

|
Weakness Nervousness Pain Referred Pain and Reflexes Hysterical Anesthesia or Palsy Peripheral Nerve Injuries Classification of Nerve Trauma Nerve Pinch or Stretch Syndromes Examination Management Major Types of Neuritides Local Neuritis Peripheral Neuritis Common Reflex Irritations Autonomic Imbalance Physiologic Control of Body Activity Factors Involved in Vegetative Imbalance Sympathicotonia and Vagotonia Special Therapeutic Considerations Neurotherapy and Spondylotherapy Tissue Goading and Pressure Neurovascular and Neurolymphatic ReceptorsChapter 17:
Peripheral Nerve Injuries
From R. C. Schafer, DC, PhD, FICC's best-selling book:
“Chiropractic Management of Sports and Recreational Injuries”
Second Edition ~ Wiliams & Wilkins
The following materials are provided as a service to our profession. There is no charge for individuals to copy and file these materials. However, they cannot be sold or used in any group or commercial venture without written permission from ACAPress.
All of Dr. Schafer's books are now available on CDs, with all proceeds being donated
to chiropractic research. Please review the complete list of available books.
Examination History Spinal Reflexes and Muscle Tone Evaluating the Sensory System Evaluating the Motor System Evaluating the Cerebellar System Common Symptoms of Neural Disorder
Chapter 17: Peripheral Nerve Injutries
To express a totally healthy state, body habitus must be coordinated and integrated as a whole. Coordination of almost all body functions is accomplished by activity of various parts of the nervous system. This coordination is accomplished by the presence and integrity of the functional unity of the nervous system, ie, the reflex arc. It is for these reasons that chiropractic health care places such emphasis on neurologic coordination and integrity. The neurologic examination thus incorporates testing muscle tone and strength, evaluating normal and abnormal reflexes, coordination, sensation, along with structural and functional abnormalities. No objective neurologic examination is complete without a thorough patient history and physical examination of the whole body.
(1) consider the autonomic, motor, and sensory nerve supply to the area, Thus, if a problem concerns a visceral area, consider the somatic structures and other viscera that share the same autonomic, motor, and sensory innervation as the organ involved. It is for this reason that reflexes are labeled somatosomatic, somatovisceral, viscerovisceral, or viscerosomatic.
(1) In upper motor neuron or pyramidal fiber lesions, the deep tendon reflexes are exaggerated, but the superfical skin reflexes are decreased or absent.
Localize areas of diminished or absent tactile sensation, increased pain sensation, and abnormal sensations. Seek temperature, vibratory, and proprioceptive impairments. Once sensory perceptions are found to be abnormal and the areas can be localized, the spinal nerves or higher centers affected can then be identified. Sensory deficits are usually found in areas of pain, muscle weakness and atrophy, and areas of excessive sweating when in conjunction with sympathetic nervous system involvement.
General Patterns of Sensory Loss. The pattern of sensory loss is helpful in differentiating lower and upper motor lesions. Sensory loss in one half of the body usually points toward impairment in the cerebral or thalamic area and above the pons, wherein the deficit is almost to the midline of the body. In hysteria, the deficit is to the midline or greater. Sensory loss in the saddle area, associated with absent anal sphincter and anal skin reflexes, points toward a tumor in the conus medullaris of the spinal cord or a malignancy in the cord, probably from the prostate. A lower motor neuron lesion is usually at the upper lumbar area. If the lower lumbar and sacral nerves are involved, it usually means a lesion in the cauda equina. An upper motor lesion results in loss of bladder and bowel control and a loss of potency. Sensory loss in the lower trunk and legs is indicative of spinal cord lesions. Sensory loss in the distal half of the extremities (stocking-glove deficit) is a common finding in peripheral neuropathy and sometimes in hysteria. The radial sensory area, located on the back of the hand toward the thumb. The median area, occupying the tips of the index and middle fingers. The ulnar area, limited to the small finger. The musculocutaneous area, located on the medial aspect of the forearm. The axillary area, located over the point of the shoulder. The femoral area, situated on the anterior medial aspect of the thigh. The femoral lateral-cutaneous area, located over the distal part of the lateral surface of the thigh. The common peroneal area, presented as a vertical strip on the front of the ankle. The sciatic sensory area, occupying the entire foot and ankle except the medial aspect.
(1) Peripheral lesions give a segmental loss picture, and the loss will be on the same side as the lesion (eg, nerve root compression).
(a) the loss will be on the side opposite the lesion for exteroceptive sensations; or
Muscle Strength. Have the patient perform various muscular actions against resistance, and always test bilaterally. Be mindful that the nervous system is concerned with patterns of movement and not with contraction of isolated, named muscles. There is a loss of both superficial and deep reflexes. The stretch and tendon reflexes are abolished thus producing a hypotonus state. No classic pathologic reflexes are present. Fibrillations and fasciculations are present only in the early stage during which muscles are undergoing atrophic changes. A flaccid type of paralysis is seen if there is no regeneration; the muscles involved eventually shrink and possibly are replaced by connective and adipose tissues. Muscle tone no longer exists because the peripheral nerve is unable to maintain it, and the muscles become limp. Severe atrophy of muscles is observed within a few weeks due to a lack of efferent impulses which results in a degeneration of muscle fibers. Reaction of degeneration is seen from 10-14 days after the injury. The nerve is unable to conduct the electrical current because of structural alterations. A spastic type of paralysis or paresis is seen on the opposite side of the body and below the level of the lesion if the lesion is at or above the medullary pyramid. Weakness is especially pronounced in the muscles of the limbs, and there is great difficulty with movements of the hands. Increased muscle tone expresses as firmness and stiffness, especially in the arm flexors and the leg extensors. There is minimal or no atrophy of the muscles involved. However, there will be a later disuse atrophy. After a few days to a few weeks, stretch reflexes return in the involved muscles and usually become more active than usual. Muscle resistance to passive movements is exaggerated; often strong at the beginning of movement, then collapsing in a peculiar "clasp-knife" method as more force is applied. The superficial reflexes are abolished. There is an increase of deep reflexes since the normal operation of gravity against the weight of the body may initiate stretch reflexes. Reflex contractions are exaggerated due to a loss of the inhibitory mechanism from the higher central level. The combination of this effect with contractions resulting from continuous discharge of brain stem excitatory mechanisms leads to a hypertonic state. The flexor reflex or nociceptive reflex and the Babinski sign can be observed. The nociceptive reflex evokes withdrawal of a body part by action of flexor muscles at one or several joints, depending on severity of stimulus, in response to injurious stimuli such as pricking, pinching, or burning. In a patient with a pyramidal tract lesion, the Babinski reflex is positive. Hoffmann's sign is usually present but not a reliable sign since it is seen occasionally in normal individuals. No reaction of degeneration will be present in an upper motor neuron lesion; ie, no ability of the muscle or nerve to respond to galvanic or faradic current. If the peripheral nerve responds to electrical stimulation, it can be assumed that the lesion is in an upper motor neuron.
Malcoordination Tests.
Test cerebellar function by the evaluation of gait, carriage, station, limb pronation/supination, hand patting, finger-to-nose tests, heel-to-knee, heel-to-toe, Romberg, and foot-to-buttock tests.
Keep in mind that the left side of the body is under the influence of the left cerebellar hemisphere, and vice versa. Any symptoms that occur unilaterally will then be on the same side as the cerebellar lesion. The opposite is true with cerebral lesions, where the lesion invariably produces contralateral symptoms and signs.
Weakness, paralysis, nervousness, pain, tenderness, sensory loss, paresthesia, and abnormalities of muscle mass or tone are the most common signs and symptoms noted in neural disorders. Obvious direct trauma or injury. Reflex pain from visceral reflexes or reflex pain from musculoskeletal lesions, which deep pressure often exaggerates, such as trigger points. Peripheral nerve injury (eg, causalgia) which results in an intense burning superficial pain. A history of injury usually helps to evaluate this disorder. Presence of nerve inflammations and degenerations of the peripheral or central nervous system. They frequently cause other changes indicative of such lesions. Vascular disease, which is usually associated with other changes such as swelling, redness, blanching, or other vascular disorder signs, depending upon whether it is an arterial or venous problem. Certain neurovascular syndromes may be associated with pain and paresthesia. Vasomotor disturbances may also be caused or aggravated by vertebral subluxations such as the deep congestive leg aches associated with upper-lumbar subluxations or the cranial vasomotor headaches and other symptoms of cervical subluxation. Sensory root pressure characterized by pain, paresthesia, and often by abnormal sensitivity to touch along the course of the involved nerve root's segmental skin supply. Thus, this becomes an important consideration and needs to be traced and demarcated with a skin pencil to see if the area corresponds to a specific dermatome.
Pain and other sensory disturbances caused by subluxations may be due to direct nerve root involvement and, therefore, of the nature mentioned above. They may also be due to reflex irritation of the paravertebral ligaments, tendons, or muscles and, like other myofascial trigger areas, refer pain into somatic areas that do not correlate to direct dermatomes or specific nerve roots.
Headaches. Headaches, the most frequent symptom in America today, are usually attributed to tension, migraine, abnormal sinus, tumor, vascular disorders, or hysteria. Often neglected causes are overall postural strain and trauma to the cervical spine. Headaches caused by viscerosomatic reflexes from the gallbladder, stomach, and duodenum are much more common than suspected. Nausea or vomiting with headaches is usually considered to have a neurologic basis of a vascular nature; however, a vagal disturbance due to upper cervical function may be the offender.
Damage to an individual peripheral nerve (eg, trauma) is characterized by
(1) flaccid, atrophic paralysis of the muscles supplied by the involved nerve and
When partial destruction to various peripheral nerves occurs, the effects are usually more prominent in the distal extremities. The condition is characterized by muscular weakness and atrophy and poorly demarked areas of sensory changes. Contusion (neurapraxia). Recovery is usually within 6 weeks. Contusion may be the result of either a single blow or through persistent compression. Fractures and blunt trauma are often associated with nerve contusion and crush. Peripheral nerve contusions exhibit early symptoms when produced by falls or blows. Late symptoms arise from pressure by callus, scars, or supports. Mild cases produce pain, tingling, and numbness, with some degree of paresthesia. Moderate cases manifest these same symptoms with some degree of motor-sensory paralysis and atrophy.
Crush (axonotmesis). Recovery rate is about an inch per month between the site of trauma and the next innervated muscle. If innervation is delayed from this schedule or if the distance is more than 6 inches, surgical exploration should be considered.
Laceration (neurotmesis). Laceration follows sharp or penetrating wounds and is less frequently seen associated with tears from a fractured bone's fragments. Surgery is usually required. A traction injury typically features several sites of laceration along the nerve. Stretching injury is usually limited to the brachial plexus.
Typical Examples of Findings: Sensation is lost on the ulnar side of the hand, including the little finger and medial half of the ring finger, in ulnar nerve damage. In median nerve damage, sensation of the remainder of the anterior surface of the hand is lost. As time goes on, the affected part assumes a posture and atrophy peculiar to the particular nerve involved; for example, "wrist drop" with the radial nerve, "claw hand" with the ulnar nerve, "flat hand" with the median nerve, "ape hand" with the ulnar and median nerves, and "foot drop" with the peroneal nerve.
Acute Neuritis: Pain and hyperalgesia are witnessed in the area of nerve distribution along with tenderness on palpation of the nerve trunk and muscles supplied by the nerve. Trigger spots may be present. Reflexes are either unaffected or possibly increased. Marked hypertonicity and tenderness of the occipital musculature and the consequent C1 or C2 neuralgia associated with upper motor cervical subluxations. Hypertonicity and tenderness of the muscles and tendons of the rotator cuff consequent to rotator cuff tendinitis and associated with referred pain into the posterolateral arm. These manifestations are often predisposed by cervical subluxation and spondyloarthrosis. Hypertonicity and tenderness of the musculature around the scapula common to the scapulocostal syndrome. These areas often cause reflex pain down the ulnar side of the upper extremity and are often predisposed by a sectional thoracic scoliosis and thoracocostal subluxations or duodenal malfunction. Hypertonicity and tenderness of the gluteal musculature and sacroiliac ligaments which may reflect pain over the sciatic trajectory. Such disorders are often caused or affected by sacroiliac subluxations or reflexes from pelvic congestion. Hypertonicity and tenderness of the piriformis which may cause a posterior sciatic reflex neuralgia and even peripheral nerve pressure, which is common to many sacral subluxations or gonadal irritation/malfunction. Hypertonicity and tenderness of the tensor fascia latae and the consequent reflex pain down the lateral thigh associated with iliofemoral tendinitis and innominate subluxation.
The diagnosis of neurologic injuries and diseases can be frustrating because of the transient nature of many symptoms and signs. In addition to frequent symptomatic peaks and valleys, neurologic symptoms may mimic a large variety of organic and functional disturbances. The various aspects of general nerve injury which do not lend themselves to a regional basis are discussed in this section. Some of the topics discussed will be infrequently seen in the active athlete, but they often arise with the week-end athlete who seeks attention long after the condition has manifested.
Examination
History
All symptoms of pain, neurologic episodes, malcoordination, and behavioral changes should be investigated thoroughly. Symptoms of headache, weakness, sensory perversions, seizures, tics, syncope, and vertigo lend suspicion to a neurologic disorder. One should assess the nervous system in relation to its influence on other systems and the manner in which its functions are influenced by all the other systems of the body. If a problem is somatic, for example:
(2) consider the visceral and somatic structures that receive innervation from those same areas, and
(3) consider the influence each may have on the others.
Spinal Reflexes and Muscle Tone
Healthy muscle possesses a small amount of tension even at complete rest. It feels resilient rather than flabby. During passive manipulation of a joint, a slight degree of resistance is encountered in the muscle that is not a conscious effort on the part of the patient. Thus, the chief characteristics of normal muscle tone are subdued activity during relaxation and an involuntary reaction opposing mechanical stretch. If the function of the ventral roots are impaired, a muscle loses its tone immediately; and the same is true if the dorsal roots containing sensory fibers from the muscle are damaged. Thus, tone must be considered not a property of muscle itself, but of reflex activity.
The basic neural mechanism for maintaining muscle tone is the stretch reflex. In addition to this function of tone maintenance, the stretch reflex is responsible for regulating tension within various muscle groups which provides the basis of postural muscle tone on which voluntary movements are superimposed. Stretch (myotatic) reflexes are tested via the tendon reflexes.
While a diagnosis of a neurologic disorder cannot be determined by reflexes alone, they are important aids in establishing the type and location of a lesion. Deep reflexes vary in direct proportion to muscle tone. Superficial reflexes apply to any reflex phenomenon which may be induced by a light stimulus such as stroking the skin with a wisp of cotton, resulting in horripilation (gooseflesh) or muscle contraction. Note that:
(2) In lesions of a lower motor neuron or the motor fibers from the anterior horn cells of the cord, both the deep and the superficial reflexes are decreased or absent.
Evaluating the Sensory System
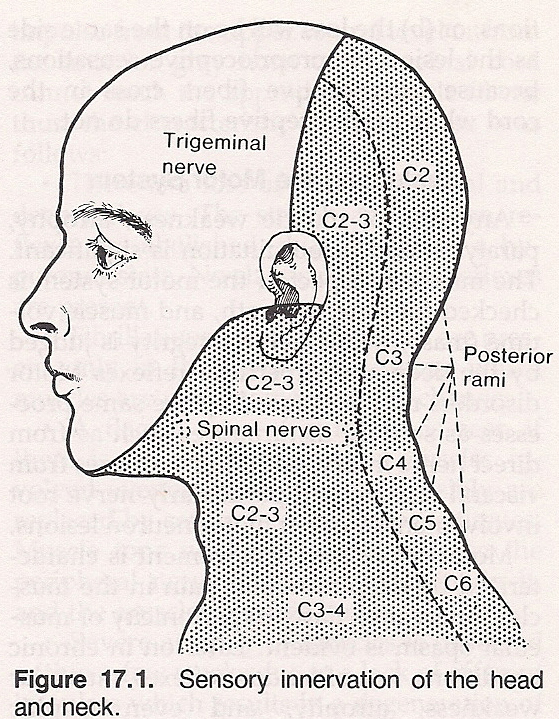
Diagnostic Sensory Areas. Most skin areas are innervated by an overlapping nerve supply from adjacent nerve branches, thus making it difficult in testing cutaneous sensations to isolate a specific spinal nerve that may be affected. However, in certain parts of the body, there are isolated areas of cutaneous innervation by a specific nerve (diagnostic sensory areas). Skully lists the more important areas as follows:
Peripheral vs Central Lesions. By evaluating the sensory bed, it is often possible to determine if a lesion is in the peripheral nerves or whether it is in the central system:
(2) Central lesions cause a sensory loss from the level of the lesion caudally in the following manner:
(b) the loss will be on the same side as the lesion for proprioceptive sensations because exteroceptive fibers cross in the cord while proprioceptive fibers do not.
Evaluating the Motor System
Any sign of muscle weakness, atrophy, paralysis, and incoordination is significant. The muscular aspect of the motor system is checked for tone, strength, and muscle volume (mass), while nerve integrity is judged by the deep and superfical reflexes. Motor disorders may be caused by the same processes as sensory disturbances such as from direct nerve injury, pathology, reflexes from visceral organs, and particularly nerve root involvement or upper motor neuron lesions.
Motor nerve root involvement is characterized by deep muscular pain in the muscles innervated. Early hypertonicity or muscular spasm is evident. Later or in chronic conditions, loss of tendon reflexes, muscular weakness, atrophy, and even trophic changes in the overlying skin may be present. Motor disturbances from upper motor lesions may also be a factor (hyperreflexia). Remember that abnormal reflexes, particularly if bilateral or similar in other reflexes, may be normal for a particular person. All signs must be correlated.
Muscle Mass. Palpation and mensuration are used to determine muscle volume. Upon palpation, there should be a mass that is symmetrical bilaterally. A decrease in size (eg, midcalf or thigh) is indicative of atrophy and usually associated with some degree of hypotonicity. Atrophy is difficult to evaluate in the aged or malnourished individual. The affected muscle becomes shrunken, poor in tone, and weak in strength. Take age, sex, occupation, righthandedness and lefthandedness into consideration.
Muscle Tone. The typical feeling of a normal muscle upon palpation is one of resilience. An increased perception of tone by the examiner denotes a hypertonic muscle; decreased tone, a hypotonic muscle. In evaluating muscle tone, age, sex, body structure, occupation, physical avocations, and nutritional status of the patient must be considered.
Paralysis. True paralysis is the complete inability to control a muscle or group of muscles. Spastic paralysis is commonly seen in lesions of upper motor neurons. Flaccid paralysis occurs in the peripheral type of nerve lesions affecting the lower motor neurons of the anterior horn cells. Peripheral nerve paralyses are especially apt to be accompanied by sensory symptoms, electrical changes, and wasting. Brain-originating paralyses have relatively few sensory symptoms (sometimes paresthesias) and relatively slight wasting; mental changes, coma, or convulsions often precede or follow. Cord paralyses may or may not show these associations but are often accompanied by disorders of the bladder and rectum.
The extent of the symptomatology frequently offers a clue to the location of the disorder. In most chronic pyramidal tract lesions, especially when the trauma has been sudden but not insidious, a partial recovery of control is expected. This occurs mostly in the large proximal muscles of the shoulder and hip. Disorders of the pyramidal tract commonly produce defects that are more conspicuous in the upper limb. This is possibly because highly skilled movements are more prevalent there in comparison to mass contractions.
Electrical Examinations. Electrical examination of muscles and nerves is often indispensible in affections of peripheral nerves. Such tests help to determine if disease of the upper or lower motor neuron is being delt with, help to determine if the nerve is interrupted, and help to determine if the muscles are undergoing degeneration.
LOWER MOTOR NEURON LESION CHARACTERISTICS
Lesions of the lower motor neurons result from fractures, trauma, infection, toxins, vascular disorders, tumors, congenital malformation, and degenerative processes. Lesions involving spinal nerves or peripheral nerves induce both motor and sensory losses. In this type of lesion, the neuronal impulse from the upper central level or from the anterior gray horn of the spinal cord cannot reach the appropriate muscle fibers; thus, the characteristic clinical picture is as follows:
UPPER MOTOR NEURON LESION CHARACTERISTICS
Any lesion producing an interruption of connections between the motor cortex or subcortical levels and the motor axons found in the anterior horn of the spinal cord is considered to be an upper motor neuron lesion. Such a lesion may interrupt corticospinal fibers or extrapyramidal fibers, or both, since the pyramidal and extrapyramidal systems are so closely associated that lesions involving one will invariably encompass both. On the other hand, any lesion producing damage to motor neurons whose axons reach skeletal muscle fibers produces a lower motor neuron lesion, whether the destruction is in the anterior horns, ventral roots, or peripheral nerves.
Lesions of the upper motor neurons may occur anywhere along their course and may be the result of hemorrhage, thrombosis, trauma, inflammation, neoplasm, or a degenerative process. The classical clinical picture of an upper motor neuron lesion is portrayed as follows:
Evaluating the Cerebellar System
Once the cerebral cortex receives an afferent impulse and decides what task must be performed in response, the cerebellum coordinates the reaction so that the act will be carried out smoothly.
Signs of Cerebellar Lesions. The major motor signs seen in cerebellar lesions include tremor, nystagmus, ataxia, decomposition of movement, dysmetria, dysdiadochokinesia or adiadochokinesia, scanning speech, hypotonia, and asthenia. Other signs include vertigo, cerebellar fits presenting a rigid convulsion, and vocal dysarthria characterized by explosive, slurred speech peculiar to cerebellar lesions. Note any sign of skew deviation of the eyes where one eyeball is deviated up and outward and the other is deviated down and inward (brachium pontis lesion). In time, cerebellar defects are compensated for to a considerable degree by other brain mechanisms; thus, symptoms are less severe in slowly progressing diseases than in acute cerebellar disorders.
Common Symptoms of Neural Disorder
Weakness
Weakness (fatigue) and nervousness are frequently presented together, and can usually be attributed to psychological disorders, physical disorders, or appear as a complication in organic disease. Weakness in the absence of further symptoms or signs is indicative of an emotional problem (eg, depression). However, weakness may be the only symptom of an early systemic disease (eg, Guillain-Barre syndrome).
Weakness is characterized by feelings of lassitude, tiredness, weariness, depletion, exhaustion, malaise, loss of energy and motivation. It may be general or local. If local, the weakness may be described in lower or upper extremities, either distal or proximal. It may be localized in the trunk, head, or in respiration. It is important to analyze weakness in terms of body segments because weakness always follows a neuroanatomic distribution in organic disease.
Neuromuscular defects are usually marked by weakness, and fatigue may be an early symptom in the myopathies. A rule of thumb is that proximal weakness is the result of a myopathy, while a distal weakness is caused by a neuropathy. Weakness upon exertion that is progressive with muscular effort is called fatigability.
Nervousness
Nervousness is sensed as a feeling of tension, arousal, uncertainty, a threatened loss of self-control, alarm, and vulnerability. It usually results from psychological disturbances or abnormalities in the fight-flight (ergotropic) response. Psychogenic nervousness and the nervousness associated with hyperthyroidism are not usually difficult to differentiate, sometimes even from the case history. Differentiation between fatigue of psychic and physical origins is more difficult to obtain unless there is no evidence of any physical disturbance. When there is, there is usually fatigue from both psychic and physical origins.
Pain
All pain is mediated by the nervous system, yet only some pain originates from neuropathology. When an inflammatory process involves the sensory fibers, neuralgia is often presented along the total nerve course. For example, in medial nerve entrapment (carpal tunnel syndrome), pain is rarely localized in the wrist; it often extends into the upper arm and shoulder. Hypersensitive points can often be located where touching a certain point only slightly initiates severe radiating pain.
Fortunately, nerve course is fairly predictable and varies little because of body type. The exception to this is that nerves which normally pass over or under a muscle, may pass through it thus subjecting it to abnormal stress. The sciatic nerve, for example, may pass over, under, or through the piriformis, or it may be divided. Abnormal bone formation may also be a consideration such as a cervical rib encroaching upon a branch of the brachial plexus. A callus formation may have the same effect.
DERMATOMES
Inflammation or compression of dorsal nerve roots irritate pain fibers and commonly produces pain felt along the anatomic distribution of the roots affected (dermatome). Myotomes are groups of muscles innervated by a single spinal segment. Evaluation of the integrity of the neurologic levels rests upon the examiner's knowledge of dermatomes, sclerotomes, myotomes, and reflexes. Pain may be limited in distribution to one or more dermatomes (radicular pain).
Sensory changes other than pain may be associated with dorsal root irritation; eg, localized areas of paresthesia or hyperesthesia. If the pathologic process is a progressive one which gradually destroys fibers, dorsal roots finally lose their ability to conduct sensory impulses, resulting in hypesthesia which eventually leads to anesthesia.
TYPICAL CAUSES OF PAIN AND PARESTHESIA
Local paresthesia, as expressed by prickling, tingling, crawling, or burning sensations, is not uncommon in lesions of the cerebral cortex. Typical causative factors include:
EXTREMITY PAIN
The origin of nerve root lesions may be traced during the history to trauma, herniated discs, compression, hypertrophic changes in the vertebrae, neoplasms, and inflammation of the nerve root. Peripheral nerve disease frequently indicates a history of trauma of the entrapment neuropathies. Rare nutritional disorders may result in a polyneuropathy because of unfavorable metabolic activities within the nerve cells. Peripheral neuritis, less common than peripheral neuropathy, can be classified into one of three types: infectious, allergic, or idiopathic.
Limb pain may be the result of any structural disorder of the extremities or a disturbance elsewhere wherein the sensory phenomena are referred to the limbs. Pain situated in various parts of the extremities will reveal the point of origin by its peculiar location and quality. The pain may be of mechanical, chemical, thermal, toxic, nutritional, metabolic, or circulatory origin, or a combination of some of these factors, depending upon the nature of the pathologic process involved. The most important clues toward determining cause type of pain, its distribution, and its associated symptoms-are the result of a carefully taken case history.
Referred Pain and Reflexes
Pain in one region of the body may indicate disease elsewhere because nerve supply often overlaps; eg, pain associated with the ureter can result in reflex spasm of the lumbar muscles. Such pain radiates to distant parts of the body depending upon the intensity of the stimulus, amplitude of the afferent impulse, and the excitatory state of the spinal cord at the level into which the noxious impulses enter.
Visceral disease or dysfunction frequently refers pain to the spinal segments supplying the involved viscera and also alters the function of other viscera sharing the same nerve supply. In addition, the probability should be considered of somatic dysfunction occurring in segmentally involved areas causing visceral dysfunction or of other somatic structures sharing the same nerve supply. The nervous system is not a one-way street: somatosomatic, somatovisceral, viscerovisceral, and viscersomatic reflexes must be considered.
Cervical Reflexes. Cervical reflexes can be easily overlooked. Vertigo makes basilar insufficiency or Meniere's syndrome suspect, but vertebral artery ischemia due to upper cervical dysfunction or an atlanto-occipital subluxation secondary to scoliosis may be the reason. In blackout spells of an unexplained nature, epilepsy and arterial occlusive disease are suspect, but cervical somatic dysfunction involving the cervical ganglia may be the cause. Numbness or tingling in the hands is seen in a number of neuropathies. However, the cause may be musculoskeletal in origin such as degenerative disease or somatic dysfunction of the cervical spine, brachial plexus entrapment due to clavicular and upper rib abnormality, or carpal tunnel syndrome. In a lower cervical motor-unit dysfunction resulting in brachial distribution symptoms, there are somatosomatic reflexes which have afferents from and efferents to the soma.
Shoulder Symptoms. Gallbladder disease associated with referred pain near the right scapular tip is an example of viscerosomatic reflexes having afferents from a viscus and efferents to a somatic area. Frequently overlooked is the gallbladder reflex causing cardiac arrhythmia. However, several diseases may refer pain to the shoulder or arm other than the gallbladder such as coronary artery disease, empyema, pneumothorax, pericarditis, mediastinal lesions, peptic ulcer, diaphragmatic hernia, perisplenitis, and subphrenic abscess. In coronary occlusion associated with nausea and vomiting, there are viscerovisceral reflexes which have afferents from a viscus and efferents to a viscus. Pain radiating to the arm may also be a reflex from brachial neuropathy caused by dysfunction or degenerative disease of the cervical spine or a trigger point.
Chest Symptoms. Several common chest symptoms may indicate visceral disease or as often referred musculoskeletal problems. Ventilatory impairment is usually suspected in dyspnea, but it may be the result of rib-cage dysfunction, spondylitis, or paravertebral muscle spasm and pain. Air hunger at rest is a cardinal sign of anxiety and often seen in chronic obstructive pulmonary disease; it is, however, also a reflex sign of rib-cage dysfunction of a musculoskeletal nature. Chest pain points to coronary insufficiency, dissecting aneurysm, or may be of esophageal or pleural origin; but chest pain may also be the result of somatic rib-cage dysfunction, costochondral or costovertebral strain, or be referred pain from the gallbladder, stomach, duodenum, or pancreas.
In chest pains associated with a cough, pulmonary infections, pneumonia, lung abscess, and bronchitis are usually suspected, along with pleuritis and lung or pleural tumors. Reflex considerations would include costovertebral dysfunction, costochondral dysfunction or separation, or costal fracture. In cough with chest pain, one normally thinks of acute or chronic infection, chronic bronchitis, bronchial tumor, pulmonary embolism, broncholith, brochchiectasis, postnasal discharge, or the inhalation of irritants. However, reflexes from clavicular strain affecting recurrent laryngeal nerves, cervical subluxation, or cerumen impaction should not be overlooked.
Referred Pain and Tenderness. The segmental distribution of referred pain and tenderness in visceral dysfunction is usually listed as follows; however, authorities differ somewhat. Bladder body: S1-S4
Bladder neck: T11-L1
Breast: T4-5
Epididymis: T11-L1
Esophagus: T5-T8
Heart: C3, T1-T3
Intestines: T9-T12
Kidney: T10-T11
Liver and
gallbladder: T6-T10
Lungs: C3-C4, T1-T10, but especially T3-T5
Ovary: T10
Prostate: T10-T12, L3, S1-S3
Rectum: S2-S4
Stomach: C3-C4; cardiac portion, T6-T7;
pyloric portion, T9
Testis: T10
Ureter: T12-L1
Uterine body: T10-L1
Uterine neck: S1-S4
Hysterical Anesthesia or Palsy
Hysterical anesthesia or palsy following injury to an arm or leg is not rare. The involvement of the extremity in both sensory loss or motor control, ideational rather than neuroanatomic, is a characteristic feature of this neurosis. For example, a hysterically anesthetic arm will be insensitive as far as the shoulder line, whereafter normal sensation abruptly returns. This contrasts with sensory zones demarcated by injury to a peripheral nerve or spinal cord segment. Motor loss is similarly referred to the arm as a whole rather than to identically innervated muscle groups. These nonanatomic findings, as well as normal or hyperactive reflexes, prompt electric responses, and good muscle tone serve as signs differentiating functional from organic nerve, nerve root, and cord-segment lesions.
Peripheral Nerve Injuries
(2) loss of all sensation, including proprioception, in the skin areas distal to the lesion.
Trophic lesions of the joints, muscles (atrophy), skin, and nails are common. They blend and are somewhat explained as the results of vasomotor changes.
Classification of Nerve Trauma
Nerve trauma occurs from contusion, stretching, or laceration:
Nerve Pinch or Stretch Syndromes
Nerve "pinch" or "stretch" syndromes are especially common in sports. They are often seen in football "spearing" with the neck in flexion, but these syndromes appear throughout the cranium, spine, pelvis, and extremities in many sports. Hardly any peripheral nerve is exempt. Terms used synonymously include nerve compression, nerve contusion, nerve lesion, nerve pinch syndrome, nerve root syndrome, nerve stretch syndrome, radiculopathy, spinal dysarthria, subluxation, or traumatic neuritis.
A nerve stretch syndrome is commonly associated with sprains, lateral cervical flexion with shoulder depression (eg, football blocking, tackling), or dislocations. Nerve fibers may be stretched, partially torn, or ruptured most anywhere in the nervous system from the cord to peripheral nerve terminals.
A nerve pinch syndrome may be due to direct trauma (contusion and swelling), subluxation, a protruded disc which results in nerve compression, or fracture (callus formation and associated posttraumatic adhesions). Any telescoping, hyperflexion, hyperextension, or hyperrotational blow or force to the spine may result in a nerve "pinch" syndrome where pain may be local or extending distally. In sports, nerve pinch syndromes are less common than nerve stretch syndromes but more serious.
Examination
Painstaking examination is required as multiple nerve injury, related tendon or other soft-tissue damage, and fractured bones complicate the picture. The 3
immediate site of injury should be first investigated, followed by the part's general appearance, voluntary motion, reflexes, and vasomotor changes. In addition to sensory and motor loss, the response to electrical stimulation should be evaluated.
Management
The effect of treatment depends largely upon early recognition of the nerve injury with removal of the initiating cause. Management consists of support of the affected part and normal regimens for severe contusions. As with most injuries, associated or concomitant subluxations or fixations must be adjusted to aid recovery, and sites of abnormal reflexes and stasis must be normalized. Cold is applicable in the acute stage to reduce adjacent swelling and bleeding. Heat, massage, passive and active exercises, electrical stimulation, and nutritional control are helpful.
A reaction of degeneration added to typical sensory and motor loss is indicative of complete anatomic or physiologic nerve damage usually requiring surgical intervention. If surgery is required, careful attention must be given to postoperative care directed to maintaining as much as possible normal joint flexibility, fascia and ligamentous resiliency, muscle elasticity, and adequate nutrition to all tissues involved. Approximately one month before it can be detected clinically, an electromyogram will exhibit reinnervation.
When a peripheral nerve fiber is permanently destroyed by either trauma or disease, the portion distal to the nerve cell body completely degenerates, and the fiber loses its myelin sheath in the process. In time, the isolated fiber stump tries to sprout in random directions in an attempt to make a bridge with the severed portion of the nerve. Some of these sprouts may, apparently by chance, cross the gap and enter neurilemmal tubes leading to a peripheral motor or sensory terminal. Function may be restored if the connection is a suitable match. Fibers in the spinal cord and brain do not regenerate effectively; however, recent evidence discloses that some regeneration can occur.
Major Types of Neuritides
Local Neuritis
Chronic Neuritis: Paresthesias are witnessed over the area of nerve distribution along with tenderness on palpation of the nerve trunk and muscles supplied by the nerve. Hypesthesia and hypalgesia are usually present. Diminished reflexes and motor weakness of the muscles supplied by the affected nerve are typical.
Radiculitis: Paresthesia and sensory changes are expressed similar to those present in typical neuritis, but the area affected corresponds to dermatome, myotome, and sclerotome of affected roots. Coughing, straining, jugular compression, and other causes of increased cerebral spinal fluid pressure will increase symptoms. In chronic cases, there may be paresis of muscles that are partly supplied by the affected root, but not complete paralysis.
Peripheral Neuritis
Rarely seen in the sportsperson, general peripheral neuritis is seen in such conditions as diabetes, anemia, and vitamin deficiency. Decreased sensation perception will be noted, with proprioception affected most. Stocking-like distribution with a poorly defined border is commonly witnessed. Glove-like distribution may appear later along with paresthesias in the most distal areas of sensory distribution. The clinical picture does not conform to either dermatome or nerve patterns of distribution.
Common Reflex Irritations
In addition to nerve root involvements and/or peripheral irritations, many sensory disturbances can be caused by reflex irritation to somatic musculoskeletal tissues. These symptoms lack the typical features of nerve root involvement such as observed in cervical compression tests and usually do not create significant motor changes. They may arise from inflammatory tissues or fibrotic muscles, tendons, or ligaments which characteristically act as trigger areas. That is, their stimulation such as with deep pressure initiates the reflex pain.
Some of the typical reflex neuralgias are listed in the following examples:
Peripheral Nerve Entrapment Syndromes
A peripheral entrapment syndromes represents a distinct type of neuropathy in which a single nerve is compressed at a specific site (eg, within fibrous tissue, a fibrous-osseous tunnel, or a muscle), either by external forces or by surrounding tissues. Local impairment of blood supply may further damage the entraped nerve if associated vessels become stretched, kinked, or compressed.
So that a patient may avoid unnecessary pain and disability, it is important to identify a peripheral entrapment syndrome rapidly through careful examination and appropriate diagnostic studies such as electromyography, nerve conduction evaluations, and roentgenography. Severe impairment of nerve function is usually only reversible in its early stages.
Table 17.1. Common Nerve Entrapment Syndromes
UPPER-EXTREMITY SYNDROMES
Syndrome Site Nerve Major Findings*
Anterior Proximal Anterior Abnormal pinch sign; normal
interosseous forearm interosseous sensations; flexor pollicis longus,
pronator quadratus, and flexor
digitorum profundus weakness;
poorly defined ache in forearm.
Carpal Wrist Median Pain, paresthesiae, numbness, and
tunnel poor two-point discrimination
in thumb and radial 2 1/2 fingers;
hypoesthesia especially on palmar
aspect ofsecond digit; thenar
weakness and wasting; positive
Tinel's and Phalen's signs.
Cubital Elbow Ulnar Sensory loss in ulnar 1 1/2 fingers
tunnel and ulnar aspect of the hand;
weakness and wasting of ulnar
intrinsic and flexor digitorum
profundus; ache in medial elbow
and forearm; little finger
numbness; positive Tinel's sign.
Guyon's Wrist Ulnar Sensory loss in ulnar 1 1/2 fingers;
canal weakness and wasting of ulnar
intrinsic muscles.
Postcondylar Elbow Ulnar Sensory loss in ulnar 1 1/2 fingers
groove and ulnar aspect of the hand;
weakness and wasting of ulnar
intrinsic and flexor carpi ulnaris
muscles; elbow joint deformity.
Posterior Proximal Posterior Normal sensation; wrist drop;
forearm interosseous dull ache in dorsal forearm;
difficult finger extension.
Pronator Proximal Median Proximal forearm pain and
forearm tenderness; flexor pollicis
longus and abductor pollicis
brevis weakness; paresthesiae in
thumb and radial 3 1/3 fingers;
forearm and hand pain;
positive Tinel's sign.
Radial Midarm, Radial Sensory loss in radial side of
spiral dorsal hand; wrist drop; weak
groove wrist and finger extensors;
possible sensory impairment in
web of thumb.
Crutch or Axilla, Radial Sensory loss of radial forearm;
sleep palsy humeral loss of elbow extension;
groove wrist drop.
LOWER-EXTREMITY SYNDROMES
Syndrome Site Nerve Major Findings*
Femoral Inguinal Femoral Sensory loss of anteromedial
area or thigh; weakness and wasting of
pelvis quadriceps femoris; local
tenderness in groin; impaired
knee jerk.
Meralgia Inguinal Lateral Sensory loss, paresthesiae,
paresthetica area cutaneous of burning pain, and numbness in
thigh anterolateral thigh; no
motor weakness.
Obturator Pelvis Obturator Sensory loss of superomedial
thigh; thigh adductor weakness.
Peroneal Neck of Common Sensory loss of dorsal foot
fibula peroneal and lateral leg; foot drop;
steppage gait; local tenderness;
anterior and lateral
compartment atrophy.
Tarsal Ankle Posterior Burning pain and paresthesiae
tunnel tibial of sole and toes; weakness of
intrinsic foot muscles.
* Adapted from Reddy
In health, the autonomic divisions are tonically stimulated to maintain a physiologic balance. However, for various reasons, this balanced harmony may be shifted in favor of one or the other division and create visceral malfunction. An understanding of visceral neurology is indispensible to appreciate and explain the pathophysiologic processes involved. The vegetative nerves correlate and integrate action in the body and are often subjected to an amount of stimulation necessary to overbalance their normal function. When the autonomic system is involved, causalgic pain must be differentiated from somatic pain.
(1) activating or inhibiting to a given muscle or secreting cell, or
The vegetative nerves consist of two systems which are antagonistic for the most part. Each system also contains neurons that often produce effects opposite to those which are common to that system. This complicates the common idea that the two systems are always antagonistic.
(1) the state of activity of the organ when it receives the stimulus, and
(1) the necessary electrolytes are supplied in the right proportions,
Sympathicotonia and Vagotonia
Irritability, a fundamental property of living tissue, governs an organism's ability to respond to a stimulus if applied with sufficient intensity to create a response. This property lies chiefly with the integrity of the nervous system. In injury or disease, nerve irritation results from an abnormal duration, quantity, or quality of stimulation resulting in an excessive physiologic response. Any interference with impulse generation or transmission must result in a degree of dysfunction.
(1) the soles of the feet,
Neurotherapy and Spondylotherapy
Neuroinhibition. Abnormal reflexes appear to be inhibited more by pressure and cold than by any other methods. For example, a painful splinting erectormuscle spasm can be relaxed by placing the muscle in a position of functional rest and then applying mild continuous stretching or pressure. Cold is an excellent neuroinhibitor, especially with nerves which are located not too deep. Functional inhibition can be gained by stimulating a nerve whose chief function is inhibitory. Pressure may be applied digitally or with a pressor instrument at or near the paravertebral spaces. Steady pressure on the surface of the body, usually applied digitally, over the course of a nerve tends to be a restraining influence. There also appears to be a reflex influence upon vessels and glandular secretions. Certain skin areas (eg, suboccipital, paraspinal, parasacral, perianal, peripheral-meridian) are highly responsive to mild pressure from which reflexes of vasodilation and muscle relaxation can be initiated.
C1–C2:
initiates vagal responses of increased gastric secretion and peristalsis; increased nasal, buccal, and pulmonary mucosal secretions.
(1) applying sinusoidal stimulation to the area of C7,
It has been Johnson's experience when sinusoidal current is used that stimulation should not exceed 30 sec, with current alternated 5 sec on and 5 sec off, at 6–8 cycles, otherwise the reflex becomes exhausted. Others have found that vagal inhibitory action can also be aroused through several methods such as
(1) pinching the sternocleidomastoideus between the thumb and the forefinger and working deeply under the muscle's medial margin,
Autonomic Imbalance
Physiologic Control of Body Activity
Vegetative imbalance implies visceral instability wherein the normal physiologic control of visceral activity throughout the body, or in some organ or system, is so unstable that a comparatively mild stimulus, when applied to the system of unstable cells, is sufficient to produce a marked effect to overcome all antagonistic forces and create a pathologic state. Patients having such an imbalance show reactions beyond what is natural for the stimulus applied. For instance, such factors as subluxations, emotions, fatigue, weather changes, and toxemia produce changes in such individuals which are far greater than would normally be expected.
Stimuli that act upon muscle or secreting cells present either an activating or an inhibiting effect. In the vegetative structures, the divisions are either
(2) nerves of the same system which produce opposing action by different chemical substances through which they transmit their effects to motor cells.
Visceral nerve action varies according to
(2) the transmitter substances which are liberated into the circulation at the site of action. For the most part, parasympathetic effects in the visceral tissues are cholinergic and the sympathetic effects are adrenergic. But this is not exclusively true as there are some cholinergic sympathetic fibers and adrenergic parasympathetic fibers.
Factors Involved in Vegetative Imbalance
Through their innervation of blood vessels, sympathetic fibers reach almost every tissue of the body. They control blood vessel constriction, subdermal structures, heart muscle, sphincter system of the gut and urinary apparatus, parts of the bladder and genitalia and reproductive organs, inhibit many structures in the head and chest, and reach the enteral system's muscles and glands. The adrenergic transmitter of sympathetic action to effector mechanisms is adrenalin-like sympathin; one form of which causes excitation, the other causes inhibition.
The parasympathetics activate the intrinsic eye muscles, glands of the peripheral head, bronchi muscles and glands, the entire enteral system, body of the bladder, and inhibit the heart and provide vasodilation in many structures (especially the head and penis). Choline esters transmit these effects and also cause perspiration (recognized as a sympathetic action) and vasodilation throughout the entire vascular tree.
Vegetative functional activity and control are complex affairs conducted by the cells, the electrolytes, chemicals of the various hormones, and the sympathetic and parasympathetic nerves. The action of these systems is interdependent and can be understood only when considered together because imbalance in one may mean imbalance in all. Imbalance may have as its chief cause a disturbance in any one or more of these factors. The cells may be at fault, the electrolytes that have an important part to play in cellular activity may be abnormal in their proportions, or the chemical or nervous regulators may create too little or too much stimulation. Usually, the cells will do their job if the environment is right. This puts the onus on nerve supply, nutrition, electrolytes, and lymph circulation. Regardless, deviations from the norm result in abnormal function.
Normal vegetative function can be maintained if proper nutrition is supplied the cells and their colloidal phases are usual for the structure under consideration provided
(2) the hormones from the various endocrine glands and vitamins are supplied in normal amounts, and
(3) the activating and inhibiting impulses which are carried to the cells by nerves balance each other or at least fail to overbalance each other. If these factors are not provided, deviations from the normal will lead to vegetative imbalance.
The two common deviations from normal are sympathicotonia and vagotonia (parasympathicotonia). These disorders may be general or limited to certain systems or organs. Although they are expressed in terms of sympathetic and parasympathetic action, this does not mean that the nervous system is primarily at fault. The fault may lie with the cells, electrolytes, hormones, or vitamins. Regardless of cause, there are large numbers of people who have a marked tendency to respond to stimuli which act on one or the other part of the vegetative system to such a degree that it amounts to malfunction or disease.
The disorders most commonly associated with a sympathetic predominance are hyperthyroidism effects, dryness and paleness of the mucous membranes of the head, deficient salivary secretion, tachycardia, dilatation of the stomach, hypochlorhydria, poor digestion, and atonic constipation. Pottenger states that sympathicotonics react more markedly than normal to cold, toxins, and emotions in an adrenalin-like manner. They readily produce reflexes wherein the sympathetics are involved. Contrary to this, parasympathicotonics are particularly susceptible to allergic excitants and respond in an atropine-like manner.
Stimuli to the sympathetic-accelerator side of the autonomic nervous system are initiated frequently by anger, exercise, and emotions. Within a reasonable time, the symptoms created by the stimuli should return to normal. However, if these stimuli are too prolonged or too pronounced, then the balancing parasympathetic should be investigated to see why it is not exerting its proper opposition force.
Common disorders associated with a parasympathetic predominance are lacrimation, hay fever, urticaria, angioneurotic edema, intestinal allergies, sinusitis, rhinitis, pharyngitis, excessive salivary secretion, bradycardia, asthma, hyperchlorhydria, peptic ulcer, diarrhea, spastic constipation, mucous colitis, and anaphylaxis. Addison's disease is a classic parasympathetic disease.
Stimuli to the parasympathetic-brake side of the autonomic system are initiated frequently by bad news, fright, or shock. Again, within a reasonable time, the patient should recover from the effects of these stimuli and emotions return to normal. If these stimuli are too prolonged or too pronounced, then the balancing sympathetics should be investigated to see why they are not exerting their proper opposition force.
Syndromes may be produced by stimuli that act either centrally or peripherally. Toxins, for example, act centrally and result in widespread sympathetic effects. Inflammation in an organ, on the other hand, may act upon the nerve endings therein and create reflex sympathetic or parasympathetic effects only in the specific organs or tissues whose nerves receive the reflex stimulation.
A patient need not be sympathicotonic or vagotonic throughout the vegetative structures. He/she may have a sympathicotonic heart while the rest of the structures are normal or may express symptoms of vagotonia elsewhere such as hyperchlorhydria or spastic colon. The important thing during diagnosis is to assign these phenomena when they arise to the components of the vegetative nervous system to which they belong and determine the cause.
Special Therapeutic Considerations
In addition to osseous spinal adjustment and extremity manipulation, various forms of neurotherapy are worthy of mention. Once structural correction has been made, adjunctive therapy is often helpful in enhancing physiologic balance to speed recovery. That is, once structural interferences with normal nerve transmission has been corrected, peripheral neurotherapy or spondylotherapy may be utilized to inhibit pain, spasm, or enhance healing by stimulation.
At certain points on the body surface, there are areas from which the reflexes of muscle relaxation, vasodilation, and postural competence can be initiated. These are referred to by some as the Valleau zones. The primary zones include
(2) the parasacral areas, and
(3) the suboccipital zones.
Neurotherapy refers to the inhibition of overly active nerve function or the activation of sluggish function. Spondylotherapy is the treatment by physical methods applied to the spinal region. A nerve fiber may be stimulated artificially (ie, mechanically, thermally, chemically, electrically) anywhere along its course.
Certain nerve fibers function specifically for certain sensory and motor acts and may be stimulated at either their central or peripheral ends: efferent nerves are stimulated centrally and afferent nerves peripherally. The ability of sensory nerve stimulation to produce a motor or glandular response is readily demonstrated in eliciting any tendon reflex where superficial percussion produces the characteristic jerk, the muscle-spasm reflex resulting from skin exposure to a cool wind or proprioceptive excitement from strain or sprain, or the salivary response from seeing a person eat a lemon.
Neurostimulation. Deep and rapid short-duration percussion, applied either by hand or by a percussion-type vibrator, upon spinous processes at a rate 1-2/sec for about 20 sec with 30-sec rest intervals can be used to stimulate a spinal center. Prolonged stimulation such as 3 min or longer fatigues excitability and produces an inhibitory effect. When a medium-strength electric current passes through a portion of nerve, an impulse is created at the instant the current is initiated and broken, as evidenced by muscle contraction. Experience has shown that sinusoidal current is the best method to contract involuntary muscle without irritation, but pulsating ultrasound is also effective in stimulating spinal centers. Therapeutic heat in most any form increases nerve conductivity.
Effects of Spinal Center Stimulation:
C3:
initiates phrenic influence to increase depth of diaphragmatic excursions. Note that C3 inhibition is helpful in chronic cough, hiccups.
C4–C5:
initiates lung reflex contraction (eg, used in expiratory dyspnea, emphysema) and pulmonary vascular vasoconstriction.
C6–C7:
reflex center for increasing generalized vasoconstriction and myocardial tone.
T1–T3:
initiates lung reflex dilation (eg, inspiratory dyspnea), dilates stomach body, and contracts pylorus; inhibits heart action (ie, antitachycardia reflex) and gastric hypermotility.
T4:
initiates cardiac and aortic dilation and inhibits viscerospasms.
T5:
initiates pyloric and duodenal dilation when applied to the right side.
T6:
initiates gallbladder contraction when applied to the right side.
T7:
initiates slight visceromotor renal dilation when applied bilaterally and stimulates hepatic function.
T8–T9:
initiates gall duct dilation.
T10–T11:
initiates slight visceromotor renal contraction, enhances pancreatic secretion, relaxes intestines and colon, and stimulates adrenals when applied bilaterally; initiates splenic contraction (and vascular rbc's) when applied on the left.
T12:
initiates prostate contraction and tone of the cecum and bladder sphincter.
L1–L3:
initiates uterine body, round ligament, and bladder contraction; pelvic vasoconstriction; vesicular sphincter relaxation.
L4–L5:
initiates sigmoidal and rectal contraction; increases tone of lower bowel.
Vagal Tone. Johnson states that the tone of the parasympathetics may be increased through several methods such as
(2) moderate percussion of the C7 spinous process,
(3) extending the neck to raise the hyoid,
(4) mild percussion of the upper cervical area,
(5) pressure in an intercostal space, and
(6) rectal dilation.
(2) bilateral submastoid pressure,
(3) concussion over the T2–T4 spinous processes, and
(4) paravertebral pressure near T4.
Tissue Goading and Pressure
Deep tissue goading has been applied within the profession for many decades as a means to arouse driving impulses, break up areas of stasis, and stretch contractures and adhesions. A site of localized stasis or muscle contraction, approximately the size and shape of a small pea, is often the site of noxious reflexes and referred pain. Quite frequently, they are found in the the deep tissues of the iliac crest and associated with sciatic-like pain that persists in spite of vertebral and disc correction, but they may be found almost anywhere in the musculoskeletal system.
A thumb, ball of a finger (never a fingertip), or small-blunt instrument is used to deeply massage (up to patient tolerance) a localized tender site within subcutaneous tissues. During goading, with strokes about 1-inch in length, the skin should not be moved. The therapy is quite uncomfortable but often brings dramatic relief in a few hours when more conservative measures have failed.
Hanes feels that many disorders are the result of a post-traumatic neuritis, produced intrinsically or extrinsically, and has isolated several specific points of major irritation. The sites are palpated as excessively tender local spasms. He recommends a firm, constant pressure with no thumb motion which is easily bearable for the patient. The typical pressure duration is 10-30 sec.
Neurovascular and Neurolymphatic Receptors
Lactic acid is a normal byproduct of muscle contraction; ie, when a muscle contracts, lactic acid is produced. Bennett and Goodheart base their work in this area on the hypothesis that any blockage (eg, inhibitory reflex) of the 3
neurovascular receptors will prohibit the normal lactic acid response from occurring, leading to an accumulation of lactic acid in the muscles. This in turn causes further blood vessel dilation. As vascular dilation occurs through a vasomotor response, any blockage of the neurovascular receptor prohibits normal lactic acid response.
Neurolymphatic receptors are located singularly or in multiples on the anterior and posterior aspects of the body, varying in size from that of a pea to a bean. Most of the larger muscles have about four drainage points; ie, two anterior and two posterior. The neurolymphatic receptors do not correspond to the sites of lymph glands; however, they are related to the lymphatic system according to a hypothesis developed by Chapman and later expanded by Goodheart who has correlated these receptors with the musculature system. It is believed that the neurolymphatic reflex points inhibit normal lymphatic flow when the system becomes "overloaded" and that neurolymphatic receptor "blockage" has the same effect as that of neurovascular blockage; ie, a prohibition of normal dilation and an abnormal lactic acid response.