

How Long-Term Multi-Supplement
Use Affects Blood SugarPrevalence of Elevated HbA1c Among
Multiple Dietary Supplement Users
This section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: American Diabetes Association’s 2017 Conference Presentation ~ FULL TEXT
Paul F. Jacques 1, Gail Rogers 1, Sonhee Park 2,
Francis C. Lau 2, Jamie F. Mcmanus 2, Bruce P. Daggy 2
1 Tufts University,
Boston, MA
2 Shaklee Corporation,
Pleasanton, CA
Why was this study done?
A previous study of 20+ year users of multi-supplements (multi vitamin, fish oil, calcium, vitamin D and more, from Shaklee Corp.) can have a big positive impact on health. This study looked into blood sugar control of people from that original study who now have used multiple supplements for 30+ years, and also evaluated a group who used multiple Shaklee supplements for just 3-5 years.
What This Study Found
The earlier Shaklee study showed a low prevalence (~2.9%) of self-reported diabetes among long-term multiple supplement users (average age, 63 yrs), compared with population norms found in a major government study (NHANES). A decade later, researchers investigated self-reported diabetes diagnosis, diabetes medication use, and HbA1c levels (a measurement of long-term blood sugar control) in those long-term users and a group of 3-5 year multiple supplement users, compared to people in the same government database using no supplements, a multivitamin, a single purpose supplement, or multiple supplements sourced from a wide variety of manufacturers.
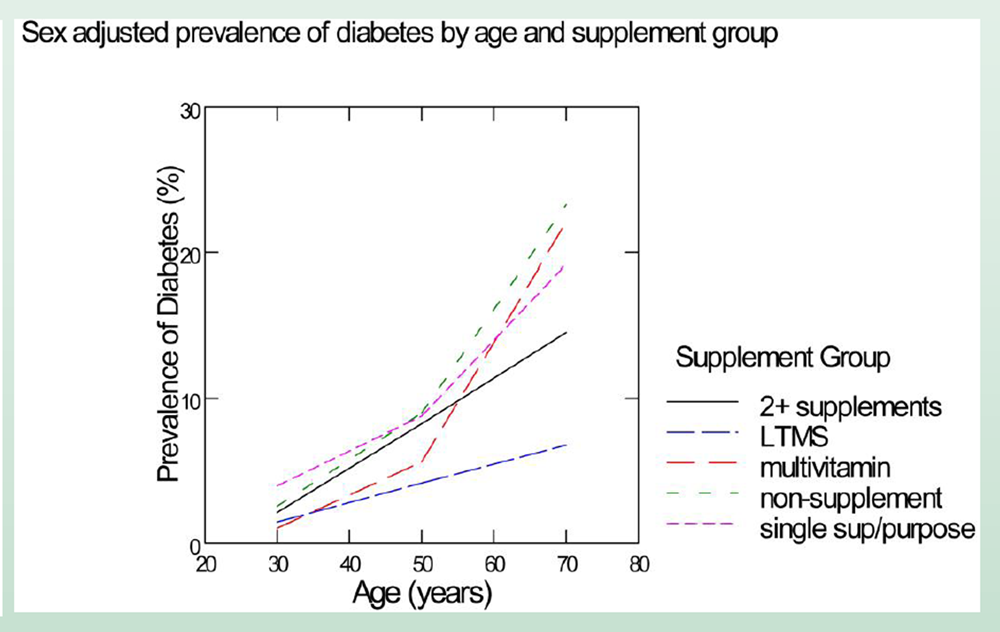
As expected, the prevalence of diabetes (based on self-report, diabetes medication use, or elevated HbA1c) was found to increase with age. After adjusting for age, sex, income, education, and BMI, the study showed that by about age 70, the prevalence of diabetes among non-supplement users, multivitamin users, and single purpose supplement users was about 3-fold higher compared to the long-term users of multiple Shaklee supplements. At the same age, the prevalence of diabetes was about two-fold higher for the users of multiple supplements from other companies, compared with the Shaklee group. Ongoing analyses will seek to further understand these observations.
Approximately 25% of older Americans consume ≥4 dietary supplements/day. (NOTE: ≥ means “more than or equal to”) Block et al. reported an unusually low prevalence of diabetes in a cohort of long-term (≥20 y) users of multiple nutritional supplements. A decade later, we collected medical histories and measured HbA1c in members of the original sample plus an additional sample of the cohort who used multiple supplements for 3-5 years.
Long-term multi-supplement users (LTMS, n = 206, 22-89 y) (NOTE: n = 206 means there was 206 participants) were compared to NHANES 07-10 participants (20-80 y), characterized as non-supplement users (n = 1409), multivitamin only users defined as ≥10 vitamins/minerals (n = 488), users of only one single component supplement (e.g., fish oil) or one single purpose supplement with fewer than 10 vitamins and minerals (e.g., calcium and vitamin D) (n = 300), or users of ≥2 supplement products (n = 1,170).
As the Block study participants were essentially all non-Hispanic white (98.1%) and all non-smokers, we limited the NHANES sample to NHW, non-smoking participants. However, even after this restriction, the LTMS sample showed demographic differences from the NHANES sample including an older age, a higher percentage of women, higher incomes, more college educated, and lower BMI.
The sex & BMI adjusted prevalence of diabetes was lower among members of the long-term multi-supplement users (LTMS) cohort compared to the NHANES sample, with the most striking difference among those aged ≥60 years (6.2% for LTMS cohort vs 17.7% for the NHANES sample). After adjusting for age, sex, income, education and BMI, we observed that the prevalence of diabetes among non-supplement users was almost 2-fold higher (9.2%, 95%CI: 7.6-10.9%) compared to the long-term multi-supplement users (LTMS) users (5.4%, 95%CI: 2.0-8.8%).
Prevalence of diabetes in other supplement user groups was not significantly difference from that of the non-supplement users. Analyses yet to be completed will assess nutritional status and additional metabolic risk factors. A limitation of this study is potential for self-selection of healthier individuals into the LTMS group. However, given the importance of addressing the high incidence of type 2 diabetes and the relative safety of fortified food and supplement use, and the previous observation of improved cardiovascular health [1], further investigations in LTMS users are warranted.
BACKGROUND
A previous study of a cohort of 20+ year users of multiple dietary supplements found, in addition to better nutritional status vs. NHANES controls, improved risk factors and lower prevalence of disease, including diabetes. [1] That study did not include diabetes-related clinical chemistry, or collect information on the use of diabetes medication. We report initial findings with respect to diabetes prevalence from a new study of this cohort, including both participants in the original study and a sample of 3-5 year multiple supplement users.
METHODS
Long term multiple vitamin users (LTMS), 2+ supplements/week, were recruited from a dietary supplement manufacturer and distributor (Shaklee Corp.). Participants from the 2007-2010 NHANES were used for comparison to the LTMS sample. To match the characteristics of the LTMS sample, NHANES subjects were restricted to non-Hispanic white (NHW) adults, 20 + years of age, who did not currently smoke, were not pregnant, and were free of cancer.
LTMS and NHANES data were combined for analysis. To preserve complex sampling design of NHANES, we incorporated the strata & primary sampling unit (PSU) designations for NHANES participants and recalibrated the sample weights as the original sample weight divided by the sum of the sample weights within the supplement category. The LTMS sample was assigned one strata, and each LTMS subject was given a unique PSU and a weight of 1/LTMS sample size. This recalibration allowed for equal weighting for each supplement group and more precise variance estimation but no longer provides estimates that are considered nationally representative. We used SUDAAN statistical software and SAS survey procedures to account for the complex sampling design in the variance estimates.
RESULTS
Table 1. Participant characteristics

Diabetes Prevalence: We separated subjects into 3 age groups (20-39, 40-59, 60+ years), and performed an ANCOVA adjusting for sex & BMI. Least square means and 95% CIs by age group stratified by cohort are presented below.
We used the same methods to provide sex adjusted estimates for each age group by supplement group, graphed as line series. Compared with NHANES, the long-term multi-supplement users (LTMS) group exhibited progressively improved diabetes prevalence with age. (see Fig 1B) Within the NHANES data, the use of two or more supplements also trended towards better outcomes with age (significant interaction with age, p<0.01).
Figure 1. Diabetes prevalence, sorted by by age group and by age and supplement use
Fig. 1A. Incidence by age

Fig. 1B. Incidence by supplement use
DISCUSSION
There is evidence that improved nutritional status (e.g., calcium & D [2]), choice of a low glycemic index meal plan [3], or low levels of nutritionally modifiable markers of inflammation [4, 5] can lower the risk of type 2 diabetes.
In a previous study of the long-term multi-supplement users (LTMS) population, the sample showed improved nutritional status, lower risk factors including C-reactive protein (CRP), and the prevalence of diabetes was only 2.9% at an average age of 63. [1]
We have now repeated this diabetes observation and further supported it with measurement of HbA1c and capture of diabetes medication use. Analyses yet to be completed include measures of nutritional status and risk factors. A limitation of this study is non-random nature of the subject selection. However, given the importance of addressing the high incidence of type 2 diabetes and the relative safety of fortified food & supplement use, further investigations in this population are warranted.
References:
Gladys Block, Christopher D Jensen, Edward P Norkus, Tapashi B Dalvi,
Les G Wong, Jamie F McManus and Mark L Hudes 2007.
Usage Patterns, Health, and Nutritional Status of Long-term
Multiple Dietary Supplement Users
Nutrition Journal 2007 (Oct 24); 6: 30Pittas AG et al. 2007.
The Role of Vitamin D and Calcium in Type 2 Diabetes.
A Systematic Review and Meta-Analysis
J Clin Endocrinol Metab 2007 (Jun); 92 (6): 2017–2029Willett W, Manson J, Liu S. 2002.
Glycemic Index, Glycemic Load, and Risk of Type 2 Diabetes
Am J Clin Nutr 2002 (Jul); 76 (1): 274S–280SHu FB et al. 2004.
Inflammatory Markers and Risk of Developing Type 2 Diabetes in Women
Diabetes 2004 (Mar); 53 (3): 693–700Spranger J et al. 2003.
Inflammatory Cytokines and the Risk to Develop Type 2 Diabetes
Diabetes 2003 (Mar); 52 (3): 812–817
Return to SHAKLEE STUDIES
Since 8–11–2017


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |