|
Unconventional Medicine in the United States -- Prevalence, Costs, and Patterns of Use

| Volume 328:246-252 |
 |
January 28, 1993 |
 |
Number 4 |
|
|
Unconventional Medicine in the United States --
Prevalence, Costs, and Patterns of Use
David M. Eisenberg, Ronald C. Kessler, Cindy Foster,
Frances E. Norlock, David R. Calkins, and Thomas L. Delbanco
ABSTRACT
Background Many people use unconventional therapies for health problems, but the extent of this use and the costs are not known. We conducted a national survey to determine the prevalence, costs, and patterns of use of unconventional therapies, such as acupuncture and chiropractic.
Methods We limited the therapies studied to 16 commonly used interventions neither taught widely in U.S. medical schools nor generally available in U.S. hospitals. We completed telephone interviews with 1539 adults (response rate, 67 percent) in a national sample of adults 18 years of age or older in 1990. We asked respondents to report any serious or bothersome medical conditions and details of their use of conventional medical services; we then inquired about their use of unconventional therapy.
Results One in three respondents (34 percent) reported using at least one unconventional therapy in the past year, and a third of these saw providers for unconventional therapy. The latter group had made an average of 19 visits to such providers during the preceding year, with an average charge per visit of $27.60. The frequency of use of unconventional therapy varied somewhat among sociodemographic groups, with the highest use reported by nonblack persons from 25 to 49 years of age who had relatively more education and higher incomes. The majority used unconventional therapy for chronic, as opposed to life-threatening, medical conditions. Among those who used unconventional therapy for serious medical conditions, the vast majority (83 percent) also sought treatment for the same condition from a medical doctor; however, 72 percent of the respondents who used unconventional therapy did not inform their medical doctor that they had done so. Extrapolation to the U.S. population suggests that in 1990 Americans made an estimated 425 million visits to providers of unconventional therapy. This number exceeds the number of visits to all U.S. primary care physicians (388 million). Expenditures associated with use of unconventional therapy in 1990 amounted to approximately $13.7 billion, three quarters of which ($10.3 billion) was paid out of pocket. This figure is comparable to the $12.8 billion spent out of pocket annually for all hospitalizations in the United States.
Conclusions The frequency of use of unconventional therapy in the United States is far higher than previously reported. Medical doctors should ask about their patients' use of unconventional therapy whenever they obtain a medical history.
Unconventional, alternative, or unorthodox therapies are difficult to define, because they encompass a broad spectrum of practices and beliefs. As Murray and Rubel have written, "Many are well known, others are exotic or mysterious, and some are dangerous" [ 1 ]. From a sociological standpoint, unconventional therapy refers to medical practices that are not in conformity with the standards of the medical community [ 2 ]. Here we define unconventional therapies as medical interventions not taught widely at U.S. medical schools or generally available at U.S. hospitals. Examples include acupuncture, chiropractic, and massage therapy.
Studies based on samples in limited geographic areas suggest that the use of unconventional therapy is widespread [ 3 ], [ 4 ], [ 5 ]. In particular, unconventional therapies are frequently used by patients with cancer, [ 6 ], [ 7 ], [ 8 ], [ 9 ], [ 10 ], [ 11 ] arthritis, [ 11 ], [ 12 ], [ 13 ] chronic back pain, [ 3 ], [ 14 ] the acquired immunodeficiency syndrome, [ 15 ] gastrointestinal problems, [ 16 ], [ 17 ] chronic renal failure, [ 18 ] and eating disorders [ 19 ]. Little is known, however, about the overall prevalence, cost, and patterns of use of unconventional therapy in the United States [ 1 ], [ 20 ].
To improve our understanding of the use of unconventional therapy, we conducted a national telephone survey focusing on 16 interventions found, on the basis of pilot research, to be representative of unconventional therapies used commonly in the United States. Our study focused on the following questions: What is the extent of use of unconventional therapy in the United States? How much is spent annually on these therapies, including out-of-pocket and third-party payments? What sociodemographic factors distinguish users of unconventional therapy from nonusers? For what medical conditions do people most commonly use unconventional therapy? And to what extent are medical doctors responsible for or informed about the use of unconventional therapy by their patients?
Methods
Sample
We conducted our survey by telephone between January 18 and March 7, 1991. The sample was selected by means of random-digit dialing [ 21 ]. We limited eligibility to English-speaking persons, 18 years of age or older, in whom cognitive or physical impairment did not prevent the completion of the interview. We designed the survey with a target sample of 1500. Assuming an estimated prevalence of use of unconventional therapy between 10 and 50 percent, we calculated that 1500 interviews should produce estimated prevalence rates with 95 percent confidence intervals of 2 to 3 percent.
Of the initial sample of 5158 telephone numbers, 38 percent were nonworking, and 13 percent were not assigned to households. We declared 221 respondents ineligible because they did not speak English (97), because of cognitive or physical incapacity (96), or because they were temporarily unavailable (28). Among the remaining 2295 eligible respondents, 1539 completed the interview, 653 declined to participate (81 of them before we could establish eligibility), and 103 began the interview but stopped before completing all questions. These figures correspond to a 67 percent overall response rate among eligible respondents. Only one respondent per household was eligible to be interviewed. This person was selected by computer randomization from the list of household members given by the first household member contacted. Persons with responses substantially different from the remainder of the sample (for example, those with frequent visits to a provider of unconventional therapy at no cost) were contacted again by a supervisor for verification or clarification of their responses. Since we asked respondents about the use of unconventional therapy during the 12 months before the interview, we considered the results representative of 1990.
The Interview
We described the interview to the respondents as a survey by investigators from Harvard Medical School that was designed to assess the health care practices of Americans. We made no mention of unconventional therapy while recruiting the respondents. The interviews, which averaged 25 minutes in length, began with questions on the respondents' health, health worries, days in bed at home or in the hospital, and indicators of functional impairment caused by health problems. We then asked the respondents about their interactions with medical doctors during the past 12 months. A "medical doctor" was defined early in the interview as "a medical doctor (M.D.) or an osteopath (D.O.), not a chiropractor or other nonmedical doctor." Throughout the remainder of the interview we used the term "medical doctor." We use the same term in this report when referring to a respondent's provider of conventional medical care.
We next assessed the respondents' medical problems. The interviewers stated: "Now I'm going to read a list of conditions. Please tell me if you have had any of these conditions in the past 12 months." The interviewers then asked about 24 medical conditions and offered a follow-up question, "What other important conditions did you have?" The 24 conditions included common symptoms (such as back problems, digestive problems, dizziness, headache, and allergies), as well as specific diagnoses (such as high blood pressure, diabetes, and cancer). Only 8 percent of the respondents reported conditions not included in our list.
The respondents were then asked to identify the three (or fewer) "most bothersome or serious" health problems from the list they had just provided. These health problems are referred to here as "principal medical conditions." We asked the respondents whether they had seen their medical doctor for each principal medical condition during the past 12 months and what their perceptions of these interactions had been.
At this point we asked respondents about their use of unconventional therapy. The interviewers' text read as follows: "Now I'd like to ask you about your use of some other kinds of therapies and treatments." The respondents were asked whether they had ever used 1 or more of 16 unconventional therapies for their principal medical conditions and, if so, whether they had used any of them in the past 12 months. For example, a respondent listing back problems as a principal medical condition was asked whether he or she had used any of the 16 unconventional therapies for this problem during the past 12 months. The respondents were next asked whether they had used "any other therapy not generally provided by most clinics and hospitals." Only a small number (1 percent of the sample) reported using any other unconventional therapy.
Some of the unconventional therapies studied warrant further clarification. For example, "massage therapy" or "relaxation therapy" may mean different things to different people. A respondent who used "massage therapy" for a specific principal medical condition was asked, "Could you tell me more about your use of massage therapy? For example, what technique do you use?" Similar questions followed a report of the use of herbal therapy, spiritual or religious healing by others, commercial weight-loss programs, lifestyle diets, energy healing, folk remedies, and megavitamin therapy. (With regard to megavitamin use, the interviewers specifically stated that "megavitamin therapy does not include taking a daily vitamin.") Given that some unconventional therapies, such as massage, were available in more than 100 reported varieties, further subclassification of each of the 16 unconventional therapies is beyond the scope of this paper.
When respondents reported the use of unconventional therapy during the past 12 months, we asked whether a "professional" was involved. Specifically, the interviewers described a professional as "someone who provides care or gives advice and is paid for his or her services." Such persons are referred to in this report as "providers of unconventional therapy." Some forms of unconventional therapy typically involve a provider (for example, a chiropractor or acupuncturist), whereas others do not (for example, lifestyle diet or self-help groups). In addition, some users of unconventional therapy may visit a provider less often than once a year but may continue to use the prescribed unconventional therapy. In order to learn more about these variations, we asked about lifetime visits and recent visits (in the past 12 months) to providers of unconventional therapy. We did not ask whether the respondents' providers of unconventional therapy were medical doctors. We asked about total charges for visits to providers of unconventional therapy during the past 12 months and whether insurance paid any of these charges. The interviewers asked whether the respondents had discussed the use of each unconventional therapy with their medical doctors and collected data on the respondents' demographic characteristics. We also asked questions pertaining to the respondents' perceptions of the efficacy of unconventional therapies and the quality of their interactions with the providers. We shall report these data separately.
Pilot research suggested that, in addition to the 16 unconventional therapies we studied, prayer and exercise are commonly used in the United States for purposes related to health. We therefore asked respondents whether they had used prayer or exercise as a medical "therapy or treatment" in the past year. No additional questions were asked about these two activities. In the case of prayer, we thought such questions would be inappropriate. As for exercise, we thought the term was too vague and the practice sufficiently ubiquitous to preclude the gathering of useful data. Unless they are explicitly mentioned, all analyses described here excluded prayer and exercise.
Statistical Analysis
We weighted the data to adjust for variations among households in the number of telephones and number of household members eligible to participate in the survey. We also weighted the data to match our sample to the distribution of the U.S. population, as reported in the U.S. Census, for age, sex, and education. Using the Taylor series approximation method for calculating standard errors, we carried out tests of significance appropriate for weighted data using the SUDAAN software system [ 22 ]. We based our extrapolations of the estimates from the survey to the total U.S. household population (which, according to the U.S. Census Bureau, excludes homeless and institutionalized persons) on preliminary figures from the 1990 U.S. Census, which reports the total U.S. population as 242 million, with 74 percent (approximately 180 million persons) made up of adults 18 years of age or older living in U.S. households.
Results
Characteristics of the Respondents and Generalizability of the Sample
The characteristics of the subjects we interviewed are shown in [ Table 1 ]. The sociodemographic characteristics of the survey population were similar to those in the 1989 U.S. National Health Interview Survey [ 23 ] with respect to age, sex, race, education, marital status, and region of the country.
View this table:
[in a new window]
|
Table 1. Characteristics of the 1539 Subjects Interviewed.
|
|
[ Table 2 ] summarizes the use of unconventional therapy in the 12 months before the survey for all 1539 respondents interviewed. Excluding exercise and prayer, one in three respondents (34 percent) used at least one unconventional therapy in 1990. Nearly two thirds (64 percent) of those who used unconventional therapy did so without visiting a provider of unconventional therapy during the 12 months before the interview, whereas the one third who did see a provider made an average of 19 visits.
View this table:
[in a new window]
|
Table 2. Prevalence and Frequency of Use of Unconventional Therapy among 1539 Adult Respondents in 1990.
|
|
The use of unconventional therapy was not confined to any narrow segment of U.S. society. The rates of use ranged from 23 to 53 percent in all sociodemographic groups we considered. There were no significant differences according to sex or insurance status and only small variations according to the size of the community. The use of unconventional therapy was significantly more common among people 25 to 49 years of age (38 percent) than among those who were younger (33 percent) or older (28 percent) (P<0.05 for both comparisons). The use of unconventional therapy was significantly less common among blacks (23 percent) than among members of other racial groups (35 percent; P<0.05). It was significantly more common among persons with some college education (44 percent) than among those with no college education (27 percent; P<0.05) and significantly more common among people with annual incomes above $35,000 (39 percent) than among those with lower incomes (31 percent; P<0.05). Use was also significantly more common among those living in the West (44 percent) than among those living in the rest of the country (31 percent; P<0.05).
Patterns of Use
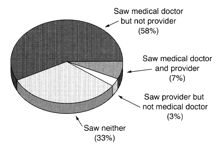
The vast majority of respondents (83 percent) reported one or more principal medical conditions in 1990. More than half (58 percent) of respondents with at least one principal medical condition saw a medical doctor but not a provider of unconventional therapy in 1990; 3 percent saw only a provider of unconventional therapy; 7 percent saw both a medical doctor and a provider of unconventional therapy; and 33 percent saw neither for at least one principal medical condition [ Figure 1 ].
View larger version (34K):
[in a new window]
|
Figure 1. Percentage of Respondents Reporting at Least One Principal Medical Condition Who Saw a Medical Doctor or Provider of Unconventional Therapy in 1990.
Eighty-three percent (1279) of the 1539 respondents reported one or more principal medical conditions. "Provider" denotes a provider of unconventional therapy.
|
|
Table 3 summarizes the rates of use of unconventional therapy for the 10 most common principal medical conditions. On average, 1 in 4 respondents (25 percent) used unconventional therapy and 1 in 10 (10 percent) went to a provider of unconventional therapy for a principal medical condition in 1990. Among all the conditions studied, the frequency of use of unconventional therapy was highest for back problems (36 percent), anxiety (28 percent), headaches (27 percent), chronic pain (26 percent), and cancer or tumors (24 percent). Consistent with the prevalence of cancer in the general population, the use of unconventional therapy for cancer accounted for less than 3 percent of all use. Relaxation techniques, chiropractic, and massage were the unconventional therapies used most often in 1990.
View this table:
[in a new window]
|
Table 3. Use of Unconventional Therapy for the 10 Most Frequently Reported Principal Medical Conditions.
|
|
Among respondents who reported a principal medical condition and used unconventional therapy for that condition, only 4 percent saw a provider of unconventional therapy without also seeing a medical doctor. No respondent saw a provider of unconventional therapy, but not a medical doctor, for the treatment of cancer, diabetes, lung problems, skin problems, high blood pressure, urinary tract problems, or dental problems.
To clarify further the patterns of use of unconventional therapy, we defined and investigated two predominant patterns of care for each principal medical condition: the conventional pattern (in which the respondent sought the services of a medical doctor but did not use unconventional therapies) and the unconventional pattern (the respondent used unconventional therapy with or without seeing a medical doctor). The unconventional pattern was more common than the conventional pattern for 5 of the 10 most frequently cited principal medical conditions: back problems, insomnia, headache, anxiety, and depression.
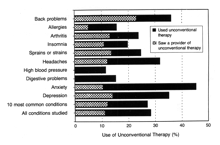
Among respondents who saw a medical doctor for at least one principal medical condition, more than one in four (28 percent) also used unconventional therapy, and one in nine (11 percent) saw a provider of unconventional therapy for the same condition during the 12 months before the survey [ Figure 2 ]. The rates of use of unconventional therapy among those who consulted a medical doctor varied from condition to condition. The probability that an individual patient who saw a medical doctor also used unconventional therapy in 1990 was higher than one in three for patients with anxiety (45 percent), obesity (41 percent), back problems (36 percent), depression (35 percent), or chronic pain (34 percent). Respondents who consulted a medical doctor used unconventional therapy least often for diabetes (2 percent), dermatologic problems (7 percent), urinary problems (10 percent), gynecologic problems (11 percent), dental problems (11 percent), pulmonary problems (11 percent), and high blood pressure (12 percent).
View larger version (112K):
[in a new window]
|
Figure 2. Use of Unconventional Therapy by Respondents Who Saw a Medical Doctor for a Principal Medical Condition in 1990.
The 10 most commonly reported conditions are shown in descending order of prevalence.
|
|
Almost 9 of 10 respondents (89 percent) who saw a provider of unconventional therapy in 1990 did so without the recommendation of their medical doctor. In more than 7 of 10 instances (72 percent), users of unconventional therapy did not inform their medical doctor of their use of the therapy. Medical doctors were most likely to be informed about the use of homeopathy (73 percent), megavitamin therapy (72 percent), and self-help groups (61 percent) and least likely to be informed about folk remedies (11 percent), religious or spiritual healing by others (17 percent), or imagery (19 percent).
As shown in [ Figure 1 ], respondents with one or more principal medical conditions were far more likely to see a medical doctor (65 percent) than a provider of unconventional therapy (10 percent). We observed a similar pattern favoring conventional medical care among the group of respondents who reported principal medical conditions and who used unconventional therapy for these conditions. Such persons were far more likely to have sought treatment from a conventional medical doctor (83 percent) during the past 12 months than they were to have seen a provider of unconventional therapy (36 percent). However, as mentioned earlier, the majority of users of unconventional therapy did not inform their medical doctors of their use of unconventional therapy. As a result, nearly half (47 percent) of respondents who used unconventional therapy for their principal medical condition did so without any professional supervision; that is, without either visiting a provider of unconventional therapy or discussing their unconventional therapy with their medical doctor.
Payment for Unconventional Therapy
Data on reimbursement for expenditures for unconventional therapy are shown in [ Table 4 ]. The majority of respondents (55 percent) paid the entire cost of their visits out of pocket. Third-party payment was most common for the services of herbal therapists (83 percent), providers of biofeedback (40 percent), chiropractors (39 percent), and providers of megavitamins (30 percent).
View this table:
[in a new window]
|
Table 4. Payment for Unconventional Therapy in the United States in 1990.
|
|
National Projections of Use and Expenditures
Extrapolation to the total U.S. household population suggests that in 1990 an estimated 61 million Americans used at least 1 of the 16 unconventional therapies we studied and approximately 22 million Americans saw providers of unconventional therapy for a principal medical condition. Fourteen of the 16 unconventional therapies studied were used by an estimated million or more persons in 1990.
The estimated number of ambulatory visits to providers of unconventional therapy in 1990 was 425 million (95 percent confidence interval, 302 million to 548 million). This number exceeds the estimated 388 million visits in 1990 to all primary care physicians (general and family practitioners, pediatricians, and specialists in internal medicine) combined [ 24 ].
National projections of expenditures for unconventional therapy are summarized in [ Table 5 ]. If one assumes that charges for visits to providers of unconventional therapy were paid in full, Americans spent approximately $11.7 billion for these services in 1990. This estimate refers only to the services of providers and does not include expenditures for drugs such as herbs or for medical equipment, devices, books, and other materials.
View this table:
[in a new window]
|
Table 5. National Projections of Expenditures for Unconventional Therapy in the United States in 1990.
|
|
We investigated two additional expenditures by asking respondents about their use of commercial diet supplements (such as instant diet formulas, diet pills, and prepackaged meals) and over-the-counter megavitamins. Respondents who used these supplements reported out-of-pocket expenditures averaging $228 per person per year for diet supplements and $203 per person per year for megavitamins. These results yield national projections of approximately $1.2 billion and $0.8 billion, respectively. Adding these supplemental expenses to the projected expenditures for all visits to providers of unconventional therapy, we estimate that expenditures in 1990 amounted to $13.7 billion.
The total projected out-of-pocket expenditure for unconventional therapy plus supplements was $10.3 billion in 1990. This is comparable to the out-of-pocket expenditure for all hospital care in the United States in 1990 ($12.8 billion), and it is nearly half the amount spent out of pocket for all physicians' services in the United States ($23.5 billion) [ 25 ].
Discussion
We found that unconventional medicine has an enormous presence in the U.S. health care system. An estimated one in three persons in the U.S. adult population used unconventional therapy in 1990. The estimated number of visits made in 1990 to providers of unconventional therapy was greater than the number of visits to all primary care medical doctors nationwide, and the amount spent out of pocket on unconventional therapy was comparable to the amount spent out of pocket by Americans for all hospitalizations. Roughly 1 in 4 Americans who see their medical doctors for a serious health problem may be using unconventional therapy in addition to conventional medicine for that problem, and 7 of 10 such encounters take place without patients' telling their medical doctors that they use unconventional therapy. Furthermore, use is distributed widely across all sociodemographic groups.
There are limits to the representativeness of our sample because it was confined to households with telephones. People living in households without telephones, those in shelters or on the street, and those in institutions were not sampled. In addition, we excluded non-English-speakers and persons for whom the interview would be burdensome because of physical or mental impairment. The frequency and patterns of use of unconventional therapy among these subgroups (and among children) are not known.
As regards the generalizability of the responses of the 67 percent of the respondents who completed the interview, we made two sets of comparisons with preexisting national surveys. Our sample corresponded with the distribution of the subjects of the National Health Interview Survey [ 23 ] with respect to age, sex, race, social class, and other sociodemographic variables, suggesting that our sample was representative of the U.S. household population. Compared with the national Health and Nutrition Examination Survey, [ 26 ] however, our survey involved fewer people who reported poor health on a five-point scale of health status (3 percent vs. 7 percent). This underrepresentation of respondents with poor health reflects our exclusion of those for whom the survey would have been burdensome because of their physical incapacity. Since we found that persons who reported poor health had substantially higher rates of use of unconventional therapy than those who perceived themselves to be in better health (52 percent vs. 33 percent), the study design may have resulted in an underestimate of the use of unconventional therapy.
Unconventional therapies are generally used as adjuncts to conventional therapy, rather than as replacements for it. Users of unconventional therapy were more likely to see a medical doctor than a provider of unconventional therapy, and visits to providers for serious medical conditions in the absence of contact with a medical doctor were rare. Moreover, in contrast to previous reports of research involving patients with cancer, [ 6 ], [ 7 ], [ 9 ] no respondents in this national survey who identified cancer as a principal medical problem reported seeing a provider of unconventional therapy without also seeing a medical doctor for this condition.
Although much of the literature dealing with unconventional medical practices focuses on potentially life-threatening or debilitating illness, the use of unconventional therapy was not limited to life-threatening conditions. Projections from survey data indicate that millions of Americans used unconventional therapy for each of the conditions we studied, the majority of which are not life-threatening. Put somewhat differently, it is likely that virtually all medical doctors see patients who routinely use unconventional therapies. Indeed, for medical doctors currently caring for patients with back problems, anxiety, depression, or chronic pain, the odds are greater than one in three that a patient is simultaneously using unconventional therapy for these medical problems without disclosing this fact.
Our results also suggest that the use of unconventional therapy is not limited to the person's principal medical conditions. A full third of the respondents who used unconventional therapy in 1990 did not use it for any of their principal medical conditions. From this fact we infer that a substantial amount of unconventional therapy is used for nonserious medical conditions, health promotion, or disease prevention. However, these issues were not a focus of our inquiry.
Although users of unconventional therapy are more likely to be in contact with medical doctors than with providers of unconventional therapy, fewer than 3 in 10 users of unconventional therapy mention its use to their medical doctors. Moreover, roughly half of those who use unconventional therapy for their principal medical conditions have no supervision of this treatment by either a medical doctor or a provider of unconventional therapy. Extrapolations to the U.S. population suggest that approximately 20 million Americans fall into this unsupervised category.
Our observation that the majority of users of unconventional therapy did not discuss this therapy with their medical doctors suggests a deficiency in current patient-doctor relations. Perhaps this lack of communication derives from medical doctors' mistaken assumption that their patients do not routinely use unconventional therapies for serious medical problems. Perhaps medical doctors do not discuss the use of unconventional therapies because they lack adequate knowledge of these techniques. In either case, this failure to communicate is not in the best interest of the patients, since the use of unconventional therapy, especially if it is totally unsupervised, may be harmful [ 11 ], [ 27 ].
Medical doctors should begin to ask their patients about their use of unconventional therapy whenever they obtain a history. Some doctors may be uncomfortable with this line of questioning. Nonetheless, as Kleinman and colleagues suggested more than a decade ago, [ 28 ], [ 29 ] an exploration of the use of unconventional therapy and enhanced understanding of these practices will improve both communication between patients and doctors and clinical care. We suggest that medical schools include information about unconventional therapies and the clinical social sciences (anthropology and sociology) in their curriculums. The newly established National Institutes of Health Office for the Study of Unconventional Medical Practices should help promote scholarly research and education in this area.
Supported by a contract with the John E. Fetzer Institute and a grant from the Nathan Cummings Foundation.
We are indebted to Ms. Debi Arcarese for technical and editorial assistance.
Source Information
From the Division of General Medicine and Primary Care, Department of Medicine, Beth Israel Hospital and Harvard Medical School, Boston (D.M.E., T.L.D.); the Institute for Social Research, University of Michigan, Ann Arbor (R.C.K., C.F.); the Division of General Medicine, Department of Medicine, New England Deaconess Hospital and Harvard Medical School, Boston (D.R.C.); and Chicago College for Osteopathic Medicine, Chicago (F.E.N.).
Address reprint requests to Dr. Eisenberg at the Division of General Medicine and Primary Care, Beth Israel Hospital, 330 Brookline Ave., Boston, MA 02215.
References:
-
Murray RH, Rubel AJ. Physicians and healers -- unwitting partners in health care. N Engl J Med 1992;326:61-64
-
Gevitz N. Three perspectives on unorthodox medicine. In: Gevitz N, ed. Other healers: unorthodox medicine in America. Baltimore: Johns Hopkins University Press, 1988:1-28
-
Cleary PD. Chiropractic use: a test of several hypotheses. Am J Public Health 1982;72:727-730
-
McGuire MB. Ritual healing in suburban America. New Brunswick, N.J.: Rutgers University Press, 1988
-
Cook C, Baisden D. Ancillary use of folk medicine by patients in primary care clinics in southwestern West Virginia. South Med J 1986;79:1098-1101
-
Cassileth BR, Lusk EJ, Strouse TB, Bodenheimer BJ. Contemporary unorthodox treatments in cancer medicine. Ann Intern Med 1984;101:105-112
-
U.S. Congress, Office of Technology Assessment. Unconventional cancer treatments. Washington, D.C.: Government Printing Office, 1990 (OTA-H-405)
-
Clinical Oncology Group. New Zealand cancer patients and alternative medicine. N Z Med J 1987;100:110-113
-
Brigden ML. Unorthodox therapy and your cancer patient. Postgrad Med 1987;81:271-280
-
Cassileth BR. The social implications of questionable cancer therapies. Cancer 1989;63:1247-1250
-
Harris and Associates. Health, information and the use of questionable treatments: a study of the American public. Washington, D.C.: Department of Health and Human Services, 1987
-
Cronan TA, Kaplan RM, Posner L, Blumberg E, Kozin F. Prevalence of the use of unconventional remedies for arthritis in a metropolitan community. Arthritis Rheum 1989;32:1604-1607
-
Kronenfeld JJ, Wasner C. The use of unorthodox therapies and marginal practitioners. Soc Sci Med 1982;16:1119-1125
-
Cherkin DC, MacCornack FA. Patient evaluations of low back pain care from family physicians and chiropractors. West J Med 1989;150:351-355
-
Cohen CJ, Eisenberg DM, Mayer KH, Delbanco TL. Prevalence of non-conventional medical treatments in HIV-infected patients: implications for primary care. Clin Res 1990;38:692A-692A.abstract
-
Smart HL, Mayberry JF, Atkinson M. Alternative medicine consultations and remedies in patients with the irritable bowel syndrome. Gut 1986;27:826-828
-
Verhoef MJ, Sutherland LR, Brkich L. Use of alternative medicine by patients attending a gastroenterology clinic. Can Med Assoc J 1990;142:121-125
-
Snyder P. The use of nonprescribed treatments by hemodialysis patients. Cult Med Psychiatry 1983;7:57-76
-
Yager J, Landsverk J, Edelstein CK. Help seeking and satisfaction with care in 641 women with eating disorders. I. Patterns of utilization, attributed change, and perceived efficacy of treatment. J Nerv Ment Dis 1989;177:632-637
-
Gillick MR. Common-sense models of health and disease. N Engl J Med 1985;313:700-703
-
Lepkowski JM. Telephone sampling methods in the United States. In: Groves RM, Biemer PP, Lyberg LE, Massey JT, Nicholls WL II, Waksberg J, eds. Telephone survey methodology. New York: John Wiley, 1988:73-98
-
SUDAAN: professional software for survey data analysis, version 5.3. Research Triangle Park, N.C.: Research Triangle Institute, 1989
-
National health interview survey. Hyattsville, Md.: National Center for Health Statistics, 1989 (electronic data file)
-
Schappert SM. National ambulatory medical care survey: 1990 summary. Advance data from vital and health statistics. No. 213. Hyattsville, Md.: National Center for Health Statistics, 1992. (DHHS publication no. (PHS) 92-1250.)
-
Levit KR, Lazenby HC, Cowan CA, Letsch SW. National health expenditures, 1990. Health Care Financ Rev 1991;13:29-54
-
National Center for Health Statistics. Health and nutrition examination survey II, 1976-1980: medical history ages 12-74 years (ICPSR 8183). 2nd ICPSR ed. Ann Arbor, Mich.: Inter-university Consortium for Political and Social Research, 1984 (electronic data file)
-
Subcommittee on Health and Long-Term Care of the Select Committee on Aging, House of Representatives, Ninety-Eighth Congress, Second Session. Quackery: a $10 billion scandal. Washington, D.C.: Government Printing Office, 1984
-
Kleinman A, Eisenberg L, Good B. Culture, illness, and care: clinical lessons from anthropologic and cross-cultural research. Ann Intern Med 1978;88:251-258
-
Culture, health care systems, and clinical reality. In: Kleinman A. Patients and healers in the context of culture: an exploration of the borderland between anthropology, medicine, and psychiatry. Berkeley: University of California Press, 1980:50-60
Related Letters:
Unconventional Medicine
Amoils S., Korte D., Nelson C. F., Rosner A. L., Friedman R., Zuttermeister P., Benson H., Roter B., Meserole L., Rahlmann J., Santosh S., Stackhouse F. A., Dawson H. R., Stotland N. L., Gellert G. A., Campion T., Eisenberg D., Delbanco T., Kessler R., Campion E. W.
N Engl J Med 1993; 329:1200-1204, Oct 14, 1993.
Correspondence
This article has been cited by other articles:
Ganz, M. L.
(2007). The Lifetime Distribution of the Incremental Societal Costs of Autism. Arch Pediatr Adolesc Med
161: 343-349
Wu, P., Fuller, C., Liu, X., Lee, H.-C., Fan, B., Hoven, C. W., Mandell, D., Wade, C., Kronenberg, F.
(2007). Use of Complementary and Alternative Medicine Among Women With Depression: Results of a National Survey. Psychiatr. Serv.
58: 349-356
Hlubocky, F. J., Ratain, M. J., Wen, M., Daugherty, C. K.
(2007). Complementary and Alternative Medicine Among Advanced Cancer Patients Enrolled on Phase I Trials: A Study of Prognosis, Quality of Life, and Preferences for Decision Making. JCO
25: 548-554
Marinac, J. S., Buchinger, C. L., Godfrey, L. A., Wooten, J. M., Sun, C., Willsie, S. K.
(2007). Herbal Products and Dietary Supplements: A Survey of Use, Attitudes, and Knowledge Among Older Adults. JAOA: Journal of the American Osteopathic Association
107: 13-23
Wahner-Roedler, D. L., Vincent, A., Elkin, P. L., Loehrer, L. L., Cha, S. S., Bauer, B. A.
(2006). Physicians' Attitudes Toward Complementary and Alternative Medicine and Their Knowledge of Specific Therapies: A Survey at an Academic Medical Center. Evid Based Complement Alternat Med
3: 495-501
Carrese, J. A., Sugarman, J.
(2006). The Inescapable Relevance of Bioethics for the Practicing Clinician. Chest
130: 1864-1872
Mukai, H., Watanabe, T., Ando, M., Katsumata, N.
(2006). An Alternative Medicine, Agaricus blazei, May Have Induced Severe Hepatic Dysfunction in Cancer Patients. Jpn J Clin Oncol
36: 808-810
Howell, L., Kochhar, K., Saywell, R. Jr, Zollinger, T., Koehler, J., Mandzuk, C., Sutton, B., Sevilla-Martir, J., Allen, D.
(2006). Use of Herbal Remedies by Hispanic Patients: Do They Inform Their Physician?. J Am Board Fam Med
19: 566-578
Gawarammana, I B, Dargan, P I, Woodcock, S, Sculley, M, House, I M, Wood, D M, Jones, A L
(2006). Should all patients with unexplained anaemia be screened for chronic lead poisoning?. Hum Exp Toxicol
25: 645-649
Davies, A. A., Davey Smith, G., Harbord, R., Bekkering, G. E., Sterne, J. A. C., Beynon, R., Thomas, S.
(2006). Nutritional interventions and outcome in patients with cancer or preinvasive lesions: systematic review.. JNCI J Natl Cancer Inst
98: 961-973
WISNIOSKI, S. W. III
(2006). "Circle turns round" to "allopathic osteopathy".. JAOA: Journal of the American Osteopathic Association
106: 423-424
Kronenberg, F., Cushman, L. F., Wade, C. M., Kalmuss, D., Chao, M. T.
(2006). Race/Ethnicity and Women's Use of Complementary and Alternative Medicine in the United States: Results of a National Survey. Am. J. Public Health
96: 1236-1242
Hanje, A. J., Fortune, B., Song, M., Hill, D., McClain, C.
(2006). The use of selected nutrition supplements and complementary and alternative medicine in liver disease.. Nutr Clin Pract
21: 255-272
Lewith, G., Verhoef, M., Koithan, M., Zick, S. M.
(2006). Developing CAM Research Capacity for Complementary Medicine. Evid Based Complement Alternat Med
3: 283-289
Shmueli, A., Shuval, J.
(2006). Satisfaction with Family Physicians and Specialists and the use of Complementary and Alternative Medicine in Israel. Evid Based Complement Alternat Med
3: 273-278
Stumpf, S. H., Shapiro, S. J.
(2006). Bilateral Integrative Medicine, Obviously. Evid Based Complement Alternat Med
3: 279-282
Winnick, T. A.
(2006). Medical doctors and complementary and alternative medicine: the context of holistic practice.. Health (London)
10: 149-173
Tester, F. J., McNicoll, P.
(2006). 'Why Don't they Get It?' Talk of Medicine as Science. St Luke's Hospital, Panniqtuuq, Baffin Island. Soc Hist Med
19: 87-106
Clay, P. G, Glaros, A. G, Clauson, K. A
(2006). Perceived Efficacy, Indications, and Information Sources for Medically Indigent Patients and Their Healthcare Providers Regarding Dietary Supplements. The Annals of Pharmacotherapy
40: 427-432
WERNEKE, U., TURNER, T., PRIEBE, S.
(2006). Complementary medicines in psychiatry: Review of effectiveness and safety. Br. J. Psychiatry
188: 109-121
Borneman, J. P., Field, R. I.
(2006). Regulation of homeopathic drug products. Am J Health Syst Pharm
63: 86-91
DiGianni, L. M., Rue, M., Emmons, K., Garber, J. E.
(2006). Complementary Medicine Use before and 1 Year Following Genetic Testing for BRCA1/2 Mutations. Cancer Epidemiol. Biomarkers Prev.
15: 70-75
Montalto, C. P., Bhargava, V., Hong, G. S.
(2006). Use of Complementary and Alternative Medicine by Older Adults: An Exploratory Study. Complementary Health Practice Review
11: 27-46
Garrow, D., Egede, L. E.
(2006). Association Between Complementary and Alternative Medicine Use, Preventive Care Practices, and Use of Conventional Medical Services Among Adults With Diabetes. Diabetes Care
29: 15-19
Azaizeh, H., Ljubuncic, P., Portnaya, I., Said, O., Cogan, U., Bomzon, A.
(2005). Fertilization-Induced Changes in Growth Parameters and Antioxidant Activity of Medicinal Plants Used in Traditional Arab Medicine. Evid Based Complement Alternat Med
2: 549-556
Staehle, H.-J., Koch, M.J., Pioch, T.
(2005). Double-blind Study on Materials Testing with Applied Kinesiology. J. Dent. Res.
84: 1066-1069
Menefee, L. A., Monti, D. A.
(2005). Nonpharmacologic and Complementary Approaches to Cancer Pain Management. JAOA: Journal of the American Osteopathic Association
105: S15-S20
Kang, J. X., Liu, J., Wang, J., He, C., Li, F. P.
(2005). The extract of huanglian, a medicinal herb, induces cell growth arrest and apoptosis by upregulation of interferon-{beta} and TNF-{alpha} in human breast cancer cells. Carcinogenesis
26: 1934-1939
Grzywacz, J. G., Lang, W., Suerken, C., Quandt, S. A., Bell, R. A., Arcury, T. A.
(2005). Age, Race, and Ethnicity in the Use of Complementary and Alternative Medicine for Health Self-Management: Evidence from the 2002 National Health Interview Survey. J Aging Health
17: 547-572
Braganza, S. F., Ozuah, P. O.
(2005). Fad Therapies. Pediatr. Rev.
26: 371-376
Ghassemi, J.
(2005). Finding the Evidence in CAM: a Student's Perspective. Evid Based Complement Alternat Med
2: 395-397
Tracy, M. F., Lindquist, R., Savik, K., Watanuki, S., Sendelbach, S., Kreitzer, M. J., Berman, B.
(2005). Use of Complementary and Alternative Therapies: A National Survey of Critical Care Nurses. Am J Crit Care
14: 404-415
Tovey, P., Chatwin, J., Ahmad, S.
(2005). Toward an Understanding of Decision Making on Complementary and Alternative Medicine Use in Poorer Countries: The Case of Cancer Care in Pakistan. Integr Cancer Ther
4: 236-241
Naidu, S., Wilkinson, J. M, Simpson, M. D
(2005). Attitudes of Australian Pharmacists Toward Complementary and Alternative Medicines. The Annals of Pharmacotherapy
39: 1456-1461
Nahin, R. L.
(2005). Identifying and pursuing research priorities at the National Center for Complementary and Alternative Medicine. FASEB J.
19: 1209-1215
Ness, J., Cirillo, D. J., Weir, D. R., Nisly, N. L., Wallace, R. B.
(2005). Use of Complementary Medicine in Older Americans: Results From the Health and Retirement Study. Gerontologist
45: 516-524
Vogel, J. H.K., Bolling, S. F., Costello, R. B., Guarneri, E. M., Krucoff, M. W., Longhurst, J. C., Olshansky, B., Pelletier, K. R., Tracy, C. M., Vogel, R. A., Vogel, R. A., Abrams, J., Anderson, J. L., Bates, E. R., Brodie, B. R., Grines, C. L., Danias, P. G., Gregoratos, G., Hlatky, M. A., Hochman, J. S., Kaul, S., Lichtenberg, R. C., Lindner, J. R., O'Rourke, R. A., Pohost, G. M., Schofield, R. S., Shubrooks, S. J., Tracy, C. M., Winters, W. L. Jr
(2005). Integrating Complementary Medicine Into Cardiovascular Medicine: A Report of the American College of Cardiology Foundation Task Force on Clinical Expert Consensus Documents (Writing Committee to Develop an Expert Consensus Document on Complementary and Integrative Medicine). J Am Coll Cardiol
46: 184-221
Ruggie, M.
(2005). Mainstreaming Complementary Therapies: New Directions In Health Care. Health Aff (Millwood)
24: 980-990
Silva, M. I., Sousa, F. C., Gondim, A. P.
(2005). Herbal Therapy in Primary Health Care in Maracanau, Ceara, Brazil. The Annals of Pharmacotherapy
39: 1336-1341
Cohen, A. J., Menter, A., Hale, L.
(2005). Acupuncture: Role in Comprehensive Cancer Care--A Primer for the Oncologist and Review of the Literature. Integr Cancer Ther
4: 131-143
Tsao, J. C. I., Zeltzer, L. K.
(2005). Complementary and Alternative Medicine Approaches for Pediatric Pain: A Review of the State-of-the-science. Evid Based Complement Alternat Med
2: 149-159
Crisostomo, M. M., Li, P., Tjen-A-Looi, S. C., Longhurst, J. C.
(2005). Nociceptin in rVLM mediates electroacupuncture inhibition of cardiovascular reflex excitatory response in rats. J. Appl. Physiol.
98: 2056-2063
Wang, P. S., Lane, M., Olfson, M., Pincus, H. A., Wells, K. B., Kessler, R. C.
(2005). Twelve-Month Use of Mental Health Services in the United States: Results From the National Comorbidity Survey Replication. Arch Gen Psychiatry
62: 629-640
Woodward, K N
(2005). The potential impact of the use of homeopathic and herbal remedies on monitoring the safety of prescription products. Hum Exp Toxicol
24: 219-233
Lindquist, R., Tracy, M. F., Savik, K., Watanuki, S.
(2005). Regional Use of Complementary and Alternative Therapies by Critical Care Nurses. Crit Care Nurse
25: 63-75
Koenig, K.
(2005). Management of the Depression-Pain Syndrome. J Am Psychiatr Nurses Assoc
11: 81-87
Kiela, P. R., Midura, A. J., Kuscuoglu, N., Jolad, S. D., Solyom, A. M., Besselsen, D. G., Timmermann, B. N., Ghishan, F. K.
(2005). Effects of Boswellia serrata in mouse models of chemically induced colitis. Am. J. Physiol. Gastrointest. Liver Physiol.
288: G798-G808
Smitherman, L. C., Janisse, J., Mathur, A.
(2005). The Use of Folk Remedies Among Children in an Urban Black Community: Remedies for Fever, Colic, and Teething. Pediatrics
115: e297-e304
Kelly, J. P., Kaufman, D. W., Kelley, K., Rosenberg, L., Anderson, T. E., Mitchell, A. A.
(2005). Recent Trends in Use of Herbal and Other Natural Products. Arch Intern Med
165: 281-286
Curtis, P., Gaylord, S.
(2005). Safety Issues in the Interaction of Conventional, Complementary, and Alternative Health Care. Complementary Health Practice Review
10: 3-31
Dy, G. K., Bekele, L., Hanson, L. J., Furth, A., Mandrekar, S., Sloan, J. A., Adjei, A. A.
(2004). Complementary and Alternative Medicine Use by Patients Enrolled Onto Phase I Clinical Trials. JCO
22: 4810-4815
Shim, B.-S., Koh, B.-H., Ahn, K.-S.
(2004). Education in Oriental Medicine in Kyung Hee University. Evid Based Complement Alternat Med
1: 331-334
Yoon, S. L., Horne, C. H., Adams, C.
(2004). Herbal Product Use by African American Older Women. Clin Nurs Res
13: 271-288
Mann, D., Gaylord, S., Norton, S.
(2004). Moving Toward Integrative Care: Rationales, Models, and Steps for Conventional-Care Providers. Complementary Health Practice Review
9: 155-172
Feldman, R. H., Laura, R.
(2004). The Use of Complementary and Alternative Medicine Practices Among Australian University Students. Complementary Health Practice Review
9: 173-179
Daaleman, T. P.
(2004). Religion, Spirituality, and the Practice of Medicine. J Am Board Fam Med
17: 370-376
Wright, L. D.
(2004). Complementary and alternative medicine for hospice and palliative care. AM J HOSP PALLIAT CARE
21: 327-330
Haramati, A., Lumpkin, M. D.
(2004). Complementary and Alternative Medicine: Opportunities for Education and Research. Exp. Biol. Med.
229: 695-697
Suzuki, N.
(2004). Complementary and Alternative Medicine: a Japanese Perspective. Evid Based Complement Alternat Med
1: 113-118
Cushman, M. J., Hoffman, M. J.
(2004). Complementary and Alternative Health Care and the Home Care Population. Home Health Care Management Practice
16: 360-373
LEE, S. S., ZHANG, W., LI, Y.
(2004). The antimicrobial potential of 14 natural herbal dentifrices: Results of an in vitro diffusion method study. Journal of the American Dental Association
135: 1133-1141
Goldstein, M. S.
(2004). The Persistence and Resurgence of Medical Pluralism. Journal of Health Politics, Policy and Law
29: 925-946
Gale, E.A.M.
(2004). The Hawthorne studies--a fable for our times?. QJM
97: 439-449
Yale, S. H., Liu, K.
(2004). Echinacea purpurea Therapy for the Treatment of the Common Cold: A Randomized, Double-blind, Placebo-Controlled Clinical Trial. Arch Intern Med
164: 1237-1241
Gross, D. W., Hamm, J., Ashworth, N. L., Quigley, D.
(2004). Marijuana use and epilepsy: Prevalence in patients of a tertiary care epilepsy center. Neurology
62: 2095-2097
Ernst, E.
(2004). Equivalence and Non-inferiority Trials of CAM. Evid Based Complement Alternat Med
1: 9-10
Block, K. I., Gyllenhaal, C., Mead, M. N.
(2004). Safety and Efficacy of Herbal Sedatives in Cancer Care. Integr Cancer Ther
3: 128-148
McMahan, S., Lutz, R.
(2004). Alternative Therapy Use Among the Young-Old (Ages 65 to 74): An Evaluation of the MIDUS Database. Journal of Applied Gerontology
23: 91-103
Richardson, J.
(2004). What Patients Expect From Complementary Therapy: A Qualitative Study. Am. J. Public Health
94: 1049-1053
Gunnarsdottir, T. J., Peden-McAlpine, C.
(2004). The Experience of Using a Combination of Complementary Therapies: A Journey of Balance Through Self-Healing. J Holist Nurs
22: 116-132
Rhee, S. M., Garg, V. K., Hershey, C. O.
(2004). Use of Complementary and Alternative Medicines by Ambulatory Patients. Arch Intern Med
164: 1004-1009
Barrett, B., Marchand, L., Scheder, J., Appelbaum, D., Plane, M. B., Blustein, J., Maberry, R., Capperino, C.
(2004). What Complementary and Alternative Medicine Practitioners Say About Health and Health Care. Ann Fam Med
2: 253-259
Subcommittee on Management of Acute Otitis Media,
(2004). Diagnosis and Management of Acute Otitis Media. Pediatrics
113: 1451-1465
Joudrey, R., McKay, S., Gough, J.
(2004). Student Nurses' Perceptions of Alternative and Allopathic Medicine. West J Nurs Res
26: 356-366
Peng, C. C., Glassman, P. A., Trilli, L. E., Hayes-Hunter, J., Good, C. B.
(2004). Incidence and Severity of Potential Drug-Dietary Supplement Interactions in Primary Care Patients: An Exploratory Study of 2 Outpatient Practices. Arch Intern Med
164: 630-636
Struthers, R., Eschiti, V. S.
(2004). The Experience of Indigenous Traditional Healing and Cancer. Integr Cancer Ther
3: 13-23
Saxon, D. W., Tunnicliff, G., Brokaw, J. J., Raess, B. U.
(2004). Status of Complementary and Alternative Medicine in the Osteopathic Medical School Curriculum. JAOA: Journal of the American Osteopathic Association
104: 121-126
Rosen, L. D.
(2004). Complementary and Alternative Medicine Use in Children Is Underestimated. Arch Pediatr Adolesc Med
158: 291-291
Kunkel, E. J. S., Meyer, B., Daskalakis, C., Cocroft, J., Jennings-Dozier, K., Myers, R. E.
(2004). Behaviors Used by Men to Protect Themselves against Prostate Cancer. Cancer Epidemiol. Biomarkers Prev.
13: 78-86
Caspi, O., Koithan, M., Criddle, M. W.
(2004). Alternative Medicine or "Alternative" Patients: A Qualitative Study of Patient-Oriented Decision-Making Processes with Respect to Complementary and Alternative Medicine. Med Decis Making
24: 64-79
Edwards, R H T
(2003). Nemesis, Sisyphus, and a contribution from the medical humanities to health research. J. Epidemiol. Community Health
57: 926-927
Correa-Velez, I., Clavarino, A., Barnett, A. G, Eastwood, H.
(2003). Use of complementary and alternative medicine and quality of life: changes at the end of life. Palliat Med
17: 695-703
Sharma, R., Haas, M., Stano, M.
(2003). Patient Attitudes, Insurance, and Other Determinants of Self-Referral to Medical and Chiropractic Physicians. Am. J. Public Health
93: 2111-2117
Chow, E. L., Cherry, J. D., Harrison, R., McDiarmid, S. V., Bhuta, S.
(2003). Reassessing Reye Syndrome. Arch Pediatr Adolesc Med
157: 1241-1242
Alderman, C. P, Kiepfer, B.
(2003). Complementary Medicine Use by Psychiatry Patients of an Australian Hospital. The Annals of Pharmacotherapy
37: 1779-1784
DOMONEY, C. L., VASHISHT, A., STUDD, J. W. W.
(2003). Premenstrual Syndrome and the Use of Alternative Therapies. Ann. N. Y. Acad. Sci.
997: 330-340
Garrard, J., Harms, S., Eberly, L. E., Matiak, A.
(2003). Variations in Product Choices of Frequently Purchased Herbs: Caveat Emptor. Arch Intern Med
163: 2290-2295
Desai, A. K., Grossberg, G. T.
(2003). Herbals and Botanicals in Geriatric Psychiatry. AJGP
11: 498-506
Zuess, J.
(2003). Complementary and Alternative Medicine and Mental Health Care: Shared Challenges. Complementary Health Practice Review
8: 193-197
Marrie, R. A., Hadjimichael, O., Vollmer, T.
(2003). Predictors of alternative medicine use by multiple sclerosis patients. Mult Scler
9: 461-466
Sztajnkrycer, M. D., Otten, E. J., Bond, G. R., Lindsell, C. J., Goetz, R. J.
(2003). Mitigation of Pennyroyal Oil Hepatotoxicity in the Mouse. Acad. Emerg. Med.
10: 1024-1028
Bharucha, D. X, Morling, B. A, Niesenbaum, R. A
(2003). Use and Definition of Herbal Medicines Differ by Ethnicity. The Annals of Pharmacotherapy
37: 1409-1413
Wang, S.-M., Caldwell-Andrews, A. A., Kain, Z. N.
(2003). The Use of Complementary and Alternative Medicines by Surgical Patients: A Follow-Up Survey Study. Anesth. Analg.
97: 1010-1015
Winemiller, M. H., Billow, R. G., Laskowski, E. R., Harmsen, W. S.
(2003). Effect of Magnetic vs Sham-Magnetic Insoles on Plantar Heel Pain: A Randomized Controlled Trial. JAMA
290: 1474-1478
Block, K. I., Mead, M. N.
(2003). Immune System Effects of Echinacea, Ginseng, and Astragalus: A Review. Integr Cancer Ther
2: 247-267
Leong, K P, Pong, L Y, Chan, S P
(2003). Why lupus patients use alternative medicine. Lupus
12: 659-664
Estes, J. D., Stolpman, D., Olyaei, A., Corless, C. L., Ham, J. M., Schwartz, J. M., Orloff, S. L.
(2003). High Prevalence of Potentially Hepatotoxic Herbal Supplement Use in Patients With Fulminant Hepatic Failure. Arch Surg
138: 852-858
Swenson, R., Haldeman, S.
(2003). Spinal Manipulative Therapy for Low Back Pain. J Am Acad Orthop Surg
11: 228-237
Levine, S. M., Weber-Levine, M. L., Mayberry, R. M.
(2003). Complementary and Alternative Medical Practices: Training, Experience, and Attitudes of a Primary Care Medical School Faculty. J Am Board Fam Med
16: 318-326
Idler, E. L., Musick, M. A., Ellison, C. G., George, L. K., Krause, N., Ory, M. G., Pargament, K. I., Powell, L. H., Underwood, L. G., Williams, D. R.
(2003). Measuring Multiple Dimensions of Religion and Spirituality for Health Research: Conceptual Background and Findings from the 1998 General Social Survey. Research on Aging
25: 327-365
|