Multimodal Chiropractic Care for Pain and Disability
in a Patient Diagnosed With Ehlers-Danlos Syndrome-
Hypermobility Type: A Case ReportThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: J Chiropractic Medicine 2017 (Jun); 16 (2): 170–174 ~ FULL TEXT
OPEN ACCESS Richard G. Strunk, DC
Private Practice,
Research Department,
Cleveland Chiropractic College,
Overland Park, KansasOBJECTIVE: The purpose of this article is to describe the clinical response to multimodal chiropractic treatment of a patient diagnosed with Ehlers-Danlos syndrome, hypermobility type (EDS-HT), and chronic pain.
CLINICAL FEATURES: A 22-year-old woman presented with severe chronic neck and low back pain, headaches, and bilateral hand pain and stiffness. In addition to these pain complaints, the patient had a family history of EDS, weekly or daily recurring joint dislocations, and upper and lower extremity joint hypermobility. As a result of her significant history and examination findings, which met the Brighton and Villefranche criteria, she was diagnosed with EDS-HT.
INTERVENTIONS AND OUTCOMES: Treatment primarily consisted of low force joint manipulative therapy and soft tissue therapy intermittently over 21 months concurrently with conventional and complementary medical care. Multiple outcome questionnaires were administered pragmatically at follow-up intervals of 3, 5˝, 8˝, 19, and 21 months, including but not limited to the Headache and Neck Disability Indices and the Oswestry Low Back Questionnaire. The patient had clinically meaningful improvements on the Neck Disability Index, the Headache Disability Index, and the Revised Oswestry after 3, 5˝, 8˝, and 21 months from baseline.
CONCLUSION: This patient with EDS-HT had clinically meaningful decreases in disability, headache, and spine pain after a course of multimodal chiropractic care combined with conventional and complementary medical care.
KEYWORDS: Chiropractic; Ehlers-Danlos Syndrome; Headaches; Low Back Pain; Manipulation; Neck Pain
From the FULL TEXT Article:
Introduction
Ehlers-Danlos syndrome (EDS) is a clinically and genetically heterogeneous group of disorders of connective tissue which cause various amounts of tissue fragility involving the skin, ligaments, blood vessels and internal organs. [1] According to the most recent classification standards, EDS consists of 6 main subtypes with the hypermobility type (EDS-HT) being considered the most common subtype [2] (Table 1). Although there have been no systematic epidemiological studies examining the true incidence of EDS-HT, it has been proposed that EDS-HT has a frequency of 0.75–2% [3] and is known to be more common among nonwhite populations and women. [4]

Table 1

Figure 1

Figure 2 Like in other EDS subtypes, EDS-HT is thought to be caused by mutations in gene encoding collagen chains but molecular based studies have yet to prove this theory true and as a result the etiology of EDS-HT remains unknown. [2] EDS-HT is also known as joint hypermobility syndrome (JHS) due to both conditions having similar clinical features. [2, 5] The similar clinical features of both conditions include generalized joint hypermobility, abnormal skin signs, reoccurring joint dislocations, chronic joint/extremity pain, and a positive family history. The diagnosis of EDS-HT is made with either the Brighton or the Villefranche criteria [2, 6] (Table 1; Figures 1 and 2). Both sets of criteria use similar history and examination findings to substantiate the diagnosis. Important findings to the diagnosis criteria include the amount and duration of arthralgia, extent of joint dislocations/subluxations, presence of various soft tissue lesions, and number of joints with joint hypermobility/laxity (on examination). Because the molecular basis of EDS-HT remains unknown, there is no confirmatory laboratory or molecular test to diagnose this EDS subtype. Several studies have reported higher rates of pain in patients with EDS-HT compared with those patients without it, but these findings are not universal. [7–13]
Rigorous high-quality treatment studies (eg, randomized controlled trials) of EDS-HT patients with spinal pain are quite limited. To date, 2 randomized controlled trials have been conducted on patients with EDS-HT. [14, 15] Both reported a benefit of various forms of exercise and physiotherapy on patients with knee pain and with unspecified pain. It is generally recommended that the best management strategy should be a multidisciplinary approach including physical therapy, cognitive behavioral therapy, pharmacology, and adherence to lifestyle recommendations. [2, 16] These general recommendations are helpful and an important step in addressing this complex condition, but because it is based on limited and weak (low) levels of evidence such as case studies and expert opinion it should be viewed with some caution. Within these recommendations, caution should be directed at the role of analgesic medications, including opioids, for patients with this condition given reports of ineffectiveness and potential adverse reactions involving the gastrointestinal system and addiction. [2, 16–20]
The role of physical therapy or physiotherapy also should be investigated further because of accounts of ineffectiveness and questions about long-term efficacy. [16, 20] Presently the prognosis of EDS-HT regarding long-term amelioration of symptoms is poor. At this time, the best conventional medicine can do is provide short-term, partial, or complete relief of symptoms. [2] Because of these known limitations regarding proposed treatment and poor prognosis, it is important to explore other treatments. Specific spinal manipulative therapy techniques performed by chiropractic physicians might offer a safe and effective option for EDS-HT patients. The role of a “low”-force chiropractic manipulative technique combined with either soft tissue therapy or exercise has been reported to have some promise at decreasing pain in EDS-HT patients, but it has only been studied to a limited extent as demonstrated in a few case reports. [17, 21, 22] The purpose of this case report is to describe the effects of multimodal spinal manipulative treatment on a patient diagnosed with EDS-HT and severe, chronic pain.
Case Report
Baseline Visit: August 30, 2011Patient History A 22–year-old white female presented with primary complaints of neck pain, headaches, low back pain, and bilateral hand and finger pain and stiffness in August 2011. All areas were rated 8/10 for average pain, 6/10 at initial visit, 5/10 for best pain, and 10/10 for worst pain using the Numeric Pain Rating Scale. [23, 24] The neck and low back pain and headaches all began insidiously at about 14 years of age. The neck was described as having a constant tight feeling localized to the posterior cervical spine, upper trapezius, and posterior shoulders bilaterally. The patient stated that turning her head side to side increased her neck pain, whereas rubbing the painful areas helped decrease it. She associated the neck pain with occasional numbness and tingling in the right and left hands. Her initial Neck Disability Index (NDI) score was 70%, which indicated frequent difficulty concentrating, working, and sleeping and reduced time spent participating in recreational activities. The NDI is recognized as a reliable and valid means of assessing the disability of patients with neck pain. [25, 26] The patient’s low back pain was localized to the lumbar spine and sacroiliac region and was described as a constant achiness aggravated by multiple daily tasks such as sitting still and frequent hip dislocations. The pain was primarily lessoned by general movement, prescription pain medication (methadone), and self-administered hip joint reduction using a medicine ball.
Her initial Revised Oswestry Low Back Questionnaire (OLBQ) score was 74%, which indicated severe disability. According to the questionnaire, her low back and sacroiliac joint pain caused substantial restrictions in her daily life including but not limited to her ability to sit for more than 10 minutes, walk more than a quarter mile, and stand for longer than 10 minutes at a time. Also, because of her pain, her normal night’s sleep was reduced by half. The Lower Extremity Functional Index (LEFI) questionnaire also indicated similar activity limitations (initial score was 68%) as the OLBQ, including not participating in any recreational/sports activities and having to use only slow and concise movements when washing and dressing. The LEFI, which measures the patient’s ability to perform activities of daily living by self-report (walking, etc), is reported to be reliable as a general index for lower extremity disorders. [27] The OLBQ, which assesses disability levels associated with low back pain, has been reported to have good reliability and has been responsive to clinically meaningful change. [28–32]
The patient also presented with bilateral wrist, hand, and finger pain and stiffness. Although generalized hand movement helped decrease the pain intensity, the pain was described as sharp and constant throughout the day. Dislocations of her left and right second proximal interphalangeal joints and metacarpophalangeal (MCP) joints had occurred daily until she starting wearing stabilizing bracelets. Her initial Upper Extremity Functional Index (UEFI) score was 44%, representing marked restrictions when she lifted, pushed, or pulled items. As a result of these limitations, her work, recreational, and social activities suffered. The UEFI was modified for use in the teaching clinic and does not have any reliability or validity research on its use.
Headaches with associated lightheadedness were another problem in which she reported at her initial visit. Her initial Headache Disability Index (HDI) score was 72%, indicating a high degree of disability. [33] Analogous to other areas of pain, she reported her headaches often affected her social life (social gatherings), emotional well-being, traveling, recreational activities and hobbies, and thinking. Like many other patients with EDS-HT and widespread pain, our patient also presented with recurring joint dislocations occurring many times a week, sometimes daily, in her second proximal interphalangeal/MCP joints, elbows, shoulders, right fifth and sixth ribs, and hip joints. The patient didn’t report any types of self/home care including any dietary changes prior to seeking care at our clinic.
Before her initial visit with us the patient experienced several months of exacerbations and remissions of fevers; red, itchy, and dry eyes; skin hives or rash; swollen neck glands; swelling of the hands and feet; leg cramps; and chronic bladder infections. She was subsequently diagnosed with systemic lupus erythematosus and was prescribed mycophenolic acid (CellCept) by her rheumatologist. Before receiving care (and during care) at our clinic, the patient was treated with low-dose methadone (10 mg 3 times daily), cyclobenzaprine (Flexeril), and lidocaine patches (Lidoderm) to help her manage her pain. Since 19 years of age, she had been unable to attend college courses or remain employed. During this same period, the patient was diagnosed with fibromyalgia, EDS-HT, and Raynaud phenomenon by her rheumatologist. In addition to the pain medications, she also was prescribed medications to manage her depression and ulcerative colitis. At 15 years of age, the patient had bilateral carpal tunnel release surgery for carpal tunnel syndrome and chiropractic care for low back and neck pain. Family history revealed the presence of JHS/EDS-HT in her mother, confirmed by the presence of 4 minor criteria (low back pain for longer than 1 year, history of thumb and temporomandibular joint dislocations, myopic vision, and varicose veins in posterior knees bilaterally) on history and examination.
Initial Examination The orthopedic examination of the cervical and lumbopelvic spinal regions produced mechanically induced nociceptive type pain in both regions. Cervical spine stretching and compressive tests produced achy pain in the cervicothoracic junction paraspinally, whereas lumbopelvic stretching and compressive tests caused sharp pain localized to the left and right sacroiliac joint region. The orthopedic testing of both wrists also caused mechanically induced nociceptive pain specifically at the radioulnar–carpal joint complex. Orthopedic testing of both hips was not possible because of the severity of her lumbopelvic pain presentation. Cervical and lumbopelvic active and passive range of motion produced localized pain with range visualized within normal limits. Cervical active and passive range of motion produced achy pain at the cervicothoracic junction in almost all directions, with lumbopelvic active and passive range of motion triggering sharp pain in both sacroiliac joints. Hip active and passive range of motion was decreased in both hips, eliciting sharp pain. The postural examination in the coronal view displayed a forward head carriage, protracted shoulders, posterior pelvic tilt where the sagittal view indicated a high left shoulder, bilateral scapular winging, and a high right iliac crest.
Overactivity of the upper trapezius muscles was indicated by a “failed” shoulder abduction movement pattern test. The soft tissue palpation examination revealed multiple tender and hypertonic spinal areas consistent to the location of the chief complaints. The segmental joint motion examination indicated hypomobilities in the upper cervical, upper and lower thoracic, right sacroiliac, and multiple left wrist joints. In addition to the previously diagnosed conditions of EDS, fibromyalgia, systemic lupus erythematosus, and Raynaud, the patient was diagnosed with cervical and lumbopelvic myalgia, bilateral carpal tendinopathy, idiopathic headaches, and joint dysfunction of the cervical, thoracic, sacroiliac, and wrist regions.
Examination for EDS-HT
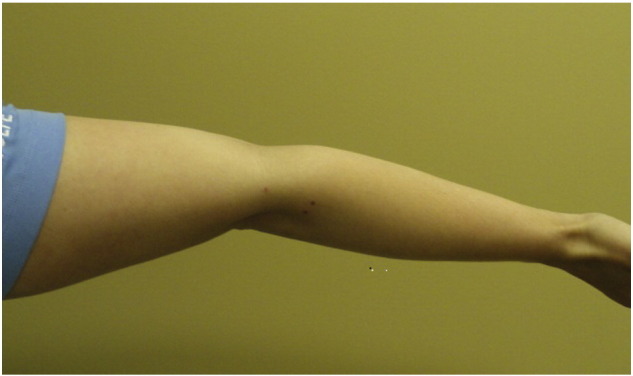
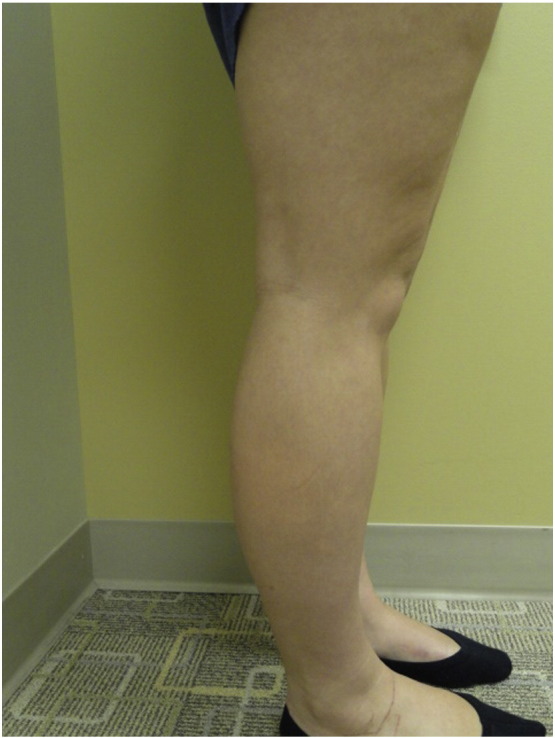
Because the EDS-HT examination procedures are not part of the standard examination performed on the initial visit by interns, the examination for EDS-HT was performed on June 20, 2013, to evaluate the severity and to confirm the EDS-HT diagnosis for this case report. The patient’s Beighton score was a 3 out of 9. Range of motion of the elbows, knees, and fifth MCP joint was measured with a 2–arm goniometer with thumb opposition, and lumbopelvic flexion visually observed. Positive Beighton findings (counting toward the total Beighton score of 3) were left elbow (humeroulnar joint) hyperextension at 20°, right elbow hyperextension at 18°, and right knee hyperextension at 10° (Fig 3, Fig 4, Fig 5). Left knee hyperextension (5°), left and right fifth MCP joints (less than 90°), left and right thumb opposition, and lumbopelvic forward flexion were all negative Beighton findings. The physical examination of the patient’s hip and iliac crest region revealed skin striae bilaterally in these regions. The patient displayed no signs of skin hyperextensibility or abnormal scarring commonly seen in the classic subtype and no molecular testing had been performed because of the high costs of such tests.
Confirmation of the EDS-HT diagnosis was made by the presence of 4 minor Brighton Criteria (Beighton score = 3, 10–year history of low back pain, history of joint dislocations in more than 1 joint, and skin striae) and confirmation of EDS-HT diagnosis in her mother. The patient also had Villefranche diagnostic findings including the presence of 1 major (generalized joint hypermobility) and 3 minor criteria (recurring joint dislocations, chronic joint/limb pain, and positive family history).
Interventions and Outcomes
Treatment
Generally, the multimodal treatment consisted of joint manipulation combined with soft tissue treatment. The most common type of manipulation (applied to 33 of the 34 visits) administered was a mechanical force, manually assisted technique applied by the Activator IV adjusting instrument to the spine and pelvis and at times the extremities (41% of the time). [34] This instrument allows for a specific, low-force impulse to the vertebral and extremity joints. Gentle drop-table technique was administered to the hip joints on 7 visits, and modified high-velocity, low-amplitude spinal manipulation was performed to the cervical spine on 15 visits. [35] In accompaniment with joint manipulation techniques, a soft tissue technique was used in 68% of the visits, with Graston technique applied most often and manual myofascial release and post-isometric relaxation technique performed on 5 visits. [36, 37]
All examinations and outcome assessments (except for the EDS-HT examination) and treatment were performed at a chiropractic college outpatient clinic by qualified chiropractic interns under the direction of a licensed doctor of chiropractic. The EDS-HT examination was performed by the lead author. In addition, the patient received limited complementary medical care since starting chiropractic treatment at the college clinic. The complementary care consisted of massage therapy (2 times/y), dietary changes, and relaxation exercises with an outside therapist. Also, during the chiropractic care, the patient was concurrently seeing a rheumatologist and her general practitioner.
Outcomes

Table 2 The NDI, HDI, and Revised OLBQ were administered pragmatically at follow-up intervals of 3, 5˝, 8˝, 19, and 21 months. The initial UEFI was administered 1 month after the other outcome measures were administered and at follow-up intervals of 2, 5, and 8 months. The patient received 34 treatment visits intermittently over a 21–month period with the majority of the treatment (26 visits) over the first 12 months. After 12 months of care, the patient dropped out of care for 7 months for unknown reasons. After the 7 months of no care, the patient returned to our clinic in April 2013 for 8 visits over a period of 2 months. The patient had clinically meaningful improvements on the NDI, the HDI, and the Revised Oswestry after 3, 5˝, and 8˝ months from baseline [2, 32, 33, 38] (Table 2). Also, after 21 months from baseline, the NDI and the HDI but not the Revised Oswestry indicated clinically meaningful improvements. According to the NDI 8˝– and 21–month follow-up scores, the patient reported less intense neck pain and improvements performing many daily tasks such as concentrating, sleeping, and participating in recreational activities.
Her sleeping time was one of the largest improvements made, from 3 to 5 hours sleepless at baseline to less than 1 hour sleepless after the 8˝–month follow-up. Her Revised Oswestry and HDI indicated improvements in daily tasks similar to the NDI. Social activities and sitting had the greatest improvement after 8˝ months, according to the Revised Oswestry. It also appears the patient had clinically meaningful improvements after 8˝ months on the LEFI and the UEFI, but further research is needed to define the amount of change that constitutes clinically meaningful improvements on these questionnaires. Qualitatively, the UEFI indicated the patient made mild improvements with reaching tasks and pushing and pulling jobs after 8˝ months but still had disability present with these roles. The LEFI indicated positive progress with her personal care, recreational activities, and sitting and standing tasks after 8˝ months, like the Revised Oswestry. The Patient Global Impression of Change scale (PGIC) indicated the patient was “much better” at the 21–month follow-up. The PGIC is a self-reported 7–point Likert scale in which a patient assesses his or her degree of change since starting treatment, ranging from very much better to very much worse. The PGIC has been well validated and has been commonly used by pain researchers as a standard outcome instrument. [39–42] On a qualitative postcare questionnaire that asked about the importance of chiropractic care to the patient, the patient stated, “It was so very valuable, I can’t even think where I might be without it!…It has given me my life back and I’m very thankful for my chiropractic care!”
The patient gave consent for this study to be published, and the study was exempt from review by the college’s Institutional Review Board.
Discussion
This is one of only a few case reports describing the results of multimodal chiropractic care of a patient with EDS, hypermobility type, and chronic pain. [17, 21, 22] The results of the outcome indices indicated that the patient had clinically meaningful improvements on the NDI, the HDI, and the Oswestry from baseline through 8˝ months. A similar pain reduction was also identified with the patient’s NDI and HDI scores after the second round of treatment in June 2013 and with the LEFI and the UEFI scores from baseline to 8˝ months. The reduced pain and disability identified in this patient was similar to other EDS patients treated with multimodal chiropractic care. Colloca and Polkinghorn [17] reported on 2 chronic pain patients who had decreased pain and disability after being treated with a mechanical force, manually assisted technique (applied by the Activator II adjusting instrument) combined with stabilization and postural corrective exercises. Similar results were obtained in other EDS/JHS patients who received comparable forms of multimodal chiropractic care. [21, 22] It is noteworthy to convey that the patients in Colloca and Polkinghorn’s case report not only had reduced pain and disability but were able to reduce their pain and anti-inflammatory medication usage during and after their chiropractic treatment. Because medication usage was not an outcome measure in this study, it is not known whether our patient had any medication usage changes as a result of her reduced pain during or after her chiropractic care. In future studies, medication usage would be a valuable outcome to track because many EDS patients are prescribed pain medications and have adverse reactions. [20]
The patient’s lack of full recovery observed in this case report is typical of patients with EDS-HT treated for chronic pain. In a small study by Ashton, [43] 9 EDS/JHS patients with chronic back pain had poorer physical outcome measurements after 3 months compared with those with chronic back pain without EDS/JHS. Patients with EDS or EDS-HT often have exacerbations of pain symptoms and disability as observed in Colloca and Polkinghorn’s case report and others. [17, 21, 22] The common occurrence of exacerbations may explain in part why EDS/EDS-HT patients usually don’t have a full recovery and often still have disability after improvements are reported on the outcome measurements. As in Colloca and Polkinghorn’s and Morley and Perrault’s case reports, the patient’s exacerbations can be from normal activities of daily living without any physical traumatic event reported. Our patient had frequent random joint dislocations or subluxations that occurred with normal activities of daily living.
Limitations
Given that this is a case report it is not understood what factors were precisely responsible for the outcomes, but considering that headaches, neck pain, and low back pain tend to follow a recurrent and continual natural course, [44–49] combined with the patient’s positive outcome scores, it is hypothesized the multimodal chiropractic treatment was at least partially responsible for the patient’s reduced pain and disability. It is also possible that the other nontreatment variables such as natural illness progression/course and or the lifestyle changes or other treatment (eg, relaxation exercises) contributed to her decreased symptoms. Another limitation important to mention that may have affected the patient outcomes pertains to treatment delivered by interns. It is difficult to speculate what affect intern treatment (vs experienced doctor’s treatment) may have had on this patient, but it is possible the outcomes could have been better if the treatment was provided by a more experienced, licensed doctor of chiropractic. It is noteworthy to state that the interns who provided the treatment achieved basic competencies in their respective course work before applying it on the clinic patient.
In this particular case, the patient appeared to experience clinical benefit from the multimodal low-force chiropractic treatment when combined with other medical care. This case report is notable to health care providers, especially doctors of chiropractic, because of the low amount of experimental research on effective conservative treatment of EDS-HT. Because there is no single treatment that provides complete long-term pain relief in these patients, it is vital that more clinical research in the form of case reports or series or controlled studies on multimodal low-force chiropractic treatment are conducted in EDS-HT patients.
Conclusion
This case report is important because it describes the positive response of 2 trials of multimodal low-force chiropractic treatment combined with conventional and complementary medical care in a patient diagnosed with EDS-HT and severe chronic pain. The relationship between multimodal low-force chiropractic care and its effect on patients with chronic pain and EDS-HT needs further study.
Practical Applications
This study presents similar positive outcome findings observed in other studies
on EDS-HT and multimodal chiropractic care.Multimodal chiropractic care consisting of low force joint manipulative therapy and
soft tissue therapy may help decrease pain and disability in individuals with EDS-HT.The results from this study may be valuable due to the lack of any long term cure
available for patients with EDS-HT.Funding Sources and Conflicts of Interest
No funding sources or conflicts of interest were reported for this study.References
Callewaert B, Malfait F, Loeys B, De Paepe A.
Ehlers-Danlos syndromes and Marfan syndrome.
Best Pract Res Clin Rheumatol. 2008;22(1):165–189Castori M.
Ehlers-Danlos syndrome, hypermobility type: an underdiagnosed hereditary connective tissue disorder with mucocutaneous, articular, and systemic manifestations.
ISRN Dermatol. 2012;2012:751768Hakim AJ, Sahota A.
Joint hypermobility and skin elasticity: the hereditary disorders of connective tissue.
Clin Dermatol. 2006;24(6):521–533Grahame R, Hakim A.
Joint hypermobility syndrome is highly prevalent in general rheumatology clinics, its occurrence and clinical presentation being gender, age and race related.
Ann Rheum. 2006;65:263.Tinkle BT, Bird HA, Grahame R, Lavallee M, Levy HP, Sillence D.
The lack of clinical distinction between the hypermobility type of Ehlers-Danlos syndrome and the joint hypermobility syndrome (a.k.a. hypermobility syndrome)
Am J Med Genet A. 2009;149A(11):2368–2370Grahame R, Bird HA, Child A.
The revised (Brighton 1998) criteria for the diagnosis of benign joint hypermobility syndrome (BJHS)
J Rheumatol. 2000;27(7):1777–1779Voermans NC, Knoop H.
Both pain and fatigue are important possible determinants of disability in patients with the Ehlers-Danlos syndrome hypermobility type.
Disabil Rehabil. 2011;33(8):706–707Rombaut L, Malfait F, Cools A, De Paepe A, Calders P.
Musculoskeletal complaints, physical activity and health-related quality of life among patients with the Ehlers-Danlos syndrome hypermobility type.
Disabil Rehabil. 2010;32(16):1339–1345Al-Rawi ZS, Al-Aszawi AJ, Al-Chalabi T.
Joint mobility among university students in Iraq.
Br J Rheumatol. 1985;24(4):326–331Larsson LG, Baum J, Mudholkar GS, Kollia GD.
Benefits and disadvantages of joint hypermobility among musicians.
N Engl J Med. 1993;329(15):1079–1082Acasuso Diaz M, Collantes Estevez E, Sanchez Guijo P.
Joint hyperlaxity and musculoligamentous lesions: study of a population of homogeneous age, sex and physical exertion.
Br J Rheumatol. 1993;32(2):120–122El-Metwally A, Salminen JJ, Auvinen A, Kautiainen H, Mikkelsson M.
Prognosis of non-specific musculoskeletal pain in preadolescents: a prospective 4-year follow-up study till adolescence.
Pain. 2004;110(3):550–559Tobias JH, Deere K, Palmer S, Clark EM, Clinch J.
Joint hypermobility is a risk factor for musculoskeletal pain during adolescence: findings of a prospective cohort study.
Arthritis Rheum. 2013;65(4):1107–1115Sahin N, Baskent A, Cakmak A, Salli A, Ugurlu H, Berker E.
Evaluation of knee proprioception and effects of proprioception exercise in patients with benign joint hypermobility syndrome.
Rheumatol Int. 2008;28(10):995–1000Kemp S, Roberts I, Gamble C.
A randomized comparative trial of generalized vs targeted physiotherapy in the management of childhood hypermobility.
Rheumatology (Oxford) 2010;49(2):315–325Castori M, Morlino S, Celletti C.
Management of pain and fatigue in the joint hypermobility syndrome (a.k.a. Ehlers-Danlos syndrome, hypermobility type): principles and proposal for a multidisciplinary approach.
Am J Med Genet A. 2012;158A(8):2055–2070Colloca CJ, Polkinghorn BS.
Chiropractic management of Ehlers-Danlos syndrome: a report of two cases.
J Manipulative Physiol Ther. 2003;26(7):448–459Dowell D, Haegerich TM, Chou R.
CDC Guideline for prescribing opioids for chronic pain - United States, 2016.
MMWR Morb Mortal Wkly Rep. 2016;65(1):1–49Abdel Shaheed C, Maher CG, Williams KA, Day R, McLachlan AJ.
Efficacy, tolerability, and dose-dependent effects of opioid analgesics for low back pain: a systematic review and meta-analysis.
JAMA Intern Med. 2016;176(7):958–968Ferman J, Hamm D.
World-wide EDS Awareness Survey [Power Point Slides].
EDS Awareness. 2017.
http://www.chronicpainpartners.com/webinar/free-webinar-results-eds-
awareness-world-wide-surveyMorley J, Perrault T.
Chiropractic management of Ehlers-Danlos Syndrome: a case report.
J Am Chiropr Assoc. 2010;47:6–15.Strunk RG, Pfefer MT, Dube D.
Multimodal chiropractic care of pain and disability for a patient diagnosed with benign joint hypermobility syndrome: a case report.
J Chiropr Med. 2014;13(1):35–42Jensen MP, Karoly P, Braver S.
The measurement of clinical pain intensity: a comparison of six methods.
Pain. 1986;27(1):117–126Bijur PE, Latimer CT, Gallagher EJ.
Validation of a verbally administered numerical rating scale of acute pain for use in the emergency department.
Acad Emerg Med. 2003;10(4):390–392Vernon H, Mior S.
The Neck Disability Index: a study of reliability and validity.
J Manipulative Physiol Ther. 1991;14(7):409–415Hains F, Waalen J, Mior S.
Psychometric properties of the neck disability index.
J Manipulative Physiol Ther. 1998;21(2):75–80Schunk C, Rutt R.
TAOS Functional Index: orthopaedic rehabilitation outcomes tool.
J Rehabil Outcomes Measure. 1998;2(2):55–61.Hsieh CY, Phillips RB, Adams AH, Pope MH.
Functional outcomes of low back pain: comparison of four treatment groups in a randomized controlled trial.
J Manipulative Physiol Ther. 1992;15(1):4–9Meade TW, Dyer S, Browne W, Townsend J, Frank AO.
Low back pain of mechanical origin: randomised comparison of chiropractic and hospital outpatient treatment.
BMJ. 1990;300(6737):1431–1437Manniche C, Asmussen K, Lauritsen B, Vinterberg H, Kreiner S, Jordan A.
Low Back Pain Rating Scale: validation of a tool for assessment of low back pain.
Pain. 1994;57(3):317–326Roland M, Fairbank J.
The Roland-Morris Disability Questionnaire and the Oswestry Disability Questionnaire.
Spine. 2000;25(24):3115–3124Fritz JM, Irrgang JJ.
A comparison of a modified Oswestry Low Back Pain Disability Questionnaire and the Quebec Back Pain Disability Scale.
Phys Ther. 2001;81(2):776–788Jacobson GP, Ramadan NM, Aggarwal SK, Newman CW.
The Henry Ford Hospital Headache Disability Inventory (HDI)
Neurology. 1994;44(5):837–842Fuhr A. 2nd ed.
Mosby Elsevier; St. Louis: 2009.
Activator Method.Peterson D, Bergman T. 2nd ed.
Mosby; St. Louis: 2002.
Chiropractic Technique: Principles and Procedures.Chaitow L.
In: Muscle Energy Techniques. 3rd ed.
Churchill Linvingstone; Edinburgh, UK: 2006.
An introduction to muscle energy techniques; pp. 13–57.Hammer W. 3rd ed. Sudbury, MA;
Jones and Bartlett: 2007.
Functional Soft-Tissue Examination and Treatment by Manual Methods.Pool JJ, Ostelo RW, Hoving JL, Bouter LM, de Vet HC.
Minimal clinically important change of the Neck Disability Index and the Numerical Rating Scale for patients with neck pain.
Spine. 2007;32(26):3047–3051Farrar JT, Young JP, Jr, LaMoreaux L, Werth JL, Poole MR.
Clinical Importance of Changes in Chronic Pain Intensity
Measured on an 11-point Numerical Pain Rating Scale
Pain 2001 (Nov); 94 (2): 149-158Goldsmith CH, Boers M, Bombardier C, Tugwell P.
Criteria for clinically important changes in outcomes: development, scoring and evaluation of rheumatoid arthritis patient and trial profiles. OMERACT Committee.
J Rheumatol. 1993;20(3):561–565Jenkinson C, Peto V, Coulter A.
Measuring change over time: a comparison of results from a global single item of health status and the multi-dimensional SF-36 health status survey questionnaire in patients presenting with menorrhagia.
Qual Life Res. 1994;3(5):317–321Juniper EF, Guyatt GH, Willan A, Griffith LE.
Determining a minimal important change in a disease-specific Quality of Life Questionnaire.
J Clin Epidemiol. 1994;47(1):81–87Ashton S, Hakim AJ.
Paper presented at: Soft Tissue and Regional Musculoskeletal Disease
and Fibromyalgia Conference. 2005. Underdiagnosed joint hypermobility
syndrome patients have poorer outcomes than peers following chronic back pain rehabilitation.Kienbacher C, Wober C, Zesch HE.
Clinical features, classification and prognosis of migraine and tension-type headache in children and adolescents: a long-term follow-up study.
Cephalalgia. 2006;26(7):820–830Lyngberg AC, Rasmussen BK, Jorgensen T, Jensen R.
Prognosis of migraine and tension-type headache: a population-based follow-up study.
Neurology. 2005;65(4):580–585Cote P, Cassidy JD, Carroll LJ, Kristman V.
The annual incidence and course of neck pain in the general population: a population-based cohort study.
Pain. 2004;112(3):267–273Von Korff M, Saunders K.
The course of back pain in primary care.
Spine. 1996;21(24):2833–2837. discussion 2838-2839Philips HC, Grant L.
The evolution of chronic back pain problems: a longitudinal study.
Behav Res Ther. 1991;29(5):435–441Bot SD, van der Waal JM, Terwee CB.
Predictors of outcome in neck and shoulder symptoms: a cohort study in general practice.
Spine. 2005;30(16):E459–E470
Return to CASE STUDIES
Since 12–07–2017


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |