

Patient Expectations of Benefit from Common Interventions for
Low Back Pain and Effects on Outcome: Secondary Analysis
of a Clinical Trial of Manual Therapy InterventionsThis section is compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




FROM: J Man Manip Ther. 2011 (Feb); 19 (1): 20–25 ~ FULL TEXT
OPEN ACCESS Mark D Bishop, Joel E Bialosky & Josh A Cleland
Department of Physical Therapy,
University of Florida, USA.
OBJECTIVES: The purpose of this secondary analysis was 1) to examine patient expectations related to a variety of common interventions for low back pain (LBP) and 2) to determine the influence that specific expectations about spinal manipulation might have had on self-report of disability.
METHODS: We collected patients' expectations about the benefit of specific interventions for low back pain. We also collected patients' general expectations about treatment and tested the relationships among the expectation of benefit from an intervention, receiving that intervention and disability-related outcomes.
RESULTS: Patients expected exercise and manual therapy interventions to provide more benefit than surgery and medication. There was a statistical association between expecting relief from thrust techniques and receiving thrust techniques, related to meeting the general expectation for treatment (chi-square: 15.5, P = 0.008). This was not the case for patients who expected relief from thrust techniques but did not receive it (chi-square: 6.9, P = 0.4). Logistic regression modeling was used to predict change in disability at treatment visit 5. When controlling for whether the general expectations for treatment were met, intervention assignment and the interaction between intervention assignment and expectations regarding thrust techniques, the parsimonious model only included intervention as the significant contributor to the model (P < 0.001). The adjusted odds ratio of success comparing thrust techniques to non-thrust in this study was 41.2 (11.0, 201.7).
DISCUSSION: The findings of this secondary analysis indicate that patients seeking intervention for LBP expect active interventions and manual therapy to significantly help improve their pain more than interventions like traction, rest, surgery, or medication. Additionally, in patients who meet the clinical prediction rule for good prognosis when managed with thrust techniques, treating with thrust techniques is more important than matching treatment to patient expectation.
KEYWORDS: Expectations; Low back pain; Spinal manipulation
From the FULL TEXT Article:
Introduction
Patient expectations, in the healthcare setting, are a set of beliefs regarding treatment and clinical outcomes associated with that treatment. These beliefs include what the patient wants to happen during treatment (ideal expectation), what the patient believes is going to occur (predicted expectation), and what the patient thinks should occur (normative expectation). [1] Patient expectations are influenced by a range of individual demographics (sex, [2–4] education level, [2, 4] age, [2, 3] and race [3]) and psychological (fear [5] and depression [4, 5]) factors, as well as prior experiences of the patient.
A recent systemic review of patient expectations indicates that these expectations are related to a wide variety of different outcomes ranging from medication use to distance walked after surgery for conditions ranging from alcoholism to musculoskeletal pain conditions. [6] In patients with low back pain (LBP), associations between expectations and functional outcome have been shown in several studies. [7, 8]
For example, Myers et al. tested whether expectations for recovery from acute LBP measured at the initial evaluation were related to self-report of disability in patients participating in a trial comparing usual medical care to a combination of usual care and complementary and alternative medicine interventions (chiropractic, acupuncture, or massage). In that study, the general expectation for improvement was associated with improvements in self-report of disability at 5 and 12 weeks after beginning treatment. [8]
In a different trial of interventions for LBP, participants with higher expectations for the treatment they received had greater improvements in reported function, that is, improvement was dependent on whether the patient expected the treatment to help regardless of which treatment the patient received. [7]
This evidence suggests that incorporation of patient expectations into an evidence-based plan of care can potentially improve the outcomes related to that care. Recent work in manual therapy research has examined factors that are associated with favorable prognosis for patients managed with manual therapy. [9–13] However, despite the potential influence of expectation, these have not been routinely assessed in the literature assessing manual therapy outcomes. In this current study, we performed a secondary analysis of data from a randomized controlled clinical trial of interventions for LBP comparing two types of manual therapy: a thrust technique characterized by high velocity low amplitude movements (stress management training, SMT) and a non-thrust technique of lower velocity. [14]
Our first goal was to examine patient expectations related to a variety of common interventions for LBP. These were the expectations that patients had prior to beginning the physical therapy program. Our second goal was to determine the influence that specific expectations about SMT might have had on the patient outcomes in that primary trial. Predicted expectation for a specific intervention corresponds to clinical outcomes in individuals experiencing musculoskeletal pain. [7] Subsequently, interventions associated with higher predicted expectation may be inherently more effective than those for which patients have lower predicted expectations.
Methods
We performed a secondary analysis of data from a randomized controlled clinical trial14 comparing three interventions for patients who met the criteria of a validated clinical prediction rule (CPR). [15] Patients were recruited from four clinics in different geographic regions of the USA. The recruitment methods and description of the trial have been previously described. [14]
Participants
Patients with a report of LBP (with or without lower extremity symptoms) were recruited over a 28–month period (June 2005–September 2007). For patients to be eligible, they had to have a modified Oswestry Disability Questionnaire16 score of > 25%, be between 18 and 60 years of age, and to be positive for the validated spinal manipulation CPR using the originally published criteria. [15] Exclusion criteria included the presence of any red flags (i.e. tumor, metabolic diseases, RA, osteoporosis, prolonged history of steroid use, etc.), signs consistent with nerve root compression (reproduction of low back or leg pain with straight leg raise at less than 45°, muscle weakness involving a major muscle group of the lower extremity, diminished lower extremity muscle stretch reflex, or diminished or absent sensation to pinprick in any lower extremity dermatome). Other exclusion criteria included prior surgery to the lumbar spine and current pregnancy. This study was approved by the Institutional Review Boards at Andrews Air Force base, San Antonio, TX, USA; Concord Hospital, Concord, NH, USA; Intermountain Healthcare, Salt Lake City, UT, USA; and the University of Southern California, Los Angeles, CA, USA. All patients provided informed consent before their enrollment in the study. The primary trial was registered with ClinicalTrials.gov (NCT00257998). [14]
Interventions
In the primary study, participants were randomly assigned to one of three groups, two of which were thrust techniques and the other was a non-thrust intervention. [14] In addition to receiving the manual therapy interventions, patients were instructed at the first and second visit to perform anterior and posterior tilting in a pain free range. [14] On the third visit, patients began the strengthening and stabilization exercise program used in the validation of the CPR. [15] No other interventions were received.
Data collection
In addition to the demographic information and the primary outcome measures collected for the original trial, participants completed additional questionnaires. We measured two sets of expectations: expectations of benefit related to a specific intervention, and general or overall expectations about treatment. The participants' expectation of benefit related to a specific intervention was assessed before beginning treatment by asking them to consider the following statement: ‘I believe … will significantly help to improve this episode of my back pain’. Participants used a five-point Likert scale anchored at one end with ‘completely disagree’ and at the other with ‘completely agree’ to rate 10 interventions routinely used in rehabilitation practice. The list of interventions included aerobic exercise, manipulation, massage, medication, modalities, range of motion exercises, rest, traction, strengthening exercises, and surgery.
Separate from the expectations of benefit associated with specific interventions, we were also interested in participants' overall (general) expectations for treatment of their LBP. First, at the initial evaluation, we asked participants ‘What results do you expect from your treatment?’ related to complete relief from symptoms (pain, stiffness, swelling, numbness, weakness, and instability). Participants used a five-point Likert scale anchored with ‘definitely yes’ to ‘definitely not’ to indicate their general expectation for physical therapy. To determine whether these expectations were met during treatment, patients completed another questionnaire at the fifth treatment visit (4 weeks) considering the question: ‘Were your expectations for treatment met?’ and rating this using a Likert scale ranging from ‘not at all’ to ‘totally.’
Analysis
For analyses of expectations for a specific intervention, the categories ‘completely’ and ‘somewhat’ were collapsed resulting in three categories of response for each intervention (high, neutral, and low expectation). We were interested in patient predicted expectations for common physical therapy interventions in the treatment of individuals experiencing LBP related to the primary interventions used in the trial, namely, SMT. Therefore, we compared expectations for SMT to other interventions using Wilcoxon ranks testing. Given the large number of comparisons, we planned to conservatively correct for a type 1 error.
Next, we examined the association between specific expectations about SMT and outcomes. First, we examined whether a participant's baseline general expectation for treatment was met by the fifth visit to physical therapy. We used a three-way Pearson's chi-square test (group×belief×expectation met) to test the association between patient specific expectation regarding SMT and the intervention assignment; that is, we examined whether matching expectation to the intervention improved the odds of meeting the general expectation of having complete relief.
Then we tested the relationship between expectations and the patients' self-reports of disability. In the primary study, patients were classified as having a ‘successful outcome’ if the Oswestry Disability Index decreased 50% from baseline by visit 5 (week 4). [14] The unadjusted univariate association between a participants specific expectations about SMT and ‘successful outcome’ was calculated using chi-square tests. We also examined the association between ‘successful outcome’ and whether a participant's general expectation about treatment was met. Variables showing near significant (P < 0.10) univariate associations with the outcome were entered as independent variables into a multivariate analysis. Successful outcome was used as the response variable in a generalized linear model (logit link function). Predictor variables included belief that manipulation would improve the episode of pain, whether general expectations were. In addition, we wanted to include a variable representing the interaction between group assignment (thrust vs non-thrust) and specific expectation of benefit. A term was calculated using the simple product of the binary variables, and intervention group was entered.
Results

Table 1 A total of 112 patients (mean age: 40.4 years; 49% female) met the inclusion criteria of the primary study and agreed to participate. Sixty-one patients were recruited from New Hampshire, 33 from Utah, 16 from Los Angeles, and 2 from the Military Health Care System. Baseline characteristics of the participants are summarized in Table 1. There were no differences in the characteristics of the patients in each of the intervention groups, including the expectation of benefit from SMT.
Expectations regarding specific interventions for LBP
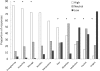
Figure 1 The expectations of benefit for the common interventions are summarized in Figure 1. In general, exercise and manual therapy interventions were expected to provide more benefit than surgery and medication. More than a quarter of the patients completely agreed that strengthening and stretching would provide the greatest relief for their current episode of LBP. In contrast, less than 5% of participants completely agreed that medication or surgery would provide relief. Statistically, strengthening, stretching, massage and aerobic exercise were all perceived to be more likely to provide relief than SMT (P < 0.001 for all comparisons). SMT was perceived to be more likely to provide relief than treatments such as traction, rest, medication, and surgery.
Association between expectation about SMT and general expectation for treatment

Table 2 General expectations for treatment were assessed at the fifth visit by asking patients the question: ‘Were your expectations for treatmentment?’ The proportion of patients for whom these general expectations were met was 52% (Table 2). The association between predicted expectation for the specific intervention and whether general expectations were met was tested by performing chi-square analyses layered by type of intervention. The results indicated a statistical association between expectation of relief from SMT (chi-square: 15.5, P = 0.008), but no association for patients who expected relief from SMT but did not receive it (chi-square: 6.9, P = 0.4). Furthermore, there was weak evidence of an association between having expectations met and experiencing successful outcome at visit 5 (chi-square: 11.9, P = 0.065).
Association between successful outcome and expectations
The univariate association between the specific expectation for SMT and a successful outcome was not significant (P = 0.063). Nor was the association between meeting expectations for treatment and a successful outcome (P = 0.065). However, both were within the threshold set for the multivariate analysis and therefore included in the multivariate model.

Table 3 The unadjusted odds ratio for successful outcome related to expectation of improvement from SMT compared to the expectation that SMT would not result in improvement was 3.6 (1.0, 12.9; P = 0.05). When this was adjusted to control for whether the general expectations for treatment were met, group assignment, and the interaction between group assignment and expectations regarding SMT, the parsimonious model only included group assignment as the significant contributor to the model (P < 0.001). The full model is presented in Table 3.
Discussion
The primary finding of this secondary analysis was that patients seeking intervention for LBP expect active interventions and manual therapy to significantly help improve their pain more than interventions such as rest, modalities, or medication. International guidelines for the management of LBP direct practitioners to adopt active intervention programs. [17, 18] Our finding that patients have highest expectations of relief attached to these interventions should encourage rehabilitation professionals to continue to advocate for such programs. Similarly, the finding that patients attach lower expectations of benefit to modalities and rest should encourage clinicians to de-emphasize use of these passive interventions in patient management. Not only is there limited evidence of the effectiveness of these interventions for patients with acute LBP, [19] the results of our study indicate that patients in this clinical trial did not expect these interventions to provide relief.
The low expectation of benefit, particularly for modalities, may also present a quandary for investigators performing experimental studies. Often modalities, such as subthermal ultrasound, [20] or detuned laser, [21] have been used as sham treatments in trials of manual therapy interventions. The effectiveness of a sham intervention or placebo hinges on the ‘believability’ of the intervention; that is, patients must expect that the sham intervention will be as effective as the comparison. Clearly, in this group of patients in the current study, this was not the case. In fact, these results indicate that less than 40% of the patients expected relief from modalities. While our findings must be replicated in larger samples of patients with LBP, we suggest that any proposed sham interventions be rigorously tested for the patient expectations associated with such interventions.
The primary study on which our secondary analysis was based examined whether the velocity of the technique was important in determining the prognosis of patients who met a specific clinical prediction rule. Therefore, we were interested in how patients' expectations for SMT compared to the other common interventions for LBP. The results indicated that more than half the patients agreed that they would experience improvement in their back pain if they received a thrust technique as an intervention. While this was less than the active exercise interventions and massage, it was greater than the other interventions. We think this to be important given anecdotal suggestions that one of the limitations to the application of SMT in clinical practice might be the reluctance of patients to receive the intervention. Our data indicate that patients are more likely to have high expectations of pain relief from SMT than other common interventions.
In addition to expectations regarding individual interventions, we also assessed patients' overall expectations for their treatment. At the fifth patient visit (in week 4), 52% of patients indicated that they had met their expectations. When we examined the relationship between the general expectation for treatment and specific expectation for SMT, we found that if subjects had the expectation that SMT would help and received SMT, approximately 90% of patients indicated that their general expectations had been ‘quite a bit’, ‘almost totally’ or ‘totally’. In contrast, this proportion was only 44% if they did not receive SMT. This means that if the patient believed that SMT would help, and he received SMT, he was more likely to report that his overall general expectation about what he wanted to have happen by coming to PT was met. Prior work has indicated that meeting general expectations is associated with patient satisfaction and higher reported function. [22]
When we ran a model predicting successful outcome, however, the interaction between having high expectations for SMT and receiving SMT was NOT significant. The effect of treatment was so large in this model that no other factors contributed anything. The import of this finding is that treating someone who fits the CPR with SMT is likely to result in a successful outcome even if that person does not believe that SMT will help. However, we are limited in applying our findings to other patients with LBP. All patients in our study met the clinical prediction rule suggesting homogeneity in this group of patients. Consequently, our preliminary observations regarding the interactions among specific expectations about an intervention and factors salient to outcome must be studied in larger samples of patients and across a variety of interventions. One might expect, for example, that the effect sizes related to specific expectations about an intervention will be different when interventions that vary to a greater degree are compared. In the current study, the interventions were manual therapy techniques that differed by velocity. There is the potential that patients naive to the practice of manual therapy may not discern great differences between thrust and non-thrust interventions. In contrast, studies that have demonstrated larger effects related to expectation have compared varied interventions, such as acupuncture and massage.
None-the-less, we are confident that our findings indicate that patients expect active interventions and manual therapy (manipulation and massage) to be more effective than passive interventions. Physical therapists should be very encouraged by these findings.
Acknowledgments
We would like to thank American Academy of Orthopaedic Manual Physical Therapists, 2005 Cardon Rehabilitation Products Grant, for providing funding for the initial clinical trial. This manuscript was written while MDB received support from the National Institute of Arthritis and Musculoskeletal and Skin Disorders (no. K01AR054331) and JEB received support from the Rehabilitation Research Career Development Program (no. 5K12HD055929-02).
References:
Thompson AG, Sunol R.
Expectations as determinants of patient satisfaction:
concepts, theory and evidence.
Int J Qual Health Care 1995;7:127–41Gepstein R, Arinzon Z, Adunsky A, Folman Y.
Decompression surgery for lumbar spinal stenosis in the elderly:
preoperative expectations and postoperative satisfaction.
Spinal Cord 2006;44:427–31Goldstein MS, Morgenstern H, Hurwitz EL, Yu F.
The impact of treatment confidence on pain and related disability among patients
with low-back pain: results from the University of California, Los Angeles, low-back pain study.
Spine J 2002;2:391–9Ozegovic D, Carroll LJ, David CJ.
Does expecting mean achieving? The association between expecting to return to work
and recovery in whiplash associated disorders: a population-based prospective cohort study.
Eur Spine J 2009;18:893–9Goossens ME, Vlaeyen JW, Hidding A, et al.
Treatment Expectancy Affects the Outcome of Cognitive-Behavioral Interventions in Chronic Pain
Clin J Pain 2005 (Jan); 21 (1): 18–26Mondloch MV, Cole DC, Frank JW.
Does how you do depend on how you think you'll do? A systematic review
of the evidence for a relation between patients' recovery expectations and health outcomes.
CMAJ 2001;165:174–9Kalauokalani D, Cherkin DC, Sherman KJ, Koepsell TD, Deyo RA.
Lessons from a trial of acupuncture and massage for low back pain:
patient expectations and treatment effects.
Spine (Phila Pa 1976) 2001;26:1418–24Myers SS, Phillips RS, Davis RB, Cherkin DC, Legedza A,
Kaptchuk TJ, Hrbek A, Buring JE, Post D, Connelly MT, Eisenberg DM.
Patient Expectations as Predictors of Outcome in Patients with Acute Low Back Pain
Journal of General Internal Medicine 2008 (Feb); 23 (2): 148–153Childs JD, Cleland JA.
Development and application of clinical prediction rules to improve decision making
in physical therapist practice.
Phys Ther 2006;86:122–31Cleland JA, Childs JD, Fritz JM, Whitman JM, Eberhart SL.
Development of a Clinical Prediction Rule for Guiding Treatment of a Subgroup of Patients With Neck Pain:
Use of Thoracic Spine Manipulation, Exercise, and Patient Education
Phys Ther. 2007 (Jan); 87 (1): 9–23Fernandez-de-las-Penas C, Cleland JA, Cuadrado ML, Pareja JA.
Predictor variables for identifying patients with chronic tension-type
headache who are likely to achieve short-term success with muscle trigger point therapy.
Cephalalgia 2008;28:264–75Flynn T, Fritz J, Whitman J, Wainner R, Magel J, Rendeiro D, et al.
A Clinical Prediction Rule for Classifying Patients with Low Back Pain
who Demonstrate Short-term Improvement with Spinal Manipulation
Spine (Phila Pa 1976). 2002 (Dec 15); 27 (24): 2835–2843Whitman JM, Cleland J, Mintken P.
Clinical prediction rules in physical therapy: coming of age?
J Orthop Sports Phys Ther 2009;39:231–3Cleland JA, Fritz JM, Childs JD, Kulig K.
Comparison of the effectiveness of three manual physical therapy techniques in
a subgroup of patients with low back pain who satisfy a clinical prediction rule:
study protocol of a randomized clinical trial [NCT00257998].
BMC Musculoskelet Disord 2006;7:11.Childs JD, Fritz JM, Flynn TW, Irrgang JJ, Johnson KK, Majkowski GR, et al.
A Clinical Prediction Rule To Identify Patients With Low Back Pain Most Likely To Benefit
from Spinal Manipulation: A Validation Study
Annals of Internal Medicine 2004 (Dec 21); 141 (12): 920–928Fritz JM, Irrgang JJ.
A comparison of a modified Oswestry Low Back Pain Disability Questionnaire
and the Quebec Back Pain Disability Scale.
Phys Ther 2001;81:776–88Koes BW, van Tulder MW, Ostelo R, Kim Burton A, Waddell G.
Clinical Guidelines for the Management of Low Back Pain in Primary Care:
An International Comparison
Spine (Phila Pa 1976) 2001 (Nov 15); 26 (22): 2504–2513Spitzer WO, Skovron ML, Salmi LR, Cassidy JD, Duranceau J, Suissa S, Zeiss E.
Scientific Monograph of the Quebec Task Force on Whiplash-Associated Disorders
Redefining Whiplash and its Management
Spine (Phila Pa 1976). 1995 (Apr 15); 20 (8 Suppl): S1-S73Stanley J. Bigos, MD, Rev. O. Richard Bowyer, G. Richard Braen, MD, et al.
Acute Lower Back Problems in Adults. Clinical Practice Guideline No. 14.
Rockville, MD: Agency for Health Care Policy and Research, [AHCPR Publication No. 95-0642].
Public Health Service, U.S. Department of Health and Human Services; 1994Deyle GD, Henderson NE, Matekel RL, Ryder MG, Garber MB, Allison SC.
Effectiveness of manual physical therapy and exercise in osteoarthritis of the knee.
A randomized, controlled trial.
Ann Intern Med 2000;132:173–81Preyde M.
Effectiveness of massage therapy for subacute low-back pain: a randomized controlled trial.
CMAJ 2000;162:1815–20George SZ, Hirsh AT.
Distinguishing patient satisfaction with treatment delivery from treatment effect:
a preliminary investigation of patient satisfaction with symptoms after
physical therapy treatment of low back pain.
Arch Phys Med Rehabil 2005;86:1338–44

Return to LOW BACK PAIN
Return to PATIENT EXPECTATIONS OF RELIEF
Since 10–11–2017


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |