The Safety of Chiropractic This section was compiled by Frank M. Painter, D.C.
Send all comments or additions to: Frankp@chiro.org




|
|
Conditions That Respond | Alternative Medicine Approaches to Disease |




Controversy. The Media feeds on it.
Millions of patients love their chiropractor and appreciate our unique and safe approach to recovery from pain. Significant research suggests that chiropractic is the safest approach available for relief from neck pain, back pain, headaches and other “musculo–skeletal” complaints. Lets review that research, and discuss how Organized Medicine (or at the very least, some of her angry minions) has contributed to the myth that chiropractic care is dangerous.
First, a short review of historyIn the early 1960's, the American Medical Association (AMA) decided to try to contain and eliminate Chiropractic as a profession. [1]
The AMA's plan was to:
prevent medical physicians from referring patients to Chiropractors, and preventing them from accepting referrals from Chiropractors;
preventing Chiropractors from obtaining access to hospital diagnostic and radiology services;
preventing medical physicians from teaching at chiropractic colleges, or engaging in any form of joint research;
and, to stifle any other form of cooperation between the two professions.
Medical journals were also told not to publish any chiropractic research, unless the results were negative. This practice persisted until the mid- to late-1990s.
The AMA also told its membership, medical students, insurance companies, and the general public that Chiropractic was an “unscientific cult”.
In 1976, five Chiropractors filed a lawsuit against the AMA and 20 other medical specialty organizations as co-conspirators, for violation of the Sherman Anti-trust Laws. After 15 years of litigation, the U.S. Court of Appeals stated that the AMA intended to “destroy a competitor,” and that there was evidence “showing that the AMA was motivated by economic concerns”. The court found that the AMA had concealed evidence showing it's guilt, and was caught “doctoring” documents. The AMA was also “guilty of systematic, long term wrong doing and has not acknowledged its lawlessness”. [1]
Following the Court enforced reversal of AMA's policy, tiny splinter groups formed, with the intention of labeling chiropractic as a quackish cult. Their methods mimicked the earlier AMA suppression tactics: Create doubt about the quality of chiropractic education, and mislead the public into believing that chiropractic claims ALL disease is caused by subluxations. Although these groups hide behind the noble claim that they wish to protect the public from unscientific practices, their true motives are transparent. Their sole intention is to suggest that only allopathic medicine is well supported by scientific research. However, that is just not true!
In an editorial in the highly esteemed British Medical Journal, titled Where is the Wisdom? The Poverty of Medical Evidence, BMJ's editor Dr. Richard Smith recounts a lecture he attended with renowned health policy consultant Dr. David Eddy. Eddy found, after doing significant research, that only about 13% of medical interventions are supported by, solid scientific evidence and that only 1% of the articles in medical journals are scientifically sound. Why is that? Because most of those articles quote from other articles which make unsupported and unfounded claims.
The Increasing Popularity of Alternative Medicine
After publication of David M. Eisenberg's 1993 New England Journal of Medicine article, titled Unconventional Medicine in the United States, various factions of organized medicine became increasingly anxious, and aggressive in their accusations that alternative approaches to medical healthcare were not supported by research. [2]
This same group was hardly forthcoming in mentioning the small fraction of established medical practices that had ever met those same stringent requirements. They certainly never mention the low level of success which medicine delivers for the same health complaints for which chiropractic has become famous.
Interesting Sidebar from the British Medical Journal (PDF) Scientific heavyweights deplore the NHS money wasted on “unproved and disproved” treatments used by practitioners of complementary and alternative medicine (CAM), [1, 2] but Lewith, a CAM proponent (see previous letter), is cited elsewhere as saying that the BMJ reckons that 50% of the treatments used in general practice aren’t proved, and 5% are pretty harmful but still being used. [3]
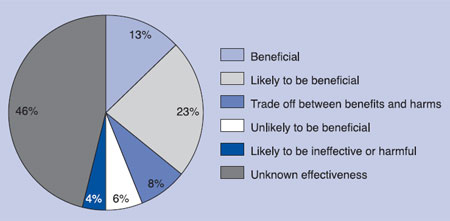
His data were taken from the BMJ Clinical Evidence website. A pie chart (see it below in the Evidence-based Practice posting) indicates that, of about 2500 treatments supported by good evidence, only 15% of treatments were rated as beneficial, 22% as likely to be beneficial, 7% part beneficial and part harmful, 5% unlikely to be beneficial, 4% likely to be ineffective or harmful, and in the remaining 47% the effect of the treatment was “unknown.”
Read more on this topic
The text says, “The figures suggest that the research community has a large task ahead and that most decisions about treatments still rest on the individual judgements of clinicians and patients.” On 9 October 2007 the situation had changed—but not for the better. Treatments rated “beneficial” had decreased from 15% to 13%.
REFERENCES:
- Kamerow D.
Wham, bang, thank you CAM.
British Medical Journal 2007 (Sep 29); 335: 647
- Colquhoun D.
What to do about CAM?
British Medical Journal 2007 (Oct 13); 335: 736
- Cope J.
The great debate.
Healthwriter 2007 (Apr): 1-3.
The High Risks of the Medical ApproachDr. Lucian Leape, researcher at the Harvard Medical School of Public Health, also states that only 13-15% of medical procedures have ever been tested for appropriateness by randomized trials. He noted that adverse events occurred in 3.7 percent of all hospitalizations. Worse yet, 13.6 percent of those adverse events led to death! [3]. He is also quoted as saying:
“Medicine is now a high risk industry, like aviation. But, the chance of dying in an aviation accident is one in 2 million, while the risk of dying from a medical accident is one in 200!” [4]
The most comprehensive review of “adverse events” (also referred to as “Iatrogenic Injury”) caused by modern medicine is the article Death by Medicine, written by Gary Null, Ph.D.; Carolyn Dean MD, ND; Martin Feldman, MD; Debora Rasio, MD; and Dorothy Smith, PhD. [5].
This fully referenced report reveals that:
2.2 million people experience in-hospital, adverse reactions to prescribed drugs per year.
20 million unnecessary antibiotics are prescribed annually for viral infections
7.5 million unnecessary medical and surgical procedures are performed annually, and
8.9 million people are exposed to unnecessary hospitalization every year!
The most stunning statistic, however, is that the total number of deaths caused by conventional medicine is an astounding 783,936 per year!
That is a mind-boggling 2,147 people killed daily!
That's 7 jumbo jet plane crashes, each and every day.
That's a 9-11 incident occurring EVERY OTHER DAY...FOREVER.
God help us all.
Now, Lets Discuss the Safety of Chiropractic
Canada has a government-run national health care system. As occurred with Medicare in this country, there had been such pressure on the Canadian government to include chiropractic as a covered benefit, that the Ontario Ministry of Health hired a renowned heath care economist to make a recommendation. The first “Manga Report” [6] was published in 1993.
This comprehensive study reviewed all the published literature on low back pain and made some astounding suggestions. In a nutshell, it concluded that: chiropractic should be the treatment of choice for low back pain – excluding traditional medical care altogether!The specific Findings of the report were:
There is an overwhelming body of evidence indicating that chiropractic management of low-back pain is more cost-effective than medical management
Many medical therapies are of questionable validity or are clearly inadequate
There is no clinical or case-control study that demonstrates or even implies that chiropractic spinal manipulation is unsafe in the treatment of low-back pain. Some medical treatments are equally safe, but others are unsafe and generate iatrogenic complications for LBP patients.
Chiropractic is more cost-effective. There would be highly significant cost savings if more management of LBP was transferred from medical physicians to chiropractors.
There is good empirical evidence that patients are very satisfied with chiropractic management of LBP, and they are also considerably less satisfied with medical management.
The specific Recommendations were:
Chiropractic services should be fully insured under the Ontario Health Insurance Plan
Chiropractic services should be fully integrated into the health care system. Because of the high incidence and cost of LBP, hospitals, managed health care groups, community health centers, comprehensive health organizations, and health service organizations and long-term care facilities should employ chiropractors on a full-time and/or part-time basis
A good case could be made for placing chiropractic as the gatekeepers for all musculoskeletal complaints that presented to hospitals.
More Bad News For Medical PatientsA series of articles reporting on the lack of medical training in musculoskeletal disorders was published between 1998 and 2002 by Kevin B. Freedman, MD [7], [8]. It seems that the department chairs of several hospital-based orthopedic residency programs designed a basic examination on musculoskeletal competency and gave it to their residents. 82 per cent of medical school graduates failed the examination. Four years later the test was simplified and, once again, 78% of the examinees failed to demonstrate basic competency in musculoskeletal medicine. When this test was given to final quarter chiropractic students 70% of them passed the exact same exam! [9]
The differences between these 2 student groups MUST be noted.
The medical students had already graduated from medical school (as MDs) and they had also completed several years worth of residency rotations through every hospital department. Finally, they had been accepted into a hightly competitive orthopedic residency program... the pinnacle of medical musculoskeletal specialists. The chiropractic students however were still just final year students.
An 80% medical failure versus 70% chiropractic success. Quite astonishing!
Review of Specific Safety Studies
A. The Safety of Cervical AdjustingNo one pays closer attention to injury statistics than Malpractice Insurance carriers.
Scott Haldeman, MD, DC reviewed malpractice claims records for a 10-year period between 1988 and 1997. In reviewing the outcomes following the application of 134.5 million cervical manipulations (commonly referred to as the chiropractic adjustment), the records indicated that there were 23 reported cases of stroke or vertebral artery dissection (VAD). [10] Of this group, 10 of the patients had the complicating factors of high blood pressure, use of oral contraceptives, or a history of smoking, all of which are associated with vascular disease. The actual incidence of stroke or VAD following cervical manipulation was found to be one per 5.85 million cervical adjustments. That means that the average chiropractor could work for 1,430 years (or practice 48 full chiropractic careers!) before they might be involved with this type of litigation.
Other reports, listing a higher frequency of adverse events, have been compromised by the tendency of those authors to inappropriately list the pracitioner as a chiropractor, even when it turned out that the injury was caused by a medical doctor, a physical therapist or a hairdresser! [11], [12]
Rather than raising concerns about the safety of chiropractic, these statistics emphasize that spinal manipulation, in the hands of unskilled practitioners, is dangerous, and the practice must be closely regulated. [13]
The World Health Organization recently released a comprehensive set of guidelines that clearly states that chiropractic is a separate profession, rather than a set of techniques that can be learned in short courses by other health professionals. They also make it clear that medical doctors and other health professionals, in countries where the practice of chiropractic is not regulated by law, should undergo extensive training to re-qualify as chiropractors before claiming to offer chiropractic services. In some countries there have been recent efforts by medical groups to provide short courses of approximately 200 hours in chiropractic technique.
WHO’s guidelines indicate that a medical graduate should a require an additional minimum of 1,800 class hours, which would include 1,000 hours of supervised clinical training, before claiming to offer chiropractic services. [14]
B. The Safety of Low Back AdjustingLower back injury alleged to have occurred following spinal manipulative therapy has been reported in patients with pre-existing disc herniation or prolapse. While it is suggested that the forces required to cause a disruption of the annular fibers of the healthy intervertebral disc well exceed that of a rotational manipulative thrust, some disc herniation/protrusion may certainly be aggravated by an inappropriately applied manipulative maneuver, as it may be by other simple activities of daily living such as bending, sneezing, or lifting. The most frequently described severe complication is compression of the cauda equina by massive midline nuclear herniation at the level of the 3rd, 4th or 5th intervertebral disc.
Of the 30 cauda equina complications associated with manipulation reported in the French, German and English literature over an 80 year period, only 8 were allegedly related to chiropractic treatment. [15]
The Risks of Medical Procedures Aimed at Relief of Similar Symptoms ” [25]
A. Non Steriodal Anti-Inflammatories (NSAIDs)One group of patients who rely on NSAIDs for pain relief are those suffering from rheumatoid arthritis. In 1998, Dr. Singh of the Stanford University of Medicine reviewed the records of 11,000 arthritis patients at 8 participating institutions. He extrapolated that approximately 107,000 patients are hospitalized annually for nonsteroidal anti-inflammatory drug (NSAID)-related gastrointestinal (GI) complications (internal bleeding) and at least 16,500 NSAID-related deaths occur each year among arthritis patients alone.
The figures for ALL of the NSAID users combined would be overwhelming, yet the scope of this problem is generally under-reported. [16]
Another article titled “36 Percent of Acute Liver Failures Are Linked to Acetaminophen” suggests that other organ systems are also compromised by the use of over-the-counter pain medications. [17]
Lauretti's review of the literature found that The best evidence indicates that cervical manipulation for neck pain is much safer than the use of NSAIDs, by as much as a factor of several hundred times. [27]
B. Spinal SurgeryFirst, let's review some history. In 1974, the Congressional Committee on Interstate and Foreign Commerce held hearings on unnecessary surgery. Their findings from the First Surgical Second Opinion Program found that 17.6% of recommendations for surgery were not confirmed. The House Subcommittee on Oversight and Investigations extrapolated these figures to estimate that, on a nationwide basis, there were 2.4 million unnecessary surgeries performed annually resulting in 11,900 deaths at an annual cost of $3.9 billion. [18]
With the total number of lower back surgeries having been estimated in 1995 to exceed 250,000 in the U.S. at a hospital cost of $11,000 per patient. [19] This would mean that the total number of unnecessary back surgeries each year in the U.S. could approach 44,000, costing as much as $484 million. [20]
So, the biggest risk of spinal surgery is that it may not be necessary.
In fact, the most-recent studies suggests that:
Back Surgery Fails 74% of the Time
The next set of risks include:
a 2.1% chance of a serious adverse drug reaction. [21]
a 5-6% chance of acquiring a nosocomial infection [22]
a 4-36% chance of having an iatrogenic injury (medical error or adverse drug reactions). [23]
a 17% chance of a procedure error. [24]
As few as 3%, and no more than 20% of iatrogenic injuries are ever reported! Yipes! [5]
That takes all the fun out of being a statistic, doesn't it?
This September 2006 article from the Journal of the American Academy of Orthopedic Surgeons says it all:“Failed back surgery syndrome is a common problem with enormous costs to patients, insurers, and society. The etiology of failed back surgery can be poor patient selection, incorrect diagnosis, suboptimal selection of surgery, poor technique, failure to achieve surgical goals, and/or recurrent pathology.
That my friends is right from the horse's mouth.
The most recent controversy is from the New York Times:” [26]“Spinal-fusion surgery is one of the most lucrative areas of medicine. An estimated half-million Americans had the operation this year, generating billions of dollars for hospitals and doctors.
But there have been serious questions about how much the surgery actually helps patients with back pain and whether surgeons’ generous fees might motivate them to overuse the procedure. Those concerns are now heightened by a growing trend among some surgeons to profit in yet another way — by investing in companies that make the screws and other hardware that they (personally) install.
Now, added to concerns about medicine's poor musculoskeletal training and dangerous statistics, we have to wonder if the orthopedist might be motivated to install 6 of those $1,000 screws in your spine, because they are a stockholder in a lucrative medical device manufacturer that produces them.
The sanest and safest approach is to use conservative approaches like chiropractic care first. You can always resort to drugs or surgical approaches as a last-ditch resort, but the statistics suggest that most low-back and neck pain can be successfully managed with lower costs and higher patient satisfaction by chiropractors.
You may want to explore
research supporting chiropractic care for a wide variety of conditions in our Research section. There is also a significant body of work demonstrating the vastly superior Cost-Effectiveness of Chiropractic, as well as contrasting Patient Satisfaction with Chiropractic to standard Medical Care for the same conditions.
The Chiropractic Antitrust Suit ~ Wilk, et al vs. the AMA, et al Unconventional Medicine in the United States: Incidence of Adverse Events and Negligence in Hospitalized Patients The Iatrogenic Injury Page
Death by Medicine
A Study to Examine the Effectiveness and Cost-Effectiveness of Chiropractic
The Adequacy of Medical School Education in Musculoskeletal Medicine
Educational Deficiencies in Musculoskeletal Medicine
A Comparison of Chiropractic Student Knowledge Versus Medical Residents Haldeman S, Carey P, Townsend M, Papadopoulos C. Terrett AGJ:
Inappropriate Use of the Title Chiropractor and Term Chiropractic Manipulation
Are German Orthopedic Surgeons Killing People With Chiropractic? World Health Organization (WHO) Guidelines for Chiropractic Quality Assurance and Practice Parameters
Recent Considerations in Nonsteroidal Anti-inflammatory Drug Gastropathy
36 Percent of Acute Liver Failures Are Linked to Acetaminophen US Congressional House Subcommittee Oversight Investigation. Herman R.
Testimony to the Department of Veterans Affairs' Chiropractic Advisory Committee
Incidence of Adverse Drug Reactions in Hospitalized Patients Nosocomial Infection Update Error in Medicine Medication errors in hospitalized cardiovascular patients
Failed Back Surgery Syndrome: Diagnostic Evaluation
The Spine as Profit Center Dabbs V Lauretti WJ
REFERENCES:
The Chiropractic Resource Archives
https://www.chiro.org/Wilk/
Prevalence, Costs, and Patterns of Use
New England Journal of Medicine 1993 (Jan 28); 328 (4):246–252
Results of the Harvard Medical Practice Study I
Iatrogenic_Page.shtml
Life Extension Foundation
Management of Low-Back Pain
Ministry of Health, Government of Ontario Canada 1993
Journal of Bone and Joint Surgery 1998 (Oct); 80-A (10): 1421–1427
Journal of Bone and Joint Surgery 2002 (Apr); 84–A (4): 604–608
Proceedings of the World Federation of Chiropractic Congress 2001 Pgs. 255
Arterial Dissections Following Cervical Manipulation: The Chiropractic Experience
Canadian Medical Association Journal (CMAJ) 2001 (Oct 2); 165: 905–906
Misuse of the Literature by Medical Authors in Discussing Spinal Manipulative Therapy Injury
J Manipulative Physiol Ther 1995 (May); 18 (4): 203–210
in the Peer-reviewed Biomedical Literature
Chiropractic & Osteopathy 2006 (Aug 22); 14 (1): 16
ChiroZine ~ 3-26-2005 ~ Editorial Commentary
WHO Guidelines on Basic Training and Safety in Chiropractic
Geneva, Switzerland: (November 2005)
Preceedings of the Mercy Center Consensus Conference; Page 171
Aspen Publications 1993
American Journal of Medicine 1998 (Jul 27);105 (1B):31S–38S
U.S. News & World Report July 2, 2001
Cost and Quality of Health Care: Unnecessary Surgery.
Washington, DC: Government Printing Office, 1976
Back Surgery.
Washington Post [Health Section], April 18, 1995
George B. McClelland, D.C.,
Foundation for Chiropractic Education and Research March 25, 2003
JAMA 1998 (Apr 15); 279 (15): 1200-1205
Emerg Infect Dis 1998 (Jul); 4 (3): 416-420
JAMA 1994 (Dec 21); 272 (23): 1851-1857
Arch Intern Med 2003 (Jun 23); 163 (12): 1461-1466
Journal of the American Academy of Orthopaedic Surgeons 2006 (Sep); 14 (9): 534-543
New York Times December 30, 2006
A Risk Assessment of Cervical Manipulation vs. NSAIDs for the Treatment of Neck Pain
J Manipulative Physiol Ther 1995 (Oct); 18 (8): 530–536

Return to the LINKS
Return to ChiroZINE
Return to TELL ME ABOUT CHIROPRACTIC
Since 10–17–2006Updated 10–24–2025


| Home Page | Visit Our Sponsors | Become a Sponsor |
Please read our DISCLAIMER |