

Monograph 13
TMJ Trauma and Its Rehabilitation By R. C. Schafer, DC, PhD, FICC
Manuscript Prepublication Copyright 1997Copied with permission from ACAPress
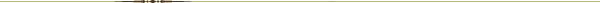
|
Temporomandibular Joint Dysfunction Symptomatology Muscle Strength Range of Motion Applied_Anatomy of the TMJ Joint Neuromuscular Factors TMJ Clinical Management Electives Articular Disrelationship TMJ Subluxation Fixations |
Adjustive and Manipulative Approaches Mild Mobility Restriction (Fixation) Release Mobilization Technics for Moderate Fixations Unilateral TMJ Inferior Subluxation Technic Unilateral TMJ Anterior-Inferior Subluxation Technic Unilateral TMJ Lateral Subluxation Technic Uncomplicated Dislocation Reduction Associated TMJ Joint Strains and Sprains Management Considerations References and Bibliography |
TEMPOROMANDIBULAR JOINT DYSFUNCTION
Proper treatment of TMJ dysfunction must be based on a thorough case history, a complete physical workup, an evaluation of the cranial respiratory impulse and craniosacral mechanisms, and a detailed examination of the TMJ, cranium, and cervical spine. Unfortunately, radiographs to determine abnormal joint space are rarely successful unless over 30% of the bone has been destroyed.
A blow to the jaw is easily transmitted to the temporal bones. As mentioned previously, osteopathic research suggests that a subluxated temporal bone is often the focal fault. This is reported to be grossly indicated by flattening (temporal internal rotation) or protrusion (temporal external rotation) of an ear from the skull.
Symptomatology
The major symptoms of TMJ dysfunction are masticator muscle fatigue and pain, which are usually described as a severe, unilateral (rarely bilateral), dull facial ache that is often fairly localized to an area just anterior to the tragus of the ear. The onset of pain is gradual, progressively increasing over several days or months. It is aggravated by chewing and opening and closing the mouth. Precipitation is often made by eating an apple, a wide yawn, snorkeling, prolonged dental work, playing a wind instrument, prolonged chewing, a bump or pressure on the mandible, sleeping in the prone position, or a cervical whiplash.
Joint clicking, popping, or grinding are often felt and/or heard with or without auscultation. The mandible deviates to one side when opened, tenderness and muscle spasm are present, and a nervous bruxism is usually in the history. There is pain on opening and closing the mouth, or, sometimes, just by moving the head on the neck. An associated referred earache is common, but it should be noted that an ear disorder can sometimes refer pain to the TMJ area.Neurologic and Circulatory Effects. Nine of the 12 cranial nerves are in close relation to the temporal bones from which the mandible is suspended; thus, universal effects may be expressed. There is no doubt that TMJ dysfunction can have far-reaching effects, even to the point of involving peripheral circulation and paresthesias. S. D. Smith reported a case where major improvement in leg circulation directly corresponded to balancing a left TMJ compression through jaw repositioning.
Referred Pain. Within the immediate area of the TMJ are found the chorda tympanum nerve and branches of the superficial temporary artery, vein, and nerve wherein area irritation may cause reflex pain in other areas. While pain is often referred from the TMJ to the scalp, supraorbital area, ear, or neck, the TMJ is rarely a site of referred pain except in cases of a tooth abscess in the mandible or an inflamed upper or lower wisdom tooth impaction.
Differentiation should first be made from angina or cardiac infarction, both of which often refer pain, aching, or throbbing to the angle and base of the mandible. Sinusitis usually refers pain to the frontal area, but sometimes pain is referred to the jaw. Temporal arteritis and glaucoma can also refer pain to the jaw. Referred pain may also be due to dental pathology such as dental caries, pulpitis, impaction, occlusal trauma, periapical abscess, and cementitis. Referred pain from a lower molar is carried by the trigeminal, which also supplies the external pterygoid muscle.
Associated Spasticity. The location of associated muscle spasm in TMJ dysfunction according to incidence is in the external pterygoid, internal pterygoid, masseter, posterior cervical, temporalis, sternomastoideus, trapezius, and mylohyoid. Rhomboid and scalene attachments to the first rib are also commonly tender and hypertonic.
Inspection and Palpation
Active joint motion is observed by having the patient open and close the mouth, observing the movement of the mandible from the front and sides. The rhythm should be smooth, the arc should be continuous and unbroken, and the mandible should open and close in a straight line symmetrically, with the teeth easily separating and joining. An awkward arc, a restricted range of motion, and/or lateral deviation during motion suggest an abnormality.Bony Palpation. During the initial palpation of the TMJs, the examiner sits in front of the patient, places his index fingers in the patient's external auditory canals, and applies pressure anteriorly while the patient opens and closes the mouth. Motion of the mandibular condyles will be felt on the fingertips. This motion is normally smooth and equal on both sides. Next, the lateral aspects of the joints are palpated by placing the first and second fingers just anterior to the patient's tragi. The patient opens and closes the mouth, and any abnormalities are noted. A palpable crepitus suggests traumatic synovial swelling or meniscus damage, and a slight dislocation (painful) may be felt when the patient widely opens the mouth. If there is any doubt of the presence of crepitus, the joint is auscultated for clicks or grating sounds.
Soft-Tissue Palpation. The middle fibers of the temporalis muscles between the eye and the upper ear, the body portion of the masseter muscles, and the external pterygoid muscle are palpated after the patient has opened the mouth. A gloved index finger is pointed posteriorly above the last molar, between the gum and the buccal mucosa, on the mandibular neck. The external pterygoid will normally be felt to tighten and relax as the patient opens and closes the mouth. The patient will report tenderness and pain on palpation if the muscle has been strained or is in spasm. The internal pterygoid muscle is palpated intra- and extra-orally simultaneously. The mylohyoid muscle is palpated beneath the tongue. The examiner may wish to test the jaw and Chvostek's reflexes at this time if they haven't been checked previously. The posterior cervical, sternocleidomastoideus, and trapezius muscles are palpated for hypertonicity and tenderness.
Relationship to Cervical Motion. During examination, the patient is asked to slowly tap their teeth together. The bite is evaluated. Next, the relationship with cervical motion is screened. The mandible normally moves backward during cervical extension and forward in cervical flexion, producing poor occlusion during extreme flexion-extension. Thus, a patient with a cervical spine in a chronic state of fixed flexion or extension in the resting position will exhibit a constant state of malocclusion, which will lead to TMJ dysfunction.
Muscle Strength
Muscle strength is tested by placing one hand on the patient's occiput to steady the patient and the other hand, palm up, under the patient's jaw. The patient is asked to open the mouth while the examiner applies resistance with his palm. The patient should normally be able to open his mouth against the increasing resistance of the examiner's palm. When the patient is unable to close his mouth actively, an attempt should be made to can close it passively.
Range of Motion
The adult range of mandibular motion is usually normal if (1) the examiner is able to insert three finger widths between the incisor teeth when the mouth is opened; (2) the patient is able to jut the jaw forward and place the lower teeth in front of the upper teeth. If deemed necessary, an accurate measurement of the interincisal opening can be made using a Boley gauge.
Restricted joint motion can be the result of muscle spasm, rheumatoid arthritis, osteoarthritis, joint ankylosis, scar tissue, trismus from spasm of the elevating muscles of mastication from hysteria, tetanus, congenital defect, or most any type of local inflammation. If a patient with a subnormal range of mandibular motion can suddenly open the mouth wider after the TMJ area has been sprayed with a vapocoolant, muscle hypertonicity should be suspected as an important ingredient in the syndrome.
APPLIED ANATOMY OF THE TMJ JOINT
Anatomy of the TMJ | |
|---|---|
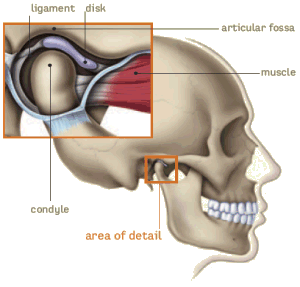 |
The TMJ is a hinge and gliding joint and is the most constantly used joint in the body. The round upper end of the lower jaw, or the movable portion of the joint, is called the condyle; the socket is called the articular fossa. Between the condyle and the fossa is a disk made of cartilage that acts as a cushion to absorb stress and allows the condyle to move easily when the mouth opens and closes. |
Function of the TMJ |
|---|
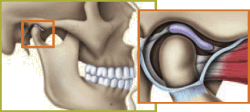 |
Temporomandibular joint — Normal closed position. Jawbone is separated from skull by a soft disk that acts as a cushion when you chew, speak or swallow. |
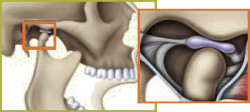 |
Temporomandibular joint — Normal open position. Disk stays in place when jaw is in use. |
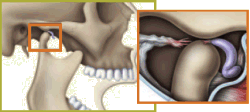 |
Temporomandibular joint — Abnormal. Disk is pulled forward when jaw is in use, causing the bone structures to grind together. |
The TMJ is the most active joint of the body, moving up to 2,000 times each day during talking, chewing, swallowing, yawning, and snoring. However, it has only been within the last decade or so that wide recognition of the clinical importance of TMJ dysfunction on the cervical spine and body as a whole has been achieved.
Like other synovial joints, the TMJ is lined with articular cartilage, possesses an internal meniscus, and has a synovial membrane. Because of the structural approximation and neuromuscular relationship of the TMJ area and the occipitoatlantal area, disorders of the TMJ can be referred biomechanically and neurologically to the upper cervical spine in particular. The reverse can be true in situations of upper-cervical fixation/subluxation syndromes. TMJ meniscus malposition frequently produces neck pain, suboccipital muscle spasms, and headaches.
The TMJ articulation hinges within the glenoid fossa of the mandible and glides anteriorly to the eminentia during normal motion. The articular space contains a small amount of viscous fluid for lubrication. The head of the condyle and the glenoid fossa are covered with fibroid cartilage that serves as a shock absorber. This cartilage tends to wear thin when subjected to prolonged overstress because it contains no direct blood supply that could assist in tissue regeneration. The blood supply to the TMJ is from the superficial temporal branch of the external carotid artery; the disc itself, however, is avascular.
The meniscus of the joint divides the joint cavity into two divisions. The lower part of the joint cavity is used during gliding motion, and the upper part is used for hinge movements. This is accomplished primarily by one head of the external pterygoid muscle pulling the meniscus forward while the second head opens the joint. Secondary assistance is provided by the mylohyoid, geniohyoid, and digastric muscles, and gravity is helpful in lowering the mandible during the upright position. Thus, the two heads of the pterygoid muscle, essentially, act asynchronously to open the TMJ. In closing the jaw (approximating the mandible and maxillae), the temporal, masseter, and internal pterygoid muscles are activated. All muscles active during TMJ function assist in maintaining the mandible in its resting position.
Neuromuscular Factors
The external pterygoid muscle, the prime opener of the mouth, is supplied by the pterygoid branch of the mandibular division of the trigeminal nerve. Secondary force in opening is provided by the hyoid muscles and gravity when upright. The masseter and temporalis muscles, both supplied by the trigeminal nerve, are the primary closers of the jaw, with secondary effort provided by the internal pterygoid muscle. The capsule and structures of the TMJ are innervated by branches of the articular temporal nerve, filaments of the masseter nerve, and a sensory branch from the 7th cranial.
TMJ nerves are not vulnerable to direct compression by the condyle, but the joint's proprioceptive bed is abundant with nerve endings. Thus, strain or subluxation, unilaterally or bilaterally, may not only cause symptoms within the joint and associated soft tissues but also by reflex action mirror distorting effects within the musculature innervated by the gray cell motor columns of the C1 C4 neuromeres. Reflex aberrant stimulation transmitted downward via the tractus spinalis of the 5th cranial nerve, with attending atlanto-occipital jamming and atlantoaxial and/or C3 rotational subluxation, may result in suboccipital and cervical migraine (occipitofrontal neuralgia) caused by asymmetrical spasm of the suboccipital muscles and the upper extensions of the cervical multifidii.
TMJ CLINICAL MANAGEMENT ELECTIVES
1. Stage of Acute Inflammation and Active Congestion
The major goals are to control pain and reduce swelling by vasoconstriction, compression, and elevation; to prevent further irritation, inflammation, and secondary infection by disinfection, protection, and rest; and to enhance healing mechanisms. Common electives include:
Cryotherapy
Cold packs
Ice massage
Vapocoolant spray
Compression
Pressure bandage
Protection (padding)
Indirect therapy (reflex therapy)
Pulsed alternating current
Iontophoresis/phonophoresis
Auriculotherapy
Meridian therapy
Spondylotherapy (upper thoracic)
Rest (chin strap, liquid diet)
Nutritional supplementation to enhance connective tissue integrity.
2. Stage of Passive Congestion
The major goals are to control residual pain and swelling, provide rest and protection, prevent stasis, disperse coagulates and gels, enhance circulation and drainage, maintain muscle tone, and discourage adhesion formation. Common electives include:
Indirect articular therapy (reflex therapy)
Alternating superficial heat and cold
Pressure bandage
Light nonpercussion vibrotherapy
Mild surging alternating current
Mild pulsed ultrasound
Cryokinetics (passive exercise)
Meridian therapy
Spondylotherapy (upper thoracic)
Rest (chin strap, soft diet)
Nutritional supplementation to enhance connective tissue integrity.
3. Stage of Consolidation and/or Formation of Fibrinous Coagulant
The major goals are the same as in Stage 2 plus enhancing muscle tone and involved tissue integrity and stimulating healing processes. Common electives include:
Mild articular adjustment technics, especially occipitocervical
Moist superficial heat
Thermowraps
Spray-and-stretch
Cryokinetics (active exercise)
Moderate active range-of-motion exercises
Meridian therapy
Alternating traction
Sinusoidal current
Ultrasound
Microwave
Vibromassage
High-volt therapy
Interferential current
Spondylotherapy
Mild transverse friction massage
Mild proprioceptive neuromuscular facilitation techniques
Rest
Diet modification
Nutritional supplementation to enhance connective tissue integrity.
4. Stage of Fibroblastic Activity and Potential Fibrosis
At this stage, causes for pain should be corrected but some local tenderness likely exists. The major goals are to defeat any tendency for the formation of adhesions, taut scar tissue, and area fibrosis and to prevent atrophy. Common electives are:
Deep heat
Articular adjustment technics, especially occipitocervical
Spondylotherapy (upper thoracic)
Local vigorous vibromassage
Transverse friction massage
Spray-and-stretch
Mild active range-of-motion exercises
Negative galvanism
Ultrasound, continuous
Sinusoidal and pulsed muscle stimulation
Microwave
High-volt therapy
Interferential current
Meridian therapy
Proprioceptive neuromuscular facilitation techniques
Nutritional supplementation to enhance connective tissue integrity.
5. Stage of Reconditioning
Direct articular therapy for chronic fixations
Progressive remedial exercise may be helpful, but it should be noted
that the TMJ is normally the most exercised joint in the body.
Nutritional supplementation to enhance connective tissue integrity.
Articular Disrelationship
If patient symptoms to not fade after a logical trial of chiropractic treatment, consultation with a dentist experienced in the care of TMJ syndromes should be made. Intraprofessional cooperation is frequently necessary for efficient patient care.
Mechanically, two major forms of TMJ malposition occur. They arise from either partial displacement or complete dislocation of the articular disc and occur in 10% 12% of the population. In partial anterior displacements, condyle translation is not blocked. That is, when the patient moves the closed jaw forward and/or toward the contralateral side, the condyle will snap forward (opening click) into its normal position so that the mouth can be fully opened. However, Farrar/McCarty state that when the jaw is retruded, the disc will displace with a snap (reciprocal click).
In complete dislocation, the disc is usually dislodged anteriorly toward the front of the condyle so its translation is restricted when the mouth is opened. This increases the joint space. Persistent condyle motion on a dislocated disc encourages irregular adaptive remodeling and osteoarthritis to develop within the joint because the dislocated disc can no longer cushion the articular surfaces. Crepitus arises if bone-on-bone articulation occurs. In time, the collateral ligaments may perforate or tear and be drawn into the articular space and osteoarthritis will develop.
Several papers by osteopaths have proposed that TMJ dysfunction is essentially caused by stress factors that distort position of the temporal bone. For example, Magoun found that the temporal bone usually rotates externally-internally on an axis that extends from the petrous apex to the jugular surface, depending on the stress pattern present.
The temporomandibular fossa moves posteromedially during temporal external rotation (temporal protrusion) and anterolaterally during temporal internal rotation (temporal flattening), with the position of the mandible moving to correspond to the positions of the temporomandibular fossae. Thus, the mandible protrudes if both temporals are fixed in external rotation, and retrudes if both temporals are fixed in internal rotation. Hruby reports that it is more common to find one temporal bone in internal rotation and one in external rotation, thus producing mandibular misalignment.
TMJ Subluxation Fixations
As with most subluxation complexes, the TMJ entity may be a cause or an effect. If primary, its effects may express itself through the whole functional-structural complex of the body. If secondary, its cause may be found as remote as the feet.
Lay explains that the actions of muscles, ligaments, and fasciae throughout the body, from head to foot, coordinate it as a functioning unit. Thus, a functional or anatomical short leg, sacroiliac fixation, lumbar subluxation complex, rib-cage distortion (especially with scalene shortening), thoracic or cervical subluxations, or occipital malalignment may be a cause or contributor to or an effect of TMJ dysfunction.
Teeth grinding, jaw clenching, and the jaw tension associated with anxiety or depression may be important psychologic or somatopsychic considerations. The major features of TMJ dysfunction are shown in Table 1.
Table 1. Major Signs and Symptoms of TMJ Dysfunction
Local Effects Remote Effects Mandible deviates to one side when opened Tenderness of posterior cervical muscles, usually unilateral Joint click (palpable and/or audible) in displacement but not in dislocation Pain radiates from TMJ area superiorly to temporoparietal region and/or inferiorly into the neck Severe, unilateral, dull facial pain, aggravated by chewing, opening and closing the mouth
Crepitus of involved joint (sometimes)Muscle spasm: Posterior cervicals
Sternocleidomastoideus
Trapezius
Mylohyoid
ScalenesTenderness at proximal mandible, usually unilateral Earache Muscle spasm: Pterygoids (internal and external) Bruxism
Masseter
Temporalis
MalocclusionPostural distortion (anywhere from the occiput to the internal pterygoids
Rib cage, spinal, and lower extremity sites of fixation and trigger points
Peripheral circulation disorders
Atypical facial neuralgia Migraine
ADJUSTIVE AND MANIPULATIVE APPROACHES
Dear Reader(s),
This article is provided for doctors as reference material, with the expectation that they are already skilled in assessment / diagnosis, in palpation, manipulative skills and in critical thinking.
It is certainly NOT intended for ANY person to use for self-diagnosis or self-treatment purposes. The biomedical literature is filled with reports of self-manipulation gone wrong. If you have a TMJ problem, seek competent care from a licensed health care provider, with a specialty knowledge level, and a strong track record in successful TMJ management.
If a site of soft-tissue hypertension is found in one or both TMJs, gentle but firm passive pressure against resistance until the tissues release is usually all that is necessary. This will be indicated when free mobility is restored. The same technique can be applied if abnormal tension is found in sphenomandibular and stylomandibular area soft tissues, as determined by exerting pressure on the angle of the mandible caudally and then cephally, and comparing the resistance found bilaterally.
When TMJ compression is a factor, and it often is, physical correction can be aided by the doctor inserting gloved thumbs against the patient's lower molars, with the fingers wrapped around the jaw, and applying pressure to bring the mandible down and forward and then down and backward several times to open the joint space.
Invariably, motion palpation of the pubic and/or sacroiliac joints will reveal a fixation when TMJ dysfunction is present. When this is found, the fixation should be mobilized unless contraindications for adjustive therapy are found.
Mild Mobility Restriction (Fixation) Release
The basic condyle motions of the TMJ essentially include rotation with and without a lateral shift; rotation with backward, upward, and lateral motion; and rotation with forward, downward, and lateral motion. Functional restriction may be the common result of muscle hypertonicity or ligamentous shortening.Passive Stretching. When jaw opening is restricted, sustained passive stretching can be administered by most any type of padded appliance (eg, a surgical mouth prop with a spring or ratchet). Slowly inserting layers of tongue blades or a tapered cork (15 30 mm) between the molars are sometimes substituted during home treatments. Regardless of what appliance is used, this technique is best conducted with the patient in the relaxed nonweight-bearing supine position at first and then in the sitting position as improvement is achieved. Special care must be used to avoid too vigorous application. Preadjustment moist heat application to the involved TMJ(s) and cervical spine for 15 to 20 minutes is beneficial.
Active Stretching. The supine patient slowly and progressively opens his mouth to a larger and larger degree but not to the degree of pain. During this exercise, the patient is asked to place the tongue against the hard palate as this will keep the motions essentially rotary and minimize protrusion. After the initial warm-up, the patient holds the full-open position for several seconds and follows this with complete jaw relaxation for several seconds in a hold-relax fashion. Kessler/Hertling state that ultrasound may be beneficial during this exercise.
Reflex Relaxation. This is done by applying slow reducing resistance as the patient attempts to open the closed mouth. After several seconds of relaxation, active jaw motion (stretching) without resistance should be conducted for several seconds. A reverse technique is then used by applying slow reducing resistance as the patient attempts to close the opened mouth. These action-rest procedures should be repeated several times until function improves.
Mobilization Technics for Moderate FixationsCaudal Traction. The patient is placed in a relaxed full-supine or semi-supine position and the doctor stands to the side of the involved joint facing the patient. The doctor's cephalad stabilizing hand is placed against the patient's forehead and scalp, and the thumbpad of his caudad hand is placed against the patient's rear molars with the doctor's fingers cupping the patient's chin. Traction is applied caudad and the patient is asked to swallow. Pressure is held several seconds, and then a similar period for relaxation is allowed.
Mobilizing Restricted Anterior Glide. After caudal traction is administered several times, anterior glide (protraction) and posterior glide (retraction) is included in the procedure. This is best accomplished by standing on the opposite side and grasping the angle of the mandible externally with the active hand's 1st and 2nd fingers with the thumb wrapped around the chin. Sustained anterior traction is applied, and the patient is asked to swallow. After a period of relaxation and holding the same contact, sustained posterior pressure is applied and the patient is again asked to swallow. These action-rest modes are done several times until function of anterior glide improves.
Mobilizing Restricted Medial-Lateral Glide. The doctor stands behind the relaxed supine patient and cups his active hand around the patient's chin, while supporting the patient's head with the stabilizing hand. With his active hand, the doctor slowly applies lateral traction, holding it for several seconds. The patient is then asked to swallow and then allow several seconds for relaxation. The procedure is then reversed by applying medial pressure, holding it for several seconds, asking the patient to swallow, and then allowing several seconds for relaxation. These procedures are repeated several times until function of medial-lateral glide improves.
Note: Lateral mandibular movements are the most restricted jaw motions in bilateral TMJ capsule restrictions (eg, contractures, spasm, adhesions). Contralateral anterior-posterior gliding movements are the most restricted jaw motions in unilateral capsule restrictions, and the mandible will deviate toward the restricted side when the mouth is opened widely.
Unilateral TMJ Inferior Subluxation Technic
A TMJ may become abnormally separated and fixed in a straight inferior position with the contralateral side normal. Before correction, the patient is placed in the sitting position facing forward. The doctor stands behind the patient, slightly to the side of the lesion. If the lesion is of the patient's left TMJ, contact is made on the medial aspect of the mandible under the angle with the fingertips of the doctor's left hand. His right stabilizing hand should be cupped under the patient's right mandibular ramus. The patient is asked to stabilize the back of his head against the doctor's chest. The adjustment is made by asking the patient to force the mouth open while the doctor applies pressure directed from the inferior to the superior.
Unilateral TMJ Anterior-Inferior Subluxation Technic
A fixated anterior-inferior misalignment of the TMJ may be found on one side with the other side normal. To correct this subluxation, the patient is placed in the sitting position facing forward. The doctor stands behind the patient and cups the patient's chin within clasped fingers. The patient is asked to stabilize the occiput against the doctor's chest. The adjustment is made from the anterior-inferior to the posterior-superior. The thrust should be short, rapid, well controlled, and in accord with normalizing the anatomical disrelationship.Associated Medial Malposition. There may also be a degree of associated medial misalignment. If this occurs, the line of correction should be diagonal toward the patient's eye on the side of misalignment rather than directly posterior-superior (ie, posterior-superior-lateral). This will requires the doctor to slightly rotate his shoulder anteriorly on the side contralateral to the lesion.
Unilateral TMJ Lateral Subluxation Technic
A TMJ joint may articulate in an abnormal lateral position. This misalignment is usually accompanied by some degree of superior jamming. Before correction, the patient is placed in the sitting position facing forward. The doctor stands behind the patient, slightly to the side of the lesion. If the lesion is of the patient's right TMJ, the doctor places his right palm on the right side of the TMJ so his thenar eminence is directly over the head of the affected condyle and the ramus of the mandible above the angle. The doctor's left stabilizing hand is placed in a like position on the patient's left mandible. The doctor leans slightly forward so his head is over the patient's head. In this position, his elbows will be bent and his wrists extended. The adjustment is made from the superior-lateral to the inferior-medial against the doctor's stabilizing hand.
Uncomplicated Dislocation Reduction
Mandibular dislocation is invariably anterior displacement of the mandibular condyle from its temporal articulation into the infratemporal fossa anterior to the articular eminences. It may involve either or both joints. The chin is displaced toward the uninjured side in unilateral dislocation and displaced forward in bilateral dislocation. The patient presents with anxiety, helplessness, aching and spastic temporal and masseter muscles, and the classic "mouth-agape." The mouth cannot be closed. Dislocation is often caused by a blow to a lax joint or simply by a wide yawn, laughing, or eating an apple.
During reduction of uncomplicated luxation confirmed by x-ray, the patient should be placed supine. The doctor's thumbpads are firmed against the last molars, with his remaining fingers extended around the patient's jaw. A diagonal inferior-posteriorly thrust is made against the molars with the thumbs while the doctor's fingers tilt (lift) the mandible superior-anteriorly upward with a rotatory motion. The downward pressure is to overcome the associated muscle spasm, and the rotation of the chin upward is to reposition the condyle(s) posteriorly to the articular eminences. If only one side is involved, only one contact thumb is used within the mouth. The doctor's other hand is applied against the patient's forehead for counterpressure. After successful reduction, the chin is mildly mobilized for several seconds, a cold pack is applied, and chin support is provided for 1 to 3 days.
Prior to reduction, special care must be taken to adequately pad the thumbs before placing them firmly on the molar and premolar surfaces. This is for the doctor's protection not the patient's benefit. Thumb padding is essential during this leverage maneuver because reduction is usually followed immediately by an involuntary contraction of the masseter and temporal muscles in unison, causing the jaws to clamp shut sharply.
ASSOCIATED TMJ JOINT STRAINS AND SPRAINSPoor occlusion leads to a chronic strain or sprain as does bruxism (teeth grinding). Bruxism is commonly increased in anxiety states, thus TMJ dysfunction is often related to various psychoneuroses.
Strains. The major muscles to be considered are the medial and lateral pterygoid, masseter, and temporalis. Strain of the suprahyoid muscles (digastric, stylohyoid, mylohyoid, and geniohyoid) and infrahyoid muscles (thyrohyoid, omohyoid, and sternohyoid) should also be considered as contributing factors. Overworked and overstretched temporalis and pterygoid muscles can become chronically spastic and produce localized pain at muscle attachments or refer pain and/or paresthesias to one or both ears, the face, the temples, or the forehead.
Overstretch causes an asymmetrical lateral motion of the jaw and malocclusion. There is usually joint clicking and transient locking, and, if not properly treated, a subluxation-fixation may result. Such strains are sometimes seen after activities where the teeth must be tightly clenched for a prolonged period (eg, underwater swimmers who clench their teeth tightly on a mouthpiece).
Sprains. The straps to be considered are the articular capsule and the lateral (temporomandibular), sphenomandibular, and stylomandibular ligaments. TMJ sprain is usually the result of malocclusion, acute or chronic subluxation, or spontaneously reduced dislocation from trauma (eg, whiplash, eating an apple, traction). Related muscle strain and spasm, tissue ruptures, and soft-tissue swelling may be involved depending on the extent of injury.
MANAGEMENT CONSIDERATIONSThe correction of structural disrelationships and fixations by chiropractic techniques coupled with referral for appropriate orthodontic and prosthodontic appliances (which are often necessary), provides the most practical approach to the treatment of TMJ function. According to several observations, the therapeutic approach is recommended to be structurally holistic because TMJ dysfunction can affect any part or the whole of the skeleton or vice versa. In other words, sites of fixation should be sought in the feet, ankles, knees, hips, pubes, sacroiliacs, spine, rib cage, and skull, and mobilized if found. Obviously, if muscle groups are weak, spastic, or shortened, therapy should be applied to restore their normal state.
Trigger Points and Spasm: Vapocoolant Technique. Many trigger points have been isolated that frequently refer pain and deep tenderness to the TMJ. The most common points are within the masseter, temporalis, and internal and external pterygoid muscles. Before correcting isolated subluxations, it is helpful to spray the located trigger areas with a vapocoolant. The patient's mouth is comfortably propped open with a roll of gauze, his eyes and nose are draped, and his neck is laterally flexed away from the involved side. A few slow, even, interrupted sweeps of the spray in one direction only from jaw angle to temple should reduce any spasm and referred pain present. The skin should not be frosted. Two or three applications a few days apart are usually sufficient. High-voltage galvanic current over spastic masseter or temporal muscles for 15 minutes is an alternative approach.
Adjunctive Procedures. Just about any therapy whose objective is to reduce pain and spasm is indicated. During the acute stage for example, cryotherapy, acupuncture, trigger-point therapy, and high-volt or interferential therapy or microcurrents are frequently recommended. After the acute stage, the common modalities used include moist heat over spastic areas, TENS, and ultrasound. Biofeedback has been reported effective in some stubborn cases. Nutritional muscle relaxants and anti-inflammatory agents are frequently recommended when pain and swelling are major factors.
Diet. During the acute stage, the diet should restrict difficult-to-chew foods (eg, steak, nuts, raw vegetables) or those that require wide opening of the mouth (eg, thick sandwiches, apples) to avoid masticatory overstretch and articular displacement.
Habits. The patient should be alerted to relax the jaw whenever muscle tension, jaw clenching, or teeth grinding are noticed. "Lips together, teeth apart" is the normal position of relaxation. Pipe smoking and sleeping on the stomach should be discontinued. Sleeping with an orthopedic pillow to maintain good cervical posture is often beneficial.
Remedial Exercises. Exercise against resistance is often helpful to relax cramped muscles and strengthen antagonists. The patient should be taught to slowly open the mouth as wide as possible without discomfort several times and continued this exercise until, in time, the knuckles of the index and middle finger can be easily inserted between the front teeth. This exercise should be followed by holding the chin between the index finger and thumb and resisting opening and closing the mouth. Next, resisted lateral movements of the jaw against the palm of the hand should be made, first on one side and then the other. Each exercise should be conducted about 10 times in 3-5 bouts daily.
REFERENCES AND BIBLIOGRAPHY:Berkman EH: The Troublesome TMJ. ACA Journal of Chiropractic, June 1971.
Common Sense Management for TMJ Troubles. Patient Care, pp 129-157, January 15, 1984.
"Doctor, My Jaw Hurts." Patient Care, pp 108-136, December 15, 1983.
Farrar WB, McCarty WL Jr: A Clinical Outline of Temporomandibular Joint Diagnosis and Treatment. Montgomery, AL, Normandie Publications, 1982.
Farrar WB: Dysfunctional Centric Relation of the Jaw Associated with Dislocation and Displacement of the Disc. Compendium of the American Equilibrium Society, 13:63-67, 1973-1974.
Gelb H (ed): Clinical Management of Head, Neck and TMJ Pain and Dysfunction. Philadelphia, W.B. Saunders, 1977.
Hruby RJ: The Total Body Approach to the Osteopathic Management of Temporomandibular Joint Dysfunction. Journal of the American Osteopathic Association, 85(8):502-509.
Kessler RM, Hertling D (eds): Management of Common Musculoskeletal Disorders. Philadelphia, Harper & Row, 1983, pp 233-271, 533-537.
Larsen NJ: Osteopathic Manipulative Contribution to Treatment of TMJ Syndrome. Osteopathic Medicine, 3:15-27, August 1976.
Lay EM: The Osteopathic Management of Temporomandibular Joint Dysfunction. In Gelb H (ed): Clinical Management of Head, Neck and TMJ Pain and Dysfunction. Philadelphia, W.B. Saunders, 1977.
Magoun HI Sr: Dental Equilibrium and Osteopathy. Journal of the American Osteopathic Association, 75:981-991, June 1975.
Mahan PE: Temporomandibular Joint Dysfunction: Physiological and Clinical Aspects. In Rowe NH (ed): Occlusion: Research in Form and Function. Proceedings of Symposium. East Lansing, MI, University of Michigan, 1975, p 112.
Royder JO: Structural Influences in Temporomandibular Joint Pain and Dysfunction. Journal of the American Osteopathic Association, 80:460-467, March 1981.
Schafer RC: Chiropractic Management of Extraspinal Articular Disorders. Arlington, Virginia, American Chiropractic Association, 1989.
Schafer RC: Chiropractic Management of Sports and Recreational Injuries, ed 2. Baltimore, Williams & Wilkins, 1986.
Schafer RC: Chiropractic Physical and Spinal Diagnosis. Oklahoma City, Associated Chiropractic Academic Press, 1980.
Schafer RC (ed): Basic Chiropractic Procedural Manual, ed 4. Des Moines, Iowa, Ameri?can Chiropractic Association, 1980.
Schafer RC: Clinical Biomechanics: Musculoskeletal Actions and Reactions, ed 2. Baltimore, Williams & Wilkins.
Schafer RC: Physical Diagnosis. Arlington, Virginia, American Chiropractic Association, 1988.
Shapiro BL: Changing Views About Temporomandibular Pain-Dysfunction. Northwest Dentistry, 60:6, 1981.
Shore NA: Occlusal Equilibration and Temporomandibular Joint Dysfunction. Philadelphia, J.B. Lippincott, 1976.
Smith SD: Vascular Analysis in Temporomandibular Orthopedics: Quantifying Blood Flow Related to Occlusal Dynamics. Osteopathic Medicine, pp 29-32, 35-41, 71, October 1980.

Return to CHIROPRACTIC & TMJ
Return to R. C. SCHAFER MONOGRAPHS


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |