

Comparative Effectiveness of Exercise, Acupuncture,
and Spinal Manipulation for Low Back PainThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: Spine (Phila Pa 1976). 2011 (Oct 1); 36 (21 Suppl): S120–130 ~ FULL TEXT
OPEN ACCESS Christopher J. Standaert , MD , Janna Friedly , MD , Mark W. Erwin , DC, PhD,
Michael J. Lee , MD, Glenn Rechtine , MD , Nora B. Henrikson , PhD, MPH,
and Daniel C. Norvell , PhD
Department of Rehabilitation Medicine,
University of Washington,
Seattle, WA 98104, USA.
cjs1@uw.eduSTUDY DESIGN: Systematic review.
OBJECTIVE: We sought to answer the following clinical questions:(1) Is structured exercise more effective in the treatment of chronic low back pain (LBP)
than spinal manipulative therapy (SMT)?
(2) Is structured exercise more effective in the treatment of chronic LBP than acupuncture?
(3) Is SMT more effective in the treatment of chronic LBP than acupuncture?
(4) Do certain subgroups respond more favorably to specific treatments?
(5) Are any of these treatments more cost-effective than the others?SUMMARY OF BACKGROUND DATA: Exercise, SMT, and acupuncture are widely used interventions in the treatment of chronic LBP. There is evidence that all of these approaches may offer some benefit for patients with chronic LBP when compared with usual care or no treatment. The relative benefits or cost-effectiveness of any one of these treatments when compared with the others are less well-defined, and it is difficult to identify specific subgroups of those with chronic LBP who may preferentially respond to a particular treatment modality.
METHODS: A systematic review of the literature was performed to identify randomized controlled trials comparing a structured exercise program, SMT, or acupuncture with one another in patients with chronic LBP.
RESULTS: Two studies were identified comparing the use of structured exercise with SMT that met our inclusion criteria. Although these studies utilized different approaches for the exercise and SMT treatment groups, patients in both groups improved in terms of pain and function in both studies. Using random-effects modeling, there was no difference between the exercise and SMT groups when the data from these studies were pooled. We identified no studies meeting our inclusion criteria that compared acupuncture with either structured exercise or SMT or that addressed the relative cost-effectiveness of these approaches in the treatment of patients with chronic LBP.
CONCLUSION: The studies identified indicate that structured exercise and SMT appear to offer equivalent benefits in terms of pain and functional improvement for those with chronic LBP with clinical benefits evident within 8 weeks of care. However, the level of evidence is low. There is insufficient evidence to comment on the relative benefit of acupuncture compared with either structured exercise or SMT or to address the differential effects of structured exercise, SMT, or acupuncture for specific subgroups of individuals with chronic LBP. There is also insufficient evidence regarding the relative cost-effectiveness of structured exercise, SMT, or acupuncture in the treatment of chronic LBP.
CLINICAL RECOMMENDATIONS: Structured exercise and SMT appear to offer equivalent benefits in the management of pain and function for patients with nonspecific chronic LBP. If no clinical benefit is appreciated after using one of these approaches for 8 weeks, then the treatment plan should be reevaluated and consideration should be given to modifying the treatment approach or using alternate forms of care. Strength of recommendation: Weak.There is insufficient evidence regarding the relative benefits of the acupuncture compared with either structured exercise or SMT in the treatment of chronic LBP.There is insufficient evidence to address differential effects of structured exercise, SMT, or acupuncture for specific subgroups of individuals with chronic LBP. There is insufficient evidence regarding the relative cost-effectiveness of structured exercise, SMT, or acupuncture in the treatment of chronic LBP.
Key words: acupuncture, chiropractic, comparative effectiveness, cost-effectiveness, exercise, low back pain, spinal manipulative therapy, systematic review
From the FULL TEXT Article
Introduction
Most people with chronic low back pain (LBP) are managed nonoperatively, but it is very difficult to know which, if any, of the myriad of treatment options available will be the most effective for a given patient. In part, this is related to the heterogeneity of the patient population. LBP can arise from a number of different anatomic structures or can be related to a large range of pathologic conditions in the spine, and people have highly variable responses to ongoing pain. Chronic pain can also be associated with significant physiologic, neurobiologic, and psychosocial changes that may vary substantially between individuals. If these multiple factors are considered alongside the large range of treatment options available, then it can be extremely challenging to match the right treatment to the right patient. The cost of this uncertainty is hardly insignificant. A recent review by Dagenais et al [1] found that nonphysician care, including physical therapy, chiropractic, and complementary alternative medicine, accounted for 30% of the direct medical costs for care of those with chronic LBP, equivalent to the amount attributed to inpatient, outpatient, surgical, and emergency medical care combined. Physical therapy alone accounted for 17% of the expenditures on chronic LBP, while the costs for surgery accounted for only 5%. [1]
Although there is clearly a critical need to identify which treatment options optimize clinical utility and cost-effectiveness for specific patients, much of the literature on the nonoperative management of chronic LBP consists of uncontrolled trials or comparisons of a particular intervention to ineffective forms of “usual care.” In addition, study patients are often clustered into mixed groups that dilute the effect of treatment on subsets of the population or they are selected by subjective criteria that limit the external validity of the findings. The purpose of this review is to assess the literature regarding comparative studies of specific noninterventional, nonoperative treatment approaches for chronic LBP, and to advance the process of selecting between specific treatments.
Three distinct, commonly utilized therapeutic modalities were chosen for study: exercise, spinal manipulative therapy (SMT), and acupuncture. These particular treatments were selected on the basis of author consensus after initial assessment of the available literature. Multiple systematic reviews are available on these approaches that provide an appropriate background for further evaluation. For each of these treatments, there are significant variations in how they are defined, applied, or practiced, as well as in the skill level and training of providers. In addition, they are all accompanied by a number of nonspecific effects through the very nature of how they are delivered. This does not limit the importance of understanding their role in clinical care, but it does make the assessment of their benefits more challenging.
EXERCISE
Exercise programs come in many forms and are delivered in a variety of settings, frequently with multiple cointerventions. Several recent systematic reviews have addressed the role of exercise in the treatment of LBP. In the work of van Middelkoop et al, [2] the authors concluded that the exercise was effective at reducing pain and increasing function compared with usual care with a small effect size. There was no evidence to indicate that one exercise approach was superior to others; however, and there were inadequate data on effects within specific subgroups. Although they also concluded that there was no difference between exercise and SMT in short- or long-term benefits for LBP, the studies included in their review did not all address comparisons between an isolated, structured exercise approach and SMT, particularly the delivery of high-velocity manipulation by trained providers. Cochrane reviews on exercise as a treatment for chronic LBP [3] and for preventing recurrences of LBP [4] have concluded that exercise is “slightly effective” at reducing pain and increasing function in adults with chronic LBP and that post-treatment exercise programs are more effective than no treatment at preventing recurrences of LBP. Overall, the level of evidence is low in these reviews, and the quality of the literature is relatively poor and hampered by heterogeneity of both treatment approaches and patient populations.
SPINAL MANIPULATION
The most recent Cochrane review of spinal manipulation in chronic LBP [5] concluded that SMT results in a small, statistically significant but not clinically significant improvement in pain and function in patients with chronic LBP compared with other treatments. The authors identified evidence of varying levels of quality indicating that SMT has a short-term effect on pain and disability when added to another treatment and felt there was a significant need for cost data. As with the exercise literature, this study and the work on which it is based are affected by heterogeneity in the patient populations studied and in the manipulative technique applied. What is referred to as SMT may include high-velocity thrust techniques, manual mobilization, or other specific techniques or even broad treatment approaches such as osteopathy, which cloud the actual treatment effect of specific manipulative techniques. Although a number of studies have assessed the physiologic effects of SMT, the proper role of this treatment modality remains elusive, as does the most appropriate use of this modality as compared with other nonoperative methods. [6–10]
ACUPUNCTURE
Traditional acupuncture is based on ancient Chinese philosophical beliefs regarding the flow of vital energy through the body along the discrete pathways termed meridians. In acupuncture treatment, specific points along these meridians are utilized to balance the energy flows within the body. Many different styles of acupuncture and adjunctive techniques have developed over time as its use has disseminated into other cultures. [11] Although its mechanism of action is poorly understood, acupuncture is widely utilized in the treatment of LBP. [12] Acupuncture may be superior or equivalent to medical care, [13] waiting list control, [14] or usual care. [15, 16] A systematic review by Furlan et al [11] found acupuncture to be more effective than no treatment or sham in the management of chronic LBP but not more effective than other conventional approaches. The authors of this study noted low-methodologic quality for most of the studies identified.
COST-EFFECTIVENESS
Given dramatic increases in medical costs and the questionable efficacy of a variety of treatments for LBP, [17, 18] it is increasingly important to include cost-effectiveness analyses in comparative effectiveness research. To date, the cost-effectiveness of many treatments for LBP, including SMT and acupuncture compared with structured exercise, has not been well-defined. Two recent systematic reviews have examined cost-effectiveness of a variety of treatments for LBP and highlight the major limitations of the existing literature on this topic. Dagenais et al [19] identified only 15 cost-utility analyses for any treatments associated with LBP, including surgical and nonsurgical interventions. Of these, no studies included SMT, two studies included acupuncture, and only two were performed in the United States. The authors concluded that there was not enough high-quality evidence to determine the relative cost-effectiveness of most treatments for LBP, including SMT and acupuncture. Most analyses were performed in the United Kingdom or other European countries with markedly different health care systems than the United States.
A similar systematic review by Lin et al [20] evaluated treatments endorsed by the clinical practice guidelines of the American College of Physicians and the American Pain Society, including interdisciplinary rehabilitation, exercise, acupuncture, massage, SMT, yoga, cognitive behavioral therapy, or relaxation for subacute or chronic LBP. This review identified 26 studies in total, although no additional studies were identified comparing SMT or acupuncture with other treatments for chronic LBP beyond those included in the review of Dagenais et al. [19] Despite the overlap in the studies that formed the basis of these reviews, Lin et al [20] reached conclusions contrary to those of Dagenais et al [19] finding that a variety of treatments for chronic LBP, including acupuncture and SMT, are relatively cost-effective. The inconsistencies in these reviews are emblematic of the need for high-quality cost-effectiveness studies comparing treatments for LBP, including exercise, SMT, and acupuncture, a need that is particularly acute within the context of the US health care system.
OBJECTIVES
The intent of this review was to evaluate the relative efficacy of structured exercise, SMT, and acupuncture in the treatment of chronic LBP and to assess the cost-effectiveness of these approaches. We sought to answer the following clinical questions:
Is structured exercise more effective in the treatment of chronic LBP than SMT?
Is structured exercise more effective in the treatment of chronic LBP than acupuncture?
Is SMT more effective in the treatment of chronic LBP than acupuncture?
Do certain subgroups respond more favorably to specific treatments?
Are any of these treatments more cost-effective than the others?
MATERIALS AND METHODS
Electronic Literature Database
We conducted a systematic search in MEDLINE and the Cochrane Collaboration Library for literature published through December 2010. The search results were limited to human studies published in the English language. Reference lists of key articles were also systematically checked to identify additional eligible articles. Considering the substantial literature on interventions for LBP, we limited our search to randomized controlled trials (RCTs) and meta-analyses that studied the interventions of interest. We included studies evaluating adult patients with chronic LBP with or without radiating pain for at least 3 months. In contrast to other published systematic reviews, we sought to identify studies where a clear comparison could be made between the interventions of interest (exercise, manipulation, and acupuncture) to avoid heterogeneity that often leads to little or no observed effect or effects that cannot be generalized to the clinical setting.

Table 1A

Table 1B Hence, we excluded studies with combination treatments (e.g. , manipulation and exercise, multimodality physical therapy). To avoid bias, we also excluded studies with selection criteria that were either too subjective, not applied in the typical clinical setting, or too strict to allow generalization to the larger population of patients with LBP (e.g., pain in a specific area of the spine required for inclusion) and studies whose data presentation did not allow separate analysis only of those with chronic LBP (Table 1).
For question 4, we assessed the RCTs that met the study criteria for questions 1 to 3 to identify those that included subgroup analysis stratifying one or more subgroups. Papers had to provide raw data for each treatment intervention by subgroup so that the heterogeneity of treatment effects could be evaluated, unless the authors reported specific tests for interaction.
For question 5, we searched for economic evaluation studies that compared treatments defined in questions 1 to 3. We limited our results to cost-effectiveness or cost-utility analyses and excluded cost-only studies. We excluded studies if the treatments of interest were not randomized, pediatric studies (< 18 years of age), and patients with cancer, inflammatory or systemic disease, instability, infection, or pregnancy. We also excluded studies where the treatment arms included multiple treatment modalities. We were interested in studies that evaluated the costs and the effectiveness of the specific treatment comparisons in questions 1 to 3.
Article Selection and Data Extraction
Two reviewers (N.H. and D.N.) independently reviewed each retrieved citation. After title and abstract review, we selected articles for full-text review that were(1) likely eligible articles or
(2) could not be excluded unequivocally from the title or abstract.
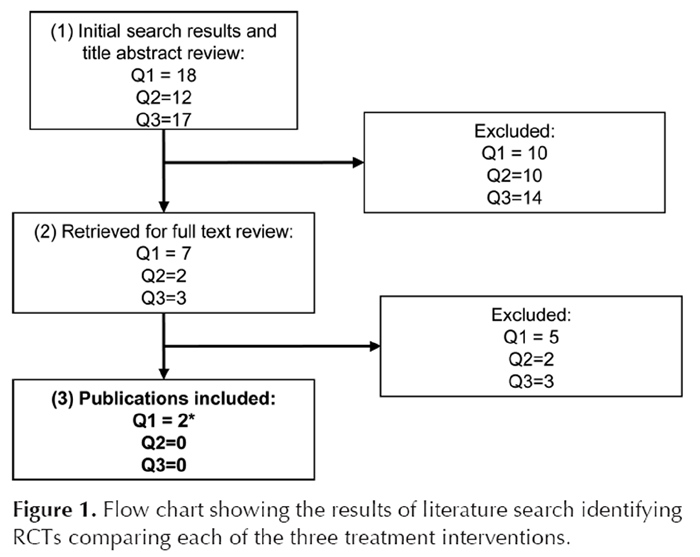
Figure 1
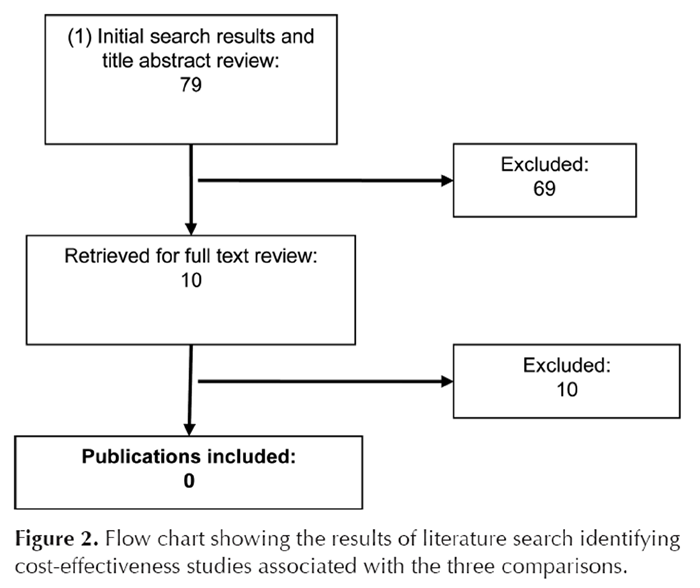
Figure 2 Full-text articles were reviewed independently by four reviewers (C.S., M.E., N.H., and D.N.); disagreements were resolved by consensus. Final-included articles were decided by consensus among the entire author team (Figures 1 and 2).
From the included articles, we extracted the following information: study design, population, diagnosis, intervention description, outcome measures, and relevant results.
Study Quality
Level of evidence ratings were assigned to each included article independently by two reviewers using criteria set by The Journal of Bone and Joint Surgery, American Volume (J Bone Joint Surg Am) 21 for therapeutic studies and modified to delineate criteria associated with methodologic quality and described elsewhere. [22]
Analysis
We performed all analyses on a study level. For pain visual analogue scales, we standardized all scales on a 0- to 10-point scale. We calculated the change scores and the corresponding standard deviations from pre- and postoperative pain and function scores reported by the authors. Study level data were pooled across studies if the treatment comparisons and outcomes were the same or similar and if sufficient data were provided to calculate effect sizes. The standardized mean differences (SMDs) comparing the overall treatment effects were calculated by subtracting the mean change scores and dividing by the change score standard deviations. The reporting of effect estimates facilitates the interpretation of the size of the effect of a specific treatment as opposed to the statistical significance. Both fixed-effect and random-effect estimates were performed for pooled data. Fixed-effects methods are based on the assumption that a single common effect underlies each study being pooled with no significant heterogeneity among the studies. Random-effects methods are based on the assumption that individual studies are estimating different treatment effects, reflective of heterogeneity. That is, random effects methods allow that the true effect could vary from study to study which accounts for both within- and between study error.
Overall Strength of Body of Literature
The initial strength of the overall body of evidence was considered high if the majority of the studies were level 1 or 2 and low if the majority of the studies were level 3 or 4. We downgraded the body of evidence one or two levels based on the following criteria:(1) inconsistency of results,
(2) indirectness of evidence, or
(3) imprecision of the effect estimates (e.g., wide confidence intervals).We upgraded the body of evidence one or two levels based on the following criteria:
(1) large magnitude of effect or
(2) dose-response gradient.The overall strength of the body of the literature was expressed in terms of our confidence in the estimate of effect and the impact that further research may have on the results. An overall strength of “high” means we have high confidence that the evidence reflects the true effect. Further research is very unlikely to change our confidence in the estimate of effect. The overall strength of “moderate” means that we have moderate confidence that the evidence reflects the true effect. Further research may change our confidence in the estimate of effect and may change the estimate. A grade of “low” means we have low confidence that the evidence reflects the true effect. Further research is likely to change the confidence in the estimate of effect and likely to change the estimate. Finally, a grade of “insufficient” means that evidence either is unavailable or does not permit a conclusion. A more detailed description of this process can be found in the “Materials and Methods” section. [22]
RESULTS
Manipulation Versus Exercise
For question 1 (manipulation vs. exercise), our systematic search identified 18 potential studies and 2 systematic reviews (Figure 1). We identified two additional studies published since the most recent review. [2] Among the 18 potential studies, we selected 7 for full-text review. [23–29] Among these, five were excluded for the following reasons: subjective selection criteria (tenderness over facet joints required), [27] lack of a clearly defined spinal manipulation group, [25] treatment intervention not randomized, [26] no structured exercise group and inclusion of patients with less than 3 months of LBP, [28] and lack of a clean exercise versus manipulation comparison. [23] Consequently, this question included two studies: one identified in the review by van Middelkoop et al [2] (Ferreira et al [24]) and the other published since that review (Cecchi et al. [29]).
Details of study characteristics and patient populations are in the supplementary digital material (see supplementary tables, Supplemental Digital Content 1, and Supplemental Digital Content 2.

Table 2A

Table 2B
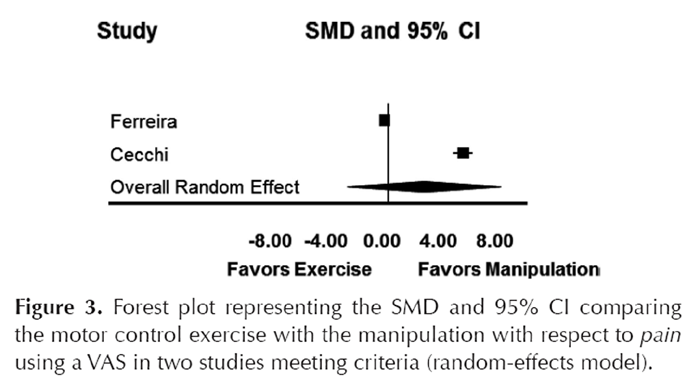
Figure 3
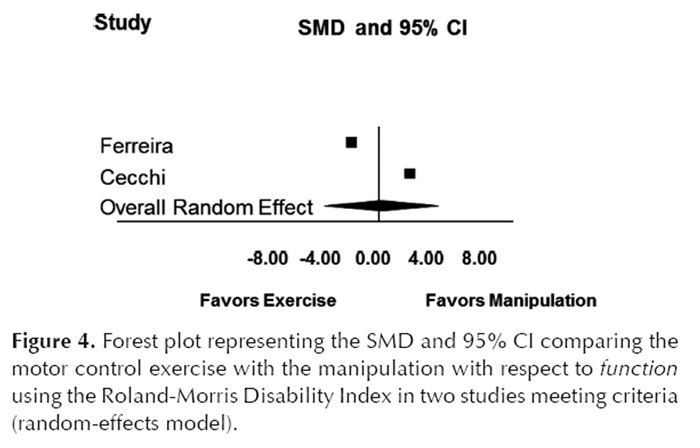
Figure 4 In the first included article, Ferreira et al [24] conducted an RCT of 240 adults with chronic LBP comparing SMT (defined as joint mobilization or manipulation applied to the spine or pelvis by a physical therapist), general exercises performed under supervision, and motor control exercises (focused on specific trunk muscles thought to control intersegmental motion in the lumbar spine). [24] Treatment was performed over an 8-week period with initial follow-up at 8 weeks and final follow-up at 12 months. Study outcomes were the patient specific functional scale, the global-perceived effect scale, pain (visual analog scale), Roland-Morris Disability Questionnaire score, and global-perceived effect scale. We summarized the visual analog scales and the Roland-Morris Disability Questionnaire scores as the other study in our review also reported these measures. Clinical improvement was noted in all groups at 8 weeks. At 12 months, there was no significant difference when comparing the motor control exercise group and the SMT group with respect to changes in pain (SMD = – 0.26; 95% confidence interval [CI]: – 0.57 to 0.51;) Table 2 and Figure 3). With respect to changes in function, the motor control exercise group was favored (SMD = – 2.07; 95% CI: – 2.46 to – 1.69) (Table 2 and Figure 4). Similar findings were observed with general exercise compared with SMT, although the relative change in function was less than that noted for the motor control exercise group (Table 2). The authors reported no significant difference between groups with respect to the patient-specific functional scale and global-perceived effect scale.
In the second included study, Cecchi et al [29] conducted an RCT of patients with chronic LBP assigned to receive a 3-week intervention of either back school (including “individual tailored” exercises) or mixed physiotherapy or a 4- to 6-week SMT intervention (performed via a “manual medicine approach” by physical medicine and rehabilitation specialists with approximately 10 years of experience). [29] Follow-up was for 12 months; the primary study outcomes were the Roland-Morris Disability Questionnaire score and secondary outcomes were pain, pain recurrence, further back pain treatment, and sick leave. Although change in pain (SMD = 5.32; 95% CI: 4.61–6.04) and function (SMD = 2.32; 95% CI: 1.89–2.76) favored the SMT group (Table 2 and Figures 3 and 4), further treatment for LBP during the follow-up period was significantly more frequent in the SMT group. Approximately 50% of this group received further SMT, and the exercise program provided in the “back school” was limited in scope and delivered only over the final 2 weeks of the program. In addition, a greater proportion of patients in the “back school” group were on sick leave due to their back pain at study inception.
The pooled analysis used the motor control exercise group instead of the general exercise group from the Ferreira et al study [24] since the effects were larger. We chose not to pool the two exercise groups from this study as they were distinct from one another. Any effect added by the general exercise group would move the difference closer to the null. When the two studies were pooled, spinal manipulation was favored slightly over motor control exercise (SMD = 0.632; 95% CI: 0.347–0.917) with respect to pain when using a fixed-effect model and no significant difference was observed when using a random-effects model (SMD = 2.52; 95% CI: – 2.95–8.0) (Table 2 and Figure 3). We are relying on the random-effects model for our conclusions due to the substantial differences between both the SMT and exercise interventions in the two studies and the significant heterogeneity in the treatment effects. Neither intervention was favored with both the fixed and random-effects models with respect to function (Table 2, Figure 4).
Acupuncture Versus Exercise
For question 2 (acupuncture vs. exercise), our initial search yielded 12 potential articles, 10 of which were excluded on the basis of our criteria (five did not include adequate exercise comparison group; three were not RCTs; two assessed pregnancy-related LBP). Two articles were selected for full text review; however, neither was selected for inclusion in our review [13, 30] (Figure 1). The study by Haake et al [13] included 1,162 patients and compared verum acupuncture, sham acupuncture, and “conventional care.” This article was excluded because the comparison group received a combination of drugs, physical therapy, and exercise. Interestingly, this study found that the “true” and “sham” acupuncture groups had equivalent degrees of improvement compared with the “conventional care” group. A smaller study of 52 patients by Yeung et al [30] comparing exercise alone to exercise with electro-acupuncture was excluded, because acupuncture was delivered as part of a combined treatment approach.
Acupuncture Versus Manipulation
For question 3 (acupuncture vs. manipulation), our initial search yielded 17 potential articles, 14 of which were excluded because they were not RCTs. Three were selected for full-text review; one was excluded because it did not include interventions of interest. [31] The remaining two articles were based on the same RCT [32, 33] and were excluded because patients had spine problems affecting the cervical, thoracic, and/or lumbar regions, not isolated chronic LBP, and the data were not presented in a manner that allowed for isolation of the patients with only LBP (Figure 1).
Subgroups and Cost-Effectiveness
For question 4 (subgroups), we examined the studies included for questions 1, 2, and 3 (total = two studies). Neither study included subgroup analyses. For question 5, cost-effectiveness studies evaluating treatment of chronic LBP, our initial search yielded 79 citations. Ten were selected for full-text review. All 10 articles were subsequently excluded from our review: two were review or methods articles [19, 34]; two did not meet our inclusion criteria for economic evaluations [35, 36]; two did not meet our patient-group criteria [37, 38]; and four did not meet our intervention criteria (Figure 2). [34, 39–41]
Evidence Summary

Table 3 The overall strength of the evidence evaluating the comparative effectiveness of the structured exercise versus SMT was “low.” That is, we have low confidence that the evidence reflects the true effect and further research is likely to change the confidence in the estimate of effect and likely to change the estimate (Table 3). The overall strength of the evidence evaluating the comparative effectiveness of the structured exercise versus acupuncture, SMT versus acupuncture, comparative subgroup effects, and cost-effectiveness comparing the aforementioned treatments was “insufficient.” That is, evidence is either unavailable or does not permit a conclusion.
DISCUSSION
Despite the high prevalence of LBP and the substantial societal and individual costs associated with it, there is very little clinical evidence from which to base comparative decisions for non-operative therapeutic options for a given patient. There are studies that support the benefit of many distinct approaches to chronic LBP, although there are also many studies that identify significant limitations for most treatments. There may well be substantial benefit to simply intervening in the pain state of individuals with chronic LBP, and the benefit associated with many treatments may be related to nonspecific effects. When considered as a whole, the evidence regarding the superiority of one treatment above others for specific patients is lacking. The problem is not necessarily that all non-operative approaches lack efficacy, but, rather, the problem may lie in the complexity of LBP and in the methodologic shortcomings of existing clinical studies.
Given the psychosocial complexities often associated with chronic pain, treatment approaches that address the psychologic functioning or fundamental belief systems of the patient regarding injury and recovery may be an important component of care for those who fail to respond to initial measures or who clearly have difficulties in this regard. Although multimodal approaches did not fall within the scope of this review, cognitive behavioral therapy may be a beneficial component of care for many patients when delivered in conjunction with more active treatments. [42, 43] Cognitive behavioral therapy is not necessarily a uniform therapeutic approach and can be delivered in many settings but generally has the primary goal of replacing maladaptive coping skills, beliefs, and behaviors with more appropriate systems. It is often a component of multidisciplinary pain programs and can also accompany structured exercise or physical therapy programs. [42, 44]
Overall, either comprehensive registries allowing for subject stratification or comparative clinical studies with rigorous design, identification of valid and identifiable subgroups and treatment arms with clearly defined interventions are a very high priority if we are to use nonoperative measures in the most efficacious and cost-effective manner.
EXERCISE VERSUS SPINAL MANIPULATIVE THERAPY
Exercise as a specific therapeutic intervention to treat LBP clearly could entail a broad range of approaches, and it may well be the case that different exercise programs are more appropriate for certain individuals. However, the current literature is not supportive of one particular exercise approach being superior to others in the treatment of chronic LBP. There may well be generalized effects from any type of structured exercise that infer benefits for those with chronic LBP. [2, 3, 45] Numerous RCTs have demonstrated the overall benefit of exercise to general health and a number of authors have noted the importance of overall fitness in LBP care and prevention. [46–49]
Similarly, many studies of SMT use variable approaches that are termed “manipulation,” often delivered with co-interventions or within the framework of a specific method of practice. In a more defined sense, SMT is a highly specific maneuver that requires considerable training and experience. A number of published studies indicate that SMT has some effectiveness in the treatment of acute and chronic back pain with respect to pain and return to function. [50] Clear delineation of the relative benefits of SMT and exercise would be beneficial for clinicians and patients.
We identified two studies meeting our inclusion criteria that compared the structured exercise with the SMT in the treatment of chronic LBP. Although the exercise and SMT interventions differed substantially between the studies, both treatment groups showed improvements in pain and function in both studies, indicating some potential benefit of each approach. However, the data provided by these studies are insufficient to establish if one of these treatments is superior to the other in the treatment of chronic LBP. As the clinical benefits of these approaches were evident within 8 weeks in the studies identified, it would seem reasonable to expect some degree of clinical improvement within this time frame for a given treatment. If there is no apparent benefit within 8 weeks, then the care plan should be reevaluated and consideration should be given to modifying the specific treatment approach or to utilizing alternate forms of care.
ACUPUNCTURE VERSUS MANIPULATION OR EXERCISE
Although there is some evidence that acupuncture may potentially offer benefit for those with LBP, [11] we did not identify any RCTs fulfilling our inclusion criteria that compared acupuncture with the manipulation or structured exercise in the treatment of chronic LBP. In the course of our literature review, we did encounter two RCTs comparing acupuncture to sham or the simulated acupuncture with “usual back care” [13, 51] that have been published since the date of the literature review by Furlan et al. [11] Both of these studies observed significant but equivalent benefit for acupuncture and sham or simulated acupuncture over “usual care” in the treatment of LBP. The lack of observed differences between acupuncture and simulated or sham acupuncture raises significant questions regarding the mechanism of action of this treatment, including the possibility of a dominant role of placebo response or other nonspecific effects. Additional high-quality comparative trials are needed to define the role of acupuncture in the treatment of chronic LBP, and these should likely include a sham or simulated treatment arm.
SUBGROUPS
As the number of comparative studies meeting our inclusion criteria was small, there were insufficient data from which to identify any subgroup that benefited from any specific treatment. This finding speaks to the substantial limitations of the medical literature in this regard. It may also speak to substantial problems in our medical classification of patients with chronic LBP. It is clear that the broad categorization of patients as having “chronic LBP” lacks the granularity needed for the researchers and the clinicians to be able to adequately study specific therapies. Further work on establishing clinically relevant, reliable methods of subgrouping individuals with chronic LBP is critically necessary. Appropriately structured registries may be one means of acquiring data that allows for the identification of valid clinical subgroups.
COST-EFFECTIVENESS
Unfortunately, there are very few published studies on the cost-effectiveness of treatments for LBP in general. The recent systematic reviews on this topic [19, 20] included studies on a wide variety of treatment modalities and came to conflicting conclusions despite largely relying on the same limited literature base. There is also controversy about the minimum effectiveness threshold (or alternatively, the maximum cost per quality adjusted life year gained) that is acceptable for the treatment of pain. This threshold could differ substantially depending on the severity and chronicity of symptoms, prevalence of disease, and societal views about rationing care. [52, 53]
We were unable to identify any studies of cost-effectiveness comparing exercise, SMT, or acupuncture that met our inclusion criteria. Although not specifically addressing chronic LBP, the UK back pain exercise and manipulation trial [38] was an interesting four-arm RCT that compared “best care” (i.e. , a standard of care providing education) with “best care” with structured group exercise, SMT, or SMT with group exercise. This study found that SMT, SMT with exercise, and “best care” could all potentially be considered cost-effective treatments for LBP depending on the maximum cost per quality adjusted life year threshold chosen (> Ł8700, between Ł8700 and Ł3800, or < Ł3800, respectively). The exercise-alone group demonstrated the clinical improvements as compared with “best care”, but to a lesser degree than the SMT groups and at a higher cost than the SMT with the exercise group. These higher costs for the exercise group were in large part due to the costs of additional physical therapy sessions as well as medical care that this group received. This study highlights the importance of defining cost-effectiveness thresholds to interpret comparative cost data. Clearly, there is a great need for additional cost-effectiveness studies of structured exercise, acupuncture, and SMT for chronic LBP.
CONCLUSIONS
Exercise therapy, SMT, and acupuncture may all have a role in the clinical management of patients with the chronic LBP. The overall evidence of benefit for any of these is not profound however, and we were unable to identify any evidence of comparative benefit of one of these over the others. Given the limitations of the literature, we are also unable to determine if they are truly equivalent, either. Acupuncture, in particular, is poorly addressed in the current literature, and evidence of equivalency between acupuncture and sham or simulated acupuncture in the treatment of LBP has implications regarding the use and mechanism of action of this treatment as well as for future study.
Further data are clearly necessary, and the establishment of the broad registries and the performance of high-quality studies on the comparative effectiveness of exercise, SMT, and acupuncture in the treatment of chronic LBP would appear to be priorities for clinicians, payers, and patients. Ideally, further clinical studies should include well-defined treatment arms, an identifiable and clinically relevant study population, appropriately trained providers, and enough subjects to allow for subgroup analyses and power to detect real differences. For exercise, a structured, active treatment program without co-interventions should be considered.
SMT should consist of a clearly defined method of manipulation performed by the appropriately trained and the experienced providers. Given the literature discussed above on acupuncture, treatment arms of established evaluation and treatment methods as well as sham or simulated acupuncture should be included. Either identifying valid subgroups a priori or obtaining thorough baseline demographics and diagnostic/clinical information in a large study group to allow post hoc analysis will be essential for identification of differential benefits for sub-populations. Cost data and long-term outcomes should be included in such studies to reliably assess clinical outcomes and cost-effectiveness over time.
Key Points
Structured exercise and SMT appear to offer equivalent benefits in the treatment
of chronic LBP, although the level of evidence in this regard is low.If there is no clinical improvement perceived within 8 weeks of initiating SMT
or a particular exercise treatment, then the care plan should be reevaluated.There is insufficient evidence in the medical literature to determine the relative
effectiveness of the acupuncture compared with either exercise or SMT
in the treatment of chronic LBP.There is insufficient evidence in the medical literature to determine the relative
cost-effectiveness of exercise, SMT, and acupuncture in the treatment of chronic LBP.Comprehensive registries and comparative clinical studies with rigorous design,
identification of valid and identifiable subgroups, and treatment arms with
clearly defined interventions are necessary if we are to optimize the clinical
and cost-effectiveness of non-operative care for the chronic LBP.
References:
Dagenais S , Caro J , Haldeman S. A systematic review of low back pain cost of illness studies in the United States and internationally. Spine J 2008; 8: 8–20.
van Middelkoop M , Rubinstein SM , Verhagen AP , et al. Exercise therapy for chronic nonspecific low-back pain. Best Pract Res Clin Rheumatol 2010; 24: 193–204.
Hayden JA , van Tulder MW , Malmivaara A , et al. Exercise therapy for treatment of non-specific low back pain. Cochrane Database Syst Rev 2005; CD000335.
Choi BK , Verbeek JH , Tam WW , et al. Exercises for prevention of recurrences of low-back pain. Cochrane Database Syst Rev 2010; CD006555.
Rubinstein SM , van Middelkoop M , Assendelft WJJ , de Boer MR , van Tulder MW. et al. Spinal manipulative therapy for chronic low-back pain. Cochrane Database Syst Rev 2011;(2): CD008112. doi: 10.1002/14651858.CD008112.pub2.
Haavik Taylor H , Murphy B. The effects of spinal manipulation on central integration of dual somatosensory input observed after motor training: a crossover study. J Manipulative Physiol Ther 2010; 33: 261–72.
Bialosky JE , Bishop MD , Robinson ME , et al. Spinal manipulative therapy has an immediate effect on thermal pain sensitivity in people with low back pain: a randomized controlled trial. Phys Ther 2009; 89: 1292–303.
Fritz JM , Koppenhaver SL , Kawchuk GN , et al. Preliminary investigation of the mechanisms underlying the effects of manipulation: exploration of a multi-variate model including spinal stiffness, multifi dus recruitment, and clinical findings [published online ahead of print March 15, 2011]. Spine (Phila Pa 1976). doi: 10.1097/BRS.0b013e318216337d.
Webb AL , Collins P , Rassoulian H , et al. Synovial folds—a pain in the neck? Man Ther 2011; 16: 118–24.
Dahm KT , Brurberg KG , Jamtvedt G , et al. Advice to rest in bed versus advice to stay active for acute low-back pain and sciatica. Cochrane Database Syst Rev 2010;(6): CD007612.
Furlan AD , van Tulder M , Cherkin D , et al. Acupuncture and dryneedling for low back pain: an updated systematic review within the framework of the Cochrane collaboration. Spine (Phila Pa 1976) 2005; 30: 944–63.
Cherkin DC , Sherman KJ , Deyo RA , et al. A review of the evidence for the effectiveness, safety, and cost of acupuncture, massage therapy, and spinal manipulation for back pain. Ann Intern Med 2003; 138: 898–906.
Haake M , Muller HH , Schade-Brittinger C , et al. German Acupuncture Trials (GERAC) for chronic low back pain: randomized, multicenter, blinded, parallel-group trial with 3 groups. Arch Intern Med 2007; 167: 1892–8.
Brinkhaus B , Witt CM , Jena S , et al. Acupuncture in patients with chronic low back pain: a randomized controlled trial. Arch Intern Med 2006; 166: 450–7.
Witt CM , Jena S , Selim D , et al. Pragmatic randomized trial evaluating the clinical and economic effectiveness of acupuncture for chronic low back pain. Am J Epidemiol 2006; 164: 487–96.
Thomas KJ , MacPherson H , Thorpe L , et al. Randomised controlled trial of a short course of traditional acupuncture compared with usual care for persistent non-specific low back pain. BMJ 2006; 333: 623.
Martin BI , Deyo RA , Mirza SK , et al. Expenditures and health status among adults with back and neck problems. JAMA 2008; 299: 656–64.
Weiner DK , Kim YS , Bonino P , et al. Low back pain in older adults: are we utilizing healthcare resources wisely? Pain Med 2006; 7: 143–50.
Dagenais S , Roffey DM , Wai EK , et al. Can cost utility evaluations inform decision making about interventions for low back pain ? Spine J 2009; 9: 944–57.
Lin CW , Haas M , Maher CG , et al. Cost- effectiveness of guidelineendorsed treatments for low back pain: a systematic review. Eur Spine J 2011;20: 1024–38.
Wright JG , Swiontkowski MF , Heckman JD. Introducing levels of evidence to the journal. J Bone Joint Surg Am 2003; 85-A (1): 1–3.
Norvell DC , Dettori JR , Fehlings MG , et al. Methodology for the systematic reviews on an evidence based approach for the management of chronic LBP. Spine 2011; 36: S10–S18.
Goldby LJ , Moore AP , Doust J , et al. A randomized controlled trial investigating the effi ciency of musculoskeletal physiotherapy on chronic low back disorder. Spine (Phila Pa 1976) 2006; 31: 1083–93.
Ferreira ML , Ferreira PH , Latimer J , et al. Comparison of general exercise, motor control exercise and spinal manipulative therapy for chronic low back pain: a randomized trial. Pain 2007; 131: 31–7.
Chown M , Whittamore L , Rush M , et al. A prospective study of patients with chronic back pain randomised to group exercise, physiotherapy or osteopathy. Physiotherapy 2008; 94: 21–28.
Marshall P , Murphy B. Self-report measures best explain changes in disability compared with physical measures after exercise rehabilitation for chronic low back pain. Spine (Phila Pa 1976) 2008; 33: 326–38.
Gudavalli MR , Cambron JA , McGregor M , et al. A randomized clinical trial and subgroup analysis to compare fl exion-distraction with active exercise for chronic low back pain. Eur Spine J 2006; 15: 1070–82.
Petersen T , Larsen K , Nordsteen J , et al. The McKenzie method compared with manipulation when used adjunctive to information and advice in low back pain patients presenting with centralization or peripheralization. A randomized controlled trial. Spine 2011; 24: 24.
Cecchi F , Molino-Lova R , Chiti M , et al. Spinal manipulation compared with back school and with individually delivered physiotherapy for the treatment of chronic low back pain: a randomized trial with one-year follow-up. Clin Rehabil 2010; 24: 26–36.
Yeung CK , Leung MC , Chow DH. The use of electro-acupuncture in conjunction with exercise for the treatment of chronic low-back pain. J Altern Complement Med 2003; 9: 479–90.
Eisenberg DM , Post DE , Davis RB , et al. Addition of choice of complementary therapies to usual care for acute low back pain: a randomized controlled trial. Spine (Phila Pa 1976) 2007; 32: 151–8.
Muller R , Giles LG. Long-term follow-up of a randomized clinical trial assessing the efficacy of medication, acupuncture, and spinal manipulation for chronic mechanical spinal pain syndromes. J Manipulative Physiol Ther 2005; 28: 3–11.
Giles LG , Muller R. Chronic spinal pain: a randomized clinical trial comparing medication, acupuncture, and spinal manipulation. Spine (Phila Pa 1976) 2003; 28: 1490–502. Discussion: 1502–3.
van der Roer N , van Tulder M , van Mechelen W , et al. Economic evaluation of an intensive group training protocol compared with usual care physiotherapy in patients with chronic low back pain. Spine (Phila Pa 1976) 2008; 33: 445–51.
Moffett JK , Torgerson D , Bell-Syer S , et al. Randomised controlled trial of exercise for low back pain: clinical outcomes, costs, and preferences. BMJ 1999; 319: 279–83.
Torstensen TA , Ljunggren AE , Meen HD , et al. Effi ciency and costs of medical exercise therapy, conventional physiotherapy, and self-exercise in patients with chronic low back pain. A pragmatic, randomized, single-blinded, controlled trial with 1-year follow-up. Spine (Phila Pa 1976) 1998; 23: 2616–24.
Sogaard R , Bunger CE , Laurberg I , et al. Cost-effectiveness evaluation of an RCT in rehabilitation after lumbar spinal fusion: a low-cost, behavioural approach is cost-effective over individual exercise therapy. Eur Spine J 2008; 17: 262–71.
Beam U. United Kingdom back pain exercise and manipulation (UK BEAM) randomised trial: cost effectiveness of physical treatments for back pain in primary care. BMJ 2004; 329: 1381.
Henchoz Y , Pinget C , Wasserfallen JB , et al. Cost-utility analysis of a three-month exercise programme vs usual care following multidisciplinary rehabilitation for chronic low back pain. J Rehabil Med 2010; 42: 846–52.
Johnson RE , Jones GT , Wiles NJ , et al. Active exercise, education, and cognitive behavioral therapy for persistent disabling low back pain: a randomized controlled trial. Spine (Phila Pa 1976) 2007; 32: 1578–85.
Niemisto L , Rissanen P , Sarna S , et al. Cost-effectiveness of combined manipulation, stabilizing exercises, and physician consultation compared to physician consultation alone for chronic low back pain: a prospective randomized trial with 2-year follow-up. Spine (Phila Pa 1976) 2005; 30: 1109–15.
Gatchel RJ , Rollings KH. Evidence-informed management of chronic low back pain with cognitive behavioral therapy. Spine J 2008; 8: 40–4.
Lamb SE , Hansen Z , Lall R , et al. Group cognitive behavioural treatment for low-back pain in primary care: a randomised controlled trial and cost-effectiveness analysis. Lancet 2010; 375: 916–23.
Fairbank J , Frost H , Wilson-MacDonald J , et al. Randomised controlled trial to compare surgical stabilisation of the lumbar spine with an intensive rehabilitation programme for patients with chronic low back pain: the MRC spine stabilisation trial. BMJ 2005; 330: 1233.
Cairns MC , Foster NE , Wright C. Randomized controlled trial of specific spinal stabilization exercises and conventional physiotherapy for recurrent low back pain. Spine (Phila Pa 1976) 2006; 31: E670–81.
Cady LD , Bischoff DP , O’Connell ER , et al. Strength and fitness and subsequent back injuries in fi refi ghters. J Occup Med 1979; 21: 269–72.
Duque I , Parra JH , Duvallet A. Maximal aerobic power in patients with chronic low back pain: a comparison with healthy subjects. Eur Spine J 2011; 20: 87–93.
Hoch AZ , Young J , Press J. Aerobic fitness in women with chronic discogenic nonradicular low back pain. Am J Phys Med Rehabil 2006; 85: 607–13.
Pedersen MT , Blangsted AK , Andersen LL , et al. The effect of worksite physical activity intervention on physical capacity, health, and productivity: a 1-year randomized controlled trial. J Occup Environ Med 2009; 51: 759–70.
Senna MK , Machaly SA. Does maintained Spinal manipulation therapy for chronic non-specific low back pain result in better long term outcome? [published online ahead of print January 17, 2011 ]. Spine (Phila Pa 1976). doi: 10.1097/BRS.0b013e3181f5dfe0.
Cherkin DC , Sherman KJ , Avins AL , et al. A randomized trial comparing acupuncture, simulated acupuncture, and usual care for chronic low back pain. Arch Intern Med 2009; 169: 858–66.
Edejer TT. Improving the use of research evidence in guideline development: 11. Incorporating considerations of cost-effectiveness, affordability and resource implications. Health Res Policy Syst 2006; 4: 23:2006.
Buyx AM , Friedrich DR , Schone-Seifert B. Ethics and effectiveness: rationing healthcare by thresholds of minimum effectiveness. BMJ 2011; 342: d54.

Return to ACUPUNCTURE
Return to EXERCISE AND CHIROPRACTIC
Since 8-05-2017


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |