ataxia), spinothalamic tract (contralateral hypesthesia), and the effects of impaired venous drainage and CSF flow (Wallenberg's syndrome).
Effects from Cervical Manipulation
It can be readily projected that the many cranial-oriented symptoms that have been relieved by chiropractic adjustments to the cervical region can be attributed to normalization of vertebral artery blood flow. Here we have a clinical paradox in that the same treatment may cause possible distress if precautions are not taken.
Reports of adverse effects (eg, paraplegia) from brainstem ischemia due to mechanical compression of the vertebral artery, dislodgment of a plaque, or a reflex spasm following forced rotation and extension of the head are rare. A Swiss study reported by Dvorak/Orelli states that slight neurologic complications are observed in only 1 out of 400,000 manipulations.
SELECTED THORACIC CONSIDERATIONS
are shown in Table 7.8.
Table 7.8. Major Muscles of the Trunk
| Muscle | Major Functions | |
| Diaphragm | Inspiration | |
| Erector spinae | Extension | |
| External oblique | Rotation, flexion, forced respiration | |
| Intercostals, external | Inspiration, extension | |
| Intercostals, internal | Expiration, extension | |
| Interspinalis | Extension, lateral flexion, rotation | |
| Intertransversarii | Lateral flexion, rotation | |
| Internal oblique | Rotation, flexion, forced respiration | |
| Longissimus dorsi | Extension | |
| Multifidus | Extension, lateral flexion, rotation | |
| Quadratus lumborum | Extension | |
| Rectus abdominis | Flexion, forced respiration | |
| Rotators | Extension, lateral flexion, rotation | |
| Semispinalis | Extension, lateral flexion, rotation | |
| Serratus posterior inferior | Expiration | |
| Serratus posterior superior | Inspiration | |
| Spinalis thoracis | Extension | |
| Transverse abdominis | Forced respiration |
Structural Considerations
Several unique factors should be considered regarding the stability of the thoracic spine. The major points are that it:
(1) is stiffer,
(2) is less mobile,
(3) has a smaller vertebral canal,
(4) has a high incidence of cord damage associated with structural damage,
(5) exhibits less vascularity for the cord,
(6) has restricting costal articulations,
(7) has an increased moment of inertia because of the added thoracic cage,
(8) has an anatomic curvature directed posteriorly,
(9) tends to be clinically unstable during flexion,
(10) has thin discs,
(11) is a common site for bursting anterior centrum fractures (lower region only),
(12) has the nuclei more centered within the anuli,
(13) has thicker yellow ligaments,
(14) has thinner and looser apophyseal capsules,
(15) has thinner and weaker interspinous ligaments,
(16) has a great resistance to extension,
(17) possesses coupling variants from top to bottom, and
(18) is the major source of supply of sympathetic fibers.
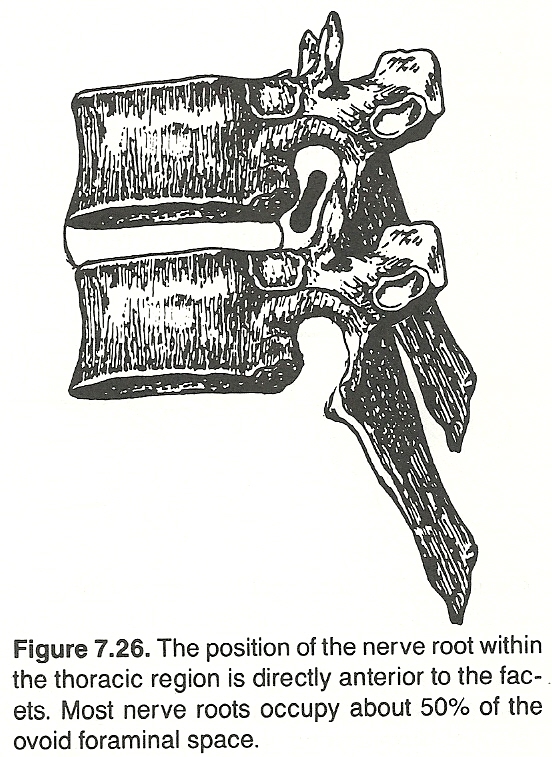 |
Thoracic Subluxation/Fixation Syndromes
The entire thoracic region is prone to a large number of various muscular, ligamentous, and costovertebral subluxation/fixations. In addition, primary thoracic fixations tend to produce secondary areas of fixation in the cervical spine, according to the studies of Gillet. In addition, it is a rare thoracic spine that does not exhibit some areas of tenderness upon careful palpation, and there are undoubtedly more trigger points and reflex fasciculations located upon the thoracic walls than any other area of the body.
The lower thoracic region (T9–T12) is predisposed to fixation development more than any other area of the spine. This is likely from the abrupt change in facet planes between the superior and inferior processes of the transitional vertebra, the altered stiffness between thoracic and lumbar vertebrae, the lack of strong supporting muscles enjoyed by the lumbar region, the lack of firm anterior support of the floating ribs, and the large compressive forces concentrated at this area. A sudden change in the stiffness properties of a structure at a given point will subject the structure to stress concentration at that point. This can lead to eventual mechanical failure with resulting neurologic implications. Intercostal neuralgia of the abdominal wall, states Carnett, often simulates gallbladder disease.
Vertebral Subluxations
Probably more than any other region, the thoracic region can be considered a critical zone neurologically and biomechanically, though the predominance of current literature emphasizes the importance of its neighboring regions —the cervical and lumbar spine. Vertebral facet subluxation syndromes, with or without severe fixation, are commonly found in general practice and frequently associated with visceral autonomic symptoms. With the well-developed muscular person subluxation is more commonly associated with acute symptoms of paravertebral strain and sprain.
Costovertebral and Costotransverse Fixations
These conditions are usually the result of hypertonic muscles or ligament shortening (eg, the anterior or posterior longitudinal ligaments). Unilateral pain, either stabbing or dull and usually episodic, may be expressed centrally and/or intercostally. The onset is usually rapid following a fall, push, misstep, stretch, sneeze, or cough. Transient but sharp neuralgia, angina, or dyspnea may be reported. Site tenderness, intercostal spasm, and tissue resistance are found at the rib angle and/or near the vertebral or sternal attachments. A midthoracic rib subluxation frequently presents pain radiating down the lateral arm, mimicking a scapulocostal syndrome.
Symptoms are frequently aggravated during deep inspiration when the trunk is flexed. Compressing the rib cage increases pain in fracture and sprain but not in intercostal strain. Springing the ribs P–A of the prone and relaxed patient to create stress at the vertebral connections aggravates symptoms and causes an immediate apprehensive muscle-guarding response in sprain and subluxation. An excessive reaction should make an examiner suspicious of a hidden fracture.
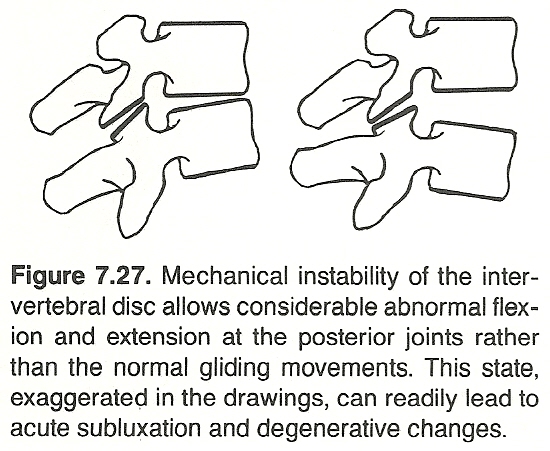 |
Thoracic Disc Lesions
The position of the protrusion determines the clinical picture. A midline protrusion usually produces intermittent pain, sensory impairment, pyramidal signs, and possibly bowel and bladder symptoms. Blits states that protrusion laterally causes more pain, is radicular in distribution, and is associated with fewer cord signs.
Thoracic cord signs probably arise because there is less vertebral canal space here for the spinal cord than in other regions of the spine. Thus, a slight posterior disc or end-plate protrusion may manifest cord and cerebrospinal flow symptoms and referred neurovascular signs and symptoms in the thoracic region that would never manifest in the cervical or lumbar spine. Added to this fact is the poor vascularity of the thoracic cord as compared to the cervical cord or even the cauda equina. Although the thoracic cord is comparatively small, its free space is extremely limited.
In moderate cases, the clinical picture is one of relative pain, usually unilateral in chronic cases or bilateral in acute cases, with girdle-like distribution. Baker emphasizes the associated intense girdle pain to be characteristic of a thoracic disc lesion. The pain may radiate to the abdomen, flank, or groin. Spastic paraparesis with sensory complaints may be involved. Motion restriction and tenderness on percussion may be the only local physical signs. Hyperactive tendon reflexes in the lower extremity and a positive Babinski reflex are sometimes seen. If disc protrusion interferes with spinal fluid flow, symptoms may mimic multiple sclerosis, arteriosclerotic myelopathy, etc.
In the upper thoracic spine, the pain of a herniated disc usually radiates anteriorly along the involved intercostal nerve. If the T1 root is involved, pain usually radiates down the medial aspect of the arm to the little finger. Sensory loss may be found on the medial side of the forearm, hand, little finger, and half the ring finger. Weakness is exhibited in the intrinsic muscles of the hand. If the T2 root is involved, pain will be referred to the axilla and the medial aspect of the arm. In the midthoracic spine, the pain and sensory impairment are intercostal (dermatomal) in nature. In the lower thoracic spine, the pain is referred anteriorly to the abdomen, pelvic organs, or groin, depending on the level of involvement. Segmental sensory impairment will help to isolate the lesion.
The associated symptoms of common posterior thoracic pain syndromes are differentiated in Table 7.9.
| Syndrome: Posterior Thoracic Pain + | Primary Suspect Disorders | |
| Hematuria | Kidney stone | Pyelonephritis |
| Neurologic focal signs | Multiple myeloma Spinal cord tumor Spinal tuberculosis | Subluxation complex Vertebral fracture |
| Pain, local | Aortic aneurysm Carcinoma Multiple myeloma Osteoarthritis | Scoliosis Spinal tuberculosis Spondylitis Sprain/strain |
| Pain, radiating | Costovertebral subluxation IVD syndrome Pyelonephritis | Radiculitis Rib fracture Spinal cord tumor Trigger point |
| Pain, upper abdominal | Cholecystitis Duodenal ulcer Gastric ulcer | Hiatal hernia Pancreatic carcinoma Pancreatitis |
| Pyrexia | Epidural abscess Hodgkin's disease Meningitis Osteomyelitis | Perinephric abscess Poliomyelitis Retrocecal appendicitis Tuberculosis |
The segmental innervation of the lumbosacral spine is shown in Table 7.10, and nerve functions of the lumbosacral plexus are shown in Table 7.11.
| Major Muscles Supplied | |
| Cremaster | |
| Iliopsoas | |
| Sartorius, pectineus, abductor longus | |
| Quadriceps, gracilis, adductor brevis | |
| Obturator externus, adductor magnus and minimus | |
| Tibialis anticus | |
| Semimembranosus, semitendinosus, extensor hallucis longus, popliteus, plantaris, extensor digitorum longus, extensor hallucis brevis, gluteus medius and minimus, quadratus | |
| Peroneus longus and brevis, tibialis posticus, flexor digiti brevis, abductor hallucis | |
| Gluteus maximus, obturator internus, biceps femoris, soleus, gastrocnemius, flexor hallucis longus | |
| Lumbricales, piriformis, abductor digiti, flexor digiti, opponens, quadratus plantae, interossei | |
| Levator ani, bulbocavernosus, schiocavernosus | |
| Sphincter vesicae | |
| Sphincter ani, coccygeus |
| Cremasteric | Patellar | ||
| Gluteal | Achilles | ||
| Plantar | |||
| Anal | |||
| Nerve | Function |
| Iliohypogastric | Sensory to skin over hypogastric and lateral gluteal areas. |
| Ilioinguinal | Sensory to skin over genitalia and upper medial thigh area. |
| Genitofemoral | Sensory to skin over scrotum, upper anterior thigh area; motor to cremaster. |
| Lateral femoral cutaneous | Sensory to skin over lateral thigh. |
| Obturator | Motor to adductor longus, brevis, magnus; obturator externis; gracilis. |
| Muscular branches | Motor to major and minor psoas, quadratus femoris, gemellus inferior and superior, piriformis, obturator internus. |
| Femoral | Sensory to skin over anterior and medial thigh, knee, leg, dorsum of foot to base of 1st metatarsal. Motor to iliacus, pectineus, sartorius, quadriceps femoris. |
| Superior gluteal | Motor to gluteus minimus and medius, tensor fascia lata. |
| Inferior gluteal | Motor to gluteus maximus. |
| Posterior femoral | Sensory to skin over inferior buttock, posterior thigh, cutaneous popliteal space, perineum, external genitalia. |
| Sciatic | Sensory to skin over posterolateral aspect of leg and lateral foot; heel; over upper third of lateral aspect of leg below knee; over anterolateral aspect of leg and dorsum of foot and toes; medial aspect of sole, great toe, 2nd to 4th toes; lateral aspect of sole, 4th and 5th toes; on dorsum of foot between great toe and 2nd toe. Motor to hamstrings, adductor magnus, gastrocnemius, plantaris, soleus, popliteus, tibialis anterior and posterior, flexor and extensor digitorum longus and brevis; peroneus longus, brevis, and tertius; abductor and adductor hallucis, flexor hallucis brevis, extensor hallucis longus, quadratus plantae, abductor digiti quinti brevis, all interossei, 1st through 4th lumbricales. |
| Pudendal | Sensory to skin of genitalia, anus, scrotum, labium majorus, penis, clitoris. Motor to levator ani, coccygeus, sphincter ani externus, transversus perinei superficialis, profundus, bulbocavernosus, ischiocavernosus, sphincter urethrae membranacae. |
The Lumbar Nociceptive Receptor System
Wyke, Gunn, and Lamb report that the lumbar ligaments and fascia are richly innervated by nociceptors. When the lumbar spine is in a relaxed neutral position, its nociceptive receptor system is somewhat inactive. However, any mechanical force that will stress or deform receptors, with or without overt damage, or any irritating chemical of sufficient concentration will depolarize unmyelinated fibers and enhance afferent activity.
Static postural support of the lumbar spine in the prolonged relaxed erect or seated postures is provided primarily by the passive elastic tension of the involved capsules, ligaments, and fascia rather than the spinal muscles whose roles can be considered insignificant during a state of relaxation. This shifting of support from the muscles to the ligaments, however, occurs slowly over a period of several minutes before significant EMG activity can be considered absent.
Mechanical and Chemical Factors of Low Back Pain
According to Calin, Waddell and associates, Kelsey, Frymoyer/Pope, and others, low-back pain experienced after trauma can be the result of mechanical factors, chemical factors, or both.
Features of Mechanical Pain
Normal mechanical force applied to normal tissue does not produce pain. However, abnormal mechanical deformation occurs whenever:
(1) abnormal stress is applied to normal tissues (eg, postural pain),
(2) abnormal stress is applied to abnormal tissues, or
(3) normal stress is applied to abnormal tissues (eg, soft-tissue shortening).
Pain from mechanical causes is sharp, acute, and occurs immediately. If mechanical pain does not occur until several minutes or hours after an activity, it is most likely that the position assumed following the activity is the cause of the pain rather than the activity itself.
Mechanical pain may be intermittent, appearing and disappearing, or vary in intensity according to aggravating and beneficial circumstances. It is usually intermittent because of increased and decreased mechanical deformation forces. In cases of pain of mechanical origin, the examiner should be able to reproduce the patient's symptoms by test movements. Continuous pain from constant mechanical deformation (eg, irreducible disc protrusion) is always possible but not common. The rule to remember is that pain of mechanical origin is affected by movement, for better or worse.
Features of Chemical Pain
Chemical irritants accumulate in damaged tissue soon after injury. When the nociceptive receptor activity is enhanced, pain will be experienced. Chemical irritation can be the result of any inflammatory, infectious, or traumatic process of sufficient degree. It also can be the result of any abnormal metabolic by-product, especially that of ischemia when of sufficient concentration to irritate bare nerve endings in the involved tissues.
In contrast to pain of mechanical origin, pain from chemical causes is constant, dull, and aggravated by normal movements as long as the chemical irritants are present in sufficient concentration. It may not occur until several minutes or hours after an injurious event has taken place. Chemical pain subsides during the natural healing process as scar tissue forms. Rarely does chemical pain from trauma extend pass 20 days after the accident.
Considerations in Adjustive Therapy
The specific motion that eases pain the most (reduces mechanical deformation) frequently determines the plane of adjustive therapy. One important exception to this would be the pain produced by motion that stretches shortened tissues. This type of pain subsides immediately when passive stress is removed and the joint returns to its neutral position.
In either subluxation or displaced IVD substance (viz, an end plate, anulus, or nucleus pulposus), a dynamic adjustment is most often given in the direction that decreases mechanical deformation and pain. When shortened tissues are involved, slow rhythmic manipulation increasing in force should be given in the direction that stretches the contracted tissues and temporarily increases pain. In some instances, an adjustment will be necessary to free adhesions and locked facets. Obviously, this requires careful differentiation before therapy.
Lumbar Subluxation/Fixation Syndromes
The articulations of the lower back are located central to the kinematic chain extending from the cranium to the feet. Thus, any alteration in normal dynamics such as a unilateral fixation must manifest biomechanical effects both above and below. Fixation at a link or links of any kinematic chain forces hypermobility and aberrant movements on the nearest possible segments, leading to neurologic and musculoskeletal signs and symptoms.
Rotational malpositions of the lower lumbar vertebrae are frequently found and invariably associated with changes in the related disc and posterior joints. In addition, rotation is coupled with tilting and vice versa. It is usually impossible to tell what is primary and what is secondary as each can cause the other. Periodic recurrence after correction can usually be attributed to congenital asymmetry of the facet planes or acquired asymmetry from the repeated deformation forces of trauma.
Whenever a vertebral motion segment is in a state of prolonged distortion, the involved connective tissues histologically adapt to their biomechanical requirements. Fibers on the side of the concavity shorten, and fibers on the side of the convexity lengthen. This process occurs in all connective tissues but becomes more overt in muscular and ligamentous tissues because motion is no longer symmetrical. Unless corrective action is taken, this state becomes progressively degenerative as the result of the abnormal weight distribution during static and dynamic activity.
Refer to Table 3.12 for the major neurologic signs in the lumbosacral radiculopathies.
Neurogenic Low-Back Pain Syndromes
Because more research has been done on the IVD than any other structure, there is a tendency to attribute almost any type of backache to some type of disc disorder. This leads to tunnel vision on the part of some clinicians because many disorders, both spinal and extraspinal, may simulate disc disease. The most common causes of nondisc functional pain are postural fatigue, spinal strains (acute and chronic), and IVF syndromes. Certain pelvic disorders also may be involved such as chronic abdominal collapse, pelvic infections or neoplasms, sacroiliac sprain, and coccygeal stress.
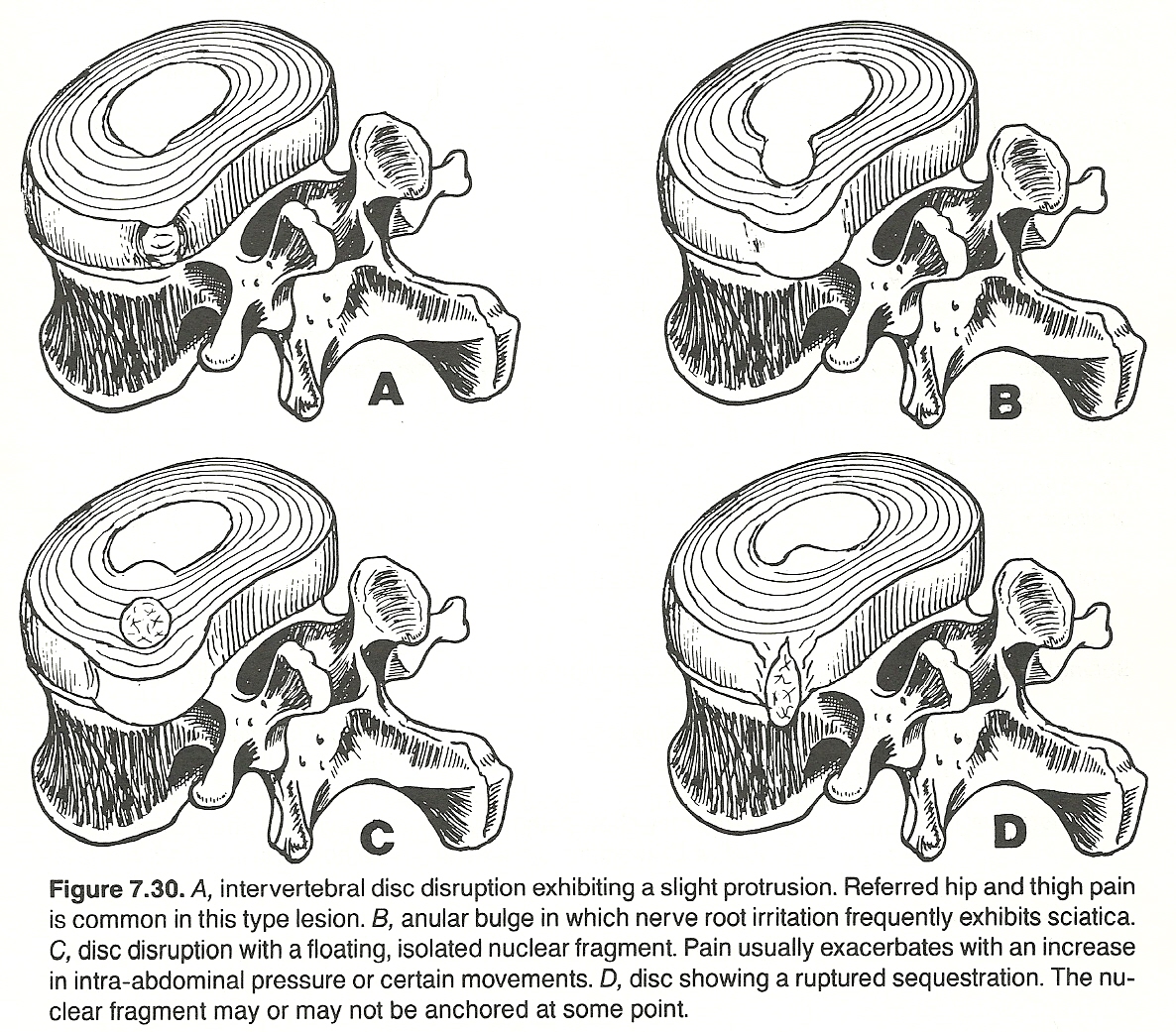
Acute Lumbosacral Angle Syndromes
An acute lumbosacral angle is frequently associated with low-back pain. The painful status of acute angulation of L5 on S1 is twofold:
(1) There is bursal involvement due to an overriding of the facets that stretches the bursa.
(2) There is a narrowing of the IVF, causing a telescoping of the facet joints from the superior to the inferior.
Intervertebral Disc Syndromes
Episodic back pain is probably the only consistent symptom in IVD syndromes, and even this may not be present until the late stage. Disc pain is usually intermittent and mechanically aggravated by standing, lifting, coughing, prolonged flexion (eg, while shaving or stooping), or a slight misstep. For some unknown reasons, these episodes often occur early in the day when nuclear turgor is at its maximum.
The major points of differentiation for nerve, root, and cord lesions are shown in Table 7.12.
| Nerve Lesions | Caudal-Root Lesions | Lumbosacral Cord Lesions |
| Usually unilateral | Usually bilateral, but not symmetrical | Usually bilateral and symmetrical |
| Pain on pressure over nerve trunks common | Not present; superficial hyperalgesia or anesthesia dolorosa | Not present |
| Symptoms present in nerve distribution | Symptoms in segmental distribution | Symptoms in segmental distribution |
| Pain often aggravated by movement, but spontaneous pain is not severe | Spontaneous pain is often severe; movement of limbs not painful; coughing, sneezing are painful | Pain absent unless nerve roots are implicated |
| Sensory loss involves pain, touch, temperature | Same | Sensory dissociation may be present with unilateral lesions in upper lumbar segments |
| Reflexes lost in areas affected; others are not increased | Same | Achilles reflex may be absent and patellar increased or vice versa, or all reflexes may be lost |
| Seldom involve dorsal divisions of peripheral nerves | Involve both dorsal and ventral distributions | Involve both dorsal and ventral distributions |
| Muscle atrophy and reaction of degeneration may be present | Same | Same |
| Fibrillation in muscles absent or slight | Same | Fibrillation of active muscles |
| Trophic sores absent | Trophic sores unusual or mild | Trophic sores common and severe |
| Sphincters not affected | Sphincters may be affected | Sphincters usually affected |
| No loss of sexual function | Often some loss of sexual function | Sexual function lost or dissociated |
| X-ray negative | X-ray may show pathology below L1 (fracture, dislocation, caries) | X-rays may show some pathology in T11, T12, or L1 |
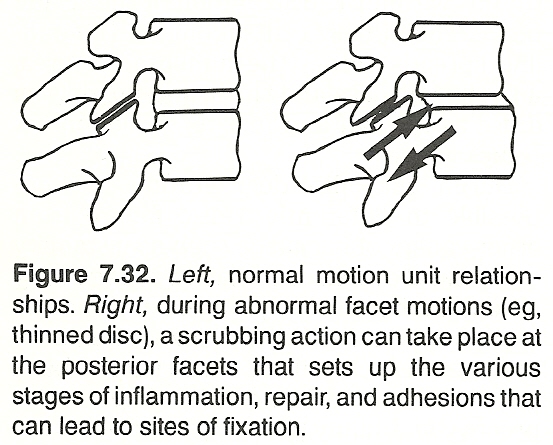 |
Facet Syndromes
It has been a popular belief that damage to a facet joint is always secondary to disc failure. However, Farfan, Grieve, and others state that autopsy evidence is clear that varying degrees of facet damage can and frequently do occur that are not secondary to disc failure. Helfet/Lee affirm that lesions of the posterior joints always affect the disc, and disc lesions always affect on the posterior joints.
The subluxation of lumbar facet structures, states Howe, is a part of all lumbar dyskinesias and must be present if a motion unit is deranged. In a three-point articular arrangement, such as that present at each vertebral segment, no disrelationship can exist that does not derange two of the three articulations. Thus, determination of the integrity of or subluxation of the facets in any given motion unit is important in assessing that unit's status.
To help differentiate the low back and sciatic neuralgia of a facet syndrome from that of a protruding disc, several physical clues are available. For example, with the patient standing with the feet moderately apart, the doctor from behind the patient firmly wraps his arms around the patient's pelvis and firms the side of his thigh against the back of the patient's pelvis. The patient is asked to bend forward. If it is a facet involvement, the patient will feel relief. If it is a disc that is stressed, symptoms will be aggravated.
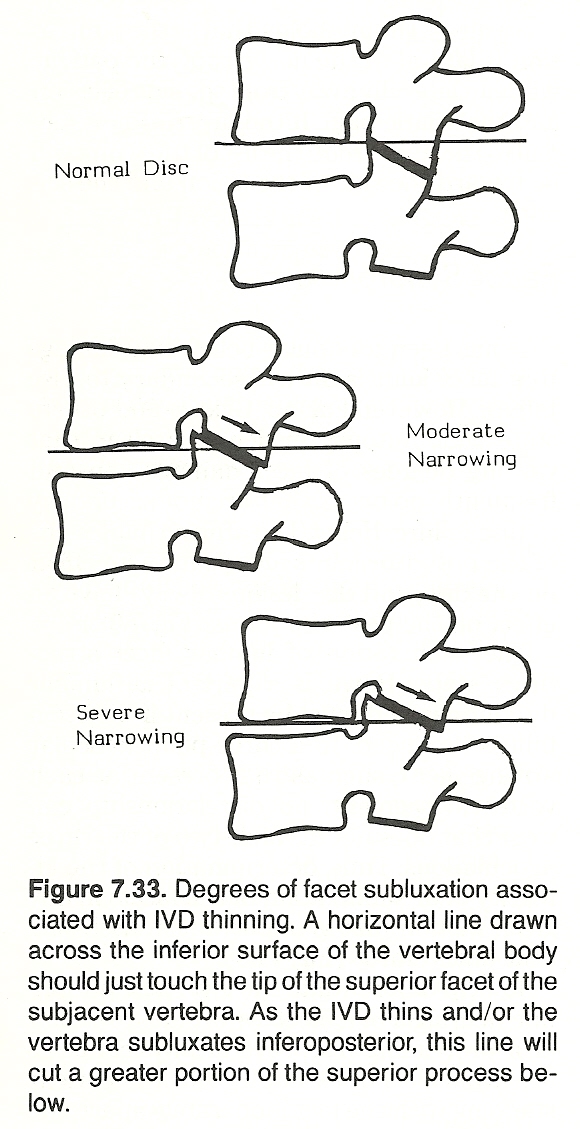 |
In facet involvement, the patient seeks to find relief by sitting with feet elevated and resting upon a stool, chair, or desk. In disc involvement, the patient keeps the knees flexed, sits sideways in the chair, and moves first to one side and then to the other for relief. If lumbosacral and sacroiliac pain migrates from one to the other side, it is suspected to be associated with arthritic changes.
Sciatica
Although it is the largest nerve of the body and supplies through its branches all the muscles below the knee, the sciatic nerve is rarely injured by sudden trauma. It is often affected, however, by sciatic neuritis (sciatica) that is frequently due to intermittent intrinsic trauma. Sciatic neuralgia or neuritis is characterized by pain of variable intensity to a maximum that is almost unbearable. The pain radiates from the lumbosacral or sacroiliac area down the posterior thigh and even to the sole of the foot. In time, muscular atrophy and a characteristic limp usually occur.
There is a lessening or lack of the patellar tendon reflex in sciatica (Babinski's sciatica sign). When the patient's great toe on the affected side is flexed, pain will often be experienced in the gluteal region (Turny's sign). Also in sciatica, the pelvis tends to maintain a horizontal position despite any induced degree of scoliosis (Vanzetti's sign), unlike other conditions in which scoliosis occurs where the pelvis is tilted.
Sciatic neuropathy must be differentiated from a lumbar impingement radiculopathy, and this is often challenging. The latter can be considered a nerve compression syndrome. As disc herniation rarely involves several segments, neuropathy is first suspected when multiple segments are involved. In contrast to forward flexion in the standing position, flexion in the supine position places little tension on the sciatic nerve. Thus, sciatica aggravated by both standing and supine flexion suggests a disc involvement. Sciatica aggravated in the standing but not the supine position suggests a nerve root involvement.
When Lasegue's straight-leg-raising test is made just short of pain, internal rotation of the femur increases pain and external rotation decreases pain in sciatic neuropathy but has little effect upon lumbar radiculopathies. During Lasegue's supine test, sciatic pain is invariably increased by forced dorsiflexion of the foot and relieved by flexion of the knee. As the point of pain is reached, active flexion of the patient's neck will increase pain in radicular involvement because of the increased tension on the dura. This test is considered a positive Lasegue confirmation, but it does not pinpoint the exact site of the lesion.
Lumbar Stenosis and Claudication
Studies by Porter and associates conclude that the spinal canal is relatively wide in children, reaches a maximum diameter in the late teens, and reduces slightly by late adult life. The size of the canal is particularly significant in patients who have neurogenic claudication and disc symptoms, but size is less significant in root entrapment syndromes.
Intermittent neurogenic claudication is a common manifestation secondary to lumbar spinal stenosis. The syndrome features low back pain and sciatica, which are usually aggravated when the spine is hyperextended or when walking. Gait, bowel, bladder, and sexual dysfunction is commonly associated. Sweere reports that Dejerine's triad is negative, and the femoral, popliteal, and pedal pulses are normal.
Narrowing of the IVD space with sclerosis of the adjacent vertebral bodies may occur as a consequence of infection, neoplasm, trauma, or rheumatic disease. When lumbar disc degeneration reaches the point of rotatory and lateral instability, posterolateral bulging of the anulus fibrosus into the root canal occurs when weight is taken on the ipsilateral lower limb. Symptoms of the spinal stenosis syndrome do not arise until the development of this instability.
Lumbar Nerve Root Entrapment
Entrapment of lumbar nerves may occur:
(1) at the lateral aspect of the central canal,
(2) at the lateral aspect of the IVF,
(3) at the posterior aspect of the IVD,
(4) at the anterior aspect of the zygapophyseal joints, or
(5) in the cauda equina. A wide variety of degenerative changes can occur in both the posterior joints and the disc area, which can produce central stenosis, IVD herniation, lateral entrapment, and/or ligamentous instability.
Besides the common nerve compression syndrome in the IVF by impingement (eg, subluxation complex), other types of entrapment may occur. After studying the interrelation between lumbosacral nerves and their surrounding tissue, Hasue and associates found several mechanisms leading to sciatica and lower extremity intermittent claudication. Typical mechanisms were the course of nerve roots altered by congenital anomalies or acquired lesions (eg, facet compression) and root compression by ossified ligaments. They also found that the space around the nervous tissue, both in the spinal canal and in the IVF, is narrower in males than in females.
Wiltse and associates describe an entrapment syndrome of L5 by the alar transverse process. They call it the far-out syndrome. It appears to be linked with elderly individuals with degenerative scoliosis or younger adults with isthmic spondylolisthesis with at least a 20% slip. Classical symptoms of nerve compression arise, usually at the L5–S1 level.
Lower Extremity Atrophy. Prolonged and/or severe nerve root irritation may show evidence of trophic changes in the tissues supplied. This may be characterized by obvious atrophy. Such a sign is particularly objective when the circumference of an involved limb is measured at the greatest girth in the initial stage and this value is compared to measurements taken in later stages. Chronic L5 root compression exhibits weak dorsiflexion of the foot, featuring a slapping foot-drop during gait. In contrast, chronic L4 root compression manifests weak quadriceps associated with knee pain and buckling during stance. Many knee operations have been unsuccessful because the focal irritation was of the L4 root rather than in the knee.
Referred Pain. Root pain usually has a dermatomal distribution that is aggravated by a Valsalva maneuver. In contrast, abnormal stimuli arising from the lumbar paravertebral soft tissues often refer a dull, diffuse, sclerotomal ache to the sacroiliac joints, buttocks, or posterior thighs. The pain may be solely sclerodermal or superimposed on dermatomal radicular pain and greatly confuse the clinical picture. It may originate from numerous sources.
Poole lists the subcutaneous tissues overlying the motion unit, the posterior aspect of the disc, the dura mater and epidural adipose tissue, the adventitial sheaths of the epidural and paravertebral veins, the walls of the vertebral arteries and arterioles, the articular capsules, the longitudinal ligaments, the ligamentum flavum, the interspinous ligaments, the paravertebral muscles and their tendons, and the periosteum.
Sensory Changes. The posterior sensory root in the lumbar spine is twice the thickness of the anterior motor root. When direct nerve root involvement occurs on the posterior root of a specific neuromere, it manifests as an increase or decrease in sensory awareness over the dermatome. Typical examples might include foraminal occlusion or irritating factors exhibited clinically as hyperesthesia, particularly on the:(1) anterolateral aspects of the leg, medial foot, and great toe, when involvement occurs between L4 and L5; and
(2) posterolateral aspect of the lower leg and lateral foot and toes when involvement occurs between L5 and S1.In other instances, this nerve root involvement may cause hypertonicity and deep pain in the musculature supplied by the neuromere; for example, L4 and L5 involvement, with deep pain or cramping sensations in the buttock, posterior thigh and calf, or anterior tibial musculature. In addition, direct pressure over the nerve root or distribution may be particularly painful.
Spinosomatic Reflexes. Nerve root insults from subluxations may be evident as disturbances in motor reflexes and/or infrequently as loss of muscular strength. Examples of these reflexes include the deep tendon reflexes such as seen in reduced patella and Achilles tendon reflexes when involvement occurs at L2–L4 or L5–S2, respectively. These reflexes should be compared bilaterally to judge whether the hyporeflexia is unilateral. Unilateral hyperreflexia is highly indicative of an upper motor neuron lesion.
Neurologic-Orthopedic Tests. Such tests as Kemp's, Lasegue's, Naffziger's, Bragard's, Demianoff's, Deyelle-May, and Fajersztajn's are often helpful in differentiating the various etiologies of low-back pain. An examiner should keep in mind that the originators of these maneuvers made specific claims of the significance of these tests, but the projected findings and conclusions are not duplicated consistently in practice.
Wyke has shown that because the nociceptive receptor system of the lumbar spine has such an extensive distribution, testing procedures designed to stress selected components and segments by orthopedic stress tests are extremely difficult if not impossible to perform. Only by visualizing the structures being affected by the biomechanical forces being applied will such tests be meaningful to the examiner.
Lumbar Dorsal Ramus Syndrome
This syndrome is described by Bogduk as featuring low-back pain that is referred to the lower extremity. Spasm of the lower back, gluteal area, and hamstring muscles are associated. Careful differentiation must be made to exclude an IVD lesion or nerve root irritation, as only the lumbar dorsal ramus is affected. Recognition of this syndrome may eliminate the need for unnecessary surgical referral.
Meralgia Paresthetica
This syndrome, often called lateral femoral cutaneous neuropathy, features a patch of anesthesia, paresthesia, or hyperesthesia, with or without pain, on the anterior surface of one or both thighs in the distribution of the lateral femoral cutaneous nerve. Low-back pain is often associated. The lateral femoral cutaneous nerve arises from the posterior divisions of L1–L3, appears at the lateral border of the psoas, passes obliquely across the iliacus to the anterior superior iliac spine, and then travels under the inguinal ligament to enter the anterolateral aspect of the thigh.
The symptom complex is thought to have its origin in some form of inflammatory process involving the lateral femoral cutaneous nerve or its roots. This focus of irritation may often be found:
(1) at the L1–L3 IVFs from subluxation encroachment or arthritic hyperplasia or
(2) in the pelvis from repetitive trauma as seen in athletic injuries and late pregnancy.
Nevertheless, pathology lying anywhere along the course of the nerve may be responsible, whether it be intraspinal, intersegmental, paraspinal, retroperitoneal, pelvic, or, rarely, abdominal.
Serious visceral pathology and hernias often simulate musculoskeletal dysfunction. It is unexplained why leukemia and other systemic diseases may present only backache as the presenting symptom, but it does occur. Back pain often arises early in visceral disease, long before classic physical signs and hematologic changes are noted. A few pathologies may extend from or affect the sacroiliac joints and lumbar spine early that often mimic the symptoms of sprain or chronic subluxation. Confusion may exist when related symptoms are brought out after trauma.
(1) irritative microtrauma to the interarticular structures,
The most common errors of analysis stem from misleading visual signs, subjective responses to testing procedures, structural symmetry, and subjective descriptions of pain. Many procedures are helpful in differentiation; eg, the iliac compression test, Piedallu's sign, the belt test, Berry's sign, Erichsen's pelvic rock test, Gaenslen's test, Hibb's test, Mennell's test, and Yeoman's test.
Typically, the patient reports a sense of numbness or burning in the anterolateral aspect of the thigh, which is rarely painful until the late stages. Care must be taken to differentiate this syndrome from trochanteric or iliopectineal (iliopsoas) bursitis, both of which refer pain to the anterolateral thigh. It also should be kept in mind that pronation or supination of the ankle, genu varum, genu valgum, genu recurvatum, flexion contracture, etc, can cause or contribute to anterosuperior thigh pain.
Reiter's Syndrome
The triad of sterile spondylitis, uveitis, and urethritis or prostatitis is called Reiter's Syndrome. The cause is unknown. Backache is usually the presenting symptom, but urinary or conjunctival complaints may manifest first. The weight-bearing joints show the first arthritic changes, and later the proximal joints of the fingers and toes become afflicted.
SELECTED PELVIC CONSIDERATIONS
Sacroiliac Subluxation/Fixation Syndromes
For many years, Gray's Anatomy classified the sacroiliac joint as an immovable synarthrosis. Throughout the efforts of chiropractic and osteopathic research, however, most anatomists today describe it as a movable diarthrosis, complete with joint cavity, synovial membrane, and synovial fluid.
Sacroiliac subluxations produce:
(2) induction of a vertebral motion unit subluxation and/or contributions to the chronicity of existing subluxations,
(3) induction of spinal curvatures and/or contributions to the chronicity of existing curvatures, and
(4) biomechanical impropriety of the pelvis in static postural accommodation and locomotion.
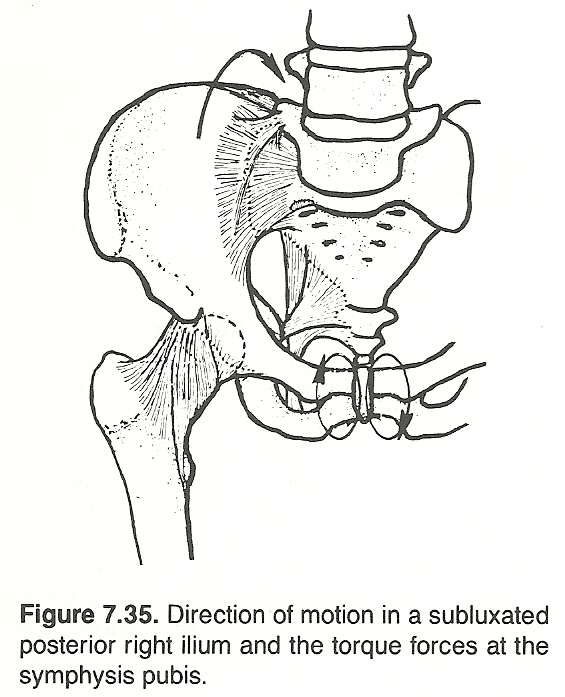 |
Local pain and acute tenderness are rarely seen contralaterally in chronic cases unless the fixated site is irritated by trauma. Old lesions appear to enjoy confusing the examiner by referring signs and symptoms far above or below. Roentgenography is helpful, but rarely is it an end in itself. Thus, signs of immobility, the results of stress tests, and signs of spinal balance are the most reliable clues.
Kaplan and associates found that a radiculopathic process on the convex side is associated with idiopathic thoracic scoliosis. EMG studies of the erector spinae muscles showed the radiculopathy to be maximal near the apex of the curve. It was thought at one time that a polyneuropathy or polyneuritis was involved in the development of adolescent idiopathic scoliosis. This theory, however, has been shown by nerve conduction velocity studies conducted by Sahlstrand/Sellden to be false.
Abrahams VC:
Several authorities say sacroiliac pain will always be on the side of hypermobility, while others of equal credentials place the pain on the side of fixation. Some say the side of fixation is always the major, while others say that the side of hypermobility is always the major because the joint is normally hypomobile. This confuses everybody except the mentor's disciples. It is this author's opinion that the typical pain of sacroiliac stress is diffuse across the sacroiliac area and most difficult for the patient to isolate with a finger. The palm of the hand is usually used.
It is not uncommon for referred pain to detour from textbook descriptions (eg, gallbladder distress does not always refer to the right scapula, anginal pain does not always refer to the left arm). Even palpable tenderness may be referred. The most reliable clues are the site of consistently increased pain on biomechanical stress tests and, conversely, opposite maneuvers that relieve pain, tenderness, and structural imbalance. When dealing with individual patients, each of which is unique, the doctor is best directed by what is found true in the situation at hand and not on the theories of other doctors that are based upon their patients.
Coccyx Syndromes
The terminal of the spinal cord is attached to the cornua of the coccyx. As the segment moves anteriorly, the apex of the sacrum acts as a fulcrum. As the cornua moves backward and downward, traction is applied to the spinal cord. Thus, symptoms from the resulting cord tension need not be confined to the pelvic region alone (eg, occipital headaches, torticollis).
An irritating coccygeal displacement referring pain to the sacroiliac area is more common among women than men. Coccygodynia may be from mild to severe, and urogenital, rectal, and sciatic-like complaints, along with general nervousness, may be related. Associated pain is usually far greater than the degree of displacement would indicate. In traumatic situations, pain and local levator ani spasm may be pronounced and often episodic. Local tenderness is consistently present, and pain is aggravated by pressure in the direction of displacement.
Pubic Syndromes
Pubic sprain and subluxation are often mistaken for sacroiliac slip, although sacroiliac displacement may have occurred and been spontaneously reduced. The disorder is also associated with lateral hip subluxations. In primary pubic subluxation (essentially torsional), the predominant evidence will be found at the pubic symphysis. The sacroiliac area will not be excessively tender, but acute tenderness will be found over the painful pubis. After severe trauma, pubic and sacroiliac displacement may coexist. Anatomically, they must exist together, but one joint may be more acutely involved than the other.
NEUROLOGIC ASPECTS OF SCOLIOSIS
The Node Theory
After studying the range of motion from the atlas to the sacrum in 30 cadaveric spines, Kashimoto and associates determined that individual spines had a characteristic level-dependent difference in the capacity for elementary motions at the facet joints. Segments with restricted motion capacity were called spinal nodes.
The human spine was usually found to have three or four spinal nodes between the skull and the sacrum. Their located was determined at C7–T1, T4–T5, T8–T9, and T11–T12 levels. This intrinsic structural character of the human spine is expressed as "nodal motion structure" by these researchers whom postulated that this state plays an important role in the formation of curve patterns in idiopathic scoliosis and other spinal deformities. It should be noted that Gillet, Illi, King, and Ward have frequently pointed out the high incidence of subluxation-fixation at similar areas.
Spinal Cord Maladaptation
A survey by Lloyd-Roberts and associates has shown that idiopathic structural scoliosis of mild degree is generally not progressive. These researchers report that although the spinal cord is displaced toward the concavity of a scoliotic curve, it does not rotate in company with the vertebrae. This exposes the involved nerve roots to traction and possible entrapment. It is suggested that progression occurs when the neuraxis is unable to adjust to the change in the anatomy of the vertebral column: a significant increase in degenerated cells was demonstrated in the posterior root ganglia at the apex of the curve on the convex side.
Equilibrium Sway Effects in Scoliosis
In an analysis by Sahlstrand and associates of sagittal, lateral, and total postural sway when erect, the patterns of scoliotic children were compared to those of healthy children. Scoliotic patients had significantly poorer postural control, especially in tests in which the proprioceptive functions were most important for maintaining postural equilibrium.
Patients with a left convex curve had more pronounced reactions quantitatively than patients with a right convex curve, and patients with small curvatures had significantly increased postural sway compared with patients with more severe deformity. It was concluded that these facts together with findings in patients with double primary curves, and the result of studies of brace effects, indirectly indicate the possibility of postural disequilibrium as a contributory cause in adolescent scoliosis. This observation appears to support reports of those who specialize in upper-cervical techniques.
Scoliosis Presenting with Severe Low-Back Pain
The incidence of low-back pain appears to be the same in patients with or without obvious spinal deformity. However, the degree of pain experienced may vary.
Jackson and associates found that patients with major lumbar curves had more pain, and the area of complaint was frequently below the site of the major deformity. The most painful and disabling patterns concerned the compensatory lumbosacral curves. It appeared that the pain originated from the concavity side of the curve and included discogenic, facet joint, and radicular origins.
Kostuik/Bentivoglio found that as the degree of curvature increased, the severity of pain increased, especially for curves of 45ş or larger. They also reported that:
(1) the presence of facet sclerosis correlated with a history of pain in 64% of the cases, and
(2) there was a high correlation between radiologic changes to the incidence of pain.
Prophylactic surgery to prevent future back pain in patients having abnormal lumbar curves is generally not justified. Nachemson reports that whether severe low-back pain occurs more often in patients who have distorted lumbar curves than in those whose spines are straight is open to question since calculations show approximately the same incidence of surgery for back pain in scoliotic patients and in those whose spines are straight. Because surgery for scoliosis in the adult carries a high risk and long-term efficacy is unproved, he recommends that all types of conservative measures be tried before considering an operation. However, if unremitting pain from root entrapment occurs (eg, foraminal compression, pedicular kinking) or a painful degenerative scoliosis develops in the elderly, referral for surgical decompression may be the only alternative.
Taylor believes that instances of scoliosis-related pain, especially night pain, are often related to underlying pathology (eg, spinal tumor, osteoblastoma, severe spondylolisthesis).
BIBLIOGRAPHY:
Sensory and motor specialization in some muscles of the neck.
TINS, 4(1):24-27, 1981.
Aiken P:
Meralgia paresthetica.
Orthopedic Brief, ACA Council on Orthopedics, date not shown.
Albrand OW, Corkill G:
Thoracic disc herniation: treatment and prognosis.
Spine, 4:41-46, 1979.
Bailey RW:
The Cervical Spine.
Philadelphia, Lea & Febiger, 1974, pp 91-97.
Baklavadzhyan OG, Arutyunyan AG, Darbinyan AG:
Influence of cervical sympathetic nerve and hypothalamus on direct cortical response.
Neuroscience Translations, :403-410, 1967.
Baloh RW:
Dizziness: Matching the symptoms to the source.
Diagnosis, 5(11):81-98, 1983.
Barge FH:
Scoliosis.
Davenport, IA, Bawden Bros, 1982, pp 119-129, 146, 227-233.
Barge FH:
Tortipelvis.
Davenport, IA, Bawden Bros, 1980, pp 101-102.
Barge FH:
Torticollis.
Davenport, IA, Bawden Bros, 1979.
Barker ME:
Manipulation in general medical practice for thoracic pain syndrome.
British Osteopathic Journal, 15(2):95-97, 1983.
Benner B, Ehni G:
Degenerative lumbar scoliosis.
Spine, 4:548-552, 1979.
Benson DR:
The back: thoracic and lumbar spine.
In D'Ambrosia RD: Musculoskeletal Disorders: Regional Examination and Differential Diagnosis.
Philadelphia, J.B. Lippincott, 1977, pp 308-309.
Blits J:
Thoracic disk herniation.
Ortho Briefs, ACA Council on Chiropractic Orthopedics, Spring 1982, pp 8-9.
Blumenthal LS:
Injury to the cervical spine as a cause of headache.
Postgraduate Medicine, 56:147-152, 1974.
Boake HK:
Cervical headache.
Canadian Family Physician, 18:75-76, 1978.
Bogduk N:
The clinical anatomy of the cervical dorsal rami.
Spine, 7(4):19-30, 1982.
Bogduk N:
Lumbar dorsal ramus syndrome.
Medical Journal of Australia, 2:537-541, 1980.
Bohlman HH:
The neck.
In D'Ambrosia RD (ed): Musculoskeletal Disorders: Regional Examination and Differential Diagnosis.
Philadelphia, J.B. Lippincott, 1977, pp 192-193, 203-204.
Bohlman HH:
The pathology and current concepts of cervical spine injuries: a critical review of 300 cases.
Journal of Bone & Joint Surgery, 54A:1363, 1972.
Bradford DS, Moe JH, Winter RB:
Scoliosis.
In Rothman RH, Simeone FA (eds): The Spine.
Philadelphia, W.B. Saunders, 1975, Vol I, pp 276, 281-283.
Brain, Lord, Wilkinson (eds):
Cervical Spondylosis.
London, Heinemann, 1967.
Breig A:
Adverse Mechanical Tension in the Central Nervous System.
Stockholm, Almquist & Wikell, 1978.
Breig A:
Biomechanics of the Central Nervous System: Some Basic Normal and Pathological Phenomena.
Stockholm, Almquist & Wiksell, 1960.
Breig A:
Overstretching of, and circumscribed pathological tension in, the spinal cord a basic cause of symptoms in cord disorders.
Journal of Biomechanics, 3:7, 1970.
Breig A, Turnbull I, Hassler O:
Effects of mechanical stress on the spinal cord in cervical spondylosis.
Journal of Neurosurgery, 15:45, 1966.
Bridge CJ:
Innervation of spinal meninges and epidural structures.
Anatomical Record, 133:533-561, 1959.
Brodal A:
Neurological Anatomy in Relation to Clinical Medicine, ed 2. London,
Oxford University Press, 1969.
Brunarski DJ:
Functional considerations of spinal manipulative therapy.
ACA Journal of Chiropractic, May 1980.
Buehler MT:
Spinal stenosis.
Journal of Manipulative and Physiological Therapeutics, 1(2), June 1978.
Burke GL:
The etiology and pathogenesis of pain of spinal origin.
Applied Therapeutics, pp 863-867, October 1966.
Cailliet R:
Low Back Pain Syndrome, ed 3.
Philadelphia, F.A. Davis, 1981, pp 21, 25, 44-51.
Cailliet R:
Neck and Arm Pain.
Philadelphia, F.A. Davis, 1974, pp 17-20, 61.
Cailliet R:
Scoliosis.
Philadelphia, F.A. Davis, 1975, pp 1-3, 99-105.
Cailliet R:
Soft Tissue Pain and Disability.
Philadelphia, F.A. Davis, 1980, pp 120-121, 128-130.
Calin A:
Back pain: mechanical or inflammatory.
American Family Physician, 20: 97-100, 1979.
Canadian Memorial Chiropractic College:
Segmental Neuropathy.
Toronto, Canadian Memorial Chiropractic College, date of publication not shown. Monograph.
Carnett JB:
The simulation of gallbladder disease by intercostal neuralgia of the abdominal wall.
Annals of Surgery, 86(5):747-757, 1927.
Causey G:
The effect of pressure on nerve fibers.
Journal of Anatomy, 82:262-270, 1948.
Causey G, Palmer E:
The effect of pressure on nerve conduction and nerve fiber size.
Journal of Physiology (British), 109:220-231, 1949.
Chrisman OD, Gervais RF:
Otologic manifestations of the cervical syndrome.
Clinical Orthopedics, 24:34-38, 1962.
Chusid JG:
Correlative Neuroanatomy & Functional Neurology, ed 19.
Los Altos, CA, Lange Medical, pp 68, 297.
Coggins WN:
Basic Technique: A System of Body Mechanics.
Creve Coeur, MO, published by author, 1983.
Cole WV:
The effects of the atlas lesion after 96 hours and after 6 weeks.
Journal of the American Osteopathic Association, 48(1):7-9, 1948.
Cole WV:
The osteopathic lesion syndrome (VIII): the effects of an experimental vertebral lesion on the gross structure of the atlanto-occipital region.
Journal of the American Osteopathic Association, 49(9):447-450, 1949.
Cyriax J:
Dural pain.
Lancet, 1(8070):919-921, 1978.
Cyriax J:
Lumbago: Mechanism of dural pain.
Lancet, 249:427-429, 1945.
Cyriax J:
Textbook of Orthopaedic Medicine; Vol one, Diagnosis of Soft Tissue Lesions, ed 8.
London, Bailliere Tindall, 1982, pp 297-298.
Davis D:
A common type of vertigo relieved by traction of the cervical spine.
Annals of Internal Medicine, 38:778-786, 1953.
Deering ID, Ling TH, McCouch GP:
Location of receptors for tonic neck reflexes.
Journal of Neurophysiology, 14:191-195, 1951.
De Rusha JL:
Upper cervical technic correlated with neurodiagnosis.
ACA Journal of Chiropractic, September 1961.
De Sterno CV:
The pathophysiology of TMJ dysfunction and related pain.
In Gelb H (ed): Clinical Management of Head, Neck and TMJ Pain and Dysfunction.
Philadelphia, W.B. Saunders, 1977.
Dionne J:
Neck torsion nystagmus.
Canadian Journal of Otolaryngology, 3(1):37-41, 1974.
Dittmar E:
Cutaneo-visceral neural pathways.
British Journal of Physical Medicine, 15:208, 1952.
Dove CI:
The occipito-atlanto-axial complex.
Manuelle Medizin, 20:11-15, 1982.
Droz JM:
The discoradicular conflict and the radicular involvement in the intervertebral foramen.
Annals of the Swiss Chiropractors' Association, 2:23-49, 1961.
Drum DC:
The vertebral motor unit and intervertebral foramen.
In Goldstein M (ed): The Research Status of Spinal Manipulative Therapy.
Bethesda, MD, National Institutes of Health, 1975, pp 63-70.
Dvorak J, Orelli FV:
How dangerous is manipulation of the cervical spine: Case report and results of an inquiry.
Manuelle Medizin, 20:44-48, 1982.
Edgar MA, Nundy S:
Innervation of the spinal dura mater.
Journal of Neurology, Neurosurgery, and Psychiatry, 29:53004, 1966.
Epstein BS:
The Spine: A Radiological Text and Atlas.
Philadelphia, Lea & Febiger, 1962, pp 268-269.
Epstein JA, Epstein BS, Jones MD.
Symptomatic lumbar scoliosis with degenerative changes in the elderly.
Spine, 4:542-547, 1979.
Evans DC:
Biomechanics of spinal injury.
In Gonzna ER, Harrington IJ: Biomechanics of Musculoskeletal Injury.
Baltimore, Williams & Wilkins, 1982, pp 165-172, 183-185, 204-212.
Farady JA:
Current principles in the nonoperative management of structural adolescent idiopathic scoliosis.
Physical Therapy, 63:512-523, 1983.
Farfan HF, et al:
The effects of torsion on the lumbar intervertebral joints: The role of torsion in the production of disc degeneration.
Journal of Bone and Joint Surgery, 52A:468, 1970.
Farfan HF:
Mechanical Disorders of the Low Back.
Philadelphia, Lea & Febiger, 1973.
Farfan HF:
Symptomatology in terms of the pathomechanics of low-back pain and sciatica.
In Haldeman S (ed): Modern Developments in the Principles and Practice of Chiropractic.
New York, Appleton-Century-Crofts, 1980.
Farkas A:
The pathogenesis of idiopathic scoliosis.
Journal of Bone and Joint Surgery, 36:617, 1954.
Fernandez JL:
The transport of protein in nerves.
ACA Journal of Chiropractic, 10:17-24, 1972.
Fielding JW:
Dynamic anatomy and cineradiography of the cervical spine.
In Bailey RW (ed): The Cervical Spine.
Philadelphia, Lea & Febiger, 1974.
Finneson BE:
Low Back Pain.
Philadelphia, J.B. Lippincott, 1973, pp 19-34, 93-132, 332.
Fisk JW:
The Painful Neck and Back.
Springfield, IL, Charles C. Thomas, 1977, pp 28-32, 35-37, 81-84.
Fitz-Ritson DE:
The direct connections of the C2 dorsal ganglia in the brain stem of the squirrel.
Journal of the Canadian Chiropractic Association, 23(4): 131-137, 1979.
Foutz CA:
Functional vascular changes affecting the posterior-inferior cerebellar artery.
Journal of the National Chiropractic Association, 30:13-14, 1960.
Freedman BG:
The biodynamical aspect of cerebrospinal fluid in disease and health.
Journal of Manipulative and Physiological Therapeutics, 2:79-84, 1979.
Fried LC, Doppman JL, Chiro G:
Direction of blood flow in the primate cervical spinal cord.
Journal of Neurosurgery, 33:325, 1970.
Frykholm R:
The clinical picture: cervical migraine.
In Hirsch C, Zotterman Y (eds): Cervical Pain.
Oxford, England, Pergamon Press, 1972, pp 5-16.
Frymoyer JW, Pope MH:
The role of trauma in low back pain: a review.
Journal of Trauma, 18:628-633, 1978.
Gayral L, Neuwirth E:
Clinical manifestations of the autonomic nervous system sequential to osteoarthritis of the cervical spine.
Lancet, pp 197-198, May 1958.
Gayral L, Neuwirth E:
Oto-neuro-ophthalmologic manifestations of cervical origin.
New York State Journal of Medicine, 54:1920-1926, 1954.
Gehweiler JA Jr, Osborne RL Jr, Becker RF:
The Radiology of Vertebrae Trauma.
Philadelphia, W.B. Saunders, 1980, pp 76-78.
Gelb H:
Patient evaluation.
In Gelb H (ed): Clinical Management of Head, Neck and TMJ Pain and Dysfunction.
Philadelphia, W.B. Saunders, 1977.
Gershon-Cohen J, Budin E, Glauser F:
Whiplash fractures of cervicodorsal spinous processes.
Journal of the American Medical Association, 155:560, 1954.
Giles LGF:
Lumbosacral facetal "joint angles" associated with leg length inequality.
Rheumatology and Rehabilitation, 10:223-238, 1981.
Giles LGF, Taylor JR:
The effect of postural scoliosis on lumbar apophyseal joints.
Scandinavian Journal of Rheumatology, 13:209-220, 1984.
Giles LGF:
Vertebral-basilar artery insufficiency.
Journal of the CCA, 21:112-17, 1977.
Gillet H:
The anatomy and physiology of spinal fixation.
Journal of the National Chiropractic Association, December 1963.
Gillet H:
Evolution of a chiropractor.
National Chiropractic Journal, November 1945, January 1949, December 1949, January 1951.
Gillet H, Liekens M:
Belgian Chiropractic Research Notes.
Huntington Beach, CA, Motion Palpation Institute, 1981, pp 11-39, 61-69, 71, 79-80, 92-100, 104-106.
Gillet H, Liekens, M:
A further study of spinal fixations.
Annals of the Swiss Chiropractors' Association, IV:41, 1967.
Gitelman R, Fitz-Ritson D:
Acceleration/deceleration injuries (whiplash).
ACA Journal of Chiropractic, 17:68, April 1983.
Gitelman R, Fitz-Ritson D:
Vertebrogenic headaches.
ACA Journal of Chiropractic, 20(2):74-75, 1983.
Glasgow EF, Twomey LT, Scull ER, Kleynhans AM, Idczak RM:
Aspects of Manipulative Therapy, ed 2.
New York, Churchill Livingstone, 1985, pp 55-58, 109-122, 128-151.
Glerak RA:
Vertebral artery compression and vascular insufficiency of the brain.
Archives of California Chiropractic Association, 2:28-39, 1972.
Goldthwait JE, et al:
The Essentials of Body Mechanics in Health and Disease, ed 5.
Philadelphia, J.B. Lippincott, 1952.
Goodheart GJ:
The cervical challenge.
Digest of Chiropractic Economics, 15(2): 36-39, 1972.
Granit R, Leksell L, Skoglund CR:
Fibre interaction in injured or compressed nerves.
Brain, 67:125-140, 1944.
Grieve GP:
Common Vertebral Joint Problems.
New York, Churchill Livingstone, 1981, pp 10, 17-33, 24-35, 56-59, 47, 48, 53-55, 60-62, 90-92, 134, 163-170, 176-196, 198.
Gunn CC, Milbrandt WE:
Early and subtle signs in low-back pain.
Spine, 3:267-281, 1978.
Guth L:
Degeneration and regeneration of taste buds.
In Handbook of Sensory Physiology: Vol 4, Chemical Senses.
Berlin, Springer-Verlag, 1969.
Hadley LA:
Anatomico-Roentgenographic Studies of the Spine.
Springfield, IL, Charles C. Thomas, 1981, pp 69-113, 162.
Hadley LA:
Constriction of the intervertebral foramen.
Journal of the American Medical Association, 140(5):473-476.
Hadley LA:
Intervertebral joint subluxation, bony impingement and foramen encroachment with nerve root changes.
American Journal of Roentgenology, 65(3):377-402, 1951.
Hanflig SS:
Pain in the shoulder girdle, arm and precordium due to foraminal compression of nerve roots.
Archives of Surgery, 46:652-663, 1963.
Hardy AG, Elson R:
Practical Management of Spinal Injuries, ed 2.
New York, Churchill Livingstone, 1976.
Hargrave-Wilson W:
The cervical syndrome.
Australian Journal of Physiotherapy, 18:144-147, 1972.
Hasue M, Kikuchi S, Sakuyama Y, Ito T:
Anatomic study of the interrelation between lumbosacral nerve roots and their surrounding tissues.
Spine, 8:50-58, 1983.
Helfet AJ, Gruebel Lee DM:
Disorders of the Lumbar Spine.
Philadelphia, J.B. Lippincott, 1978, pp 24-25, 27-30, 145-161, 170-182.
Henderson DJ:
Significance of vertebral dyskinesia in relation to the cervical syndrome.
Journal of Manipulative and Physiological Therapeutics, 2(1):3-13, March 1979.
Hewit W:
The intervertebral foramen.
Physiotherapy, 56(8):332-336, 1970.
Hilton RC, Bail J:
A systematic pathological study of the dorsolumbar spine.
Journal of Rheumatology, 9:95-96, 1983.
Hoff J, et al:
The role of ischemia in the pathogenesis of cervical spondylotic myelopathy.
Spine, 2:100, 1977.
Homewood AE:
The Neurodynamics of the Vertebral Subluxation, ed 3.
Place of publication not shown, published by author, 1981, pp 39, 125-126, 147-161, 167-249.
HIlse M:
Disequilibrium caused by a functional disturbance of the upper cervical spine: clinical aspects and differential diagnosis.
Manuelle Medizen, 1(1): 18-23, 1983.
Howe JW:
Determination of lumbo-sacral facet subluxations.
Roentgenological Briefs, Council on Roentgenology of the American Chiropractic Association, Des Moines, IA, date not shown.
Illi FW:
The Vertebral Column:
Life-Line of the Body.
Chicago, National College of Chiropractic, 1951.
Jackson H:
Diagnosis of minimal atlanto-axial subluxations.
British Journal of Radiology, 23:672, 1950.
Jackson RP, Simmons EH, Stripinis D:
Incidence and severity of back pain in adult idiopathic scoliosis.
Spine, 8:749-756, 1983.
Janse J:
History of the development of chiropractic concepts; Chiropractic terminology.
In Goldstein M (ed): The Research Status of Spinal Manipulative Therapy.
Bethesda, MD, National Institutes of Health, 1975.
Janse J:
Principles and Practice of Chiropractic.
Lombard, IL, National College of Chiropractic, 1976.
Jeffreys E:
Disorders of the Cervical Spine.
London, Butterworths, 1980.
Jepson O:
Dizziness originating in the column cervicallis.
Journal of the Canadian Chiropractic Association, 11(1):7-8, 1967.
Kale M:
The upper cervical specific.
Today's Chiropractic, part 1, pp 28-29, July-August 1984; part 2, pp 27-30, September-October 1984.
Kapandji IA:
Physiology of the Joints: The Trunk and Vertebral Column, ed 2.
New York, Churchill Livingstone, 1980, Vol three.
Kaplan PE, Sahgal V, Hughes R, Kane W, Flanagan N:
Neuropathy in thoracic scoliosis.
Acta Orthopaedica Scandinavica, 51:263-266, 1980.
Kashimoto T, Yamamuro T, Hatakeyama K:
Anatomical and biomechanical factors in the curve pattern formation of idiopathic scoliosis.
Acta Orthopaedica Scandinavica, 53:368-361, 1982.
Keggi, Granger, Southwick:
Vertebral artery insufficiency secondary to trauma and osteoarthritis of the cervical spine.
Yale Journal of Biology and Medicine, 38:471-478, 1966.
Keith WS:
"Whiplash" injury of the 2nd cervical ganglion and nerve.
Canadian Journal of Neurological Services, 12:133-137, 1986.
Khurana RK, Nirankari VS:
Bilateral sympathetic dysfunction in posttraumatic headaches.
Headache, 26:183-188, 1986.
Kelsey JL, White AA:
Epidemiology and impact of low back pain.
Spine, 5:133-142, 1980.
Kikuchi S, Hasue M, Nishiyama K, Ito T:
Anatomic and clinical studies of radicular symptoms.
Spine, 9(1):23-30, 1984.
Kimmel DL:
Innervation of spinal dura mater and dura mater of the posterior cranial fossa.
Neurology, 11:800-809, 1961.
King WE:
The King Concept: The Spinal Tetrahedron, ed 4.
Grand Forks, ND, published by author, 1985.
Kirkaldy-Willis WH:
Five common back disorders: How to diagnose and treat them.
Geriatrics, December 1978.
Kirkaldy-Willis WH:
Manipulation.
In Kirkaldy-Willis WH (ed): Managing Low Back Pain.
New York, Churchill Livingstone, 1983, pp 175-177.
Kirkaldy-Willis WH:
A more precise diagnosis for low back pain.
Spine, 4(2), March-April 1979.
Kirkaldy-Willis WH:
The relationship of structural pathology to the nerve root.
Spine, 9:49-52, 1984.
Kobayashi S, Waltz AG, Rhoton AL Jr:
Effects of stimulation of cervical sympathetic nerves on cortical blood flow and vascular reactivity.
Neurology, 21(3):297-302
Korr IM:
Discussion: Papers of Sidney Ochs and Davis E. Pleasure.
In Goldstein M (ed): The Research Status of Spinal Manipulative Therapy.
Bethesda, MD, National Institutes of Health, 1975, pp 203-207.
Korr IM (ed):
The Neurobiologic Mechanisms in Manipulative Therapy.
New York, Plenum Press, 1978, pp 8-10, 16-21, 57-58, 291-365.
Kostuik JP, Bentivoglio J:
The incidence of low-back pain in adult scoliosis.
Spine, 6:268-273, 1981.
Kovacs A:
Subluxation and deformation of the cervical apophyseal joints.
Acta Radiologica, 43:1-16, 1955.
Kraus H:
Muscular aspects of oral dysfunction.
In Gelb H (ed): Clinical Management of Head, Neck and TMJ Pain and Dysfunction.
Philadelphia, W.B. Saunders, 1977, pp 117-124.
Kunert W:
Functional disorders of internal organs due to vertebral lesions.
Ciba Symposium, 13(3), 1966.
Lamb DW:
The neurology of spinal pain.
Physical Therapy, 59:971-973, 1979.
Lay EM:
The osteopathic management of temporomandibular joint dysfunction.
In Gelb H (ed): Clinical Management of Head, Neck and TMJ Pain and Dysfunction.
Philadelphia, W.B. Saunders, 1977.
Leach RA:
The Chiropractic Theories, ed 2.
Baltimore, Williams & Wilkins, 1986, pp 45-46, 49-70, 74-84, 109-119, 121-129.
Lehman JJ:
Manual therapy in upper cervical spinal dysfunction: a clinical study.
Physiotherapy Canada, 30:302-304, 1978.
Levine M:
The Structural Approach to Chiropractic.
New York, Comet Press, 1964, p 85.
Lieb MM:
Oral orthopedics.
In Gelb H (ed): Clinical Management of Head, Neck and TMJ Pain and Dysfunction.
Philadelphia, W.B. Saunders, 1977, pp 32-71.
Lloyd-Roberts GC, Pincott JR, McMeniman P, Bayley IJL, and Kendall B:
Progression in idiopathic scoliosis: a preliminary report of a possible mechanism.
Journal of Bone & Joint Surgery, 60B:451-460, 1979.
Logan VF, Murray FM (eds):
Textbook of Logan Basic Methods (from the original manuscript of Hugh B. Logan).
St. Louis, Logan Chiropractic College, 1950.
Luttges MW, Gerren RA:
Compression physiology: Nerves and roots.
In Haldeman S (ed): Modern Developments in the Principles and Practice of Chiropractic.
New York, Appleton-Century-Crofts, 1980, pp 65-89.
MacEwen GD:
A look at the diagnosis and management of scoliosis.
Orthopaedic Review, 3:9, 1974.
MacEwen GD:
Experimental scoliosis.
In Zorab, PA (ed): Proceedings of the Second Symposium on Scoliosis: Causation.
Edinburgh, E & S Livingstone, 1969.
Macnab I:
Acceleration injuries of the cervical spine.
Journal of Bone & Joint Surgery, 46A:1797-1799, 1964.
Macnab I:
Backache.
Baltimore, Williams & Wilkins, 1977, pp 19-23, 28-30, 38-63, 69-79, 82-104, 133-207.
Macnab I:
Symptoms in cervical disc degeneration.
In The Cervical Spine Research Society: The Cervical Spine.
Philadelphia, Lippincott, 1983, pp 388-394.
Magnaes B, Hauge T:
Rheumatoid arthritis contributing to lumbar spinal stenosis.
Scandinavian Journal of Rheumatology, 7:215-218, 1978.
Markovich SE:
Pain in the head.
In Gelb H (ed): Clinical Management of Head, Neck and TMJ Pain and Dysfunction.
Philadelphia, W.B. Saunders, 1977.
Malik DD, et al:
Effectiveness of chiropractic adjustment and physical therapy to treat spinal subluxation,
ACA Journal of Chiropractic, June 1983.
Malik DD, et al:
Recovery from radiculalgia by chiropractic adjustment and physical therapy.
ACA Journal of Chiropractic, June 1984.
Mapstone T, Spetzler RF:
Vertebrobasilar insufficiency secondary to vertebral artery occlusion.
Journal of Neurosurgery, 56:581-583, 1982.
Maurer EL:
The thoraco-costal facet syndrome, with an introduction of the marginal line and the rib sign.
ACA Journal of Chiropractic, December 1976.
Mayer EG, Herrman G, Pfaffenrath V, Pollmann W, Auberger T:
Functional radiographs of the craniocervical region and the cervical spine: A new computer-aided technique.
Cephalgia, 5:237-243, 1985.
Mazzarelli JP (ed):
Chiropractic Interprofessional Research.
Torino, Italy, Edizioni Minerva Medica, 1983.
Reprinted in the United States by the International Chiropractors Association, Washington, DC, 1985.
McAlpine JE:
A discussion of the dentate ligament neural traction mechanism.
International Review of Chiropractic, pp 35-39, October-December 1980.
McKenzie JA:
The dynamic behavior of the head and cervical spine during "whiplash."
Journal of Biomechanics, 4:477-490, 1971.
McKenzie RA:
The Lumbar Spine: Mechanical Diagnosis and Therapy.
Waikane, NZ, Spinal Publications, 1981, pp 4-5, 87-90.
Mears DB:
Neurological syndrome linking the cervical spine with the dorsal-lumbar areas.
Digest of Chiropractic Economics, 14(7):28-29, 1972.
Meyermann R:
Possibilities of injury to the artery vertebralis.
Manuelle Medizin, 20:105-114, 1982.
Michelsson JE:
The development of spinal deformity in experimental scoliosis.
Acta Orthopaedia Scandinavia, Supplement 81, 1965.
Milne E:
Giddiness in vertebro-basilar arterial insufficiency.
Medical Journal of Anatomy, 55:417-418, 1968.
Moe JH, et al:
Scoliosis and Other Spinal Deformities.
Philadelphia, W.B. Saunders, 1978, p 467.
Moe JH, Kettleson DN:
Idiopathic scoliosis.
Journal of Bone & Joint Surgery, 52A:1509, 1970.
Mumenthaler M: Neurology, ed 2.
Translated by EH Burrows.
New York, Thieme-Stratton, 1983, pp 157-158.
Nachemson A:
Adult scoliosis and back pain.
Spine, 4:513-517, 1979.
Nachemson AL:
The lumbar spine, an orthopaedic challenge.
Spine, 1(1):59, 1976.
Naylor A:
Factors in the development of the spinal stenosis syndrome.
Journal of Bone & Joint Surgery, 61B:306-309, 1979.
Nelson WA:
personal correspondence.
San Francisco, CA, 1980.
Neuwirth E:
The vertebral nerve in the posterior cervical syndrome.
New York State Journal of Medicine, 55:1380, 1955.
Ochs S:
Axoplasmic flow in neurons.
In Gaito J (ed): Macromolecules and Behavior.
New York, Appleton-Century-Crofts, 1966.
Ochs S:
Axoplasmic transport.
In Tower DB (ed): The Basic Neurosciences.
New York, Raven Press, Vol 1, 1975, pp 137-146.
Ochs S:
A brief review of material transport in nerve fibers.
In Goldstein M (ed): The Research Status of Spinal Manipulative Therapy.
Bethesda, MD, National Institutes of Health, 1975, pp 189-194.
Ochs S:
Systems of material transport in nerve fibers (axoplasmic transport) related to nerve function and trophic control.
Annals of the New York Academy of Science, 228:202-223, 1974.
Olsson Y, Sourander P, Krist K:
Neuropathological aspect on root affection in the cervical region.
In Hirsch C, Zotterman Y (eds): Cervical Pain.
Oxford, England, Pergamon Press, 1972, pp 81-88.
Oppenheimer A:
Narrowing of the intervertebral foramina as a cause of pseudorheumatic pain.
Annals of Surgery, 106(3):428-438, 1937.
Palmateer DC:
Greater occipital-trigeminal syndrome.
Journal of Clinical Chiropractic, 2:46-48, 1972.
Pang LQ:
The otological aspects of whiplash injuries.
Laryngoscope, 81:1381-1387, 1971.
Penning L:
Functional Pathology of the Cervical Spine.
Amsterdam, Excerpta Medical Foundation, 1968.
Phillips RB:
Upper cervical biomechanics.
ACA Journal of Chiropractic, X:127-134, October 1976.
Pleasure D:
Nerve root compression: Effects on neural chemistry and metabolism.
In Goldstein M (ed): The Research Status of Spinal Manipulative Therapy.
Bethesda, MD, National Institutes of Health, 1975, pp 197-200.
Ponsetti IV, et al:
Biomechanical analysis of intervertebral discs in idiopathic scoliosis.
Journal of Bone & Joint Surgery, 54:1993, 1972; 56A, 1973.
Ponsetti IV, Friedman B:
Prognosis in idiopathic scoliosis.
Journal of Bone & Joint Surgery, 32A:381, 1950.
Poole PB:
Considerations of neurogenic pain.
Ortho Briefs, Council on Chiropractic Orthopedics of the American Chiropractic Association, Fall 1982.
Porter RW, Hibbert C, Wellman P:
Backache and the lumbar spinal canal.
Spine, 5:99-105, 1980.
Porter RW, Hibbert CS, Wicks M:
The spinal canal in symptomatic lumbar disc lesions.
Journal of Bone & Joint Surgery, 60B:485-487, 1978.
Porter RW, Park W:
Unilateral spondylolysis.
Journal of Bone & Joint Surgery (British), 64:344-348, 1982.
Rainer GW, Mayer J, Sadler TR, Dirks D:
Effect of graded compression on nerve conduction velocity.
Archives of Surgery, 107:719-721, 1973.
Reid JD:
Effects of flexion-extension movements of the head and spine upon the spinal cord and nerve roots.
Journal of Neurology, Neurosurgery and Psychiatry (British), 23:214. 1960.
Roaf R:
A study of the mechanics of spinal injuries.
Journal of Bone and Joint Surgery, 42B:810-823, 1960.
Roaf R:
Rotation movements of the spine with special reference to scoliosis.
Journal of Bone & Joint Surgery, 40-B:312-332, 1958.
Roaf R:
The basic anatomy of scoliosis.
Journal of Bone & Joint Surgery, 480: 786, 1966.
Roca PD:
Ocular manifestations of whiplash injuries.
Annals of Ophthalmology, 4(1):63-73, 1972.
Rothman RH, Simeone FA:
Lumbar disc disease.
In Rothman RH, Simeone FA (eds): The Spine.
Philadelphia, W.B. Saunders, 1975, Vol II, pp 476-506.
Ruge D, Wiltse LL (eds):
Spinal Disorders: Diagnosis and Treatment.
Philadelphia, Lea & Febiger, 1977.
Russell AS, Percy JS, Lentle BC:
Vertebral sclerosis in adults.
Annals of the Rheumatic Diseases, 37:18-22, 1978.
Ryan GMS, Cope S:
Cervical vertigo.
The Lancet, pp 1355-1358, December 1955.
Rydevik B, Brown MD, Lundborg G:
Pathoanatomy and pathophysiology of nerve root compression.
Spine, 9(1):7-15, 1984.
Sahlstrand T, Ortengren R, Nachemson A:
Postural equilibrium in adolescent idiopathic scoliosis.
Acta Orthopaedica Scandinavica, 49:354-365, 1978.
Sahlstrand T, Sellden U:
Nerve conduction velocity in patients with adolescent idiopathic scoliosis.
Scandinavian Journal of Rehabilitation Medicine, 12:25-26, 1980.
Sandoz R:
Some physical mechanisms and effects of spinal adjustments.
Annals of the Swiss Chiropractors Association, 6:91, 1976.
Sandoz R:
Some reflex phenomena associated with spinal derangements and adjustments.
Annals of the Swiss Chiropractors Association, 7:45, 1981.
Saternus KS, Fuchs V:
Is the artery vertebralis endangered in resuscitation.
Manuelle Medizin, 20:101-104, 1982.
Schafer RC:
Clinical Biomechanics: Musculoskeletal Actions and Reactions.
Baltimore, Williams & Wilkins, 1983, pp 215-220, 272-273, 289-319, 239-240, 336, 339, 381, 388, 399-401, 406, 427-430.
Schafer RC (ed):
Basic Chiropractic Procedural Manual, ed 4.
Arlington, VA, American Chiropractic Association, 1984, pp 3-5.
Schafer RC:
Symptomatology and Differential Diagnosis.
Arlington, VA, American Chiropractic Association, 1986, pp 335-337, 550-555, 729-732, 829-832, 906, 908.
Schaumberg HH, Spencer PS:
Pathology of spinal root compression.
In Goldstein M (ed): The Research Status of Spinal Manipulative Therapy.
Bethesda, MD, National Institutes of Health, 1975, pp 141-147.
Seeman DC:
C1 subluxation, short leg and pelvic distortion.
Upper Cervical Monograph, 2(5):1-5, 1978.
Shafar J:
The syndrome of the third neuron of the cervical sympathetics.
American Journal of Medicine, 40:97-109, 1966.
Sharpless SK:
Susceptibility of spinal roots to compression block.
In Goldstein M (ed): The Research Status of Spinal Manipulative Therapy.
Bethesda, MD, National Institutes of Health, 1975, pp 155-160.
Sheehan S, Bauer RB, Meyer JS:
Vertebral artery compression in cervical spondylosis, arteriographic demonstration during life of vertebral artery insufficiency due to rotation and extension of the neck.
Neurology, 10:968-986, 1960.
Simmons EH, Jackson RP:
The management of nerve root entrapment syndromes associated with the collapsing scoliosis of idiopathic lumbar and thoracolumbar curves.
Spine, 4:533-541, 1979.
Sjostrand J, Rydevik B, Lundborg G, McLean WG:
Impairment of intraneural microcirculation, blood nerve barrier and axonal transport in experimental nerve ischemia and compression.
In Korr IM (ed): The Neurobiologic Mechanisms in Manipulative Therapy.
New York, Plenum Press, 1978, pp 337-355,
Smith DM:
Vertebral artery. Roentgenological Briefs.
Council on Roentgenology of the American Chiropractic Association, date and number not shown.
Steer JC, Horney FD:
Evidence for passage of cerebrospinal fluid along spinal nerves.
Canadian Medical Association Journal, 98(2):71-74, 1968.
Steinbach LL:
Spinal Balance and Spinal Hygiene.
Pittsburgh, published by author, 1957.
Strang VV:
Essential Principles of Chiropractic.
Davenport, IA, Palmer College of Chiropractic, 1984, pp 104, 109-110.
Sunderland S:
Anatomical perivertebral influences on the intervertebral foramen.
In Goldstein M (ed): The Research Status of Spinal Manipulative Therapy.
Bethesda, MD, National Institutes of Health, 1975, pp 129-139.
Sunderland S:
The anatomy of the intervertebral foramen and the mechanisms of compression and stretch of nerve roots.
In Haldeman S (ed): Modern Developments in the Principles and Practice of Chiropractic.
New York, Appleton-Century-Crofts, 1980, pp 55-64.
Sunderland S:
Mechanisms of cervical nerve root avulsion in injuries of neck and shoulder.
Journal of Neurosurgery, 41:705-714, 1974.
Sunderland S:
Meningeal-neural relations in the intervertebral foramina.
Journal of Neurosurgery, 40(6):756-763, 1974.
Sweat RW:
Scanning palpation: cervical spine.
Today's Chiropractic, pp 23-24, January-February 1985.
Sweat RW, Sievert T:
Chiropractic and the vertebral arteries.
Today's Chiropractic, part 1, pp 45-48, September-October 1984; part 2, pp 23-24, November-December 1984.
Sweere JJ:
Clinical manifestations of lumbar spinal stenosis.
Orthopedic Brief, ACA Council on Chiropractic Orthopedics, June 1985.
Sweere JJ:
A method of physiological testing in the differential diagnosis of acute mechanical low back pain.
Orthopedic Brief, ACA Council on Chiropractic Orthopedics, September 1984.
Swezey RL:
The modern thrust of manipulation and traction therapy.
Seminars in Arthritis and Rheumatism, 12(3):326, 1983.
Taylor LF:
Painful scoliosis: A need for further investigation.
British Medical Journal. 292:120-122, 1986.
Toole J, Tucker SH:
Influence of head position upon cerebral circulation.
Archives of Neurology (AMA), 2:616-623, 1960.
Valentini E:
The occipito-cervical spine.
Annals of the Swiss Chiropractors' Association, 4:225-232, 1969.
Verner JR:
The Science and Logic of Chiropractic.
Englewood, NJ, published by author, 1941.
Von Torklus D, Gehle W:
The Upper Cervical Spine.
New York, Grune & Stratton, 1972.
Waddell G, McCulloch JA, Kummel E, Venner RM:
Nonorganic physical signs in low back pain.
Spine, 5:117-125, 1980.
Ward LE:
The Dynamics of Spinal Stress.
Long Beach, CA, SSS Press, 1980.
Watkins RJ:
Side effects of subluxation.
Digest of Chiropractic Economics, 24(4):32-35, 1982.
Weiss P:
Endoneurial edema in constricted nerve.
Anatomical Record, 86:491-522, 1943.
West HG Jr:
Physical and spinal examination procedures utilized in the practice of chiropractic.
In Haldeman S (ed): Modern Developments in the Principles and Practice of Chiropractic.
New York, Appleton-Century-Crofts, 1980, p 283.
West HG:
Vertebral artery considerations in cervical trauma.
ACA Journal of Chiropractic, pp 18-19, December 1968.
White AA, Panjabi MM:
Clinical Biomechanics of the Spine.
Philadelphia, J.B. Lippincott, 1978.
Whiting RJ:
Cervical spondylosis.
Roentgenological Briefs, Council on Roentgenology of the American Chiropractic Association, no date or number shown.
Will TE:
The biochemical basis of manipulative therapeutics: hypothetical considerations.
Journal of Manipulative and Physiological Therapeutics, 1(3):153-156, September 1978.
Wiltse LL, Guyer RD, Spencer CW, Glenn WV, Porter IS:
Alar transverse process impingement of the L5 spinal nerve: the far-out syndrome.
Spine, 9:31-41, 1984.
Wyke BD:
Articular neurology and manipulative therapy.
In Aspects of Manipulative Therapy.
Proceedings of Multidisciplinary International Conference on Manipulative Therapy,
Melbourne, Lincoln Institute of Health Science, Carlton, Victoria, Australia, August 1979, pp 67-72.
Wyke BD:
Clinical significance of articular receptor systems.
Annals of the Royal College of Surgeons of England, 60(2):137, 1978.
Wyke BD:
Neural aspects of pain therapy.
In Swerdlow IM (ed): The Therapy of Pain Current Status of Modern Therapy.
Lancaster, MTP Press, Vol 6.
Yamada K:
The dynamics of experimental posture.
Clinical Orthopaedics, 25:20-31, 1962.
Yamada K, et al:
A neurological approach to the etiology and treatment of scoliosis.
Journal of Bone & Joint Surgery, 53A:197, 1971.
Young G:
Chiropractic success in epileptic conditions.
ACA Journal of Chiropractic, 19(4):62-63, 1982.